Introduction
Erectile dysfunction (ED), defined medically as the persistent inability to achieve or maintain an erection sufficient for satisfactory sexual intercourse [1], is a significant health concern affecting men worldwide. While population-based studies have provided valuable insights into the prevalence of self-reported ED, these figures may not accurately represent the segment of men who actively seek medical diagnosis and treatment for this condition. These surveys, while broad, capture subjective experiences but may miss the critical aspect of clinical intervention and diagnosis.
Epidemiological studies in the United States have consistently linked ED with advancing age [2–5]. Reported overall prevalence rates vary considerably, ranging from 18% [4] to as high as 47% [2], discrepancies often arising from differences in study populations and methodologies for ED identification. Notably, data from the National Health and Nutrition Examination Survey in the US indicate a dramatic increase in ED prevalence with age, escalating from 8.2% in men aged 40–49 years to a staggering 77.5% in those 75 years and older [4]. Beyond age, a constellation of comorbidities and lifestyle factors including diabetes mellitus, obesity, smoking, cardiovascular disease, hypertension, and lower urinary tract symptoms are strongly associated with ED [3, 4, 6–11].
Population surveys, by their nature, rely on self-reporting, potentially skewing the perspective on who seeks help for ED. Men participating in these surveys might experience ED symptoms but may not be sufficiently concerned to pursue a medical diagnosis or treatment. In contrast, real-world observational data, derived from extensive health insurance claims and electronic health records (EHRs), offer a different lens. These data reflect the experiences of men who have actually sought medical attention for ED, providing clinically relevant information on diagnosis and treatment patterns. Analyzing such real-world data can complement traditional epidemiological findings, offering a more nuanced understanding of ED in clinical practice.
Previous research leveraging US health insurance claims databases has shed light on the comorbidities prevalent in men diagnosed with ED [12–15], and similar investigations using UK general practice EHR databases have corroborated these findings [16]. Claims data have also been instrumental in characterizing ED treatment patterns across large male populations [17] and in evaluating the impact of ED treatment on adherence to medications for co-existing conditions [18]. However, a critical gap remains in our understanding of how age specifically relates to ED diagnosis and treatment in real-world clinical settings. This study aims to bridge this gap by utilizing real-world observational data from the United States to investigate the relationship between age and ED diagnosis or treatment, while carefully considering the influence of ED-related comorbidities. By examining these factors, we can gain valuable insights into the Average Age Of Ed Diagnosis and the broader clinical landscape of this condition.
Methods
Data Sources
This cross-sectional, observational study employed de-identified insurance claims data from the Truven Health MarketScan® Research Databases, spanning from July 1, 2009, to June 30, 2014, for the primary analysis. MarketScan databases are a robust resource containing medical and prescription drug claims for a large population of individuals in the United States with employer-sponsored health insurance, including Medicare supplemental coverage. The data are aggregated from diverse sources, including large employers, managed care organizations, hospitals, and public organizations. The validity and utility of MarketScan databases for research are well-established, with numerous publications in peer-reviewed journals [19, 20].
To ensure the robustness and generalizability of our findings, a sensitivity analysis was conducted using the Humedica® EHR database. Humedica aggregates EHR data directly from a wide network of healthcare providers, encompassing both inpatient and ambulatory care settings. This database provides a comprehensive clinical picture, including medications, laboratory results, vital signs, physician notes, diagnoses, procedures, demographics, hospitalizations, and outpatient visits. Data within Humedica are rigorously normalized, validated, and de-identified to maintain patient privacy. The sensitivity analysis mirrored the methodology of the primary analysis and utilized data from January 1, 2007, to December 31, 2014, representing the full data availability at the time of the study.
Study Population
The study population included men aged 18 years and older who had been continuously enrolled in their health plans for at least 360 days prior to the index date. No exclusion criteria were applied, ensuring a broad representation of the adult male population. Men were classified as having ED if they had either an ED diagnosis recorded (organic and/or psychogenic origin, identified by ICD-9-CM codes 607.84 or 302.72) or a prescription for a phosphodiesterase type 5 inhibitor (PDE5I), such as avanafil, sildenafil, tadalafil, or vardenafil. It is important to note that the data did not capture men receiving other forms of ED treatment, such as penile injections or implants, which constitute a smaller proportion of overall ED treatments.
