Introduction
The classification of HIV infection has evolved to better reflect the stages of the disease and inform public health interventions. The 2014 revision of the US surveillance case definition introduced “stage 0” to represent early HIV infection, a period considered to last approximately six months post-infection. This classification is critical because early, particularly acute, HIV infection is characterized by significantly higher viral loads compared to later stages of the disease. These elevated viral loads dramatically increase the risk of HIV transmission, making the early diagnosis period a crucial window for intervention.
Prompt identification of individuals in stage 0 presents a vital opportunity to curb HIV transmission during this highly infectious acute phase. Interventions at this stage, such as immediate initiation of antiretroviral treatment (ART) to suppress viral load and comprehensive partner services, are paramount. Partner services involve public health professionals working with newly diagnosed individuals to identify and contact their sexual and needle-sharing partners from the preceding year. These partners are then offered HIV testing, counseling, and linkage to care if needed. Identifying and engaging partners is essential, as they too may be in the early stages of HIV infection, further emphasizing the need for timely intervention.
This analysis aims to underscore the elevated viral loads associated with early HIV infection, justifying the prioritization of stage 0 infections for targeted interventions to prevent onward transmission. To achieve this, we compared median earliest viral loads across different HIV stages (0, 1, 2, and 3) within the first six weeks following diagnosis. Furthermore, recognizing that acute infections pose the highest transmission risk due to peak viral loads, we sought to differentiate between acute and post-acute early infections within stage 0 using HIV surveillance data. By defining subcategories within stage 0 that approximate acute and post-acute early infection phases, we compared their respective median viral loads to highlight the heightened urgency for intervention in cases of acute infection. Understanding the Average Hiv Viral Load At Diagnosis across different stages is crucial for informing effective public health strategies.
Methods
Data Source
This study utilized data from the National HIV Surveillance System (NHSS) of the Centers for Disease Control and Prevention (CDC). The dataset encompassed 203,392 HIV infections diagnosed between 2012 and 2016, reported through December 2017 from all 50 US states, the District of Columbia, Puerto Rico, and the US Virgin Islands. While the NHSS database software automatically classified stage 0 infections for diagnoses from 2014 onwards (following the publication of the stage 0 definition in 2014), we retroactively applied the stage 0 definition to infections diagnosed in 2012 and 2013. This retroactive application aimed to increase the sample size of stage 0 diagnoses available for analysis, thereby strengthening the statistical power of our findings related to average HIV viral load at diagnosis in early infection.
Data Exclusion Criteria
We excluded 24.03% (48,880 out of 203,392) of infections where the stage at diagnosis could not be determined. These cases lacked the necessary reported negative or indeterminate HIV test results for stage 0 classification, and also lacked CD4 T-lymphocyte test results or opportunistic illness diagnoses required for staging as stage 1, 2, or 3 within three months of diagnosis.
To analyze the natural progression of viral loads before potential antiretroviral therapy influence, we focused on the earliest viral load measurement taken within the first 6 weeks post-diagnosis for each infection. This restriction removed an additional 32,047 infections from the analysis that did not have a viral load recorded within this timeframe. We assumed that initial viral load specimens are typically collected before ART initiation to establish a baseline for monitoring treatment efficacy.
Further exclusion criteria were applied to minimize the impact of antiretroviral drugs and erroneous data. We removed cases where antiretroviral drug initiation was reported to precede the date of the first viral load (10.04% of cases with reported ART start dates). We also excluded 4711 cases with reported earliest viral loads of “undetectable” or very low (0-19 copies/mL), as these values are atypical in untreated individuals and may indicate pre-diagnosis treatment or represent logarithmically transformed values unsuitable for our analysis. Cases with viral loads reported as 0-9 copies/mL were also excluded due to potential logarithmic transformation issues. Additionally, 167 cases with non-numerical viral load reports and 165 cases with incomplete diagnosis or viral load dates were removed to ensure data accuracy and precise calculation of the time interval between diagnosis and viral load measurement, crucial for analyzing the average HIV viral load at diagnosis within specific weeks post-diagnosis.
After applying all exclusion criteria, the final analytic dataset comprised 115,297 HIV infections (each with the earliest viral load within 6 weeks of diagnosis), representing 56.68% of the total reported cases diagnosed between 2012 and 2017.
