Nursing diagnosis is a critical component of patient care, serving as the foundation for personalized interventions and effective healthcare strategies. This guide delves into the concept of nursing diagnosis, exploring its significance, types, and formulation, with a specific focus on actual, potential (risk), and health promotion diagnoses. Understanding these distinctions is crucial for nurses to deliver comprehensive and proactive care.
Understanding Nursing Diagnosis
A nursing diagnosis represents a nurse’s clinical judgment about a patient’s response to actual or potential health conditions or life processes. It’s not a medical diagnosis, which focuses on disease pathology, but rather a patient-centered statement identifying problems nurses are qualified and accountable to address. Nursing diagnoses are derived from patient assessments and direct the creation of nursing care plans, ensuring interventions are targeted and effective.
The Purpose of Nursing Diagnosis
Nursing diagnoses serve several vital purposes in healthcare:
- Enhancing Critical Thinking: For nursing students, formulating diagnoses sharpens problem-solving and critical thinking skills, essential for effective patient care.
- Prioritizing Care: Diagnoses help nurses prioritize patient needs and direct nursing interventions based on the most pressing issues.
- Quality Assurance: They facilitate the formulation of expected outcomes, meeting quality assurance standards required by healthcare payers.
- Resource Identification: Nursing diagnoses highlight how patients respond to health challenges and identify their strengths, enabling nurses to leverage these resources for problem resolution and prevention.
- Professional Communication: They establish a common language among nurses and the broader healthcare team, fostering clear and effective communication.
- Evaluating Care Effectiveness: Diagnoses provide a basis for evaluating the benefits and cost-effectiveness of nursing care, ensuring optimal patient outcomes.
Nursing Diagnosis vs. Medical Diagnosis vs. Collaborative Problems
It’s essential to differentiate nursing diagnoses from medical diagnoses and collaborative problems:
- Nursing Diagnosis: Focuses on the patient’s response to a health condition. For instance, a patient with pneumonia might have a nursing diagnosis of “Ineffective Airway Clearance related to excessive mucus production.” This diagnosis guides nursing actions like suctioning and chest physiotherapy.
- Medical Diagnosis: Identifies diseases or pathological states that physicians treat. Examples include Pneumonia, Diabetes Mellitus, or Heart Failure. Medical diagnoses dictate medical treatments like medication and surgery.
- Collaborative Problems: These are potential complications arising from medical conditions requiring both medical and nursing interventions. For example, a patient with surgery is at risk for infection (a collaborative problem). Nurses monitor for infection signs and implement preventative measures, sometimes in collaboration with physician-prescribed treatments.
The key distinction is that nursing diagnoses address patient responses and functional health patterns, while medical diagnoses address diseases. Nurses manage nursing diagnoses independently and collaboratively, complementing medical treatments to provide holistic patient care.
