Bilateral parotid swelling, while not the most common condition, presents a diagnostic puzzle for healthcare professionals. Understanding the diverse range of potential causes is crucial for accurate diagnosis and effective management. This article provides an in-depth exploration of bilateral parotid swelling, focusing on differential diagnosis and utilizing a multimodality imaging approach to aid in clinical decision-making.
Understanding Bilateral Parotid Swelling
The parotid glands, the largest of the salivary glands, are located in front of and below each ear. Swelling in these glands, particularly when it occurs on both sides (bilateral), can be indicative of a variety of underlying health issues. While sometimes the cause is clinically obvious, such as in cases of mumps, many other conditions can manifest as bilateral parotid swelling, requiring careful investigation.
This guide aims to explore these conditions, categorized for clarity and diagnostic ease. We will delve into infectious, inflammatory, systemic, and neoplastic causes, highlighting key imaging features that assist in differentiating between them. Imaging modalities such as MRI, CT, ultrasonography, and sialography play a vital role in visualizing the parotid glands and identifying specific characteristics associated with different pathologies.
Table 1: Differential Diagnosis of Bilateral Parotid Swelling
| Category | Specific Conditions |
|---|---|
| Inflammation or Infection | |
| Bacterial | Acute Suppurative Parotitis (less common bilaterally) |
| Viral | Mumps, HIV Sialopathy |
| Chronic | Chronic Sialadenitis, Chronic Recurrent Parotitis |
| Autoimmune Diseases | Sjögren’s Disease |
| Granulomatous Diseases | Sarcoidosis, Wegener’s Granulomatosis, Kimura’s Disease |
| Miscellaneous | |
| Metabolic/Systemic | Sialadenosis (Diabetes, Hypothyroidism, Malnutrition) |
| Cystic | Polycystic Disease |
| Environmental | Pneumoparotid, Radiation Sialadenitis |
| Neoplastic Diseases | |
| Benign | Papillary Cystadenoma Lymphomatosum (Warthin Tumor) |
| Malignant | Mucosa-Associated Lymphoid Tissue (MALT) Lymphoma |
| Pseudolesion | |
| Muscular | Masseteric Hypertrophy |
Infectious Causes
Acute Suppurative Parotitis
Acute suppurative parotitis is typically a bacterial infection that often presents with unilateral swelling. However, bilateral involvement can occur in 15–25% of cases, particularly in individuals who are debilitated, dehydrated, or have poor oral hygiene. This condition arises from bacteria ascending through the salivary ducts.
Imaging, while not always necessary, can be helpful in complicated cases. CT scans may reveal dilated central ducts, ductal wall enhancement, and gland enlargement. MRI can show variable signal intensity on T2-weighted images depending on the balance of edema and cellular infiltration, along with diffuse glandular enhancement post-contrast.
Viral Parotitis (Mumps)
Mumps, caused by the paramyxovirus, is a classic and common cause of viral parotitis, especially in children under 15. Characteristically, mumps presents with bilateral parotid swelling in about 75% of cases. Clinical diagnosis is usually straightforward, and imaging is generally not required. However, if imaging is performed, CT may show non-specific gland enlargement with increased attenuation, while MRI may reveal increased T2 signal intensity.
HIV Sialopathy
Parotid enlargement can be seen in approximately 5% of HIV-positive individuals. Diffuse infiltrative lymphocytosis syndrome (DILS), a subset of HIV, is often associated with bilateral parotid swelling. This swelling is due to lymphoproliferation within intraparotid lymph nodes. Benign lymphoepithelial lesion (BLEL) cysts can develop later in the disease course.
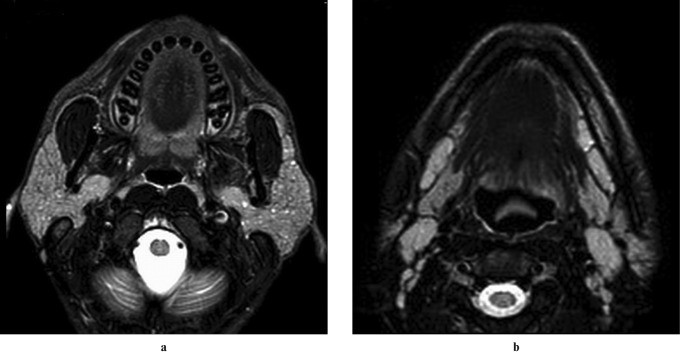
Ultrasound can detect anechoic/hypoechoic areas with debris and septa (BLEL cysts) and enlarged hypoechoic intraparotid nodes. CT and MRI findings are non-specific, showing multiple cystic and solid masses within the parotid glands, potentially along with tonsillar hypertrophy and cervical lymphadenopathy.
