Anovulation, the absence of ovulation, is a significant factor contributing to female infertility. Understanding the underlying causes of anovulation is crucial for accurate diagnosis and effective treatment strategies, particularly when considering ovulation induction. This article delves into the primary causes of anovulation that are suitable for ovulation induction, categorized by their origin within the complex hypothalamic-pituitary-ovarian axis and other endocrine factors.
Hypothalamic-Pituitary Origins of Anovulation
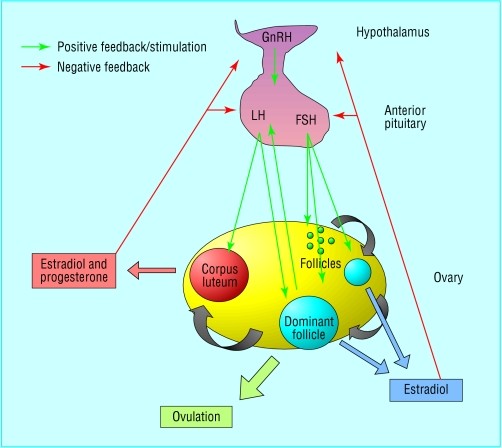
Disruptions within the hypothalamus and pituitary gland, key regulators of the reproductive system, are frequent culprits in anovulatory conditions. These disruptions often manifest as hypogonadotrophic hypogonadism, characterized by insufficient production of luteinizing hormone (LH) and follicle-stimulating hormone (FSH) by the pituitary gland.
One of the most common triggers for this hormonal imbalance is lifestyle factors. Excessive exercise and being underweight, especially resulting in a low body mass index (BMI), can significantly impair gonadotropin-releasing hormone (GnRH) secretion from the hypothalamus, subsequently affecting LH and FSH release.
Rarely, hypogonadotrophic hypogonadism can stem from more severe conditions. Sheehan’s syndrome, a consequence of pituitary gland damage due to severe postpartum hemorrhage, and Kallman’s syndrome, a genetic condition marked by GnRH deficiency and anosmia (loss of smell), are examples. Furthermore, individuals who have undergone treatment for craniopharyngioma or certain types of leukemia involving cerebral irradiation may experience secondary hypogonadotrophic hypogonadism due to radiation’s impact on the hypothalamus or pituitary gland.
Table 1: Common Causes of Anovulation Suitable for Ovulation Induction
| Hypothalamic Causes | Pituitary Causes | Ovarian Causes | Other Endocrine Causes |
|---|---|---|---|
| • Hypogonadotrophic hypogonadism (low GnRH concentration) | • Pituitary failure (hypogonadotrophic hypogonadism) | • Polycystic Ovary Syndrome (PCOS) | • Hypothyroidism |
| • Weight or exercise-related amenorrhea | • Hyperprolactinemia | • Congenital adrenal hyperplasia | |
| • Kallmann’s syndrome | • Sheehan’s syndrome | ||
| • Stress | • Craniopharyngioma or hypophysectomy | ||
| • Idiopathic | • Cerebral radiotherapy |

Hyperprolactinemia, an elevated level of prolactin in the blood, is another significant pituitary-related cause of anovulation. Often caused by a pituitary microadenoma (a small benign tumor), hyperprolactinemia disrupts the normal production of LH and FSH. While secondary amenorrhea (cessation of menstruation) is the most prevalent symptom, some women may experience galactorrhea (milky nipple discharge). In less frequent cases, a macroadenoma (larger tumor) may be present, potentially causing headaches or visual disturbances requiring prompt medical attention. Fortunately, microadenomas are typically effectively managed with medication, leading to the restoration of menstrual cycles and fertility.
Ovarian Factors in Anovulation
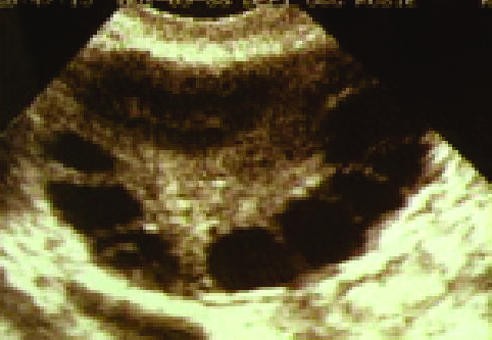
Polycystic Ovary Syndrome (PCOS) stands out as the most prevalent ovarian disorder contributing to anovulatory subfertility, accounting for approximately 70% of cases. The primary underlying issue in PCOS appears to be excessive androgen production within the ovaries. This hormonal imbalance disrupts normal follicular development, leading to the recruitment of numerous small preovulatory follicles that fail to mature properly in response to FSH. Consequently, the development of a dominant follicle, essential for ovulation, is hindered.
Women with PCOS commonly present in their late teens or early twenties with symptoms such as hirsutism (excessive hair growth), acne, and irregular menstrual cycles, often characterized by cycle lengths exceeding 35 days. Even in cases where ovulation does occur in women with PCOS, their overall chances of conception may be reduced due to the decreased frequency of ovulatory cycles. Obesity is observed in about a third of women with PCOS and significantly increases the likelihood of developing anovulation in those with the syndrome.
Other Endocrine Causes of Anovulation
Beyond the hypothalamic-pituitary-ovarian axis, other endocrine disorders can also contribute to anovulation. Hypothyroidism (underactive thyroid gland) and congenital adrenal hyperplasia (a genetic condition affecting the adrenal glands) are examples of endocrine imbalances that can disrupt ovulation.
In conclusion, anovulation arises from a diverse range of factors, primarily stemming from disruptions in the hypothalamic-pituitary-ovarian axis, with PCOS being the most common ovarian cause. Accurate diagnosis of the specific underlying cause is paramount for tailoring effective ovulation induction strategies and improving fertility outcomes for women experiencing anovulatory infertility.