Introduction
The rising rates of attention-deficit/hyperactivity disorder (ADHD) diagnoses in recent years have sparked considerable public discussion and concern. While some attribute this increase to a genuine rise in ADHD prevalence or improved diagnostic practices, a growing debate centers around the possibility of diagnostic inflation, encompassing both misdiagnosis and, crucially, overdiagnosis. Overdiagnosis, a well-recognized phenomenon in fields like cancer screening, is now being examined in non-cancerous conditions like ADHD. Understanding ADHD overdiagnosis is paramount to ensuring accurate, patient-centered care within modern healthcare systems.
ADHD overdiagnosis can manifest through various mechanisms. Diagnostic criteria may be broadened to include milder or more ambiguous symptoms, or the very definition of ADHD can shift, explicitly or implicitly medicalizing behaviors once considered within the realm of normal childhood variation. For instance, behaviors typical of younger children in a classroom cohort might be inappropriately pathologized. However, to distinguish increased detection from genuine overdiagnosis, it’s essential to demonstrate that these newly diagnosed cases do not experience a net benefit from diagnosis – that is, the harms of diagnosis and subsequent treatment outweigh any potential advantages to their overall well-being. While the benefits of appropriate ADHD diagnosis and treatment for some are acknowledged, the potential harms remain less understood and appreciated. These harms encompass physical, psychosocial, and financial burdens on individuals and families, as well as broader economic and societal costs.
This article presents a systematic review of existing literature, aiming to comprehensively evaluate the evidence for ADHD overdiagnosis in children and adolescents. Furthermore, it seeks to identify critical gaps in current research. This review employs a robust, five-question framework specifically designed to detect overdiagnosis in non-cancerous conditions, providing a structured approach to analyze the complex issue of ADHD overdiagnosis.
Methods
To address the multifaceted research question, a systematic scoping review was conducted, adhering to the rigorous guidelines of the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) Extension for Scoping Reviews and the Joanna Briggs Methodology. This review process was meticulously documented using the PRISMA-ScR Checklist. Detailed methodological specifics are available in previously published work.
For the purposes of this review, overdiagnosis is defined as the clinical diagnosis of a condition where the overall impact of the diagnosis is unfavorable to the individual. It is important to distinguish overdiagnosis from misdiagnosis (incorrectly labeling a child with ADHD when another condition is present) and false-positive diagnosis (an initial ADHD diagnosis later proven incorrect). These related, but distinct concepts are not the primary focus of this review.
The conceptual foundation for this review is a pre-established five-question framework specifically designed to identify characteristics indicative of overdiagnosis and subsequent overtreatment in non-cancer conditions. Data from the included studies were systematically mapped to these five core questions:
- Is there a potential for increased diagnosis? (Question 1)
- Has ADHD diagnosis actually increased over time? (Question 2)
- Are newly diagnosed cases characterized by subclinical or low-risk symptoms? (Question 3)
- Have a proportion of these additional, potentially less severe cases been treated? (Question 4)
- Do the potential harms of ADHD diagnosis (5a) and treatment (5b) outweigh the benefits, particularly for individuals with milder presentations? (Question 5)
Eligible studies included peer-reviewed primary and secondary research articles focused on children and adolescents (aged ≤18 years) published in English between January 1, 1979, and August 21, 2020. Studies encompassing mixed-age populations were included if data specific to the target age group could be extracted or if the majority of participants were 18 years or younger. Given the extensive literature on pharmacological ADHD treatment outcomes, systematic reviews and cohort studies were prioritized for question 5b. All studies were required to have a clear focus on ADHD.
A comprehensive literature search was conducted on August 21, 2020, across MEDLINE, Embase, PsychINFO, and the Cochrane Library databases. These electronic searches were supplemented by meticulous backward and forward citation tracking of key articles to ensure comprehensive capture of relevant studies.
Following deduplication and a pilot screening phase, two independent researchers (L.K. and R.S.) screened abstracts using the Abstrackr web-based text mining tool. Subsequently, full-text reviews of potentially relevant articles were conducted independently by L.K. and another researcher. Disagreements during the review process were resolved through careful discussion and consensus.
Data extraction was performed using a standardized template, iteratively developed and refined. Qualitative data were managed and analyzed using NVivo 12 Plus software. Any uncertainties during data extraction were resolved through team discussions. Quality assessment of included studies was conducted by L.K. using critical appraisal checklists developed by the Joanna Briggs Institute.