Figure 2: Axial T2-weighted MRI images showing bilateral parotid enlargement with multiple hyperintense foci, indicative of HIV-associated lymphoepithelial cysts. Enlarged cervical nodes are also visible. Alt text: T2 MRI of parotid glands in HIV patient showing cysts and lymph nodes.
Chronic Inflammatory Conditions
Chronic Sialadenitis
Chronic sialadenitis involves ongoing inflammation of the salivary gland tissue, often leading to drainage system alterations and increased infection susceptibility. This can result in progressive ductal dilatation and salivary gland enlargement, often presenting clinically as intermittent, sometimes painful, swelling, which may or may not be related to eating.
Imaging demonstrates dilated main parotid and intraglandular ducts. Figure 1 illustrates the typical imaging findings in chronic sialadenitis.
Figure 1: Axial T2-weighted, HASTE axial, and HASTE sagittal oblique MRI images showing dilated main parotid duct and intraglandular branches bilaterally in a child with chronic parotitis. Alt text: MRI of dilated parotid ducts in chronic sialadenitis.
Chronic Recurrent Parotitis (CRP)
Chronic recurrent parotitis is a less common inflammatory condition of unknown origin, characterized by repeated episodes of parotid swelling, which can be unilateral or bilateral, and may or may not involve pain. Onset is typically in childhood, between 2 and 7 years.
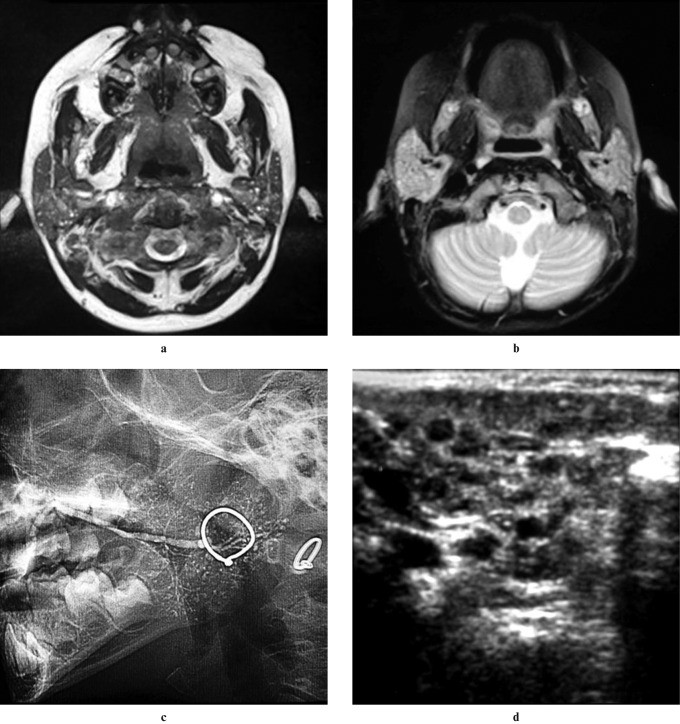
Ultrasound is useful for diagnosis, revealing multiple small hypoechoic or anechoic lesions corresponding to punctate sialectasis seen on sialography. Imaging helps differentiate CRP from conditions like benign lymphoepithelial cysts and juvenile Sjögren syndrome.
Figure 3: Axial T2-weighted MRI, 3D CISS MIP MRI, digital sialography, and axial ultrasound illustrating multiple high-signal foci and punctate collections of contrast material in bilateral parotid glands of a child with chronic recurrent parotitis. Alt text: Imaging findings in chronic recurrent parotitis of childhood.
Sjögren’s Syndrome (SS)
Primary Sjögren’s syndrome is an autoimmune disorder characterized by lymphocytic infiltration of exocrine glands, leading to dry eyes and mouth. Major salivary gland enlargement, often bilateral, occurs in a significant percentage of patients. Diagnosis is based on clinical findings, biopsy, and autoantibody detection.