Definitions of HIV Stages, Including Stage 0 Subcategories
Stage 0 Definition
Stage 0 HIV infection, as per the 2014 US surveillance case definition, indicates early infection. Our definition for stage 0 in this analysis is based on HIV test result sequences, not strictly on diagnostic algorithms due to NHSS data limitations. We classified infections as stage 0 based on specific sequences of positive (reactive), negative (nonreactive), or indeterminate HIV test results, as illustrated in Figure 1 from the original publication.
Figure 1.
Figure 1: Test sequences defining stage 0 preliminary subgroups for assessing average HIV viral load at diagnosis in early infection.
These sequences include various combinations of antibody and nucleic acid tests (NATs) within specific timeframes relative to the first positive HIV test. For instance, one sequence involves an initial positive antibody test followed within 60 days by a negative or indeterminate antibody test and a positive NAT within 180 days of the negative/indeterminate result. Another sequence starts with a positive NAT followed within 60 days by a negative or indeterminate antibody test. These criteria are designed to identify infections in the very early stages, where antibody responses may still be developing or recently developed, which are key to understanding the average HIV viral load at diagnosis in the acute phase.
Stage 0 Subcategories: 0α and 0β
We further categorized stage 0 into preliminary subcategories (0A through 0F) based on the specific test result sequences (A through F in Figure 1). Subcategories 0A and 0B align with acute infection recognition based on recommended testing algorithms. Subcategories 0C and 0D are similar to 0A and 0B, but with a different order of test results that, while not strictly fitting the published case definition for stage 0, were included due to their association with high viral loads, indicative of acute infection and relevant to the study of average HIV viral load at diagnosis. Subcategories 0E and 0F are defined by a negative or indeterminate test followed by a positive test within 180 days, differentiated by whether the first positive test was a NAT (0E) or an antibody/antigen test (0F).
Subcategories 0A-0D were prioritized over 0E or 0F in cases of overlapping test sequences, as they are based on more recent negative test results, suggesting a higher likelihood of representing acute infection and thus more relevant to assessing peak average HIV viral load at diagnosis.
Based on initial analysis revealing high viral loads in subcategories 0A-0E, we consolidated these into a larger subcategory, “0α,” to represent acute infection. Subcategory 0F was renamed “0β,” representing mostly post-acute early infection. This distinction is critical for comparing the average HIV viral load at diagnosis between acute and post-acute early stages.
Stages 1, 2, and 3 Definitions
If stage 0 criteria were not met, HIV infections were classified into stages 1, 2, or 3 based on the earliest criteria met within 3 months of diagnosis. These criteria include CD4 T-lymphocyte counts or percentages indicative of each stage, or the diagnosis of opportunistic illnesses indicative of stage 3 (AIDS). In cases where criteria for multiple stages (excluding stage 0) were met within the same month, the most advanced stage was assigned as the stage at diagnosis. These later stages reflect progression of the infection beyond the initial acute phase, and their viral load levels at diagnosis are compared to those of stage 0 to understand the trajectory of average HIV viral load at diagnosis across the spectrum of HIV infection stages.
Diagnosis Date Definition
The “diagnosis date” was defined as the earliest date of objective evidence of HIV infection. This was determined by the earliest of four events: (1) the first positive HIV test (most common); (2) the first diagnosis of an opportunistic illness indicative of stage 3; (3) the first CD4 T-lymphocyte count or percentage meeting stage 3 criteria; or (4) the first “clinical” HIV diagnosis documented in a medical record without a preceding positive HIV test result in surveillance data. This definition ensures a consistent and objective determination of the diagnosis date for all cases, crucial for accurately calculating the time elapsed between diagnosis and viral load measurements and thus for the analysis of average HIV viral load at diagnosis.
Statistical Analysis
Viral load data were analyzed weekly for the first 6 weeks post-diagnosis. For each stage and stage 0 subcategory, we calculated the median, 25th percentile, and 75th percentile of the earliest viral loads within each week. Although individual patients were only observed at a single time point (the date of their earliest viral load measurement within 6 weeks), we assumed that aggregating data by week post-diagnosis would approximate a longitudinal series of weekly viral loads, reflecting the typical viral load trajectory in the study population. This approach is essential for understanding the dynamic changes in average HIV viral load at diagnosis and in the immediate weeks following.