Data synthesis and analysis were structured around the five framework questions. Data were further categorized into themes and subthemes to facilitate analysis. Individual studies could contribute data relevant to multiple framework questions.
To investigate the potential reservoir of undiagnosed ADHD (question 1), variations in prevalence across different subpopulations and indicators of a symptom spectrum were examined. For questions 2 and 4, studies providing time-trend data on clinical diagnoses and medication rates were included. Assessing whether newly diagnosed cases represented milder forms of ADHD (question 3) was central to determining the net benefit or harm of increased diagnosis. Given the inconsistent definition and assessment of ADHD severity, evidence for question 3 was categorized into studies reporting ADHD severity directly and those using impairment levels as a proxy. For question 5, evidence on benefits and harms was divided into outcomes of diagnosis and outcomes of treatment, with a particular focus on the benefit-harm balance for youths with milder ADHD-related behaviors, and also considering the wider ADHD spectrum.
Results
From an initial retrieval of 12,267 records, a total of 334 studies (2.7%) met the inclusion criteria and were incorporated into this systematic review. The study selection process is detailed in a PRISMA flow diagram (eAppendix 3 in Supplement 1).
Of the 334 included studies, the majority were primary research articles (81.7%), with 18.3% being secondary research. A significant proportion of studies (65.0%) were published within the last decade, predominantly originating from North America (38.3%), Europe (27.8%), and Oceania/Asia (10.5%). Table 1 provides a detailed breakdown of the general characteristics of the included evidence sources.
Table 1. General Characteristics of Included Sources of Evidence.
| Characteristic | No. (%) |
|---|---|
| Total No. | 334 |
| Year of publication | |
| 1979-1990 | 5 (1.5) |
| 1991-2000 | 23 (6.9) |
| 2001-2010 | 89 (26.6) |
| 2011-2020 | 217 (65.0) |
| Region | |
| North America | 128 (38.3) |
| Rest of Europe | 35 (10.5) |
| Scandinavia | 33 (9.9) |
| United Kingdom/Ireland | 25 (7.5) |
| Asia | 18 (5.4) |
| Australia/New Zealand | 17 (5.1) |
| Middle East | 10 (3.0) |
| Not specified/various regions | 68 (20.4) |
| Study design | |
| Cohort | 90 (26.9) |
| Cross-sectional | 6 (1.8) |
| Diagnostic test accuracy | 9 (2.7) |
| Prevalence | 142 (42.5) |
| Qualitative | 12 (3.6) |
| Randomized clinical trial | 14 (4.2) |
| Systematic review | 44 (13.9) |
| Other review | 17 (5.1) |
The methodological quality of the included studies varied, with approximately one-third classified as having low, moderate, or high risk of bias. Studies providing evidence for question 5 (harms and benefits) were more likely to be at high risk of bias (45.7%). Figure 2 visually represents the risk of bias assessment across the included studies.
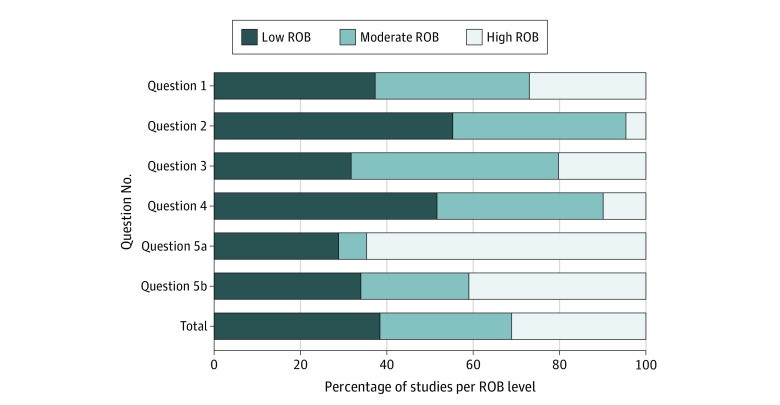 Risk of Bias (ROB) Assessment
Risk of Bias (ROB) Assessment
Table 2 summarizes the main findings of the review, mapped against the five-question framework.
