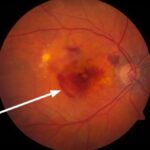
Coronary artery disease (CAD), rooted in the atherosclerotic blockage of coronary vessels, stands as a primary cause of acute coronary events. These events often arise from plaque rupture and subsequent thrombus formation. CAD is a significant contributor to cardiovascular mortality, accounting for over half of all deaths in Western nations. Alarmingly, a majority of individuals with CAD remain asymptomatic, highlighting the critical need for early detection methods. The coronary artery calcium (CAC) score has emerged as a valuable tool for quantifying coronary atherosclerosis and predicting cardiovascular risk. This article synthesizes a range of studies demonstrating the clinical correlation between coronary artery calcium levels, as measured by CAC score, and the development of cardiovascular (CV) events. We will delve into the pathophysiology and risk factors of CAD, explore various CAC scoring methodologies, and underscore the reliability of CAC scoring for the early identification of CAD, particularly in individuals without symptoms. The integration of age-dependent risk factor analysis with practical screening tools like CAC scoring is crucial for timely diagnosis, guiding effective treatment strategies, and ultimately preventing mortality in asymptomatic populations.
Keywords: Atherosclerosis Diagnosis Calcium Score, coronary artery disease, coronary artery calcium score, CAC score, myocardial infarction, Agatston score, coronary heart disease, coronary artery calcification, atherosclerotic cardiovascular disease
Introduction
Atherosclerosis, characterized by the accumulation of plaque within arterial walls, leads to the narrowing and stiffening of arteries, impeding blood flow. Coronary atherosclerosis, specifically affecting the arteries supplying the heart, results in coronary artery disease (CAD). This plaque, composed of fats, cholesterol, calcium, and other substances, can calcify and is prone to rupture, triggering thrombotic events over time [1]. CAD represents a major global health challenge, contributing significantly to morbidity and mortality worldwide. In both developed and developing nations, CAD is responsible for approximately one-third of deaths in individuals over 35 years of age, with rates approaching 50% in Western countries [2]. While both men and women are susceptible to CAD, women tend to exhibit a more favorable risk profile at younger ages, a trend that reverses in later life [3].
For decades, assessing the pre-test probability (PTP) of obstructive CAD has relied on symptom presentation and established cardiovascular (CV) risk factors, including hypertension, hyperlipidemia, family history, and smoking. However, a significant number of individuals experience major adverse cardiac events (MACEs) despite being classified as low risk based on these traditional risk factors. Current risk assessment scores are estimated to predict only 65-80% of future cardiac events [4]. Recognizing that CAD is a complex and multifactorial disease, early diagnosis in high-risk patients is paramount. Timely interventions can substantially reduce the incidence of clinical events and mortality [5].
Coronary artery calcium (CAC) has been recognized as a diagnostic marker for atherosclerosis since the 1940s [6]. In 1991, Janowitz and colleagues introduced a quantitative technique for measuring arterial calcification using Computed Tomography (CT), which became known as the Agatston score. This score quantifies the density and extent of calcium in the coronary arteries [7]. A CAC score examination is a non-invasive cardiac CT scan that quantifies the amount of calcium in the coronary arteries. Coronary calcium is a specific indicator of coronary atherosclerosis; the exception being individuals with renal insufficiency who may also develop medial calcification [8]. Generally, the quantity of calcium in the coronary vessels correlates with the extent of atheroma. The CAC score, derived from cardiac computed tomography, is a valuable tool in cardiovascular risk assessment and clinical decision-making. European guidelines on cardiovascular disease prevention in clinical practice endorse the use of CAC score for predicting heart disease risk in asymptomatic adults at intermediate risk [8–10].
This review article is structured to: 1) elucidate the pathogenic mechanisms and associated risk factors involved in the development of CAD and CAC; and 2) investigate the clinical relationship between coronary calcium and the occurrence of CV events in asymptomatic individuals at increased risk of future cardiovascular events, emphasizing the CAC score as an effective screening modality.