Pairwise two-sample Wilcoxon comparisons were used to assess the statistical significance of differences in median viral loads between different stages. We used the PROC NPAR1WAY procedure in SAS 9.4 with the Dwass, Steel, Critchlow-Fligner option for multiple comparisons, adjusting significance thresholds using Holm’s method to account for the number of comparisons within each week. This rigorous statistical approach ensures the validity of our comparisons of average HIV viral load at diagnosis across different HIV stages and subcategories.
This analysis was deemed non-research by the CDC as it utilized de-identified data from routine public health surveillance, focusing on disease control purposes.
Results
Among the 115,297 infections included in the analysis, the distribution of stages at diagnosis was as follows: stage 0 accounted for 4.40% (5081), stage 1 for 26.80% (30,910), stage 2 for 37.10% (42,784), and stage 3 for 31.70% (36,522). This distribution highlights the relative proportions of diagnoses across the HIV disease spectrum in the dataset, providing context for interpreting the average HIV viral load at diagnosis in each stage.
The median earliest viral load for stage 0 infections showed a marked decline over the first six weeks post-diagnosis, starting at 694,000 copies/mL in week 1, decreasing to 125,022 in week 2, and further down to 43,473 by week 6 (Table 1, Figure 2). In contrast, stage 1 infections exhibited a relatively stable median earliest viral load, fluctuating between 15,412 and 17,495 copies/mL across the weeks. Stage 2 infections showed a gradual decrease from 44,973 copies/mL in week 1 to 38,497 in week 6. Stage 3 infections, while starting with a high median viral load of 205,862 copies/mL in week 1, also demonstrated a decrease to 119,000 copies/mL by week 6 (Table 2).
Table 1.
Median earliest viral load (in copies/mL) by week after diagnosis and stage of disease at diagnosis of HIV infection, for stages 0 and 1. (See Table 2 to compare with stages 2 and 3.)
| Week | Stage 0 | Stage 1 |
|---|---|---|
| N | Median | 25th-75th percentiles |
| 1st | 2635 | 694,000 |
| 2nd | 934 | 125,022 |
| 3rd | 629 | 70,886 |
| 4th | 408 | 55,734 |
| 5th | 277 | 52,067 |
| 6th | 198 | 43,473 |
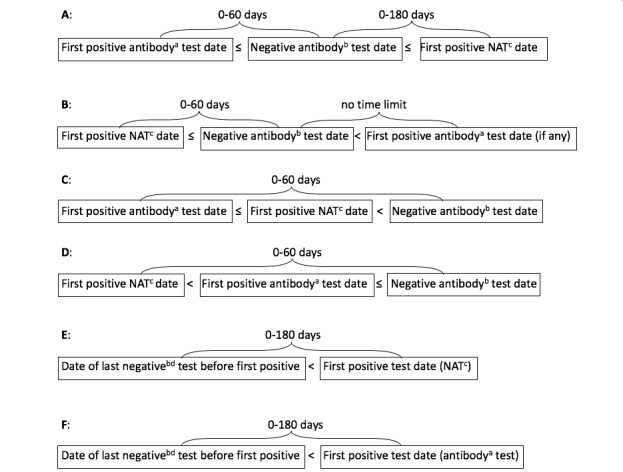
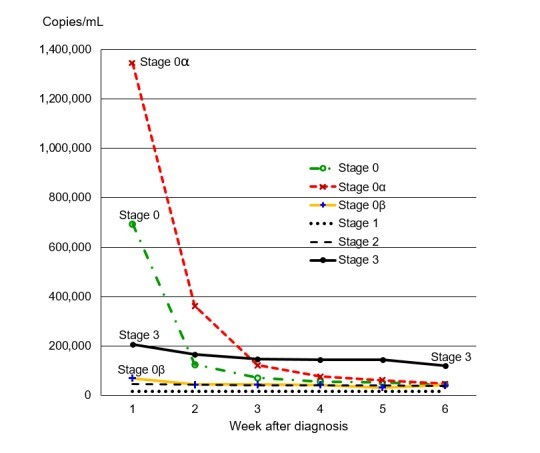
Table 1: Median earliest viral load for stages 0 and 1, demonstrating the significantly higher average HIV viral load at diagnosis in stage 0 during the initial weeks.
Figure 2.
Figure 2: Median earliest viral load by week after diagnosis, comparing HIV stages and stage 0 subcategories, visually representing the trends in average HIV viral load at diagnosis.
