Sarcoidosis is a systemic inflammatory disease characterized by the formation of noncaseating granulomas in various organs. While the lungs and intrathoracic lymph nodes are most commonly affected, sarcoidosis can involve virtually any organ system. Diagnosing sarcoidosis can be challenging due to its diverse clinical presentations and the need to exclude other granulomatous diseases. This article provides an up-to-date review of the sarcoidosis diagnosis criteria, focusing on the essential elements for accurate and timely identification of this complex condition.
Epidemiology and Clinical Presentation: Key Considerations for Diagnosis
Understanding the epidemiology and varied clinical manifestations of sarcoidosis is crucial for initiating the diagnostic process. Sarcoidosis incidence varies significantly across ethnicities, with African Americans exhibiting the highest rates, followed by whites, and lower rates in Asians and Hispanics. It typically presents in middle-aged adults, between 35 and 50 years old.
Clinically, sarcoidosis is highly heterogeneous. Pulmonary sarcoidosis, the most frequent form, may be asymptomatic or present with cough, dyspnea, and chest tightness. Extrapulmonary sarcoidosis can affect the skin, eyes, joints, liver, nervous system, kidneys, heart, and gastrointestinal tract, leading to a wide array of symptoms. This broad spectrum of presentations underscores the importance of a systematic diagnostic approach.
Core Sarcoidosis Diagnosis Criteria
The diagnosis of sarcoidosis is not solely based on clinical or radiological findings. Definitive sarcoidosis diagnosis requires a combination of three key criteria:
- Histopathologic Evidence of Noncaseating Granulomas: The hallmark of sarcoidosis is the presence of noncaseating granulomas, which are clusters of immune cells without central necrosis, observed in tissue biopsies.
- Compatible Clinical Presentation: The clinical signs and symptoms must align with sarcoidosis, considering the potential for multi-organ involvement.
- Exclusion of Other Causes of Granulomatous Disease: It is essential to rule out other conditions that can cause granulomatous inflammation, such as infections (tuberculosis, fungal infections), foreign body reactions, and certain autoimmune diseases.
Exceptions to the histopathologic requirement are limited to specific scenarios like stage I pulmonary sarcoidosis (bilateral hilar adenopathy) and Löfgren syndrome (erythema nodosum, arthritis, and bilateral hilar adenopathy), where clinical and radiological findings are highly suggestive in the absence of other explanations.
Site of Biopsy for Sarcoidosis Diagnosis
Histopathologic confirmation is central to sarcoidosis diagnosis. Biopsy site selection depends on accessibility and clinical presentation. Easily accessible sites include skin lesions, conjunctival nodules, superficial lymph nodes, and lacrimal glands.
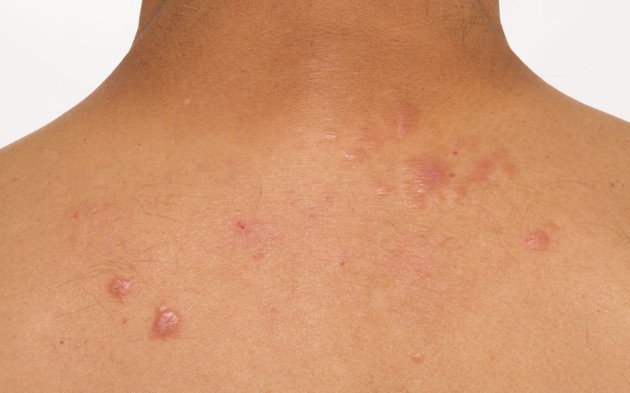 Papular sarcoidosis on the upper back, showing erythematous raised lesions, relevant for skin biopsy in sarcoidosis diagnosis.
Papular sarcoidosis on the upper back, showing erythematous raised lesions, relevant for skin biopsy in sarcoidosis diagnosis.
When superficial sites are not available or nondiagnostic, intrathoracic lymph nodes and lung parenchyma become primary targets due to their frequent involvement in sarcoidosis. Transbronchial lung biopsy (TBB) is a common procedure, with diagnostic yield improved by combining it with endobronchial biopsy. Endoscopic ultrasound-guided needle aspiration is highly effective for sampling hilar and mediastinal lymph nodes, particularly in stage I pulmonary sarcoidosis.
Histopathology of Sarcoidosis: Identifying Noncaseating Granulomas
Microscopic examination of biopsy specimens is crucial. Sarcoid granulomas are characterized as well-formed, noncaseating, consisting of epithelioid cells and multinucleated giant cells, often surrounded by lymphocytes. Special stains and cultures are necessary to exclude infectious granulomatous diseases like tuberculosis and fungal infections.
Diagnosis Criteria for Specific Organ Involvement
Diagnosing sarcoidosis in certain organs, particularly the nervous system, heart, and eyes, presents unique challenges due to biopsy inaccessibility. In these cases, diagnostic criteria incorporate clinical findings, imaging, and evidence of systemic sarcoidosis.
