Crafting an effective nursing care plan is fundamental for delivering optimal patient care. It’s a systematic approach that ensures all patient needs, both current and potential, are meticulously addressed. This comprehensive guide will walk you through the essential steps of developing a robust nursing care plan, emphasizing the critical role of nursing diagnoses. Whether you are a student nurse or a seasoned professional, this resource offers a detailed understanding of care plan components, objectives, and practical applications to enhance your nursing practice.
Understanding the Nursing Care Plan
A nursing care plan (NCP) is a structured, formal document that meticulously identifies a patient’s existing health needs and anticipates potential risks. It serves as a vital communication tool among nurses, patients, and the interdisciplinary healthcare team, ensuring cohesive and goal-oriented care. The absence of a well-defined nursing care planning process can compromise the quality and consistency of patient care.
The process of nursing care planning commences upon patient admission and is continuously revised and updated in response to changes in the patient’s condition and the ongoing evaluation of goal achievement. At its core, nursing care planning is about delivering individualized, patient-centered care, which is the hallmark of excellence in nursing practice.
Types of Nursing Care Plans: Formal vs. Informal and Standardized vs. Individualized
Nursing care plans can be broadly categorized into informal and formal types.
An informal nursing care plan is essentially a mental strategy, an action plan residing in the nurse’s mind. In contrast, a formal nursing care plan is a documented guide, either written or computerized, that systematically organizes patient care information.
Formal care plans are further divided into standardized and individualized approaches:
Standardized Care Plans: These are pre-written guides outlining nursing care for patients with common, recurring needs. They ensure consistent care for specific patient populations, promote adherence to minimum care standards, and optimize nurses’ time by eliminating repetitive planning for routine care activities.
Standardized care plans, while efficient, are not designed to address the unique needs of each patient. They serve as a starting point, a foundation upon which to build an individualized care plan.
The care plans presented in this guide are standardized examples intended to provide a framework for developing individualized care plans.
Individualized Care Plans: An individualized care plan tailors the standardized plan to meet the specific, unique needs and goals of each patient. This approach incorporates interventions proven effective for the individual, fostering personalized and holistic care.
Individualized care plans are also crucial for enhancing patient satisfaction. When patients perceive their care as tailored to their specific circumstances, they feel more valued and understood, leading to greater satisfaction with their healthcare experience. In today’s healthcare landscape, patient satisfaction is increasingly recognized as a key indicator of care quality.
Tips for Individualizing a Nursing Care Plan:
- Incorporate Patient Preferences: Actively seek and integrate the patient’s values, beliefs, and preferences into the care plan.
- Address Unique Needs: Identify and address needs not covered in standardized plans, such as cultural considerations, emotional support, or specific learning requirements.
- Focus on Strengths: Build upon the patient’s strengths and resources to promote resilience and active participation in their care.
- Collaborate with Patient: Engage the patient in the planning process to ensure the plan aligns with their goals and expectations.
- Regularly Review and Revise: Continuously assess the plan’s effectiveness and adapt it based on the patient’s evolving needs and responses.
Objectives of Nursing Care Plans
The objectives of developing a nursing care plan are multifaceted and aim to:
- Promote Evidence-Based Care: Ensure nursing care is grounded in the best available evidence, creating a consistent and reliable healthcare environment.
- Support Holistic Patient Care: Address the patient as a whole, encompassing physical, psychological, social, and spiritual dimensions in disease management and prevention.
- Establish Care Programs: Facilitate the development of structured care pathways and care bundles, ensuring standardized and best-practice approaches to specific conditions.
- Define Goals and Expected Outcomes: Clearly articulate the desired health outcomes and the steps to achieve them.
- Enhance Communication and Documentation: Improve communication among healthcare providers and ensure accurate, comprehensive documentation of patient care.
- Measure Nursing Care Effectiveness: Provide a framework for evaluating the impact and quality of nursing interventions.
Purposes and Importance of Nursing Care Plans
Nursing care plans serve several critical purposes in healthcare delivery:
- Define the Nurse’s Role: Care plans underscore the unique and independent role of nurses in addressing patients’ overall health and well-being, beyond simply executing physician’s orders.
- Guide Individualized Patient Care: They act as a roadmap for patient care, prompting nurses to think critically and develop interventions specifically tailored to each patient’s needs.
- Ensure Continuity of Care: By providing a documented plan, care plans enable nurses across different shifts and departments to deliver consistent, high-quality interventions, maximizing treatment benefits for patients.
- Coordinate Interdisciplinary Care: Care plans facilitate communication and collaboration among all members of the healthcare team, ensuring everyone is informed of the patient’s needs and the necessary actions, thus preventing gaps in care.
- Serve as Documentation: A well-written care plan accurately documents observations, nursing actions, and patient/family instructions. Proper documentation in the care plan is evidence that care was provided.
- Guide Staff Assignment: In situations requiring specific skills, care plans assist in assigning appropriate staff based on patient needs.
- Monitor Patient Progress: Care plans enable the tracking of patient progress and facilitate necessary adjustments to the care strategy in response to changes in health status and goals.
- Support Reimbursement: Insurance companies often utilize medical records, including care plans, to determine coverage and reimbursement for hospital care.
- Define Patient Goals: Care plans actively involve patients in their treatment and care by clearly outlining their goals and the strategies to achieve them.
Key Components of a Nursing Care Plan
A standard nursing care plan typically includes several core components, each playing a vital role in guiding patient care:
- Nursing Diagnoses: These are clinical judgments about individual, family, or community responses to actual or potential health problems or life processes. They provide the foundation for the care plan.
- Patient Problems/Needs: A broader description of the patient’s health issues, often derived from the assessment data.
- Expected Outcomes: Specific, measurable, achievable, relevant, and time-bound (SMART) statements describing the desired changes in patient health status as a result of nursing care.
- Nursing Interventions: Actions that nurses will perform to achieve the expected outcomes. These are evidence-based and tailored to the patient’s needs.