Table 2. Main Results Mapped to the 5-Question Framework.
| Type of evidence (No. of studies) | Theme (No. of studies) | Subtheme (No. of studies) | Main outcomes (No. of studies) |
|---|---|---|---|
| Question 1. Is there potential for increased diagnosis (n = 104 studies) | |||
| Prevalence variations (68) | By subpopulation (48) | Sex (25) | |
| SES or insurance status (21) | |||
| Race/ethnicity (21) | |||
| Relative age (12) | |||
| Location/region (8) | |||
| Other (1) | |||
| By diagnosis (20) | Diagnostic criteria (20) | ||
| Reservoir (44) attributed to | Medicalization (3) | Behavioral problems (3) | |
| Phenotype changes (5) | Trends over time (5) | ||
| Diagnostic inaccuracy (16) associated with | Over- and underdiagnosis (16) | ||
| Spectrum of disorder (22) indicated by subtheme | Implications of extent of symptoms over time (13) | ||
| Subthreshold prevalence (8) | |||
| Verification of dimensional structure (7) | |||
| Question 2. Has diagnosis actually increased? (n = 45 studies) | |||
| Diagnosis (45) | Trend over time (45) indicated by subtheme | Change in prevalence (30) | |
| Change in incidence (12) | |||
| Change in lifetime prevalence (12) | |||
| Question 3. Are additional cases subclinical or low risk? (n = 25 studies) | |||
| Severity of disorder (17) indicated by theme | Impairment levels (11) indicated by subtheme | Change in adverse outcomes over time (2) | |
| Difference in adverse outcomes by diagnostic criteria (9) | |||
| Symptom severity (6) indicated by subtheme | Trend over time (3) | ||
| Severity proportions (2) | |||
| Diagnostic criteria (1) | |||
| Level of symptoms (8) | Clinically significant symptom prevalence (8) by | Change over time (8) | |
| Question 4. Have some additional cases been treated? (n = 83 studies) | |||
| Medication (83) | Trend over time (83) indicated by subtheme | Prevalent treatment rate (58) | |
| Incident treatment rate (9) | |||
| Medication use (11) | |||
| Consultations in which ADHD medication is prescribed (10) | |||
| Question 5a. Might harms outweigh benefits of diagnosis? (n = 31 studies) | |||
| Potential benefits of diagnosis (15) | Empowered (14) through | Explanation for problems (11) | |
| Increased control (6) | |||
| Enabled (10) to | Support (10) | ||
| Potential harms of diagnosis (29) | Disempowered (22) through | Excuse for problems (15) | |
| Loss of control (15) | |||
| Stigmatization (14) through | Permanent label and identity (14) | ||
| Question 5b. Might harms outweigh benefits of treatment (n = 120 studies) | |||
| Outcomes of pharmacological treatment (120) | Academic (19) | Cognitive and motor functioning (4) | |
| Academic performance (15) | |||
| Accidents (12) | ED use and hospital admissions (5) | ||
| Injuries and poisoning (8) | |||
| Cardiovascular (8) | Blood pressure and heart rate (2) | ||
| Safety (6) | |||
| Efficacy (30) | Symptom reduction (30) | ||
| Physical (14) | Activity (2) | ||
| Height (12) and weight (5) | |||
| Psychological (20) | Other (2) | ||
| Substance abuse (12) | |||
| Suicidal behavior (6) | |||
| Social and emotional (11) | Emotional (3) | ||
| Criminal behavior (3) | |||
| Social impairment (2) | |||
| Quality of life (4) | |||
| Tolerability (29) | Adverse events (25) | ||
| Discontinuation (6) | |||
| Various (8) | Mixed (8) |
Large Reservoir of Potentially Diagnosable ADHD
Evidence from 104 studies addressed the first framework question, indicating a substantial reservoir of potentially diagnosable ADHD. Significant variations in ADHD diagnosis rates were observed across subpopulations in 48 studies. Sex differences were highlighted in 25 studies, consistently showing lower ADHD diagnosis rates in girls compared to boys. While biological factors may contribute, two studies indicated that girls with similar symptom presentations were less likely to be diagnosed than boys, suggesting a diagnostic gender bias and an under-tapped reservoir of ADHD in girls. Decreasing sex ratios in ADHD diagnosis over time, observed in eight studies, further support this reservoir in girls being increasingly identified.