Study Period Definitions
The study period encompassed a pre-index period and an index date. The pre-index period, spanning 12 months (360 days) prior to the index date, served to establish baseline characteristics and identify pre-existing comorbid conditions. For men with ED, the index date was defined as the date of their first claim for an ED diagnosis or their first PDE5I prescription. For men without ED, the index date was set as the end of their continuous enrollment period. It is crucial to note that no outcomes were assessed beyond the index date in this cross-sectional analysis.
Variable Assessment
Several key variables were examined in both men with and without ED. These included age at the index date, and the presence of ED-related comorbid conditions. The comorbidities assessed were essential hypertension (ICD9 codes 401, 4010, 4011, and 4019), other cardiovascular diseases (stroke [ICD9 430–438], myocardial infarction and angina [ICD9 410–413], coronary heart disease [ICD9 414.0], and congestive heart failure [ICD9 428]), diabetes mellitus (ICD9 2500–2509, 7751), depression (ICD9 3004, 311, 2962, 29620–29626, 2963, 29630–29636), and benign prostatic hyperplasia (BPH) (ICD9 600, 596.0, 788.20, and 788.21). Additional baseline variables included geographic region, health plan indicator, health plan type, coverage indicator, capitated service-claim indicator, and index year and month.
Statistical Analysis
Univariate statistical analysis, employing descriptive statistics, was conducted to determine the prevalence of ED, identified through diagnosis or PDE5I prescription, across the entire study population and within age-by-decade subgroups (18–29, 30–39, 40–49, 50–59, 60–69, 70–79, 80–89, and ≥90 years). Prevalence rates of ED-related comorbidities were compared between men with and without ED diagnosis or treatment. To further explore the influence of comorbidities, the prevalence of ED diagnosis or treatment within each age-by-decade subgroup was also analyzed separately for men with each specific comorbid condition.
Multivariate logistic regression analysis was performed to assess the independent relationship between ED diagnosis or treatment and age, after adjusting for ED-related comorbidities, baseline variables (geographic region, health plan, plan type, capitated vs non-capitated plan), and the year and month of the index date. Backward stepwise multivariate binary logistic regression analysis was utilized to identify which baseline variables significantly differentiated between men with and without ED. All statistical tests were two-sided, with an alpha level of 5%, and no adjustments were made for multiple comparisons.
Results
The primary analysis of the MarketScan claims database, encompassing 19,833,939 men meeting the inclusion criteria, revealed that only 1,108,842 men (5.6%) had received an ED diagnosis or a PDE5I prescription. The mean age of men with ED diagnosis or treatment was 55.2 years (SD 11.2 years). In the sensitivity analysis using the Humedica EHR database, out of 5,292,370 men, 364,723 (6.9%) had an ED diagnosis or PDE5I prescription, with a slightly higher mean age of 58.1 years. Age distribution data for men with and without ED diagnosis or PDE5I treatment in both databases are detailed in Table 1.
Based on the claims data, the prevalence of ED diagnosis or treatment showed a clear trend with age. It increased progressively with each decade, peaking in the 60–69 year age group at 11.5%. Following this peak, a decline was observed in subsequent decades: 11.0% in the 70–79 year group, 4.6% in the 80–89 year group, and dropping to 0.9% in men aged 90 years and older (Figure 1A). The Humedica EHR database exhibited a similar age-related trend in ED diagnosis or treatment prevalence (Figure 1B).