- Rationales: The scientific reasons or evidence supporting the chosen nursing interventions.
- Evaluation: A process to assess the patient’s progress toward achieving the expected outcomes and the effectiveness of the nursing care plan.
Care Plan Formats: 3-Column, 4-Column, and Student Care Plans
Nursing care plans are often organized into different column formats to structure the information clearly. Common formats include three-column and four-column plans, with variations for student nurses.
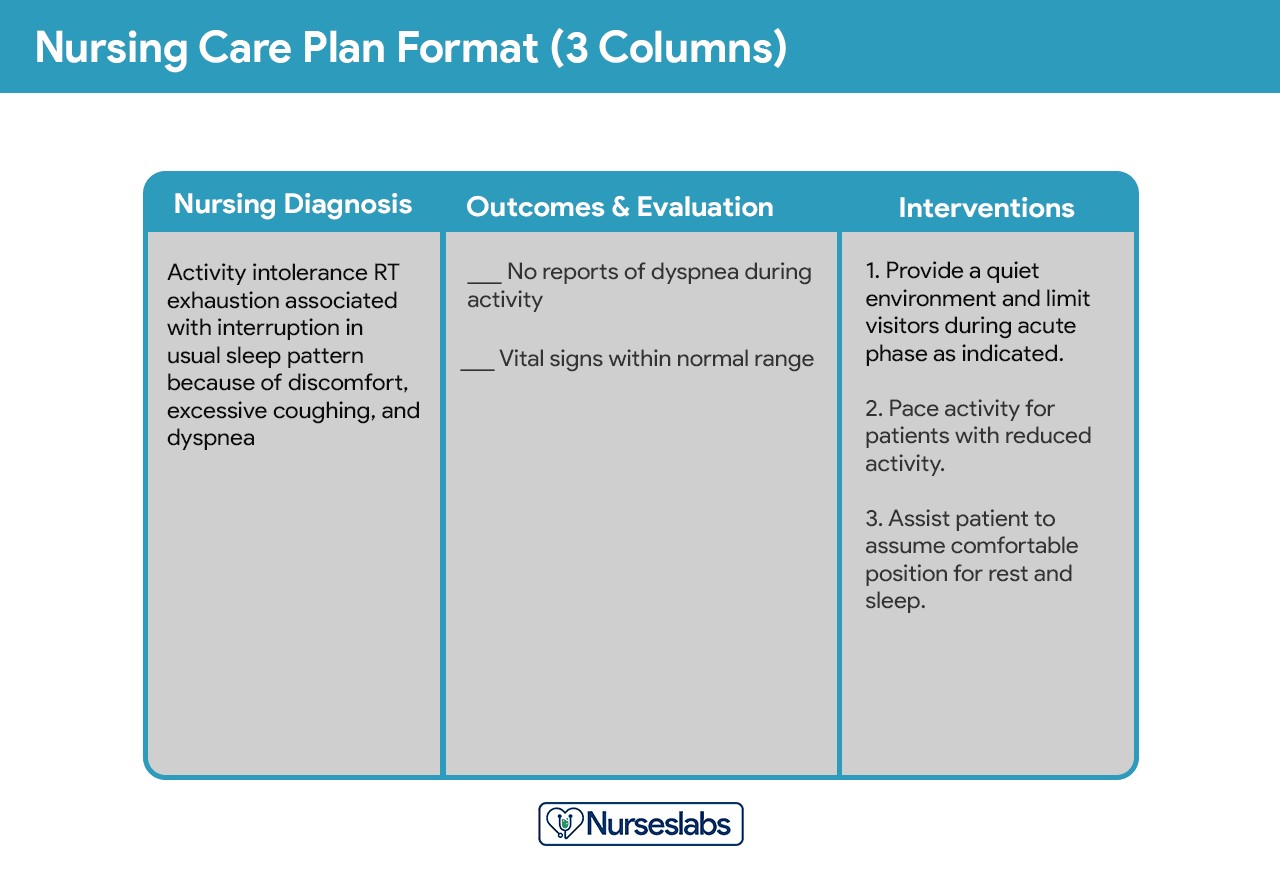
Three-Column Format: This format typically includes columns for:
- Nursing Diagnosis: The identified nursing diagnosis.
- Outcomes and Evaluation: Desired patient outcomes and criteria for evaluation.
- Interventions: Nursing actions to achieve outcomes.