Eleven out of twelve studies investigating relative age effects demonstrated that younger children within a classroom cohort were significantly more likely to receive an ADHD diagnosis compared to their older classmates. This finding suggests that developmental immaturity may be misconstrued as ADHD, particularly in younger children relative to their peers, contributing to the diagnostic reservoir. One study that did not confirm this effect was conducted in a setting with stringent diagnostic practices, implying that adherence to strict criteria may mitigate the relative age effect and reduce the diagnostic reservoir.
Fifteen studies indicated that youths from migrant backgrounds were historically less likely to be diagnosed with ADHD. However, emerging evidence reveals a rapid increase in diagnosis rates within these groups, particularly among young Black youths, in some cases surpassing rates in White youths. This suggests a shifting landscape in ADHD diagnosis across racial and ethnic groups, potentially tapping into previously undiagnosed reservoirs. Socioeconomic status and health insurance status also played a role in diagnostic variation, as shown in 21 studies, and regional variations were demonstrated in 8 studies, all pointing towards substantial differences and highlighting the influence of non-clinical factors on ADHD diagnosis and the existence of a considerable diagnostic reservoir.
Comparing diagnostic prevalence across different diagnostic criteria, 18 out of 20 studies found that broadening diagnostic criteria led to a concurrent increase in potential ADHD cases. This demonstrates how changes in diagnostic definitions directly impact the size of the diagnosable ADHD pool. Twenty-two studies pointed to a spectrum of ADHD-related behaviors, indicating that these behaviors exist on a continuum, with diagnosed ADHD at one extreme and subthreshold behaviors at the other. Seven studies placed diagnosed ADHD at the severe end of a behavioral continuum, while eight studies identified subthreshold behaviors in a considerable proportion of young people. This spectrum concept, further supported by 13 studies showing a graded increase in adverse outcomes with increasing ADHD symptom severity, underscores a large pool of individuals with varying degrees of ADHD-related behaviors, many of whom fall below the diagnostic threshold but contribute to the overall reservoir.
Medicalization of typical childhood behaviors was identified as contributing to an expanding diagnostic reservoir in three studies. Conversely, four out of five studies examining phenotype changes reported stable or declining ADHD symptoms within the general population over time. This suggests that the expanding diagnostic reservoir is not driven by a genuine increase in underlying ADHD symptoms but rather by changes in diagnostic practices and perceptions.
Sixteen studies investigating diagnostic inaccuracies highlighted the potential for both underdiagnosis (false-negative diagnoses) and overdiagnosis (false-positive diagnoses) as sources of variation. These inaccuracies, often co-occurring, further contribute to the complexity of ADHD diagnosis and the fluctuating boundaries of the diagnostic reservoir.
Consistent Increases in ADHD Diagnosis Between 1989 and 2017
Forty-five studies addressed the second framework question, focusing on trends in ADHD diagnosis rates over time. Thirty studies analyzed changes in diagnostic prevalence, with 27 reporting significant increasing trends. Three studies noted a plateau in diagnostic rates in the early 2000s, suggesting a possible deceleration in the rate of increase during that period. Consistent evidence of increasing ADHD diagnoses came from studies measuring trends in annual diagnostic incidence (12 studies) and lifetime diagnostic prevalence (12 studies). Overall, an overwhelming majority (96.0%) of studies examining temporal trends confirmed a continuous rise in ADHD diagnoses, indicating a clear pattern of increasing diagnosis rates over several decades.
Many Additional Cases On the Milder End of the ADHD Spectrum
Twenty-five studies provided data relevant to the third framework question, exploring the severity of newly diagnosed ADHD cases. Five studies indicated that only a small proportion of diagnosed youths exhibited severe ADHD behaviors, suggesting that a significant portion of new diagnoses fall into the milder symptom range.
Eleven studies used changes in impairment levels as a proxy for ADHD severity. Eight of these studies confirmed that impairment levels, adverse outcomes, and the benefits of medication decreased as the pool of diagnosed youths expanded. This inverse relationship suggests that newly diagnosed cases, representing the expansion, tend to have milder symptoms and lower levels of associated impairment. Six studies, confirming stable or declining ADHD behaviors in youths over decades, support this finding by suggesting that the increased diagnosis rates are capturing milder cases rather than reflecting a rise in severe ADHD. Two studies examining the relative age effect found an increasing proportion of younger children in class being diagnosed compared to older children in more recent birth cohorts. This may indicate a lowering of the diagnostic threshold, capturing milder, developmentally-related cases. In contrast, three studies reported larger relative increases in more severe cases over time based on parent or clinician perceptions of severity. This could reflect a shift in perception, where the same behaviors are now rated as more severe, rather than a genuine increase in severe ADHD prevalence.