Taxonomy of Nursing Diagnoses
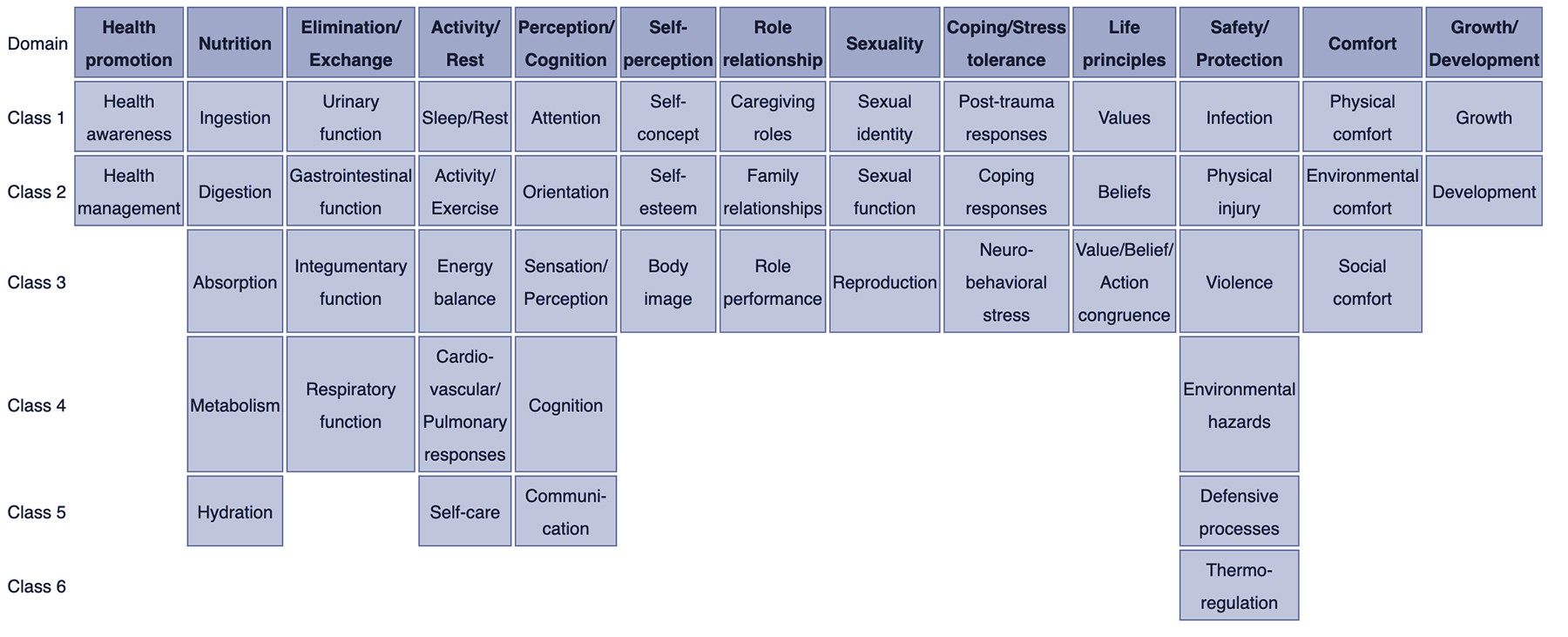
Nursing diagnoses are systematically classified to provide a standardized framework. Taxonomy II, based on Gordon’s Functional Health Patterns, organizes diagnoses into 13 domains and 47 classes. This system ensures consistency and clarity in diagnosis and documentation.
Nursing Diagnosis Taxonomy II: Illustrates the 13 Domains and 47 Classes used to categorize nursing diagnoses, providing a structured approach for nurses in identifying and classifying patient problems.
Domains of Nursing Diagnosis Taxonomy II:
- Health Promotion
- Nutrition
- Elimination and Exchange
- Activity/Rest
- Perception/Cognition
- Self-Perception
- Role Relationship
- Sexuality
- Coping/Stress Tolerance
- Life Principles
- Safety/Protection
- Comfort
- Growth/Development
Each domain further breaks down into classes, offering a granular categorization of nursing diagnoses. This structured approach helps nurses select the most appropriate diagnosis for a patient’s specific needs.
The Nursing Process and Nursing Diagnosis
Nursing diagnosis is the second step in the nursing process, a systematic approach to patient care. The five steps are:
- Assessment: Gathering patient data (physical, psychological, social).
- Diagnosis: Analyzing data to identify nursing diagnoses.
- Planning: Setting goals and outcomes and planning nursing interventions.
- Implementation: Carrying out the planned interventions.
- Evaluation: Assessing the effectiveness of interventions and patient progress.
Nursing diagnosis directly links assessment data to the rest of the care plan. It’s the critical thinking phase where nurses interpret patient information and decide on the most relevant issues to address through nursing care.