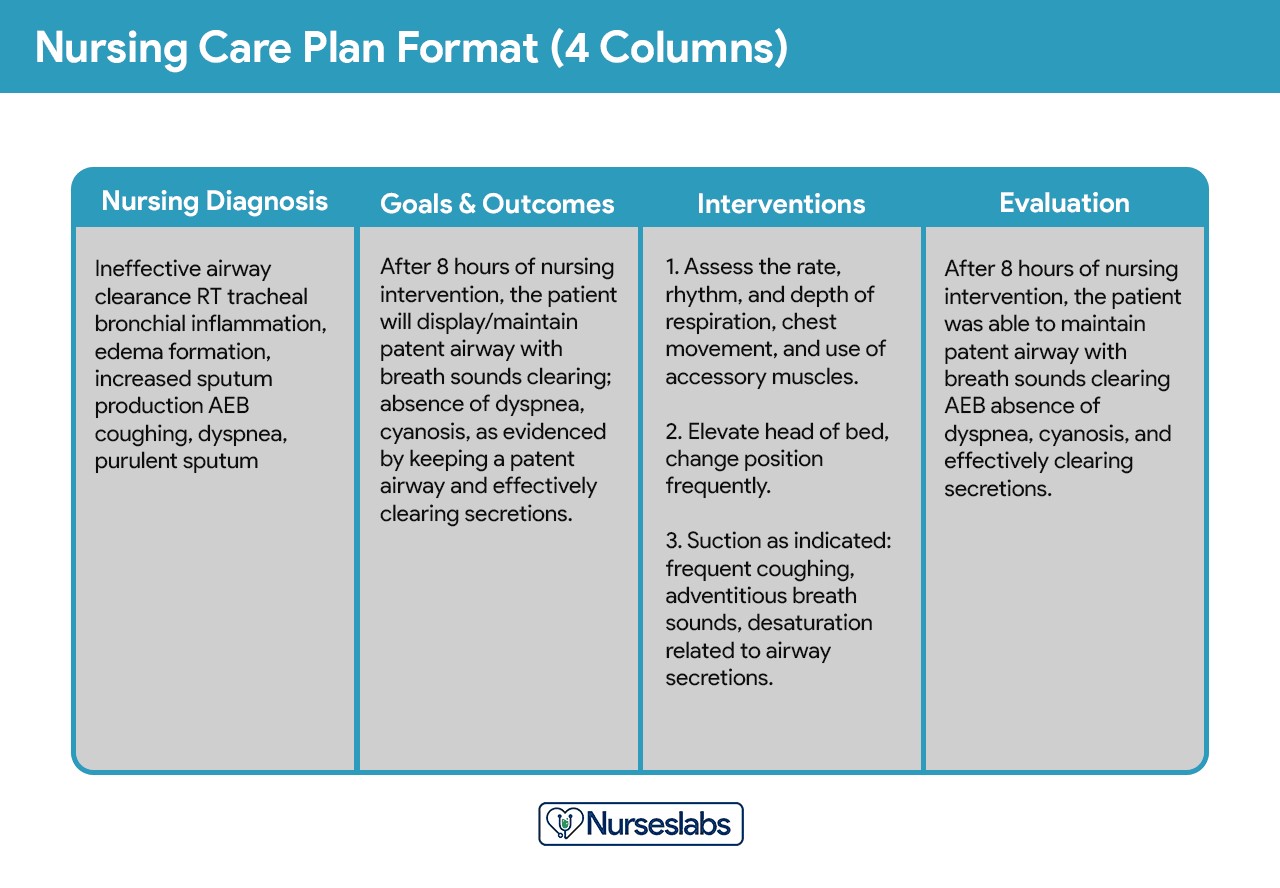
Four-Column Format: This format expands on the three-column plan by separating outcomes and evaluation into distinct columns:
- Nursing Diagnosis: The identified nursing diagnosis.
- Goals and Outcomes: Desired patient goals and expected outcomes.
- Interventions: Nursing actions to achieve outcomes.
- Evaluation: Assessment of outcome achievement.
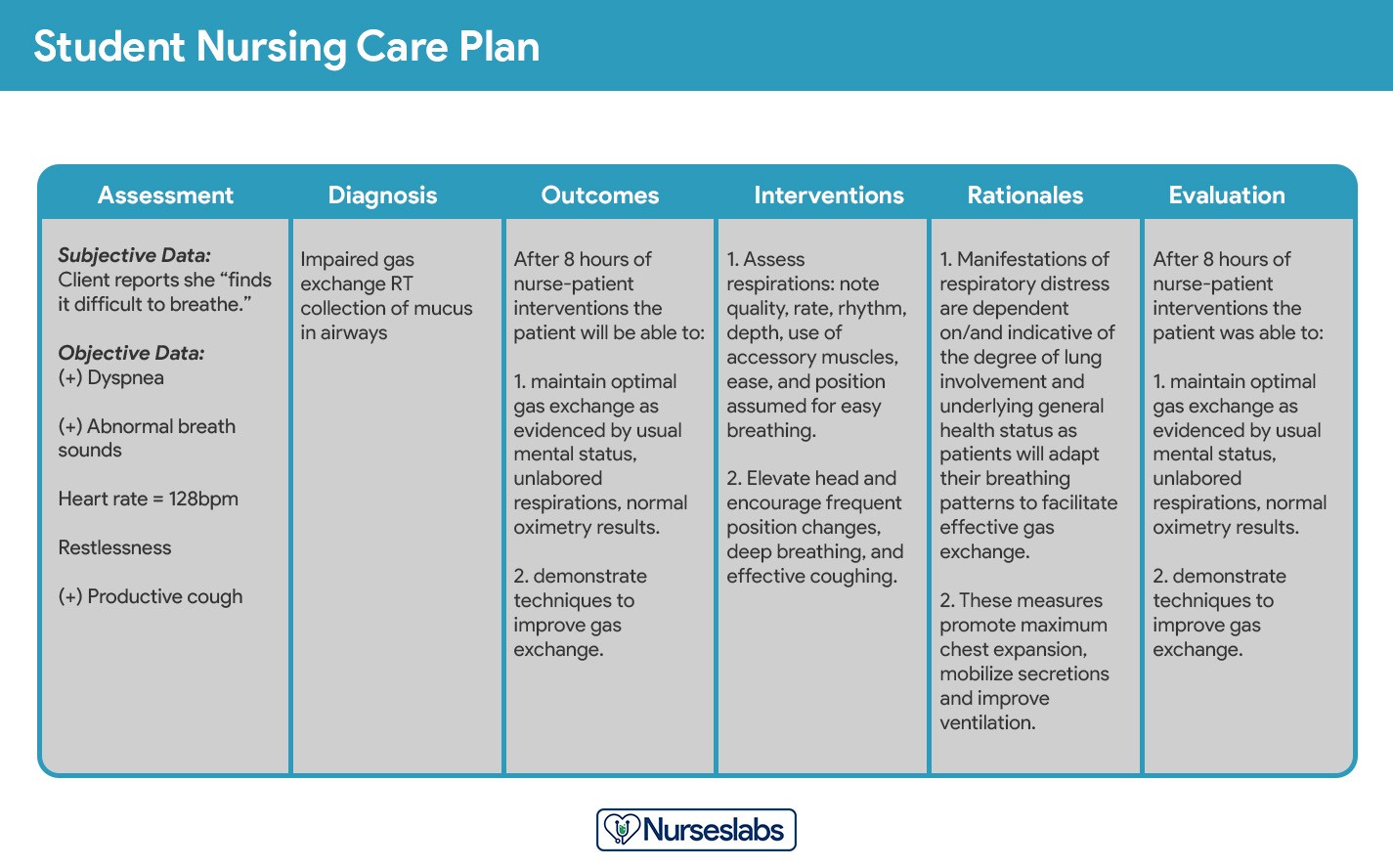
Student Care Plans: Student care plans are generally more detailed and comprehensive than those used by practicing nurses. They serve as a learning tool and often include an additional column for “Rationales” or “Scientific Explanation” after the nursing interventions. These plans are frequently handwritten and emphasize the underlying scientific principles guiding nursing actions.