Pathophysiology of CAD and Coronary Artery Calcification
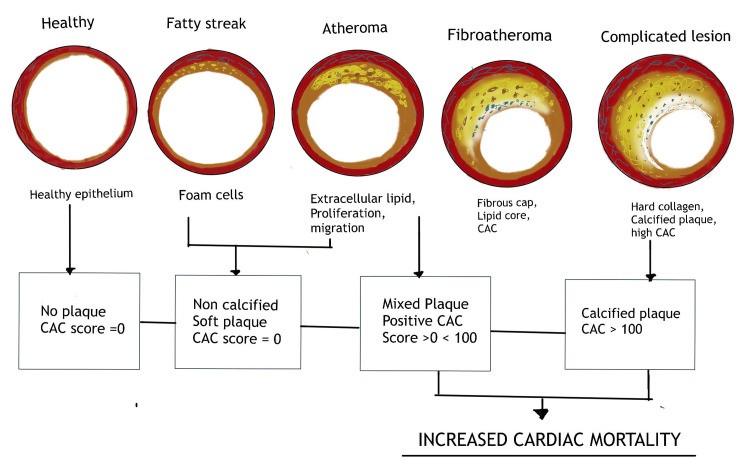
Coronary artery disease typically originates from the atheromatous narrowing and subsequent blockage of coronary vessels. Early atheromatous plaque development begins as early as young adulthood. A mature plaque consists of macrophages and smooth muscle cells, each originating from distinct cell lineages [11]. The lipid core is primarily formed by necrotic “foam cells”—monocyte-derived macrophages that migrate into the intima and accumulate lipids. Smooth muscle cells migrate from the media into the intima of the vascular wall, proliferate, and modify their phenotype to create a fibrous capsule surrounding the lipid core, forming the connective tissue matrix [11].
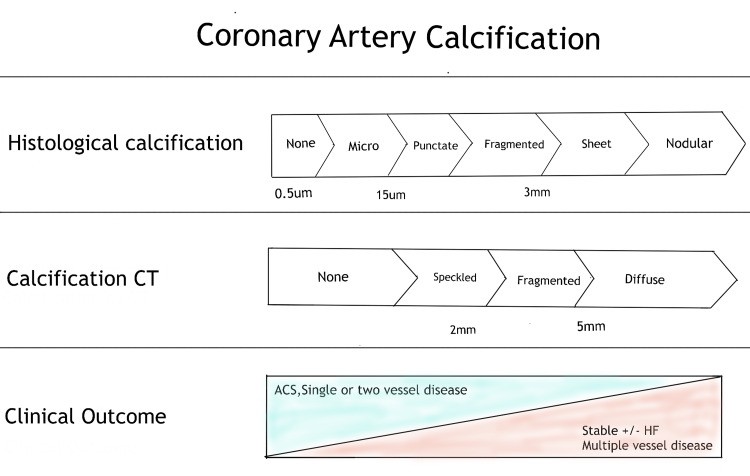
Coronary artery calcification progresses in conjunction with advanced atherosclerosis. Initially, calcification manifests as micro-nodules (0.5 to 15.0 μm), which subsequently evolve into larger calcium particles, forming sheet-like deposits (>3mm) within the arteries. These calcification processes appear to occur concurrently with plaque development (Figure 1) [12]. Significant coronary artery stenosis, defined as more than 50% narrowing or an 80% reduction in cross-sectional area, typically leads to angina during exertion. Intimal damage can trigger thrombus formation through the denudation of the thrombogenic matrix or lipid pool. Complete occlusion is more common in acute myocardial infarction compared to unstable angina, where arterial occlusion is often partial. Acute coronary events are frequently precipitated by plaque rupture, which initiates thrombus formation [11].
Figure 1. Progression of Coronary Artery Calcification in Atherosclerosis
Caption: This figure illustrates the stages of coronary artery calcification within atherosclerotic plaques, as visualized by Computed Tomography (CT). It highlights the progression from early plaque formation to advanced calcification, associated with conditions like Acute Coronary Syndrome (ACS) and Heart Failure (HF).