Types of Nursing Diagnoses: Actual, Risk, Health Promotion, and Syndrome
Nursing diagnoses are categorized into four main types, each addressing different aspects of patient health:
Types of Nursing Diagnoses: A visual representation highlighting the four categories: Problem-Focused (Actual), Risk, Health Promotion, and Syndrome, essential for comprehensive nursing care planning.
1. Problem-Focused (Actual) Nursing Diagnosis
A problem-focused diagnosis, also known as an actual diagnosis, describes a current patient problem identified during nursing assessment. It’s based on observable defining characteristics (signs and symptoms).
Components of a Problem-Focused Diagnosis:
- Nursing Diagnosis Label: A concise term describing the problem (e.g., “Acute Pain”).
- Related Factors: The “related to” phrase followed by factors contributing to the problem (e.g., “related to surgical incision”).
- Defining Characteristics: The “as evidenced by” phrase followed by observable signs and symptoms (e.g., “as evidenced by patient reporting pain level of 7/10 and guarding behavior”).
Example: Acute Pain related to surgical incision as evidenced by patient reporting pain level of 7/10 and guarding behavior.
2. Risk Nursing Diagnosis (Potential)
A risk nursing diagnosis (or potential diagnosis) identifies potential problems a patient is vulnerable to developing. It doesn’t describe an existing problem but predicts possible future issues based on risk factors.
Components of a Risk Diagnosis:
- Risk Diagnosis Label: “Risk for” followed by the potential problem (e.g., “Risk for Infection”).
- Risk Factors: The “as evidenced by” phrase followed by factors increasing vulnerability (e.g., “as evidenced by surgical incision and compromised immune system”).
Example: Risk for Infection as evidenced by surgical incision and compromised immune system.
Key Difference: Risk diagnoses use “risk factors” instead of “related factors” and “defining characteristics” because the problem hasn’t occurred yet.
3. Health Promotion Nursing Diagnosis
A health promotion diagnosis focuses on a patient’s desire to improve their well-being and health status. It highlights strengths and readiness to enhance health.
Components of a Health Promotion Diagnosis:
- Nursing Diagnosis Label: “Readiness for Enhanced…” followed by the area of health promotion (e.g., “Readiness for Enhanced Knowledge”).
Example: Readiness for Enhanced Knowledge related to diabetes management as expressed by patient’s active questioning and interest in learning.
Health promotion diagnoses are often one-part statements, focusing on the patient’s motivation for improvement.
4. Syndrome Nursing Diagnosis
A syndrome diagnosis describes a cluster of nursing diagnoses that frequently occur together. It recognizes patterns of problems associated with certain events or situations.
Components of a Syndrome Diagnosis:
- Syndrome Diagnosis Label: The name of the syndrome (e.g., “Rape-Trauma Syndrome”).
Example: Rape-Trauma Syndrome
Syndrome diagnoses are also typically one-part statements, representing a constellation of related diagnoses.
5. Possible Nursing Diagnosis
A possible nursing diagnosis indicates a suspected problem requiring further data to confirm or rule out. It’s used when initial assessment suggests a diagnosis, but more information is needed.
Example: Possible Risk for Deficient Fluid Volume related to unknown etiology. (Further assessment needed to confirm fluid volume status.)
Possible diagnoses are temporary and guide further assessment, eventually leading to an actual or risk diagnosis, or ruling out the initial suspicion.
Components of a Nursing Diagnosis Statement
Regardless of the type, a nursing diagnosis statement typically includes:
- Problem (Diagnostic Label): A concise name for the patient’s health issue. Qualifiers like “deficient,” “impaired,” or “ineffective” can add specificity.
- Etiology (Related Factors or Risk Factors): The cause of the problem (related factors for actual diagnoses) or factors increasing vulnerability (risk factors for risk diagnoses).
- Defining Characteristics (for Actual Diagnoses): Signs and symptoms demonstrating the presence of the problem.
The Diagnostic Process: From Data to Diagnosis
Formulating a nursing diagnosis involves a three-phase process:
-
Data Analysis:
- Compare data to standards: Identify deviations from normal health patterns.