Downloadable Templates: For practical use, printable nursing care plan templates and formats are readily available, offering customizable structures for various clinical settings.
Download: Printable Nursing Care Plan Templates and Formats
Step-by-Step Guide to Writing a Nursing Care Plan
Developing a comprehensive nursing care plan involves a systematic, multi-step process:
Step 1: Patient Data Collection and Assessment
The initial step in creating a nursing care plan is to establish a comprehensive patient database through thorough assessment and data collection. This involves employing various techniques such as:
- Physical Assessment: A systematic examination of the patient’s body systems.
- Health History: Gathering information about the patient’s past and present health status, including medical history, surgeries, allergies, and medications.
- Patient Interview: Direct communication with the patient to obtain subjective data about their symptoms, concerns, and perceptions.
- Medical Records Review: Examination of existing medical documentation for relevant health information.
- Diagnostic Studies: Reviewing results from laboratory tests, imaging, and other diagnostic procedures.
The patient database encompasses all collected health information. This step is crucial for identifying related or risk factors and defining characteristics that will inform the nursing diagnosis. Many healthcare facilities or nursing schools have specific assessment formats to guide this process.
Critical thinking is paramount in patient assessment, requiring the integration of knowledge from various sciences and professional guidelines to inform clinical judgments. This process is essential for effective clinical decision-making and aims to accurately identify patients’ healthcare needs within a supportive and information-rich environment.
Step 2: Data Analysis and Organization
Once patient data is collected, the next step is to analyze, cluster, and organize this information. This involves:
- Identifying Patterns: Recognizing significant cues and trends in the data.
- Clustering Data: Grouping related cues together to identify potential health problems.
- Analyzing Data: Interpreting the clustered data to determine the patient’s health status and needs.
This organized data forms the basis for formulating nursing diagnoses, setting priorities, and defining desired outcomes.
Step 3: Formulating Nursing Diagnoses
Nursing diagnoses are standardized statements that describe a patient’s health problems that nurses can legally and independently treat. They are distinct from medical diagnoses, which describe diseases or pathologies that physicians treat. Nursing diagnoses focus on the patient’s responses to health conditions or life processes.
Formulating accurate nursing diagnoses is a cornerstone of effective care planning. They provide a uniform language for identifying and addressing specific patient needs and responses to actual or potential health problems. Nursing diagnoses guide the selection of nursing interventions and expected outcomes.
For a detailed guide and list of nursing diagnoses, refer to resources such as: Nursing Diagnosis (NDx): Complete Guide and List.
Step 4: Setting Priorities
Setting priorities involves ranking nursing diagnoses in order of importance. This crucial step ensures that the most critical patient needs are addressed first. Prioritization is a collaborative process between the nurse and the patient, involving discussions to determine which problems require immediate attention.
Diagnoses can be categorized as high, medium, or low priority. Life-threatening problems or those that pose an immediate risk to patient well-being are assigned high priority.
Maslow’s Hierarchy of Needs is a useful framework for prioritizing nursing diagnoses. This theory, developed by Abraham Maslow in 1943, organizes human needs into a hierarchy, with basic physiological needs at the base and self-actualization at the peak. According to Maslow, lower-level needs must be met before higher-level needs can be addressed.
Maslow’s Hierarchy of Needs and Nursing Priorities:
-
Physiological Needs (Highest Priority): These are fundamental survival needs, including:
- ABC’s: Airway, Breathing, Circulation – ensuring adequate oxygenation and cardiovascular function.
- Nutrition: Adequate fluid and food intake.
- Elimination: Bowel and bladder function.
- Rest and Sleep: Sufficient rest to promote healing and well-being.
- Shelter and Temperature Regulation: Maintaining a safe and comfortable environment.
- Example Nursing Diagnoses: Ineffective Airway Clearance, Impaired Gas Exchange, Deficient Fluid Volume, Imbalanced Nutrition: Less Than Body Requirements, Impaired Urinary Elimination, Disturbed Sleep Pattern.
-
Safety and Security Needs: Focus on physical and emotional safety:
- Injury Prevention: Preventing falls, infections, and other injuries.
- Security and Trust: Establishing a therapeutic relationship and safe environment.
- Patient Education: Educating patients on safety measures and risk factors.
- Example Nursing Diagnoses: Risk for Falls, Risk for Infection, Risk for Injury, Anxiety, Fear, Deficient Knowledge.
-
Love and Belonging Needs: Addressing social and emotional connection:
- Supportive Relationships: Fostering positive relationships with family and healthcare team.
- Social Interaction: Preventing social isolation and promoting engagement.
- Therapeutic Communication: Using active listening and empathy.
- Example Nursing Diagnoses: Social Isolation, Loneliness, Impaired Social Interaction, Risk for Loneliness.
-
Self-Esteem Needs: Promoting feelings of self-worth and accomplishment:
- Acceptance and Recognition: Fostering a sense of value and respect.
- Personal Achievement: Supporting patient goals and celebrating progress.
- Body Image: Addressing concerns related to physical appearance and self-perception.
- Example Nursing Diagnoses: Disturbed Body Image, Chronic Low Self-Esteem, Situational Low Self-Esteem, Powerlessness.