Table 2.
Median earliest viral load (in copies/mL) by week after diagnosis and stage of disease at diagnosis of HIV infection, for stages 2 and 3. See Table 1 to compare with stages 0 and 1.
| Week | Stage 2 | Stage 3 |
|---|---|---|
| N | Median | 25th-75th percentiles |
| 1st | 17,098 | 44,973 |
| 2nd | 8968 | 42,892 |
| 3rd | 6357 | 39,800 |
| 4th | 4523 | 40,045 |
| 5th | 3326 | 41,549 |
| 6th | 2512 | 38,497 |
Table 2: Median earliest viral load for stages 2 and 3, contrasting with stages 0 and 1 to emphasize the higher initial average HIV viral load at diagnosis in early stages.
In the first week post-diagnosis, the median earliest viral load for stage 0 was significantly higher than for stages 1, 2, and 3 (p<0.001 for all comparisons). Specifically, the median viral load in stage 0 was more than four times higher than in stage 2 and more than thirty times higher than in stage 1 in week 1. By week 3, however, the median viral load in stage 0 had decreased below that of stage 3 (p<0.001). These trends illustrate the dynamic nature of average HIV viral load at diagnosis in early infection compared to later stages.
Stage 0 Subcategory Viral Load Comparisons
In the first week after diagnosis, stage 0 preliminary subcategories 0A, 0B, 0C, 0D, and 0E showed median viral loads exceeding 1.2 million copies/mL, significantly higher than the 70,114 copies/mL for subcategory 0F (Tables 3-5). In week 2, median viral loads for subcategories 0A-0E remained elevated (>290,000 copies/mL) compared to subcategory 0F (44,467 copies/mL) and also higher than median viral loads for stages 1, 2, and 3 (p<0.01 for all comparisons except stage 3, p<0.05).
Table 3.
Median earliest viral load (in copies/mL) by week after diagnosis and stage of disease at diagnosis of HIV infection, for stage 0 preliminary subcategories 0A and 0B.
| Week | Subcategory 0A | Subcategory 0B |
|---|---|---|
| N | Median | 25th-75th percentiles |
| 1st | 1,083 | 1,258,925 |
| 2nd | 426 | 338,888 |
| 3rd-6th | 715 | 77,380 |
Table 3: Median earliest viral load for stage 0 subcategories 0A and 0B, illustrating the extremely high average HIV viral load at diagnosis in these acute infection subcategories.
Table 4.
Median earliest viral load (in copies/mL) by week after diagnosis and stage of disease at diagnosis of HIV infection, for stage 0 preliminary subcategories 0C and 0D.
| Week | Subcategory 0C | Subcategory 0D |
|---|---|---|
| N | Median | 25th-75th percentiles |
| 1st | 187 | 1,780,000 |
| 2nd | 76 | 635,690 |
| 3rd-6th | 71 | 75,300 |
Table 4: Median earliest viral load for stage 0 subcategories 0C and 0D, further highlighting the acute phase average HIV viral load at diagnosis.
Table 5.
Median earliest viral load (in copies/mL) by week after diagnosis and stage of disease at diagnosis of HIV infection, for stage 0 preliminary subcategories 0E and 0F.
| Week | Subcategory 0E | Subcategory 0F |
|---|---|---|
| N | Median | 25th-75th percentiles |
| 1st | 224 | 1,346,776 |
| 2nd | 17 | 294,798 |
| 3rd-6th | 16 | 135,540 |
Table 5: Median earliest viral load for stage 0 subcategories 0E and 0F, contrasting the average HIV viral load at diagnosis between subcategories within stage 0.
The higher viral loads in subcategories 0A-0E compared to 0F are partly explained by the shorter interval between the first positive test and the preceding negative/indeterminate test in subcategories 0A-0E. For subcategory 0E, the median interval was only 9 days, compared to 98 days for subcategory 0F.
Due to limited observations in later weeks for subcategories 0D and 0E, weeks 3-6 were combined in Tables 3-5. Based on the similar viral load trends in subcategories 0A-0E, they were combined into subcategory “0α,” while 0F was renamed “0β” for further analysis (Table 6), allowing for a clearer comparison of average HIV viral load at diagnosis between presumed acute (0α) and post-acute early (0β) infections.
Table 6.