Table 1. Age of men with and without ED diagnosis or PDE5I prescription in MarketScan claims database and Humedica EHR database
| With ED Diagnosis or Treatment | Without ED Diagnosis or Treatment | |
|---|---|---|
| MarketScan Claims Database | ||
| Number of men (% of total) | ||
| Total | 1,108,842 (100) | 18,725,097 (100) |
| ED diagnosis only | 404,575 (36.5) | – |
| PDE5I prescription only | 464,039 (41.8) | – |
| ED diagnosis and PDE5I prescription | 240,228 (21.7) | – |
| Mean (SD) age, years | 55.2 (11.2) | 43.7 (16.5) |
| Range | 18–100 | 18–120 |
| Age group, years, n (% of total) | ||
| 18–29 | 19,180 (1.7) | 4,563,501 (24.4) |
| 30–39 | 73,731 (6.6) | 3,454,937 (18.5) |
| 40–49 | 223,153 (20.1) | 3,723,583 (19.9) |
| 50–59 | 399,669 (36.0) | 3,609,524 (19.3) |
| 60–69 | 289,919 (26.1) | 2,221,472 (11.9) |
| 70–79 | 83,290 (7.5) | 671,891 (3.6) |
| 80–89 | 19,127 (1.7) | 396,345 (2.1) |
| ≥90 | 773 (0.1) | 83,844 (0.4) |
| Humedica EHR Database | ||
| Number of men (% of total) | 4,927,647 | |
| Total | 364,723 (100) | |
| ED diagnosis only | 107,529 (29.5) | – |
| PDE5I prescription only | 100,031 (27.4) | – |
| ED diagnosis and PDE5I prescription | 157,163 (43.1) | – |
| Mean (SD) age, years | 58.1 (11.9) | 49.9 (19.0) |
| Range | 18–84 | 18–84 |
| Age group, years, n (% of subgroup) | ||
| 18–29 | 5,212 (1.4) | 919,114 (18.7) |
| 30–39 | 18,591 (5.1) | 718,919 (14.6) |