- Cluster cues: Group related data to identify patterns.
- Identify gaps and inconsistencies: Recognize missing information or conflicting data needing further investigation.
-
Problem Identification:
- Determine if the problem is a nursing diagnosis, medical diagnosis, or collaborative problem.
- Identify patient strengths and resources.
-
Diagnostic Statement Formulation:
- Write clear, concise diagnostic statements using appropriate formats based on the type of diagnosis.
Writing Effective Nursing Diagnosis Statements
Clarity and precision are crucial in writing nursing diagnoses. The PES format (Problem, Etiology, Signs/Symptoms) is commonly used for actual diagnoses, creating a three-part statement.
- Problem (P): The diagnostic label (e.g., Impaired Physical Mobility).
- Etiology (E): Related factors (e.g., related to pain and stiffness).
- Signs/Symptoms (S): Defining characteristics (e.g., as evidenced by inability to walk without assistance and verbal report of joint stiffness).
Example using PES: Impaired Physical Mobility related to pain and stiffness as evidenced by inability to walk without assistance and verbal report of joint stiffness.
For risk diagnoses, a two-part statement is used: Risk Label “as evidenced by” Risk Factors. For health promotion and syndrome diagnoses, often a one-part statement is sufficient.
Nursing Diagnosis in Care Plans
Nursing diagnoses are the cornerstone of nursing care plans. They guide the selection of nursing interventions and outcome criteria. A well-developed nursing diagnosis leads to targeted and effective nursing care, ultimately improving patient outcomes.
Recommended Resources for Nursing Diagnosis
For further learning and reference, consider these resources:
- Ackley and Ladwig’s Nursing Diagnosis Handbook: An Evidence-Based Guide to Planning Care: A comprehensive guide with evidence-based interventions.
- Nursing Care Plans – Nursing Diagnosis & Intervention: Offers numerous care plans reflecting current best practices.
- Nurse’s Pocket Guide: Diagnoses, Prioritized Interventions, and Rationales: A quick reference tool for accurate diagnoses and interventions.
- Nursing Diagnosis Manual: Planning, Individualizing, and Documenting Client Care: Detailed information for planning and documenting individualized care.
- All-in-One Nursing Care Planning Resource – E-Book: Covers various specialties, providing a broad range of care plans.
These resources can enhance your understanding and application of nursing diagnoses in clinical practice.
Conclusion
Mastering nursing diagnosis, particularly understanding actual, risk, and health promotion types, is fundamental for competent nursing practice. By accurately identifying patient problems and potential risks, nurses can develop effective care plans, prioritize interventions, and ultimately contribute to positive patient outcomes. This guide provides a foundational understanding of nursing diagnosis, encouraging continuous learning and application in the dynamic field of healthcare.
References and Sources
- Berman, A., Snyder, S., & Frandsen, G. (2016). Kozier & Erb’s Fundamentals of Nursing: Concepts, process and practice. Boston, MA: Pearson.
- Edel, M. (1982). The nature of nursing diagnosis. In J. Carlson, C. Craft, & A. McGuire (Eds.), Nursing diagnosis (pp. 3-17). Philadelphia: Saunders.
- Fry, V. (1953). The Creative approach to nursing. AJN, 53(3), 301-302.
- Gordon, M. (1982). Nursing diagnosis: Process and application. New York: McGraw-Hill.
- Gordon, M. (2014). Manual of nursing diagnosis. Jones & Bartlett Publishers.
- Gebbie, K., & Lavin, M. (1975.) Classification of nursing diagnoses: Proceedings of the First National Conference. St. Louis, MO: Mosby.
- McManus, R. L. (1951). Assumption of functions in nursing. In Teachers College, Columbia University, Regional planning for nurses and nursing education. New York: Columbia University Press.
- Powers, P. (2002). A discourse analysis of nursing diagnosis. Qualitative health research, 12(7), 945-965.