Median earliest viral load (in copies/mL) by week after diagnosis and stage of disease at diagnosis of HIV infection, comparing stage 0 subcategory 0α with subcategory 0β.
| Week | Subcategory 0α (0A+0B+0C+0D+0E) | Subcategory 0β (0F) |
|---|---|---|
| N | Median | 25th-75th percentiles |
| 1st | 2027 | 1,344,590 |
| 2nd | 598 | 362,467 |
| 3rd | 375 | 122,970 |
| 4th | 243 | 77,100 |
| 5th | 177 | 61,414 |
| 6th | 120 | 47,320 |
Table 6: Median earliest viral load comparing stage 0 subcategories 0α and 0β, clearly demonstrating the difference in average HIV viral load at diagnosis between acute and post-acute early infection.
Median viral loads in subcategory 0α were significantly higher than in 0β for the first 4 weeks post-diagnosis (p<0.001 for weeks 1-3, p=0.008 for week 4). In weeks 5 and 6, the differences were not statistically significant (p>0.39). Subcategory 0α also had significantly higher median viral loads than stage 3 in weeks 1 and 2 (p<0.001) but lower in weeks 4-6 (p<0.001). In contrast, subcategory 0β consistently showed higher median viral loads than stage 2 in week 1 (p<0.001) and stage 1 across all weeks (p<0.001), highlighting the distinct viral load profiles and the importance of subcategorizing stage 0 when considering average HIV viral load at diagnosis.
Despite the generally higher viral loads in subcategory 0α, a proportion of infections in subcategory 0β and later stages also exhibited high viral loads. Earliest viral loads exceeding 500,000 copies/mL were observed in 11.6% of subcategory 0β, 4.20% of stage 1, 7.10% of stage 2, and 24.17% of stage 3 infections, compared to 50.0% in subcategory 0α.
Analysis of the decline in median viral loads in subcategory 0α showed similar trends between cases with missing ART start dates and those reported to have started ART after viral load measurement, suggesting that the observed viral load decline in early infection is largely independent of early ART initiation in this dataset and reflects the natural course of average HIV viral load at diagnosis and in the weeks immediately following.
Discussion
Key Findings and Implications
Our study robustly confirms that early HIV infection, represented by stage 0, is associated with significantly higher viral loads compared to infections diagnosed in later stages. This is particularly pronounced in the first week following diagnosis, where the median viral load in stage 0 is more than three times higher than in stage 3. This finding underscores the critical importance of early detection and intervention during this period of peak infectivity.
Furthermore, the differentiation of stage 0 into subcategories 0α and 0β provides valuable insights. Subcategory 0α, approximating acute infection, exhibits considerably higher viral loads than subcategory 0β, representing post-acute early infection. This distinction is crucial for public health prioritization. The higher viral loads in subcategory 0α justify targeted and urgent interventions, including immediate ART initiation and intensive partner services, to minimize onward transmission during the most infectious acute phase of HIV infection. The average HIV viral load at diagnosis in subcategory 0α signifies a heightened transmission risk, demanding immediate public health response.
The fact that 11.6% of infections in subcategory 0β and a smaller percentage in later stages also presented with viral loads exceeding 500,000 copies/mL suggests that high viral load, indicative of potential acute or recent infection, is not exclusive to stage 0α. This highlights the need for vigilance and consideration of viral load levels, even in diagnoses not classified as stage 0α, when prioritizing prevention interventions. A high average HIV viral load at diagnosis, regardless of stage classification, should trigger heightened attention for prevention efforts.
The observed decline in viral load in stage 0, particularly subcategory 0α, within the first few weeks post-diagnosis, appears to reflect the natural viral dynamics of acute HIV infection, rather than being solely attributable to ART initiation within this study timeframe. This natural decline, however, still leaves viral loads in early infection substantially higher than in later stages for a considerable period, emphasizing the ongoing transmission risk and the continued need for intervention beyond the immediate acute phase.
Comparison to Other Studies
Our findings regarding the average HIV viral load at diagnosis in early infection are consistent with previous research documenting high viral loads in acute HIV infection. The median viral load trajectory observed in our subcategory 0α closely aligns with that reported in a study of untreated individuals in Thailand, where peak viral loads in acute infection were followed by a decline but remained elevated for an extended period. This concordance strengthens the validity of our findings and reinforces the understanding of the natural history of viral load in early HIV infection.