| 40–49 | 59,392 (16.3) | 782,266 (15.9) |
| 50–59 | 111,653 (30.6) | 880,516 (17.9) |
| 60–69 | 106,105 (29.1) | 719,791 (14.6) |
| 70–79 | 54,226 (14.9) | 527,542 (10.7) |
| 80–89 | 9,544 (2.6) | 379,499 (7.7) |
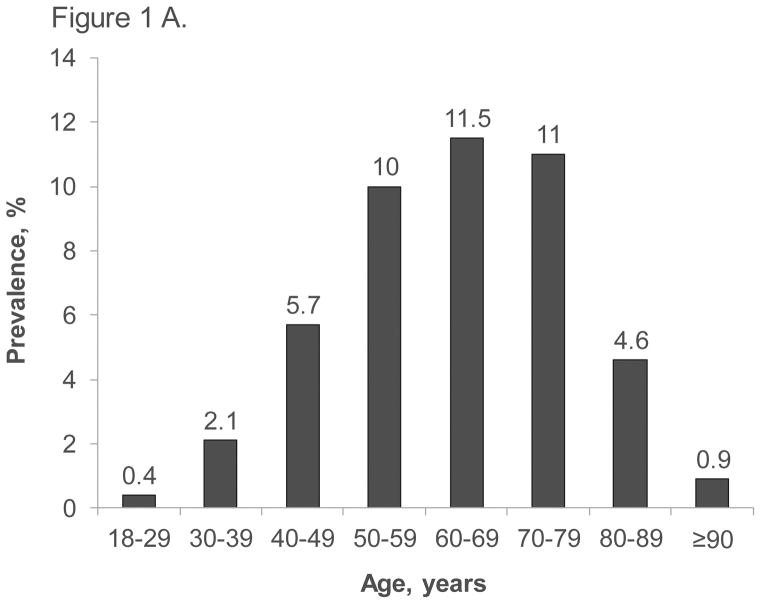

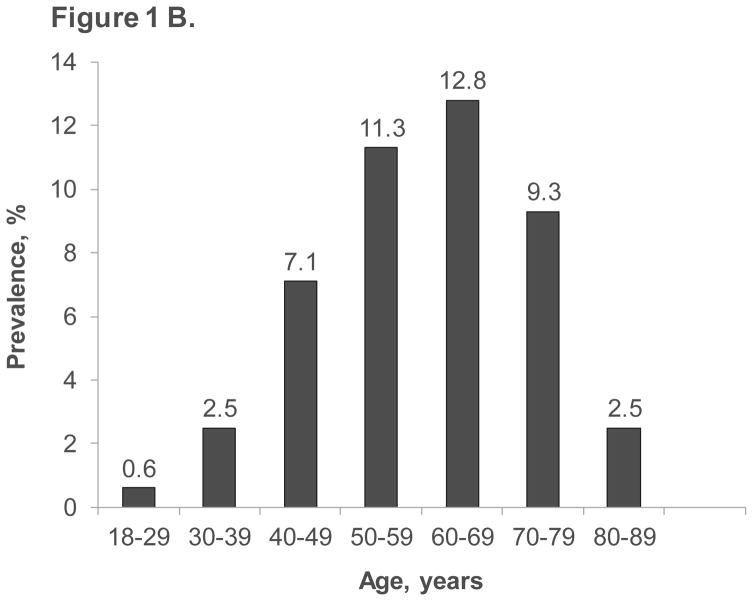
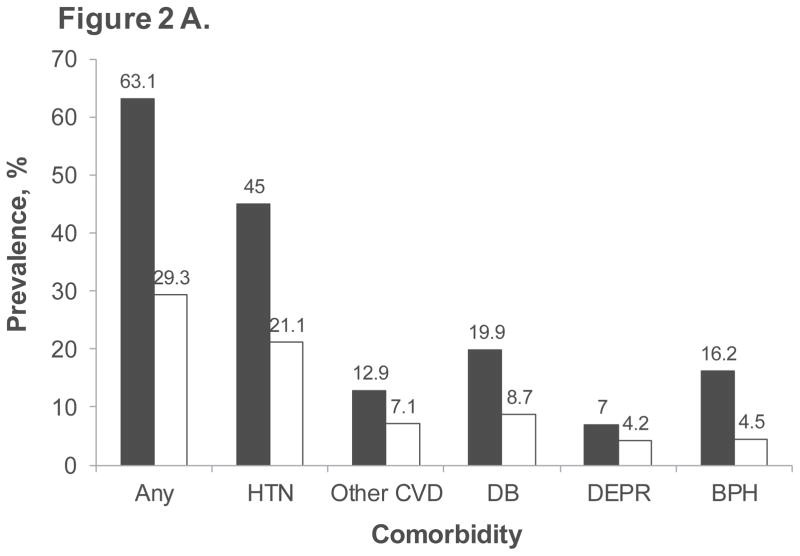
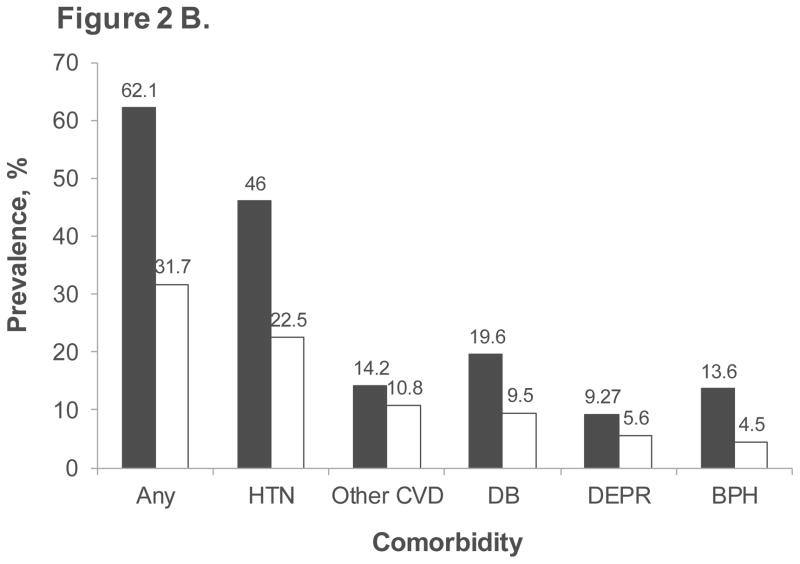
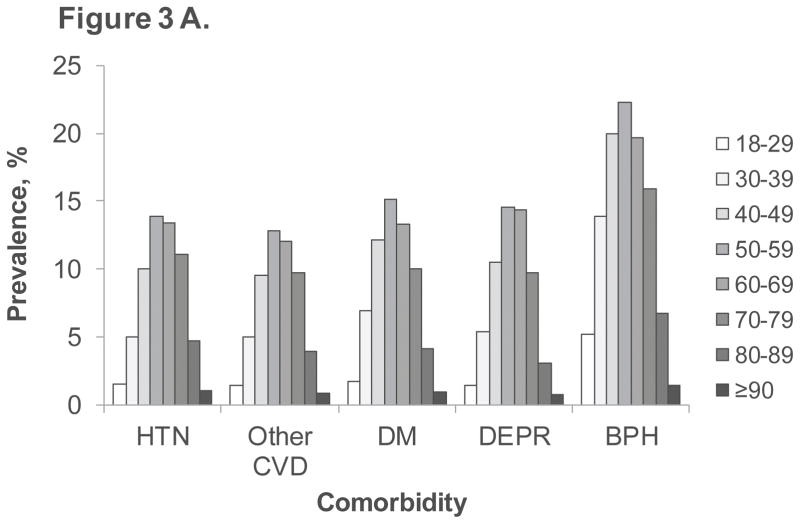
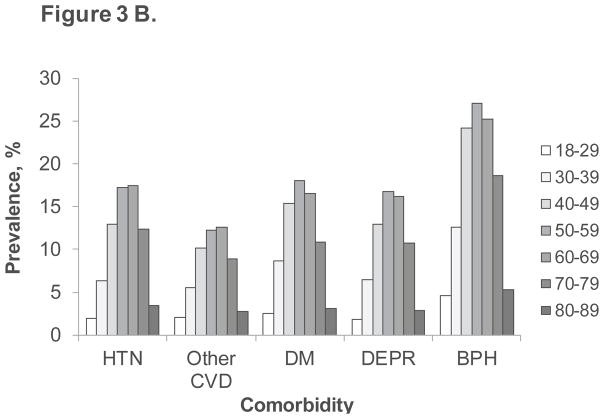
Figure 1. Prevalence of ED diagnosis or treatment by age in MarketScan claims database (A) and Humedica EHR database (B)
Comorbidity analysis in the claims database revealed that men with ED diagnosis or treatment had a significantly higher prevalence of any comorbid condition (63.1%) compared to those without ED (29.3%). This pattern extended to each specific comorbidity examined, including hypertension, other cardiovascular disease, diabetes mellitus, depression, and benign prostatic hyperplasia (Figure 2A). The EHR database corroborated these findings, showing similar prevalence rates for both overall comorbidity and individual comorbidities in men with and without ED diagnosis or treatment (Figure 2B). Further analysis within each comorbidity subgroup in both databases demonstrated a consistent age-related trend in ED diagnosis or treatment prevalence, mirroring the trend observed in the overall population (Figure 3A and 3B).