Neurosarcoidosis Diagnosis Criteria
Neurosarcoidosis diagnosis often relies on a combination of clinical presentation, exclusion of other diagnoses, and evidence of granulomas either in the nervous system or in extraneural tissues. The diagnostic criteria are categorized into definite, probable, and possible neurosarcoidosis:
Table 1: Diagnosis of Neurosarcoidosis
| Diagnosis | Criteria | Additional comments |
|---|---|---|
| Definite | Suggestive clinical presentation of neurosarcoidosis Plus: Positive histology of nervous system (sarcoid-type granulomas) Plus: Exclusion of other possible diagnoses | None |
| Probable | Suggestive clinical presentation of neurosarcoidosis Plus: Evidence of inflammation in central nervous system (CSF abnormalities or abnormal brain MRI) Plus: Evidence of systemic sarcoidosis (extraneural biopsy or indirect evidence like gallium scan, chest imaging, elevated ACE) Plus: Exclusion of other possible diagnoses | None |
| Possible | Suggestive clinical presentation of neurosarcoidosis with exclusion of other diseases when the criteria for definite and probable diagnosis are not met | None |
Diagnosis of definite neurosarcoidosis requires histological confirmation from nervous system tissue. Probable neurosarcoidosis relies on clinical presentation, CNS inflammation evidence, and systemic sarcoidosis evidence. Possible neurosarcoidosis is considered when clinical suspicion is high but definite or probable criteria are not fulfilled and other diagnoses are excluded.
Cardiac Sarcoidosis Diagnosis Criteria
Cardiac sarcoidosis diagnosis is critical due to its life-threatening potential. Endomyocardial biopsy has low sensitivity, making cardiac imaging essential. Cardiac MRI with gadolinium and FDG-PET are valuable for detecting myocardial involvement.
Diagnostic Pathways for Cardiac Sarcoidosis:
- Histopathologic Pathway: Noncaseating granulomas in myocardial tissue.
- Clinical Pathway: Histopathologic diagnosis of extracardiac sarcoidosis plus at least one of the following, after excluding other causes:
- Glucocorticoid-responsive cardiomyopathy or heart block
- Unexplained reduced LVEF (<40%)
- Unexplained sustained ventricular tachycardia
- Mobitz type II second-degree AV block or third-degree AV block
- Patchy FDG uptake on cardiac PET consistent with sarcoidosis
- Late gadolinium enhancement on cardiac MRI consistent with sarcoidosis
- Positive gallium uptake consistent with sarcoidosis
These criteria, established by the Heart Rhythm Society, emphasize the combination of extracardiac sarcoidosis confirmation with cardiac-specific findings from imaging and clinical response to treatment.
Ocular Sarcoidosis Diagnosis Criteria
Diagnosing ocular sarcoidosis (sarcoid uveitis) relies on clinical findings and evidence of sarcoidosis elsewhere. The International Workshop on Ocular Sarcoidosis proposed diagnostic categories:
Diagnostic Categories for Ocular Sarcoidosis:
- Definite Ocular Sarcoidosis: Compatible uveitis in a patient with biopsy-proven sarcoidosis of extraocular organ(s).
- Presumed Ocular Sarcoidosis: Compatible uveitis in a patient with classic bilateral hilar adenopathy on chest imaging.
- Probable Ocular Sarcoidosis: In the absence of biopsy or classic bilateral hilar adenopathy, at least 3 suggestive intraocular signs and 2 supportive laboratory investigations (See Table 2).
- Possible Ocular Sarcoidosis: Negative lung biopsy, but at least 4 suggestive intraocular signs and 2 supportive laboratory investigations (See Table 2).
Table 2: Clinical Signs and Laboratory Investigations Suggestive of Ocular Sarcoidosis
| Suggestive ocular signs Suggestive intraocular signs:
- Large and/or small keratic precipitates and/or iris nodules (Koeppe/Busacca nodules).
- Trabecular meshwork nodules and/or tent-shaped peripheral anterior synechiae.
- Snowballs/string of pearls vitreous opacities.
- Multiple chorioretinal peripheral lesions.
- Nodular/segmental periphlebitis and/or macroaneurysm in an inflamed eye.
- Optic disc nodules/granulomas and/or solitary choroidal nodule.
- Bilaterality (may be subclinical).
Supportive laboratory investigations:
- Negative tuberculin test (in BCG-vaccinated patients or those with prior positive tests).
- Elevated serum ACE and/or lysozyme levels.
- Bilateral hilar lymphadenopathy on chest X-ray.
- Abnormal liver biochemistry (elevation of ≥2 of ALP, GGT, ALT, AST, LDH).
- Abnormal chest CT compatible with pulmonary sarcoidosis (if chest X-ray is negative).
These criteria aim to standardize ocular sarcoidosis diagnosis, recognizing that intraocular signs of granulomatous uveitis are not universally present, and diagnosis can be made based on strong extraocular evidence.
Additional Diagnostic Tests and Considerations
While histopathology and clinical criteria are paramount, additional tests can support sarcoidosis diagnosis and assess disease extent. Serum angiotensin-converting enzyme (ACE) levels, although not highly sensitive or specific, can be elevated in sarcoidosis. However, ACE levels should not be used as a primary diagnostic tool.
Imaging modalities like chest radiography, CT scans, cardiac MRI, and FDG-PET play crucial roles in assessing organ involvement and disease activity. Bronchoscopy with bronchoalveolar lavage (BAL) may also be used to exclude alternative diagnoses.
Conclusion: Navigating Sarcoidosis Diagnosis
Sarcoidosis diagnosis is a multifaceted process requiring careful integration of clinical presentation, histopathology, and exclusion of other granulomatous diseases. Up-to-date diagnostic criteria, particularly for neurosarcoidosis, cardiac sarcoidosis, and ocular sarcoidosis, are essential for accurate and timely diagnosis. By adhering to these criteria and utilizing appropriate diagnostic tools, clinicians can effectively navigate the complexities of sarcoidosis and ensure optimal patient management.
References
(References are the same as the original article and are not repeated here for brevity, but would be included in a full article.)