In contrast, studies of individuals receiving immediate ART post-acute HIV diagnosis show a much more rapid and profound viral load suppression. This highlights the effectiveness of early ART in quickly reducing viral load and, consequently, transmission risk. Our study, focusing on viral load trends in a surveillance context, underscores the baseline viral load dynamics in the absence of immediate and universal ART initiation at diagnosis, providing a crucial perspective for public health strategies in diverse settings.
Implications for Public Health Intervention
The findings of this study have direct implications for public health resource allocation and intervention prioritization. Health departments, often facing resource constraints, can utilize this information to strategically target interventions to maximize their impact on HIV transmission prevention. Diagnoses in stage 0, especially subcategory 0α, should be prioritized for immediate linkage to care, counseling on transmission risk reduction, and comprehensive partner services. The significantly higher average HIV viral load at diagnosis in these early stages warrants this prioritization.
Given the rapid decline in viral load after the acute phase, but the continued elevation relative to later stages, interventions should ideally be initiated within the first two weeks post-diagnosis to capitalize on the period of highest infectivity. While stage 0α diagnoses warrant the highest priority, the presence of high viral loads in a subset of stage 0β and later-stage diagnoses suggests that viral load measurement at diagnosis can serve as an additional criterion for prioritizing interventions, ensuring that individuals with high transmission potential are promptly engaged in care and prevention services.
Furthermore, the classification of stage 0 into subcategories 0α and 0β, while analytically valuable, may be complex to implement in routine surveillance systems. However, our findings support the utility of distinguishing between acute and post-acute early infections for public health purposes. Enhancements to NHSS software to automatically classify these subcategories could aid health departments in more effectively targeting prevention efforts based on the estimated recency of infection and associated average HIV viral load at diagnosis.
Limitations
This study has several limitations. Our analysis relies on the completeness and accuracy of HIV test result reporting to the NHSS. Underreporting of negative or indeterminate test results, crucial for stage 0 classification, may lead to misclassification of early infections into later stages, potentially underestimating the prevalence and impact of high viral loads in acute infection. This limitation may affect the precise quantification of average HIV viral load at diagnosis in stage 0, but the overall trends and comparisons remain robust.
The wide range observed in viral loads within each stage and week post-diagnosis may be partly attributable to misclassification of stage “at diagnosis.” The staging criteria for stages 1, 2, and 3 allow for CD4 count measurements up to 3 months post-diagnosis, during which time CD4 levels and viral loads can fluctuate, introducing variability in stage assignment and potentially affecting the precision of average HIV viral load at diagnosis estimates for each stage.
Our study population, while large, may not be fully representative of all US residents with HIV infection. Demographic differences exist between the included and excluded populations, although these differences are unlikely to invalidate the core findings regarding stage-specific viral load trends. The large sample size and consistent trends observed across stages and subcategories strengthen the generalizability of our conclusions regarding average HIV viral load at diagnosis.
Finally, our analysis uses cross-sectional viral load data aggregated weekly to approximate longitudinal trends. While ethically and practically challenging to obtain, longitudinal viral load data from untreated individuals would provide a more direct assessment of viral load dynamics in early infection. However, our approach, utilizing a large surveillance dataset, provides a valuable and robust estimation of average HIV viral load at diagnosis and its trajectory in the weeks following diagnosis within a real-world public health context.
Conclusions
In conclusion, this study confirms that infections in early HIV infection (stage 0) are associated with significantly higher viral loads, particularly in the first week after diagnosis, compared to later stages. Subcategory 0α of stage 0 exhibits even higher viral loads than subcategory 0β in the initial weeks. These findings underscore the critical need to prioritize interventions for individuals diagnosed with early HIV infection, especially those in subcategory 0α or presenting with high viral loads at diagnosis. Public health efforts should focus on ensuring rapid linkage to care, effective prevention counseling, and comprehensive partner services for these individuals, ideally within the first two weeks of diagnosis, to maximize the impact of interventions in reducing HIV transmission. Understanding the average HIV viral load at diagnosis is paramount for guiding effective and targeted public health strategies to control the HIV epidemic.
Abbreviations
ART: Antiretroviral Treatment
CDC: Centers for Disease Control and Prevention
HIV: Human Immunodeficiency Virus
NAT: Nucleic Acid Test
NHSS: National HIV Surveillance System
Footnotes
Conflicts of Interest: None declared.