Figure 2. Prevalence of comorbid conditions in men with and without ED diagnosis or treatment in MarketScan claims database (A) and Humedica EHR database (B)
Figure 3. Prevalence of ED diagnosis or treatment by age and comorbidity in MarketScan claims database (A) and Humedica EHR database (B)
Multivariate analyses confirmed a significant association between age and ED diagnosis or treatment, even after controlling for comorbidities, baseline characteristics, and index date timing. Using the MarketScan claims database as the basis, men aged 30–39 years had over five times higher odds of ED diagnosis or treatment compared to men aged 18–29 years. This increased to over 15-fold for men aged 40–49 years, and surpassed 20-fold for men in the 50–59, 60–69, and 70–79 age groups (all p<0.001, Table 2). Interestingly, men aged 90 years and older showed significantly lower odds of ED diagnosis or treatment compared to the youngest age group (p<0.001, Table 2).
Table 2. Multivariate analysis of the relationship between age and ED diagnosis or treatment in MarketScan claims database and Humedica EHR database
| Age, y | Regression Coefficient (SE) | Odds Ratio†(95% CI) |
|---|---|---|
| MarketScan Claims Database | ||
| 18–29 | 1 | |
| 30–39 | 1.628(0.008) | 5.095‡ (5.012–5.181) |
| 40–49 | 2.732(0.00792) | 15.357‡(15.120–15.597) |
| 50–59 | 3.327(0.008) | 27.865‡(27.440–28.297) |
| 60–69 | 3.062(0.008) | 21.376‡(21.043–21.715) |
| 70–79 | 3.227(0.009) | 25.211‡(24.752–25.678) |
| 80–89 | 1.755(0.012) | 5.785‡(5.651–5.922) |
| ≥90 | −0.311(0.0381) | 0.733‡(0.680–0.790) |
| Humedica EHR Database | ||
| 18–29 | 1 | |
| 30–39 | 1.612(0.017) | 5.012‡(4.845–5.185) |
| 40–49 | 2.603(0.016) | 13.51‡(13.09–13.94) |
| 50–59 | 3.051(0.016) | 21.14‡(20.50–21.80) |
| 60–69 | 3.107(0.016) | 22.36‡(21.68–23.07) |
| 70–79 | 2.436(0.016) | 11.43‡(11.07–11.81) |
| 80–89 | 1.132(0.019) | 3.103‡(2.987–3.223) |
Multivariate analysis, controlling for age, baseline characteristics, and index date timing, revealed that several comorbidities significantly influenced the odds of ED diagnosis or treatment (Table 3). Hypertension, diabetes mellitus, depression, and benign prostatic hyperplasia were associated with a significantly increased likelihood of ED diagnosis or treatment. Conversely, other cardiovascular diseases (excluding hypertension) were significantly associated with a decreased odds of ED diagnosis or treatment (p<0.001 for all, Table 3). These patterns were consistently observed in both the MarketScan claims database and the Humedica EHR database.