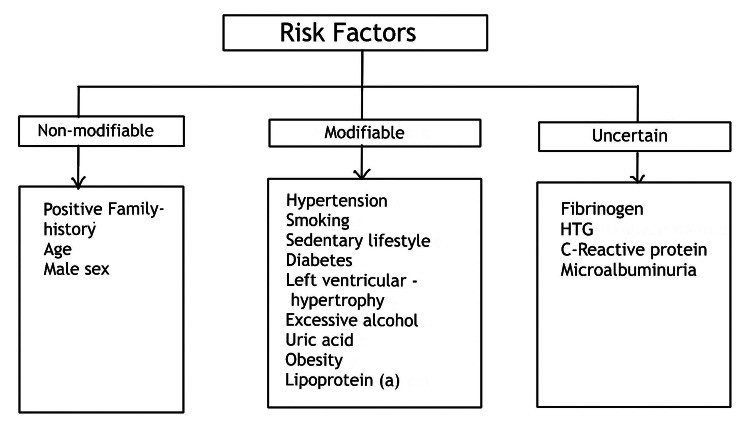
Various factors contribute to the initiation and progression of calcification, varying with the plaque stage and the surrounding environment. While aging is a common association, multiple risk factors can accelerate atheromatous plaque calcification and lead to early CAD. These include environmental factors, genetic predisposition, family history, and lifestyle choices (Figure 2) [13].
Figure 2. Key Risk Factors Associated with the Development of Coronary Artery Disease (CAD)
Caption: Diagram outlining significant risk factors for Coronary Artery Disease (CAD). These include modifiable risks such as hypertension, hyperlipidemia, diabetes, smoking, and obesity, as well as non-modifiable factors like genetics and family history. Hypertriglyceridemia (HTG) is also highlighted as a contributing factor.
Research indicates the following influences of risk factors on CAC: Women typically experience a 10 to 15-year delay in atherosclerosis development compared to men, largely attributed to the protective effects of estrogen during premenopausal years [14]. Hyperlipidemia exerts both direct and indirect effects on vascular calcification [15]. Diabetes mellitus, characterized by abnormal glucose metabolism, can directly promote vascular cell calcification, while insulin may have an inhibitory effect [16,17]. Adipose tissue-derived factors also play a regulatory role in vascular calcification; adiponectin tends to slow calcification, whereas leptin accelerates this process [18,19].
Coronary Artery Calcium (CAC) Scoring: A Reliable Diagnostic Tool
CAC is recognized as a highly specific marker of coronary artery disease. Extensive clinical and population-based studies, encompassing both short-term and long-term outcomes, have established CAC scoring as an accessible, dependable, and effective method for assessing the risk of major cardiac events. This is particularly valuable in asymptomatic individuals considering primary prevention strategies such as aspirin and statin therapy [8]. CAC testing has been shown to be cost-effective in asymptomatic groups across a broad spectrum of baseline risk [8].
Historically, vascular calcification was considered an inevitable consequence of aging. However, advancements in medical understanding have redefined atheroma calcification as an active pathological process. Ectopic bone formation is a characteristic feature of atherosclerosis and contributes to coronary artery calcification [15]. This process is influenced by developmental, inflammatory, and metabolic factors. Key transcription factors such as Msx2, Runx2, Osterix, and Sox9, along with osteogenic differentiation factors like bone morphogenetic proteins (BMPs) 2 and 4, have been implicated in vascular calcification. Matrix Gla protein, a BMP inhibitor, is found in abundance in calcified human arteries. The co-expression of both pro- and anti-osteogenic elements in CAC underscores the tightly regulated nature of this process [20]. Oxidative stress mediators are also significantly linked to calcification. Lipid oxidation generates pro-osteogenic mediators such as minimally altered low-density lipoprotein (LDL) and oxidized phospholipids [21]. Inflammation, induced by apolipoproteins and oxidized phospholipids within the vasculature, is essential for the development of both vascular calcification and atherosclerosis [22,23]. Calcification sheets and fragments can be identified through various imaging techniques, including radiography, computed tomography (CT), and intravascular imaging [11].