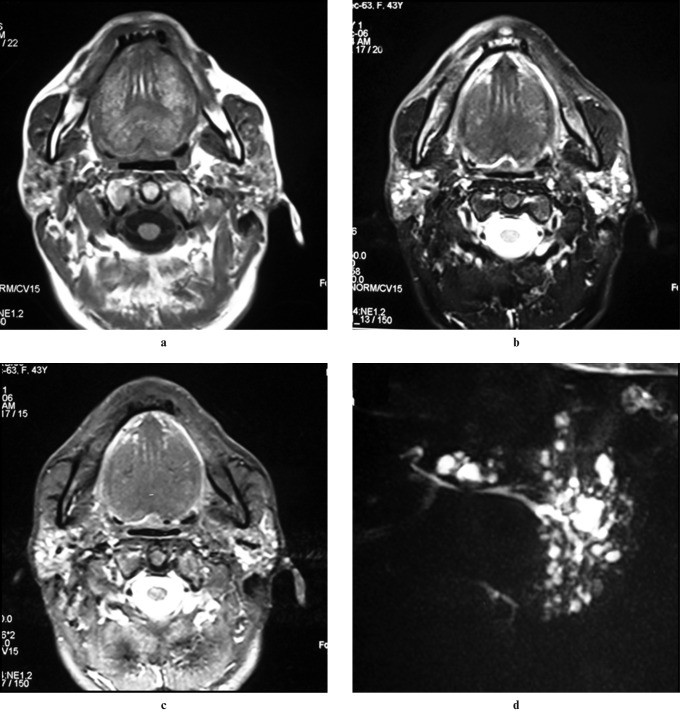
Sialography is sensitive for diagnosing SS, showing early punctate sialectasis progressing to globular collections and cavitary sialadenitis. Ultrasound in advanced SS shows inhomogeneous glands with hypoechoic areas and increased blood flow. CT reveals enlarged glands with cystic areas (honeycomb appearance). MRI in advanced SS also shows a “salt and pepper” or “honeycomb” appearance with mixed signal intensities. Fatty infiltration in parotid glands is also a characteristic finding in SS. Increased risk of parotid lymphoma is associated with SS.
Figure 4: Axial T1-weighted, fat-suppressed T2-weighted, and STIR MRI images showing fatty infiltration and sialectasis in bilateral parotid glands in a patient with Sjögren’s syndrome. Alt text: MRI features of Sjögren’s syndrome in parotid glands.
Figure 5: Contrast-enhanced CT and T1-weighted MRI images showing lymphoma in the right parotid gland of a patient with Sjögren’s syndrome. Adenopathy is also noted. Alt text: Parotid lymphoma in Sjögren’s syndrome patient.
Granulomatous Diseases: Sarcoidosis, Wegener’s Granulomatosis, and Kimura’s Disease
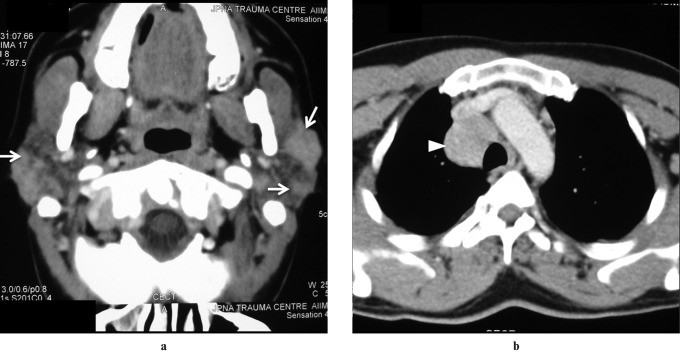
Sarcoidosis: This systemic disorder of unknown cause often presents with painless bilateral parotid enlargement in 10–30% of patients. Imaging findings are non-specific but may show multiple non-cavitatory masses representing enlarged intraparotid nodes on ultrasound and CT. Diffuse enlargement with increased T2 signal and enhancement on MRI can also be seen. Classic “panda sign” on Gallium-67 scintigraphy (increased uptake in lacrimal and parotid glands) may be present.