Table 3. Multivariate analysis of the relationship between each comorbidity and ED diagnosis or treatment in MarketScan claims database and Humedica EHR database
| Regression Coefficient (SE) | Odds Ratio† (95% CI) | |
|---|---|---|
| MarketScan Claims Database | ||
| Hypertension | 0.6324 (0.00271) | 1.882‡ (1.872–1.892) |
| Other cardiovascular disease§ | −0.4873 (0.004) | 0.614‡ (0.610–0.619) |
| Diabetes mellitus | 0.2839 (0.00333) | 1.328‡ (1.320–1.337) |
| Depression | 0.3202 (0.00488) | 1.377‡ (1.364–1.391) |
| Benign prostatic hyperplasia | 0.8991 (0.00379) | 2.457‡ (2.439–2.476) |
| Humedica EHR Database | ||
| Hypertension | 1.084 (0.005) | 2.956‡ (2.928–2.985) |
| Other cardiovascular disease§ | −0.403 (0.007) | 0.669‡ (0.660–0.677) |
| Diabetes mellitus | 0.331 (0.006) | 1.393‡ (1.376–1.410) |
| Depression | 0.442 (0.008) | 1.555‡ (1.532–1.579) |
| Benign prostatic hyperplasia | 1.110 (0.007) | 3.033‡ (2.990–3.076) |
Discussion
This real-world study, utilizing both US health insurance claims and EHR data, reveals a generally low prevalence of ED diagnosis or treatment. A significant finding is the strong association between age and ED diagnosis or treatment. The prevalence increases with age, reaching its peak in men aged 60-69 years, which could be considered the average age range where men are most likely to seek and receive an ED diagnosis. However, it’s important to note that prevalence decreases in very elderly men. This decline in older age groups might be attributed to various factors, including reduced sexual activity due to lack of partners or diminished interest, decreased concern about ED with advancing age, the overshadowing impact of other health conditions, or potentially, a lower likelihood of healthcare providers inquiring about ED in very old men.
Men who received an ED diagnosis or treatment exhibited a significantly higher prevalence of comorbidities compared to those without. Importantly, the age-related pattern of ED diagnosis or treatment remained consistent even within each comorbidity subgroup. Multivariate analyses underscored that age (for each decade after age 29 and before 90) and specific comorbidities were independent risk factors for ED diagnosis or treatment. Hypertension, diabetes, depression, and BPH were identified as significant risk factors, even after accounting for age and other baseline variables. In contrast, other cardiovascular diseases were associated with a lower odds of ED diagnosis or treatment, possibly because the severity of these conditions might make sexual activity less of a priority or medically contraindicated.
Our findings are largely consistent with previous real-world observational studies examining comorbidities in men with ED using US claims data [12–15] and UK EHR data [16]. While the UK study lacked age distribution data, the US studies reported age distributions broadly similar to our current study. Comorbidity prevalence, particularly for hypertension and diabetes, also aligned closely with previous reports. The slightly lower prevalence of depression in our study compared to some earlier reports might reflect variations in diagnostic coding or study populations. Consistent with our results, prior research has consistently shown higher comorbidity rates in men with ED compared to those without [12, 14–16], and multivariate analyses have confirmed increased risks of diabetes, hypertension, and depression across age groups [14–16].
However, our study’s prevalence rates of ED diagnosis or treatment are lower than those reported in US population-based epidemiological surveys focusing on ED symptoms. This discrepancy is expected, as our study focused on clinical diagnosis and treatment seeking, whereas surveys capture self-reported symptoms, regardless of whether men seek medical help. For example, age-specific ED prevalence from the National Health and Nutrition Examination Survey is considerably higher than our claims-based diagnosis/treatment rates across all age groups [4]. Similarly, a national probability survey also reported higher ED prevalence rates across age groups [3]. Both our study and these surveys identified hypertension and diabetes as significant risk factors for ED, despite the difference in prevalence estimates. Discrepancies between real-world data and population surveys are not unique to ED and have been observed in various health domains [21–27], potentially arising from factors like recall bias, non-response bias, coding errors, and the distinction between self-reported symptoms and clinically documented diagnoses or treatments [28].
The established link between ED diagnosis or treatment and comorbidities like hypertension and diabetes reinforces the role of ED as a potential early indicator of cardiovascular disease, a connection extensively discussed in the Princeton Consensus Conferences [29, 30]. Future real-world studies specifically focusing on myocardial infarction, stroke, and ED severity are warranted to further explore this crucial relationship.
