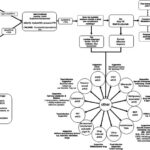
Activity intolerance is a nursing diagnosis defined as insufficient physiological or psychological energy to endure or complete required or desired daily activities. This condition affects a diverse patient population, from children to the elderly. Individuals with a history of reduced activity or previous intolerance are at a higher risk of recurrence. Numerous underlying conditions can predispose a person to activity intolerance.
Note: It’s important to recognize that the nursing diagnosis “Activity Intolerance” has been updated to “Decreased Activity Tolerance” by the NANDA International Diagnosis Development Committee (DDC). While the terminology is evolving, this article will continue using “Activity Intolerance” for broader understanding and until the updated term is widely adopted in practice.
Common Causes of Activity Intolerance
Activity intolerance can stem from various underlying health issues. Some of the common causes include:
- Respiratory Conditions: Conditions like COPD impair oxygen exchange, leading to reduced energy levels and activity intolerance.
- Anemia: Anemia reduces the oxygen-carrying capacity of the blood, causing fatigue and decreased tolerance for activity.
- Malnutrition: Inadequate nutrition or malnutrition deprives the body of essential energy sources, resulting in weakness and activity intolerance.
- Depression: Depression can significantly impact energy levels and motivation, contributing to reduced activity and fatigue.
- Pain: Both acute pain and chronic pain can limit movement and activity due to discomfort and functional limitations.
- Decreased Mobility: Reduced mobility following surgery or prolonged illness directly impacts physical activity levels and can lead to activity intolerance.
- Inadequate Sleep: Insufficient or poor quality sleep can result in fatigue and decreased energy, affecting the ability to perform daily activities.
- Cognitive Impairment: Cognitive deficits can impact a person’s ability to plan, initiate, and safely engage in physical activities.
- Generalized Weakness: Overall muscle weakness, regardless of the cause, can significantly limit physical capacity and lead to activity intolerance.
Recognizing Signs and Symptoms of Activity Intolerance
Identifying activity intolerance involves recognizing both subjective reports from the patient and objective assessments made by the nurse. These signs and symptoms can be categorized as follows:
Subjective Data (Patient Reports)
- Patient-reported weakness or decreased activity levels: Patients may express feeling weaker than usual or report a noticeable reduction in their typical activity levels.
- Shortness of breath with exertion: Dyspnea or breathlessness during activity is a common subjective symptom.
- Fatigue: Patients often describe experiencing fatigue, feeling unusually tired or exhausted even after minimal exertion.
- Exertional discomfort: Discomfort, pain, or other unpleasant sensations experienced during or after physical activity are significant subjective indicators.
Objective Data (Nurse Assessments)
- Abnormal blood pressure and heart rate response to activity: An excessive increase or decrease in blood pressure or heart rate during or after activity is an objective sign of intolerance.
- Changes in ECG: Electrocardiogram (ECG) changes during activity can indicate cardiac stress and intolerance.
- Signs of pain with movement or activity: Observable signs of pain, such as grimacing or guarding, during activity are objective indicators.
- Difficulty engaging in activity: Observable struggle or inability to perform activities as expected for their age and condition.
- Increased oxygen demand: Clinical signs like increased respiratory rate, use of accessory muscles, or decreased oxygen saturation during activity indicate increased oxygen demand and potential intolerance.
Expected Outcomes and Nursing Goals for Activity Intolerance
Setting clear and measurable goals is crucial in managing activity intolerance. Nursing care planning focuses on achieving the following expected outcomes:
- Normalization of vital signs with activity: The patient’s blood pressure, heart rate, and respiratory rate will remain within acceptable limits during and after activity.
- Active participation in physical and occupational therapy: The patient will be able to engage in prescribed PT and OT sessions to improve strength and endurance.
- Return to baseline activity level: The patient will gradually regain their pre-illness or baseline level of physical activity and function.
- Independent completion of Activities of Daily Living (ADLs): The patient will be able to perform personal care tasks like bathing, dressing, and eating independently or with minimal assistance.