-
Self-Actualization Needs (Lowest Priority in Acute Care): Reaching one’s full potential:
- Spiritual Growth: Supporting spiritual well-being and meaning-making.
- Personal Growth: Facilitating opportunities for learning and self-discovery.
- Empowerment: Encouraging patient autonomy and decision-making.
- Example Nursing Diagnoses: Readiness for Enhanced Spiritual Well-being, Hopelessness.
Patient values, beliefs, available resources, and the urgency of the health problem are also important factors to consider when setting priorities. Involving the patient in this process enhances their cooperation and commitment to the care plan.
Step 5: Establishing Patient Goals and Desired Outcomes
Once priorities are established, the nurse and patient collaboratively set goals for each nursing diagnosis. Goals or desired outcomes describe the intended changes in patient health status that the nurse aims to achieve through nursing interventions. Goals serve several key functions:
- Guide Intervention Planning: They provide direction for selecting appropriate nursing interventions.
- Evaluate Patient Progress: They serve as measurable criteria for assessing patient improvement.
- Determine Problem Resolution: They help determine when a health problem has been resolved.
- Motivate Patient and Nurse: They provide a sense of accomplishment and progress.
Goals should be SMART:
- Specific: Clearly defined and focused.
- Measurable: Quantifiable and able to be tracked.
- Attainable: Realistic and achievable for the patient.
- Relevant: Meaningful and important to the patient’s needs.
- Time-bound: With a defined timeframe for achievement.
Examples of SMART Goals:
- Nursing Diagnosis: Acute Pain related to surgical incision as evidenced by patient rating pain 7/10 and guarding incision site.
- SMART Goal: Patient will report pain level of 3/10 or less within 1 hour after pain medication administration by [Date].
- Nursing Diagnosis: Impaired Physical Mobility related to weakness as evidenced by inability to ambulate independently.
- SMART Goal: Patient will ambulate 50 feet with the assistance of one person by discharge.
REEPIG Standards for High-Quality Care Plans:
- Realistic: Feasible given available resources and patient condition.
- Explicitly Stated: Clear and unambiguous, leaving no room for misinterpretation.
- Evidence-Based: Supported by research and best practices.
- Prioritized: Addresses the most urgent needs first.
- Involve: Incorporates patient and interdisciplinary team input.
- Goal-Centered: Directly related to achieving desired patient outcomes.
Goals can be categorized as short-term or long-term:
- Short-Term Goals: Achievable within hours to days, common in acute care settings focused on immediate needs.
- Long-Term Goals: Achievable over weeks to months, relevant for chronic conditions or long-term care settings.
- Discharge Planning Goals: Long-term goals focused on continued recovery and problem resolution after discharge, often involving referrals to home health or therapy services.
Components of Goal Statements:
Goal statements typically include four components:
- Subject: Usually the patient (often implied).
- Verb: Action the patient will perform (e.g., “will verbalize,” “will demonstrate,” “will maintain”).
- Conditions/Modifiers: Circumstances under which the behavior will occur (e.g., “after teaching,” “using crutches”).
- Criterion of Performance: Standard for evaluating performance (e.g., “pain level of 3/10,” “ambulate 50 feet”).
Tips for Writing Effective Goals and Outcomes:
- Focus on patient responses, not nurse activities. Begin with “Patient will…”
- Focus on what the patient will do, not what the nurse hopes to achieve.
- Use observable and measurable terms. Avoid vague language.
- Ensure outcomes are realistic given patient resources and time frame.
- Align goals with therapies from other healthcare professionals.
- Each goal should relate to only one nursing diagnosis for clear evaluation.
- Ensure goals are important and valued by the patient for cooperation.
Step 6: Selecting Nursing Interventions
Nursing interventions are specific actions that nurses perform to help patients achieve their goals and desired outcomes. Interventions should be directed at eliminating or reducing the underlying cause (etiology) of the nursing diagnosis. For risk diagnoses, interventions focus on reducing risk factors.
Nursing interventions are identified and written during the planning phase of the nursing process but are implemented during the implementation phase.
Types of Nursing Interventions:
Nursing interventions can be categorized as:
-
Independent Interventions: Actions nurses are licensed to initiate based on their own judgment and skills. Examples include:
- Ongoing assessment and monitoring.
- Providing emotional support and counseling.
- Patient education and health teaching.
- Comfort measures and physical care.
- Making referrals to other healthcare providers.
-
Dependent Interventions: Actions carried out under a physician’s order or supervision. Examples include:
- Administering medications (oral, IV, IM, subcutaneous).
- Providing intravenous fluid therapy.
- Performing diagnostic tests and procedures.
- Implementing prescribed treatments (wound care, respiratory therapy).
- Managing diet and activity orders.
-
Collaborative Interventions: Actions carried out in coordination with other members of the healthcare team, such as physicians, therapists, dietitians, and social workers. These are developed through interdisciplinary consultation to leverage diverse expertise.
Criteria for Effective Nursing Interventions:
Nursing interventions should be:
- Safe and Appropriate: Suitable for the patient’s age, health condition, and overall status.
- Achievable and Realistic: Feasible given available resources, time, and patient capabilities.
- Congruent with Patient Values: Respectful of the patient’s cultural, spiritual, and personal beliefs.
- Compatible with Other Therapies: Integrated and coordinated with other treatments the patient is receiving.
- Evidence-Based: Grounded in nursing knowledge, research, and relevant scientific principles.
Tips for Writing Nursing Interventions:
- Date and Sign: Document the date the plan is written and sign it for accountability and to facilitate review and updates.
- Be Specific and Clear: Start with an action verb and include qualifiers specifying how, when, where, time, frequency, and amount. Examples:
- “Administer pain medication (morphine 2mg IV) every 4 hours PRN for pain level > 4/10.”
- “Educate patient on proper use of incentive spirometer every shift.”
- “Assess wound dressing for drainage and signs of infection every 8 hours.”
- Use Accepted Abbreviations: Only use abbreviations approved by the healthcare institution to ensure clarity and avoid errors.