Substantial Increases in Pharmacological Treatment for ADHD Between 1971 and 2018
Eighty-three studies addressed the fourth framework question, focusing on trends in pharmacological treatment of ADHD. Sixty-four studies demonstrated an increasing percentage of youths receiving pharmacological treatment for ADHD, mirroring the rising diagnosis rates. Three studies identified a plateau or decrease in treatment trends for preschool-aged children, and two studies indicated a general declining trend in treated youths in Germany. Five studies reported increasing annual incident treatment rates, while four studies reported stable or unclear trends. However, the majority, ten out of eleven studies, documented increasing trends in medication dispensing or sales, providing converging evidence for a substantial rise in pharmacological treatment for ADHD.
Benefits May Be Outweighed by Harms in Youth With Milder ADHD Symptoms
Diagnosis
Thirty-one studies examined the consequences of ADHD diagnosis (question 5a), with a focus on the benefit-harm balance for milder cases. Only two studies specifically provided information on this subgroup. Both studies reported potential harms, finding that the diagnostic label itself could have negative social, psychological, and academic consequences for youths with milder symptoms compared to undiagnosed peers with similar behaviors.
Considering the general benefits of ADHD diagnosis across the full spectrum of severity, two main themes emerged from 14 studies. Firstly, diagnosis often led to a sense of empowerment. It provided a biomedical explanation for difficulties, lending legitimacy to their struggles and fostering understanding and sympathy from others. This explanation reduced feelings of guilt, blame, and anger, and increased perceived control, often accompanied by expectations of solutions, enhanced confidence, and a sense of belonging. Secondly, diagnosis frequently resulted in enablement, characterized by increased support and an enhanced ability to seek and accept help.
However, potential harms of diagnosis were also evident in 29 studies. Disempowerment emerged as a prominent theme in 22 studies. The biomedical framing of difficulties could serve as an excuse for problems, potentially reducing personal responsibility and leading to inaction and stagnation. This perspective may also overshadow other underlying individual, social, or systemic issues. A self-fulfilling prophecy could ensue, where the perceived inability to change limits opportunities and fosters hopelessness and passivity. This loss of control may be particularly pronounced when diagnosis is used to coerce young people into conforming to behavioral expectations. Stigmatization was another key harm, reported in 14 studies. An ADHD diagnosis can create a stigmatized identity, leading to prejudice and judgment, which in turn can exacerbate feelings of isolation, exclusion, and shame.
Treatment
One hundred and twenty studies investigated the consequences of pharmacological ADHD treatment (question 5b). Forty studies examined direct treatment outcomes, including two studies that stratified treatment efficacy by ADHD symptom severity. These studies demonstrated significantly greater treatment response in youths with more severe baseline symptoms, with diminishing benefits observed in milder cases. Notably, none of the 29 studies reporting on direct harms of treatment differentiated between case severity, highlighting a gap in understanding severity-specific treatment harms.
Among 85 studies on indirect treatment outcomes, only three focused specifically on youths with less severe ADHD. Two of these studies suggested that treatment benefits for academic outcomes were limited to youths with severe symptoms, with one study even reporting potentially harmful academic outcomes in milder cases. Another study found that the benefits of medication in reducing hospital contacts and criminal behavior were smaller in later birth cohorts, likely reflecting the expansion of treatment to milder cases.
Across the spectrum of ADHD symptoms, 24 studies reported substantial short-term symptom reduction with medication. However, only three studies followed up beyond active treatment, finding no long-term symptom differences between treated and untreated youths. One additional study found no symptom difference after a 48-hour medication washout period. In terms of harms, active treatment was commonly associated with mild and moderate adverse events and high discontinuation rates. Ten studies noted inadequate reporting of harms, suggesting potential underestimation of treatment-related risks.
Indirect treatment effects were documented across diverse outcomes, including academic, cardiovascular, physical, psychological, social and emotional well-being, and accidents. Evidence indicated benefits for academic outcomes, injuries, hospital admissions, criminal behavior, and quality of life. However, harmful outcomes were also evident, including increased heart rate and cardiovascular events, growth suppression, weight changes, risk for psychosis and tics, and stimulant misuse or poisoning. Two studies linked treatment to reduced physical activity. For suicidal behavior, emotional and social impairment, no clear favorable or unfavorable patterns were identified.