- Stable heart rhythm throughout activity: The patient’s cardiac rhythm will remain regular and stable during physical exertion.
- Understanding and implementation of gradual activity increase: The patient will verbalize understanding of the importance of gradually increasing activity levels and demonstrate the ability to do so safely at home.
Nursing Assessment for Activity Intolerance
A thorough nursing assessment is the foundation for developing effective interventions. Key assessment areas include:
1. Current Activity Level and Tolerance: Assess the patient’s current daily activity patterns and their ability to perform these activities. This establishes a baseline and helps in creating a personalized activity plan and tracking progress.
2. Vital Signs Monitoring: Obtain baseline vital signs (blood pressure, heart rate, respiratory rate, oxygen saturation). Regular monitoring helps detect fluctuations and responses to activity.
3. Identify Underlying Causes: Investigate potential underlying medical conditions, medications, or lifestyle factors contributing to activity intolerance. Addressing the root cause is essential for effective management.
4. Medication Review: Review the patient’s medication list, as some medications can cause side effects like fatigue and weakness, contributing to activity intolerance. Consider timing adjustments or alternative medications if appropriate, in consultation with the physician.
5. Nutritional Status Evaluation: Assess the patient’s nutritional intake and status. Adequate nutrition is vital for energy production and physical function.
6. Need for Assistive Devices: Determine if the patient requires assistive devices (walkers, canes, etc.) to improve mobility and activity levels. Providing appropriate aids can significantly enhance activity tolerance.
7. Skin Integrity Assessment: Regularly assess skin integrity, especially in patients with limited mobility, as they are at increased risk for pressure ulcers.
Nursing Interventions to Improve Activity Tolerance
Nursing interventions are crucial for improving a patient’s activity tolerance and promoting recovery. Effective strategies include:
1. Range of Motion (ROM) Exercises: For bed-rest patients, initiate ROM exercises to maintain joint mobility and muscle function. Gradually increase exercise intensity as tolerated.
2. Vital Signs Monitoring During Activity: Continuously monitor vital signs before, during, and after activity to ensure hemodynamic stability and identify signs of intolerance.
3. Supplemental Oxygen Therapy: Provide supplemental oxygen as needed to maintain adequate oxygen saturation levels, especially during activity-induced shortness of breath.
4. Frequent Position Changes: Implement frequent repositioning for patients on bed rest or chair rest to prevent pressure ulcers and promote respiratory function.
5. Nutritional Support: Provide appropriate nutritional supplements or dietary modifications to address malnutrition and ensure adequate energy intake for activity.
6. Assistive Devices Provision: Ensure patients have access to and are properly using necessary assistive devices to facilitate mobility and activity.
7. Pain Management: Address pain effectively, as pain can significantly limit activity. Administer pain medication before activities as needed.
8. Physical and Occupational Therapy Consult: Collaborate with physical and occupational therapists to develop structured therapy schedules and progressive exercise plans to build endurance.
9. Emotional Support and Encouragement: Provide emotional support and encouragement to patients who may feel discouraged by their activity limitations. Foster a positive attitude towards gradual activity increases.
10. Patient Education on Safe Activity Increase at Home: Educate patients and caregivers on strategies for safely and gradually increasing activity levels at home to promote independence and long-term improvement.
Nursing Care Plans for Activity Intolerance: Examples and Goals
Nursing care plans provide structured frameworks for addressing activity intolerance, outlining diagnostic statements, expected outcomes, assessments, and interventions. Here are examples of care plan approaches:
Care Plan #1: Activity Intolerance related to Generalized Weakness
Diagnostic Statement: Activity intolerance related to generalized weakness as evidenced by verbal reports of fatigue and exertional discomfort.
Expected Outcomes:
- Patient will demonstrate stable cardiopulmonary status during activity (heart rate, blood pressure, respiratory rate within acceptable limits).
- Patient will report a reduced rating of perceived exertion (RPE) after physical activity.
- Patient will report a decrease in fatigue levels.
- Patient will participate in Activities of Daily Living (ADLs).