CAC Scoring Methodologies
The CAC score is calculated using 3 mm CT slices, acquired without overlap or gaps, focused on the cardiac region, and obtained prospectively in synchronization with the electrocardiogram (ECG) at a predetermined point in the R-R interval, typically mid-to-late diastole. Intravenous contrast medium is not used [24,25]. Calcification is defined as areas of hyper-attenuation of at least 1 mm² with a density threshold of > 130 Hounsfield Units (HU), or fewer than three consecutive pixels meeting this criterion [26].
CAC detection is feasible with several imaging modalities. However, non-contrast, electrocardiographically gated multidetector computed tomography (MDCT) and electron beam computed tomography (EBCT) are the most commonly employed in outpatient settings. EBCT was initially used for CAC scoring, and much of the early research literature is based on this technique [24]. MDCT has since become the preferred modality for CAC evaluation, rendering electron beam computed tomography largely obsolete [24].
Several methods are available for CAC score assessment, primarily categorized into the Agatston method, calcium volume determination, and calcium mass score [25–28]. The Agatston method and calcium volume determination are the most widely utilized, with the Agatston technique being particularly prevalent, cited in most population databases and research articles, and thus, the most frequently used in clinical practice. Calcium density and calcium content measurements offer greater consistency [29].
1. The Agatston Method
The Agatston method calculates a weighted sum of calcified lesions with a density exceeding 130 HU. It multiplies the calcified area by a weighting factor based on the maximum plaque attenuation: factor 1 for 130-199 HU, factor 2 for 200-299 HU, factor 3 for 300-399 HU, and factor 4 for ≥400 HU [30,31].
2. Calcium Volume Score
This method is considered the most reliable and reproducible [30]. It is determined by multiplying the number of calcified voxels by the volume of each voxel, considering all voxels with attenuation values greater than 130 HU. However, this method can be sensitive to partial volume effects, especially in plaques with high attenuation, and may exhibit variability between tests depending on plaque position within the axial slice [30,31].
3. Relative Calcium Mass Score
The relative calcium mass score is calculated by multiplying the mean attenuation of the calcified plaque by the plaque volume in each image, which reduces variability caused by partial volume effects. An absolute calcium mass score can be derived using a correction factor based on water attenuation [30,31].
The Agatston CAC score interpretation and classification can be refined by adjusting values for patient age, gender, and ethnicity, and by calculating distribution percentiles within the general population using various population databases (Table 1).
Table 1. Agatston Coronary Artery Calcium Scoring and Clinical Interpretation
| CAC Score (Agatston Method) | Risk Category | Clinical Significance |
|---|---|---|
| 0 | Absent/No Risk | Very low risk of future cardiovascular events. |
| 1-10 | Minimal | Minimal atherosclerosis likely present; low risk of future CV events. |
| 11-100 | Mild | Mild coronary artery stenosis likely; mild risk of coronary artery disease. |
| 101-400 | Moderate | Moderate plaque burden confirmed; moderately increased risk of future CV events. |
| >400 | High | High coronary calcium score; significant risk of cardiovascular event (e.g., myocardial ischemia) in the near future. |
Clinical Significance of Coronary Artery Calcium Score in Coronary Vascular Disease
Asymptomatic individuals without traditional risk factors and a CAC score of zero have a very low probability of significant luminal obstruction or atheromatous plaque. They also exhibit a very low risk of cardiovascular events within the subsequent two to five years [32]. Conversely, a positive (non-zero) CAC score indicates the presence of coronary atherosclerotic plaque, and increasing scores are associated with an elevated risk of coronary heart disease (CHD) (Figure 3) [33].