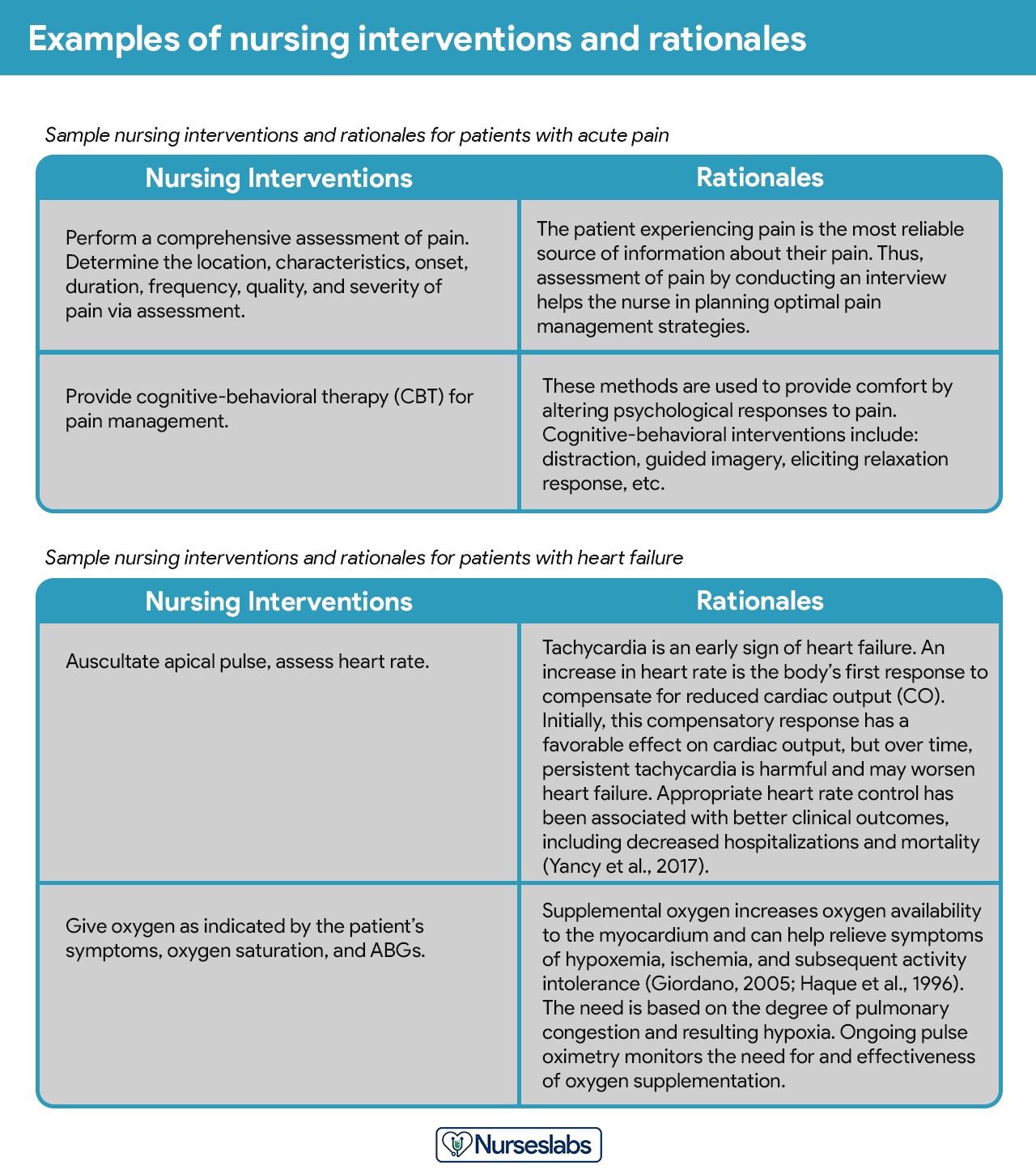
Step 7: Providing Rationales for Interventions
Rationales are scientific explanations that justify why a particular nursing intervention was selected. They explain the underlying physiological, psychological, and sociological principles that support the effectiveness of the intervention.
Rationales are particularly important in student care plans as they help students connect scientific knowledge to clinical practice and understand the reasoning behind nursing actions. While not always included in routine care plans for practicing nurses, rationales are essential for learning and demonstrating critical thinking.
Step 8: Evaluation of the Nursing Care Plan
Evaluation is a systematic and ongoing process to determine the patient’s progress toward achieving the established goals and the effectiveness of the nursing care plan. It is a crucial phase of the nursing process that involves:
- Data Collection: Gathering data related to goal achievement.
- Comparing Data to Outcomes: Assessing the extent to which the patient has met the desired outcomes.
- Analyzing Findings: Determining the effectiveness of interventions and the overall care plan.
- Modifying Care Plan (if needed): Adjusting the care plan based on evaluation findings, which may involve continuing, modifying, or terminating interventions.
Evaluation is continuous and iterative. It informs decisions about whether to:
- Continue the Care Plan: If the patient is making satisfactory progress and goals are being met.
- Modify the Care Plan: If progress is slow, goals are not being met, or the patient’s condition changes. Modifications may involve revising nursing diagnoses, goals, or interventions.
- Terminate the Care Plan: If the goals have been fully achieved and the patient’s health problem is resolved.
Step 9: Documenting the Nursing Care Plan
The final step is to document the patient’s care plan according to institutional policy. The care plan becomes part of the patient’s permanent medical record, ensuring continuity of care and providing a reference for all healthcare providers.
Different healthcare facilities and nursing programs may have specific formats for documenting care plans. Most formats are designed to guide nurses systematically through the steps of the nursing process.
Nursing Care Plan Examples and List
This section provides a categorized list of sample nursing care plans and nursing diagnoses for various health conditions. These examples serve as templates and guides for developing individualized care plans.