Overall, the findings suggest that while medication can produce relatively large symptom reductions, these translate to modest improvements in functional impairment at best, while carrying inherent risks. This benefit-harm ratio is likely less favorable for youths with milder ADHD, where substantial symptom reduction is less achievable.
Discussion
This systematic scoping review, to our knowledge the first of its kind, provides compelling evidence for the overdiagnosis and overtreatment of ADHD in children and adolescents. The review confirms the existence of a large reservoir of potentially diagnosable ADHD, consistently increasing rates of diagnosis and treatment, and a significant proportion of newly diagnosed cases presenting with milder symptoms. Importantly, the review highlights a critical evidence gap: a scarcity of studies assessing symptom severity in newly diagnosed cases under broadened diagnostic criteria, and a lack of research on the benefit-harm balance specifically for these individuals.
Implications of Findings
These findings have significant implications. Individuals, particularly those with milder symptoms, may be exposed to the harms of overdiagnosis and the adverse effects of medication throughout childhood, adolescence, and potentially into adulthood. The findings also extend relevance to the increasing number of adults receiving new ADHD diagnoses and may be applicable to understanding overdiagnosis in other conditions, such as autism.
Several key research questions emerge from this review. Larger-scale studies are needed to confirm whether the increasing number of ADHD diagnoses indeed represents milder symptom presentations. Crucially, future research must rigorously evaluate whether diagnosing and treating milder ADHD cases results in net harm. To address health and educational inequities, resources need to be strategically reallocated from potential overdiagnosis and overtreatment towards supporting youths with more severe symptoms who are likely to benefit most from intervention, including those currently underdiagnosed. While this review focused on overdiagnosis, misdiagnosis and underdiagnosis of ADHD are equally important and complementary issues that warrant further investigation within the broader context of equitable and appropriate healthcare resource allocation.
Based on these findings, it is recommended that practitioners, parents, and teachers carefully consider the potential benefits and harms associated with ADHD diagnosis and treatment, especially when evaluating youths (or adults) with milder symptoms. For this subgroup, the benefits of diagnosis and treatment may be considerably diminished or outweighed by potential harms.
A potential strategy to improve the benefit-harm balance in clinical practice is to adopt a stepped-diagnosis approach. This approach balances the need for efficient diagnosis and treatment for severe cases with a cautious, watch-and-wait approach for borderline cases. This mirrors active surveillance strategies used in low-risk cancers like prostate, breast, and thyroid, where overdiagnosis is a recognized concern. Such an approach ensures that healthcare resources are directed where they are most needed and can provide the greatest value.
Strengths and Limitations
This review possesses several notable strengths. The use of a five-question framework, aligned with international standards for systematic reviews, facilitated the synthesis of a large and diverse body of research. Critical appraisal of included studies allowed for evaluation of evidence quality across decades of global research. While previous analyses have examined specific aspects of ADHD overdiagnosis, this review provides a comprehensive, overarching assessment, enabling broader conclusions about ADHD overdiagnosis that earlier studies could not reach.
Despite these strengths, certain limitations must be acknowledged. While encompassing studies from numerous countries over a long period, the findings may not be universally applicable across all demographic groups. Due to the scope of the review, evidence for questions 4 and 5 was limited to pharmacological treatment, the most common and debated ADHD intervention. The review is also constrained by the availability and quality of existing evidence. While confidence in findings for questions 2 and 4 is high, studies informing questions 1, 3, and 5 were more frequently at high risk of bias. Furthermore, subjective measures, such as symptom severity, quality of life, and consequences of diagnosis, were often reported solely by parents or teachers. The absence of self-reported data from youths themselves leaves unanswered questions about potential differences in how benefits and harms might be perceived and reported by young people directly.
Conclusions
This systematic scoping review provides convincing evidence of ADHD overdiagnosis and overtreatment in children and adolescents. Despite extensive research on ADHD, significant evidence gaps remain. Specifically, high-quality studies investigating the long-term benefits and harms of diagnosing and treating ADHD in youths with milder symptoms are urgently needed to inform safe, equitable, and evidence-based clinical practice and policy.