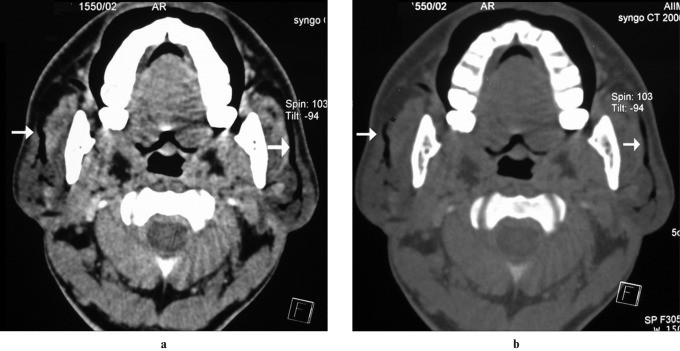
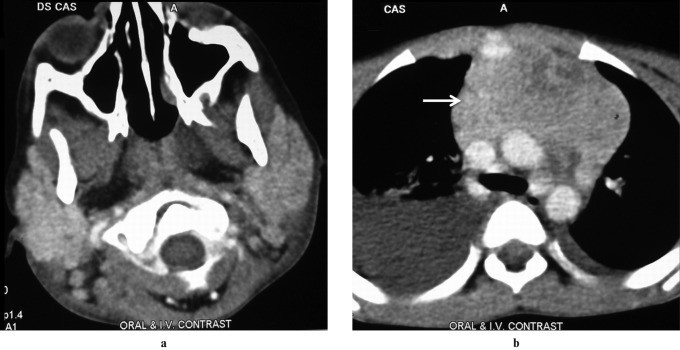
Figure 7: Contrast-enhanced CT image showing symmetrically enlarged parotid glands with multiple focal hyperdense lesions in a patient with sarcoidosis. Thoracic CT shows paratracheal node enlargement. Alt text: CT imaging of parotid sarcoidosis.
Figure 8: T2-weighted and post-contrast T1-weighted MRI images showing symmetrically enlarged parotid and lacrimal glands with increased signal intensity and diffuse enhancement in sarcoidosis. Alt text: MRI of parotid and lacrimal gland sarcoidosis.
Wegener’s Granulomatosis: Salivary gland involvement in Wegener’s granulomatosis is rare and not isolated. Patients typically have respiratory symptoms. Parotid involvement can be unilateral or bilateral with non-specific imaging findings. Diagnosis relies on clinical presentation, histology, and ANCA assay.
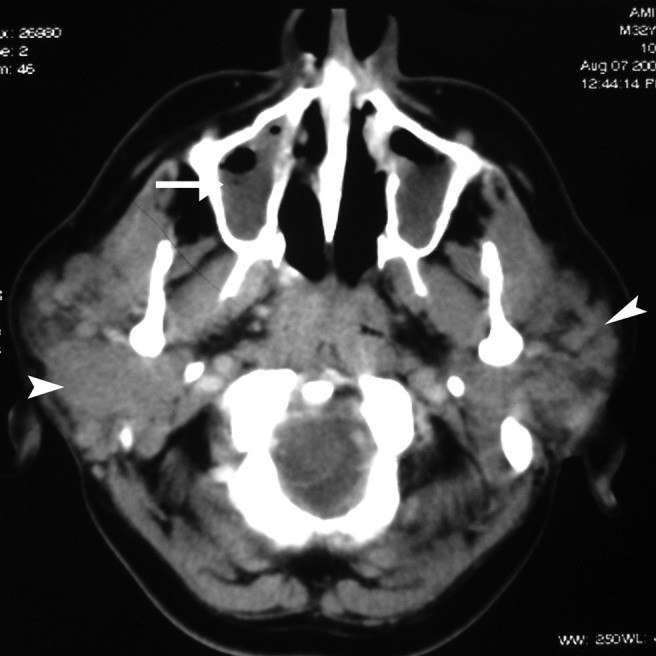
Figure 6: Contrast-enhanced CT image showing enlarged bilateral parotid glands with multiple focal lesions in a patient with Wegener’s granulomatosis and maxillary sinusitis. Alt text: CT of parotid swelling in Wegener’s granulomatosis.
Kimura’s Disease: This immune-mediated inflammatory disease can involve salivary glands, either unilaterally or bilaterally. Imaging findings are non-specific, showing enhancing intraparotid masses and potentially cervical nodes on CT. MRI signal intensity is variable.