(The original article’s extensive list of care plans by category is included here for completeness, maintaining the original structure and links.)
Basic Nursing and General Care Plans
| Basic Nursing & General Care Plans |
|---|
| Acute Confusion (Delirium) and Altered Mental Status |
| Acute Pain and Pain Management |
| Activity Intolerance and Generalized Weakness |
| Cancer (Oncology Nursing) |
| Caregiver Role Strain and Family Caregiver Support Systems |
| Chronic Confusion (Dementia) |
| End-of-Life Care (Hospice Care or Palliative) |
| Fall Risk and Fall Prevention |
| Fatigue and Lethargy |
| Geriatric Nursing (Older Adult) |
| Grieving and Loss |
| Hypothermia and Cold Injuries |
| Hyperthermia (Fever) |
| Impaired Swallowing (Dysphagia) |
| Insomnia and Sleep Deprivation |
| Prolonged Bed Rest |
| Risk for Injury and Patient Safety |
| Self-Care and Activities of Daily Living (ADLs) |
| Surgery (Perioperative Client) |
| Systemic Lupus Erythematosus |
| Total Parenteral Nutrition |




Surgery and Perioperative Care Plans
| Surgery and Perioperative Care Plans |
|---|
| Amputation |
| Appendectomy |
| Cholecystectomy |
| Fracture UPDATED! |
| Hemorrhoids |
| Hysterectomy |
| Ileostomy & Colostomy |
| Laminectomy (Disc Surgery) |
| Mastectomy |
| Subtotal Gastrectomy |
| Surgery (Perioperative Client) |
| Thyroidectomy |
| Total Joint (Knee, Hip) Replacement |
Cardiac Care Plans
| Cardiac Care Plans |
|---|
| Angina Pectoris (Coronary Artery Disease) |
| Cardiac Arrhythmia (Digitalis Toxicity) |
| Cardiac Catheterization |
| Cardiogenic Shock |
| Congenital Heart Disease |
| Decreased Cardiac Output & Cardiac Support |
| Heart Failure UPDATED! |
| Hypertension UPDATED! |
| Hypovolemic Shock |
| Impaired Tissue Perfusion & Ischemia |
| Myocardial Infarction |
| Pacemaker Therapy |
Endocrine and Metabolic Care Plans
| Endocrine and Metabolic Care Plans |
|---|
| Addison’s Disease |
| Cushing’s Disease |
| Diabetes Mellitus (Type 1, Type 2) UPDATED! |
| Diabetic Ketoacidosis (DKA) and Hyperglycemic Hyperosmolar Nonketotic Syndrome (HHNS) |
| Eating Disorders: Anorexia & Bulimia Nervosa |
| Fluid Volume Deficit (Dehydration & Hypovolemia) |
| Fluid Volume Excess (Hypervolemia) |
| Gestational Diabetes Mellitus |
| Hyperthyroidism |
| Hypothyroidism |
| Imbalanced Nutrition (Malnutrition) |
| Obesity & Overweight |
| Thyroidectomy |
| Unstable Blood Glucose Levels (Hyperglycemia & Hypoglycemia) |
| Acid-Base Imbalances |
|---|
| Metabolic Acidosis |
| Metabolic Alkalosis |
| Respiratory Acidosis |
| Respiratory Alkalosis |
| Electrolyte Imbalances |
|---|
| Calcium (Ca) Imbalances: Hypercalcemia and Hypocalcemia |
| Magnesium (Mg) Imbalances: Hypermagnesemia and Hypomagnesemia |
| Potassium (K) Imbalances: Hyperkalemia and Hypokalemia |
| Sodium (Na) Imbalances: Hypernatremia and Hyponatremia |
Gastrointestinal Care Plans
| Gastrointestinal Care Plans |
|---|
| Appendectomy |
| Bowel Incontinence (Fecal Incontinence) |
| Cholecystectomy |
| Constipation |
| Diarrhea Nursing Care Plan and Management |
| Cholecystitis and Cholelithiasis |
| Gastroenteritis |
| Gastroesophageal Reflux Disease (GERD) |
| Hemorrhoids |
| Hepatitis |
| Ileostomy & Colostomy |
| Inflammatory Bowel Disease (IBD) |
| Intussusception |
| Liver Cirrhosis |
| Nausea & Vomiting |
| Pancreatitis |
| Peritonitis |
| Peptic Ulcer Disease |
| Subtotal Gastrectomy |
| Umbilical and Inguinal Hernia |
Hematologic and Lymphatic Care Plans
| Hematologic & Lymphatic Care Plans |
|---|
| Anaphylactic Shock |
| Anemia UPDATED! |
| Aortic Aneurysm |
| Bleeding Risk & Hemophilia |
| Deep Vein Thrombosis |
| Disseminated Intravascular Coagulation |
| Hemophilia |
| Kawasaki Disease |
| Leukemia |
| Lymphoma |
| Sepsis and Septicemia |
| Sickle Cell Anemia Crisis |
Infectious Diseases Care Plans
| Infectious Diseases Care Plans |
|---|
| Acquired Immunodeficiency Syndrome (AIDS) (HIV Positive) |
| Acute Rheumatic Fever |
| Dengue Hemorrhagic Fever |
| Herpes Zoster (Shingles) |
| Influenza (Flu) |
| Pulmonary Tuberculosis |
| Risk for Infection & Infection Control |
Integumentary Care Plans
| Integumentary Care Plans |
|---|
| Burn Injury |
| Dermatitis |
| Herpes Zoster (Shingles) |
| Pressure Ulcer (Bedsores) |
| Wound Care and Skin/Tissue Integrity |
Maternal and Newborn Care Plans
| Maternal and Newborn Care Plans |
|---|
| Abortion (Termination of Pregnancy) |
| Cervical Insufficiency (Premature Dilation of the Cervix) |
| Cesarean Birth |
| Cleft Palate and Cleft Lip |
| Gestational Diabetes Mellitus |
| Hyperbilirubinemia (Jaundice) |
| Labor Stages, Induced, Augmented, Dysfunctional, Precipitous Labor |
| Neonatal Sepsis |
| Perinatal Loss (Miscarriage, Stillbirth) |
| Placental Abruption |
| Placenta Previa |
| Postpartum Hemorrhage |
| Postpartum Thrombophlebitis |