Figure 3. Correlation between Coronary Artery Calcium Scoring and Coronary Vascular Disease Risk
Caption: This graph demonstrates the relationship between increasing Coronary Artery Calcium (CAC) scores and the escalating risk of Coronary Vascular Disease. Higher CAC scores are directly correlated with a greater likelihood of future cardiovascular events.
The Multi-Ethnic Study of Atherosclerosis (MESA), initiated in 2000, is a prospective multi-center cohort study involving 6,814 men and women aged 45 to 84 years. The cohort comprised approximately 38% White, 28% African American, 22% Hispanic, and 12% Asian participants. MESA utilized EBCT scanners at three sites and MDCT systems at three sites [34]. CAC distributions were found to be similar for both EBCT and MDCT [34]. Ethnicity was observed to influence CAC, with Whites showing a higher incidence compared to the other three ethnic groups [34]. Risk factor differences did not fully account for the variations in CAC distributions across ethnicities, suggesting other contributing factors. MESA provided estimated percentile curves for the 50th, 75th, and 90th percentiles of calcium across age ranges, enabling clinicians to readily interpret the percentile significance for individual patients (Table 2) [34].
Similarly, the Framingham Heart Study (FHS) integrated CAC assessment using MDCT into examinations of the Framingham Offspring and Third Generation cohorts in 2005. Although FHS exclusively included White men and women, the distributions of CAC >0 and CAC >100 were remarkably consistent with those reported in MESA. A subsequent analysis of CAC data explored whether the distribution of CAC and coronary dominance, as determined by MDCT, improved the prediction of incident CHD beyond the standard Agatston score. The study concluded that the number of coronary arteries with CAC and CAC presence in the proximal dominant coronary artery were significantly associated with major CV events over a median follow-up of seven years (Table 2) [35].
The Coronary Artery Risk Development in Young Adults (CARDIA) study, the first prospective cohort to collect CAC data in 2,831 participants aged 32 to 46, assessed CAC during follow-up. CARDIA demonstrated that CAC >0 is not uncommon in this age group, particularly in the presence of risk factors. CAC was a strong predictor of risk beyond established risk variables in these younger individuals over a 10-year follow-up period (Table 2) [36].
Dennis et al. conducted a prospective study in 263 patients (women aged 30-65 years and men aged 30-62 years) presenting with chest pain and low-to-moderate risk of coronary artery disease. They performed a standard emergency department (ED) chest pain evaluation alongside a CT CAC scan. 133 (51%) patients had a CAC score of zero. The absence of CAC was strongly linked to noncardiac chest discomfort. Only one (1%) of the 133 patients with a CAC score of 0 developed cardiac chest discomfort during a five-year follow up. Conversely, 30 (97%) of the 31 patients with cardiac chest discomfort showed evidence of CAC on CT. The findings suggest that CT CAC assessment is a valuable adjunct in evaluating individuals at low-to-intermediate risk and concluded that cardiac chest discomfort is highly unlikely in this cohort in the absence of or with minimal CAC (Table 2) [37].
Dekker et al. conducted a single-center observational cohort study in the Netherlands from 2014-2016, involving 1265 patients. The study included only individuals who underwent coronary angiography (CAG) within 90 days before or after myocardial perfusion imaging (MPI). The final cohort comprised 150 patients after excluding those with prior coronary artery bypass grafting (CABG) or percutaneous coronary intervention (PCI), and five individuals with incomplete MPI data. The study concluded that CAC scores, when combined with MPI, enhance the diagnosis of obstructive coronary artery disease in individuals without prior revascularization procedures (Table 2) [38]. Table 2 summarizes key studies of various designs conducted between 2005 and 2019 that establish the relationship between CAC score and CAD in asymptomatic individuals.
Table 2. Summary of Studies Linking CAC Score and CAD in Asymptomatic Individuals (2005-2019)
| Reference | Study Year | Design | Sample Population | Age Range (Mean Age) | % with CAC >0 at Baseline | Key Conclusion