Assessments:
- Identify precipitating factors contributing to generalized weakness (e.g., chronic diseases).
- Monitor cardiopulmonary status (heart rate, rhythm, orthostatic blood pressure, respiratory rate, level of consciousness, skin color, chest discomfort) to guide activity progression.
Interventions:
- Assist with ADLs to conserve energy while promoting independence.
- Encourage rest periods before meals, ADLs, and exercise.
- Plan activities for periods when the patient has the most energy.
- Encourage endurance-enhancing physical activity.
- Progress activity gradually (ROM exercises, dangling legs, deep breathing, walking).
- Provide assistive devices to reduce fatigue and discomfort.
Care Plan #2: Activity Intolerance related to Compromised Oxygen Transport (Atelectasis)
Diagnostic Statement: Activity Intolerance related to compromised oxygen transport system secondary to atelectasis as evidenced by increased respiratory rate and cyanosis.
Expected Outcomes:
- Patient will exhibit resolution of respiratory distress related to atelectasis (respiratory rate < 20 breaths/min, absence of dyspnea, pink skin and nails, normal breathing effort, O2 saturation > 95%).
- Patient will utilize energy-conservation techniques.
Assessments:
- Assess for signs and symptoms of atelectasis (decreased breath sounds, crackles, cough, dyspnea, tachypnea, cyanosis).
- Monitor laboratory findings (chest x-ray, arterial blood gases, chest CT) to confirm and monitor atelectasis.
Interventions:
- Administer medications as prescribed (mucolytics, bronchodilators).
- Encourage deep breathing exercises and incentive spirometry.
- Teach energy conservation techniques (position changes, sitting for tasks, work-rest schedules).
- Refer to respiratory therapy for pulmonary rehabilitation.
- Provide supplemental oxygen as needed.
Care Plan #3: Activity Intolerance related to Physical Deconditioning
Diagnostic Statement: Activity intolerance related to physical deconditioning as evidenced by dyspnea on exertion and abnormal heart rate or blood pressure response to activity.
Expected Outcomes:
- Patient will demonstrate increased tolerance to activity over time.
- Patient will participate in prescribed physical activity with appropriate vital sign responses (heart rate, blood pressure, breathing rate).
Assessments:
- Assess the patient’s current level of physical activity and mobility.
- Determine the underlying cause of activity intolerance (physical, psychological, motivational).
- Monitor and record activity tolerance, including vital signs and signs of cardiac decompensation (dyspnea, palpitations, chest discomfort, hypotension/hypertension, tachycardia, decreased oxygen saturation, lightheadedness).
Interventions:
- Position bed-rest patients upright to minimize cardiovascular deconditioning.
- Assist with self-care activities, gradually increasing activity as tolerated (sitting, dangling, standing, ambulating).
- Perform ROM exercises for immobile patients.
- Refer to physical therapy for structured exercise plans.
- Provide emotional support and set mutual goals for increasing activity.
- Obtain necessary assistive devices before ambulation.
These care plan examples illustrate how nursing diagnoses, goals, assessments, and interventions are integrated to address activity intolerance effectively, focusing on improving patient outcomes and quality of life.
References
- Ackley, B.J., Ladwig, G.B., Flynn Makic M.B., Martinez-Kratz, M., & Zanotti, M. (2019). Nursing diagnosis handbook: An evidence-based guide to planning care (12th edition). Mosby.
- Carpenito, L.J. (2013). Nursing diagnosis: Application to clinical practice (14th ed.). Lippincott Williams & Wilkins.
- Doenges, M.E., Moorhouse, M.F., & Murr, A.C. (2019). Nursing care plans: Guidelines for individualizing client care across the life span (10th ed.). F.A. Davis Company.
- Grott, K., Chauhan, S.& Dunlap, J.D. (2022). Atelectasis. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK545316/
- Gulanick, M. & Myers, J.L. (2014). Nursing care plans: Diagnoses, interventions, and outcomes (8th ed.). Elsevier.
- Sharma, S. (2023). Pulmonary rehabilitation. MedScape. https://emedicine.medscape.com/article/319885-overview