Strengths of this study include the use of two large and distinct databases, enhancing the generalizability of the findings. MarketScan, with its diverse data sources, offers broader representation than single-payer systems. Humedica EHR data, spanning various care settings, provides a comprehensive clinical perspective. However, limitations exist. MarketScan data are primarily employer-sponsored, potentially limiting generalizability to uninsured men, those with other insurance types, or those seeking ED treatment outside formal medical channels. Elderly men in MarketScan are largely limited to those with Medicare supplemental insurance. Similarly, Humedica findings may not fully represent hospitals outside their network. The cross-sectional design precludes causal inferences between age and ED diagnosis or treatment. Finally, some men might have had prior ED diagnoses or PDE5I prescriptions before the study period, potentially leading to misclassification as not having ED at baseline.
Conclusions
In the US real-world healthcare setting, the prevalence of clinically recognized and treated ED is relatively low. ED diagnosis and treatment prevalence is significantly influenced by age, increasing until the 60-69 year age range, then decreasing in very advanced age. Comorbidities are significantly more prevalent in men diagnosed or treated for ED, and age remains an independent risk factor for ED diagnosis or treatment, even after considering comorbidities. Further research is needed to explore potential barriers to ED diagnosis and treatment in real-world settings and to understand the reasons behind the observed decline in diagnosis and treatment in very elderly men.
What’s known
Population-based surveys provide valuable self-reported data on ED prevalence, but may not capture the experiences of men who actively seek medical diagnosis and treatment. Self-reporting can introduce biases and may not fully represent the clinically relevant aspects of ED management.
What’s new
This study, based on real-world data, reveals that the prevalence of ED diagnosis and treatment in the US is low, increases with age up to the 60-69 age group, then decreases in very old men, and is strongly associated with comorbidities. Age is confirmed as an independent predictor of ED diagnosis and treatment, even after accounting for the presence of comorbidities. This highlights the importance of considering real-world clinical data to complement population-based survey findings in understanding ED.
Acknowledgments
Grant Support: P30 CA008748
This study was sponsored by Pfizer Inc. Editorial and medical writing assistance was provided by Deborah Campoli-Richards, RPh, and Patricia B. Leinen, PhD, of Complete Healthcare Communications, LLC (Chadds Ford, PA, USA), and was funded by Pfizer Inc.
Footnotes
Author Disclosures
John P. Mulhall: Consultant for Absorption Pharmaceuticals, AMS, Lilly, Meda, Nexmed, and Vivus; Scientific study/trial for AMS, Pfizer, and Vivus; other for Alliance for Fertility Preservation and Association of Peyronie’s Disease Advocates
Xuemei Luo: Employee of Pfizer Inc
Kelly H. Zou: Employee of Pfizer Inc
Vera Stecher: Employee of Pfizer Inc
Aaron Galaznik: Former employee of Pfizer Inc during the conduct of the study and initiation of the manuscript.
Author contributions
All authors contributed to this manuscript as follows: study conception and design, analysis and interpretation of data, and drafting of the manuscript or revised critically for intellectual content.
References
[1] NIH Consensus Development Panel on Impotence. Impotence. NIH Consensus Development Conference Statement. December 7-9, 1992. Am J Med. 1993;94(5A):1A-31A.
[2] Feldman HA, Goldstein I, Hatzichristou DG, Krane RJ, McKinlay JB. Impotence and its medical and psychosocial correlates: results of the Massachusetts Male Aging Study. J Urol. 1994;151(1):54-61.
[3] Laumann EO, Paik A, Rosen RC. Sexual dysfunction in the United States: prevalence and predictors. JAMA. 1999;281(6):537-544.
[4] Selvin E, Burnett AL, Platz EA. Prevalence and risk factors for erectile dysfunction in the US. Medicine (Baltimore). 2007;86(3):151-157.
[5] Shifren JL, Monz BU, Russo PA, et al. Sildenafil for treatment of erectile dysfunction in men with diabetes mellitus: results of a randomized, double-blind, placebo-controlled study. Diabetes Care. 2002;25(9):1518-1523.
[6] Allen MS, Walter EE, представительство для изучения сахарного диабета. Erectile dysfunction is common in men with type 2 diabetes and associated with cardiovascular risk factors. Eur Urol. 2009;55(6):1468-1476.
[7] Braun M, Wassmer G, Klotz T, et al. Epidemiology of erectile dysfunction: results of the ‘Cologne Male Survey’. Int J Impot Res. 2000;12(6):305-311.
[8] De Berardis G, Pellegrini F, Franciosi M, et al. Erectile dysfunction and depression in patients with type 2 diabetes: a systematic review. Diabet Med. 2002;19(12):971-978.
[9] Grover SA, Lowensteyn I, Kaouache M, et al. The prevalence of erectile dysfunction in men with established cardiovascular disease. Am J Med. 2006;119(2):123-129.