| Prenatal Hemorrhage |
| Preeclampsia and Gestational Hypertension |
| Prenatal Infection |
| Preterm Labor |
| Puerperal & Postpartum Infections |
| Substance (Alcohol and Drug) Abuse in Pregnancy |
Mental Health and Psychiatric Care Plans
| Mental Health and Psychiatric Care Plans |
|---|
| Alcohol Withdrawal |
| Anxiety & Fear |
| Anxiety and Panic Disorders |
| Bipolar Disorders |
| Body Image Disturbance & Self-Esteem |
| Impaired Thought Processes & Cognitive Impairment |
| Major Depression |
| Personality Disorders |
| Schizophrenia |
| Sexual Assault |
| Substance Dependence and Abuse |
| Suicide Behaviors |
Musculoskeletal Care Plans
| Musculoskeletal Care Plans |
|---|
| Amputation |
| Congenital Hip Dysplasia |
| Fracture UPDATED! |
| Impaired Physical Mobility & Immobility |
| Juvenile Rheumatoid Arthritis |
| Laminectomy (Disc Surgery) |
| Osteoarthritis |
| Osteogenic Sarcoma (Osteosarcoma) |
| Osteoporosis |
| Rheumatoid Arthritis |
| Scoliosis |
| Spinal Cord Injury |
| Total Joint (Knee, Hip) Replacement |
Neurological Care Plans
| Neurological Care Plans |
|---|
| Alzheimer’s Disease UPDATED! |
| Brain Tumor |
| Cerebral Palsy |
| Cerebrovascular Accident (Stroke) UPDATED! |
| Guillain-Barre Syndrome |
| Meningitis |
| Multiple Sclerosis |
| Parkinson’s Disease |
| Seizure Disorder |
| Spinal Cord Injury |
Ophthalmic Care Plans
| Ophthalmic Care Plans |
|---|
| Cataracts |
| Glaucoma |
| Macular Degeneration |
Pediatric Nursing Care Plans
| Pediatric Nursing Care Plans |
|---|
| Child Abuse |
| Cleft Lip and Cleft Palate |
| Dying Child |
| Febrile Seizure |
| Hospitalized Child |
| Hydrocephalus |
| Otitis Media |
| Spina Bifida |
| Tonsillitis and Adenoiditis |
Reproductive Care Plans
| Reproductive Care Plans |
|---|
| Cryptorchidism (Undescended Testes) |
| Hysterectomy |
| Hypospadias and Epispadias |
| Mastectomy |
| Menopause |
| Prostatectomy |
Respiratory Care Plans
| Respiratory Care Plans |
|---|
| Airway Clearance Therapy & Coughing |
| Apnea |
| Asthma UPDATED! |
| Aspiration Risk & Aspiration Pneumonia |
| Bronchiolitis UPDATED! |
| Bronchopulmonary Dysplasia (BPD) UPDATED! |
| Chronic Obstructive Pulmonary Disease (COPD) UPDATED! |
| Croup Syndrome |
| Cystic Fibrosis UPDATED! |
| Epiglottitis |
| Hemothorax and Pneumothorax UPDATED! |
| Ineffective Breathing Pattern (Dyspnea) |
| Impairment of Gas Exchange |
| Influenza (Flu) UPDATED! |
| Lung Cancer UPDATED! |
| Mechanical Ventilation |
| Near-Drowning |
| Pleural Effusion |
| Pneumonia |
| Pulmonary Embolism |
| Pulmonary Tuberculosis |
| Tracheostomy |
Urinary Care Plans
| Urinary Care Plans |
|---|
| Acute Glomerulonephritis |
| Acute Renal Failure |
| Benign Prostatic Hyperplasia (BPH) |
| Chronic Renal Failure |
| Hemodialysis |
| Nephrotic Syndrome |
| Peritoneal Dialysis |
| Urolithiasis (Renal Calculi) |
| Urinary Elimination (Urinary Incontinence & Urinary Retention) |
| Urinary Tract Infection |
| Vesicoureteral Reflux (VUR) |
| Wilms Tumor (Nephroblastoma) |
Recommended Resources for Nursing Care Planning
To further enhance your skills in nursing care planning and nursing diagnosis, consider these recommended resources:
Disclosure: Affiliate links from Amazon are included below, which may provide a small commission at no additional cost to you. See our privacy policy for more details.
Ackley and Ladwig’s Nursing Diagnosis Handbook: An Evidence-Based Guide to Planning Care
This handbook offers a three-step system for client assessment, nursing diagnosis, and care planning, emphasizing evidence-based interventions and promoting diagnostic reasoning and critical thinking skills.
Nursing Care Plans – Nursing Diagnosis & Intervention (10th Edition)
Featuring over 200 care plans based on current evidence-based guidelines, this resource includes new content on ICNP diagnoses, LGBTQ health issues, and electrolyte and acid-base balance.
Nurse’s Pocket Guide: Diagnoses, Prioritized Interventions, and Rationales
A quick-reference guide with essential information for identifying accurate diagnoses and planning efficient patient care, including the latest nursing diagnoses and interventions for over 400 disorders.
Nursing Diagnosis Manual: Planning, Individualizing, and Documenting Client Care
This manual provides interventions for planning, individualizing, and documenting care for over 800 diseases and disorders, including clinical applications, prioritized interventions with rationales, and documentation guidelines.
This comprehensive e-book includes over 100 care plans across medical-surgical, maternity, pediatric, and psychiatric-mental health settings, focusing on interprofessional patient problems.
References and Sources
(The original article’s references and sources are listed here for completeness, maintaining the original links.)