[10] Lewis RW, Fugl-Meyer KS, Corona G, et al. Definitions/epidemiology/risk factors for sexual dysfunction. J Sex Med. 2010;7(4 Pt 2):1598-1616.
[11] Saigal CS, Joyce G, Petrini M. Impact of benign prostatic hyperplasia and erectile dysfunction on patient quality of life. J Urol. 2005;173(5):1737-1741.
[12] Gill J, Marcella S, Messerli FH, et al. Erectile dysfunction and subsequent cardiovascular risk. Arch Intern Med. 2005;165(8):85-89.
[13] Jackson G, Gill J, Hackett G, et al. сердечно-сосудистый риск и эректильная дисфункция: оценка мужчин с эректильной дисфункцией как популяции сердечно-сосудистого риска. Int J Clin Pract. 2010;64(10):1294-1299.
[14] Kim SC, Fisher MD, Margolis DJ, et al. Cardiovascular risk factors and comorbidities of men with erectile dysfunction. Am J Mens Health. 2012;6(1):20-27.
[15] Vlachopoulos C, Terentes-Printzios D, Ioakeimidis N, et al. Erectile dysfunction in the metabolic syndrome and diabetes: vascular and hormonal aspects. Curr Vasc Pharmacol. 2011;9(2):212-221.
[16] Vinogradova Y, Coupland C, Hippisley-Cox J, et al. Use of phosphodiesterase type 5 inhibitors for erectile dysfunction and risk of adverse cardiovascular events in men with and without cardiovascular disease: nested case-control study using primary care data. BMJ. 2015;351:h4846.
[17] McVary KT, Rogers T, Chiou CF, et al. Characterization of erectile dysfunction treatment patterns in a large population of men in the United States. J Sex Med. 2007;4(6):1659-1666.
[18] Patel AL, Rajpathak SN, Desai R, et al. Impact of treatment of erectile dysfunction on adherence to long-term medications for comorbid conditions. Curr Med Res Opin. 2013;29(12):1583-1590.
[19] Johnson PJ, Botteman MF, Ozminkowski RJ, et al. межличностные различия в затратах на здравоохранение среди сотрудников с диабетом 2 типа: анализ данных MarketScan. J Occup Environ Med. 2007;49(8):853-862.
[20] Pauly MV, Burns R, قلمدانی на اساس داده های ادعایی: کاربردها، مزایا و محدودیت ها. Health Serv Res. 2006;41(4 Pt 2):1607-1627.
[21] Boyle JP, Honeycutt AA, Narayan KM, et al. спрогнозированная распространенность сахарного диабета типа 2 в США среди населения взрослых США: 2005-2050 гг. Diabetes Care. 2001;24(7):1255-1262.
[22] Centers for Disease Control and Prevention. Национальная статистика по диабету, 2014 г. 2014 г; http://www.cdc.gov/diabetes/pubs/statsreport14/national-diabetes-report-report.pdf. Accessed October 2, 2016.
[23] Roger VL, Go AS, Lloyd-Jones DM, et al. статистика сердечных заболеваний и инсульта – обновление 2012 г.: отчет Американской кардиологической ассоциации по статистике. Circulation. 2012;125(1):e2-e220.
[24] Centers for Disease Control and Prevention. 2014 Assisted Reproductive Technology National Summary Report. 2016; https://www.cdc.gov/art/pdf/2014-art-report/national-summary.pdf. Accessed October 2, 2016.
[25] Koch M, Ullman K, Graham J, et al. Частота посещений психиатра в США. Psychiatr Serv. 2014;65(11):1309-1316.
[26] Raebel MA, Malone DC, Conner KA, et al. оценка приверженности лекарственной терапии астмы с использованием данных рецептов аптеки, данных медицинских требований и опросов пациентов. J Manag Care Pharm. 2013;19(1):85-91.
[27] Steiner JF, ожидания, выбор, удовлетворение и данные ادعایی. Med Care. 2006;44(5 Suppl 1):S3-S5.
[28] Bowling A. Research methods in health: investigating health and health services. Buckingham: Open University Press; 2009.
[29] Jackson G, Nehra A, Miner M, et al. Второе Принстонское соглашение по эректильной дисфункции и сердечно-сосудистым заболеваниям. J Sex Med. 2006;3(1):28-38.
[30] Nehra A, Jackson G, Miner M, et al. Принстонское соглашение III. Am J Cardiol. 2012;110(10 Suppl):3-28.