Miscellaneous Causes
Sialadenosis
Sialadenosis is a non-inflammatory, painless, persistent bilateral swelling, particularly of the parotids, associated with systemic conditions like diabetes, endocrinopathies, malnutrition, certain medications, and alcohol abuse. Imaging is usually not helpful as findings are variable. Sialography may show enlarged glands with splayed ducts. Clinical history is key to diagnosis.
Figure 9: Digital sialogram and axial T2-weighted MRI demonstrating symmetrically enlarged parotid glands without focal lesions in a patient with sialadenosis due to hypothyroidism. Alt text: Imaging of sialadenosis in hypothyroidism.
Polycystic (Dysgenetic) Disease
Polycystic disease of the parotid glands is rare, often bilateral, and seen mainly in females, presenting with recurrent painless swelling. Imaging (ultrasound, CT, MRI) clearly shows bilateral enlargement with multiple cystic areas replacing glandular parenchyma.
Pneumoparotid
Pneumoparotid occurs due to increased intraoral pressure, such as from playing wind instruments or dental work, causing air to enter the parotid gland and duct. It presents as facial swelling, which can be unilateral or bilateral, possibly with crepitus. CT elegantly demonstrates air within the duct and gland.
Figure 10: Axial CT images showing air within bilateral main and intraparenchymal ducts, diagnostic of pneumoparotid. Alt text: CT scan of pneumoparotid showing air in ducts.
Radiation Sialadenitis
Radiation sialadenitis follows radioactive iodine (I131) treatment for thyroid carcinoma, causing transient bilateral parotid swelling within 24 hours of treatment, resolving spontaneously within a week. Clinical diagnosis is sufficient, and imaging is not needed.
Neoplastic Causes
Lymphoma
Primary salivary gland lymphoma, particularly MALT lymphoma, is rare. Secondary lymphoma is slightly more common. Most are B-cell non-Hodgkin lymphomas. Imaging features vary from focal masses (enlarged intraparotid nodes) to diffuse glandular infiltration. CT and MRI can help delineate the extent of disease and identify extraparotid nodal involvement.
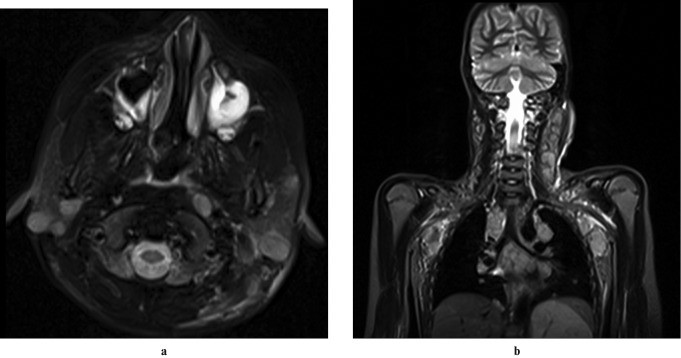
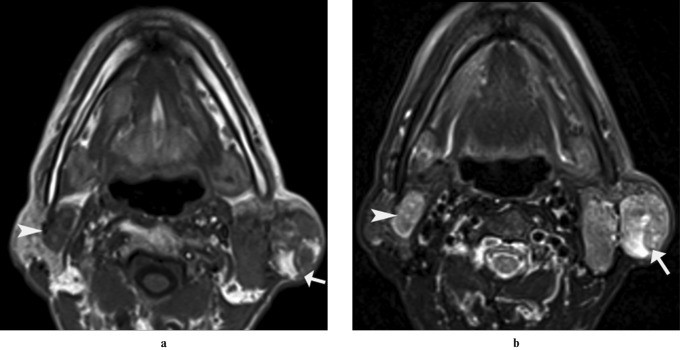
Figure 11: Axial and coronal T2-weighted MRI images showing multiple focal hyperintense lesions in bilateral parotid glands and nodes in jugular chain, axilla, and mediastinum in a child with non-Hodgkin lymphoma. Alt text: MRI of parotid lymphoma with nodal involvement.
Figure 12: Contrast-enhanced CT images showing symmetrically enlarged parotid glands and anterior mediastinal mass with pleural effusion in a child with non-Hodgkin lymphoma. Alt text: CT of diffuse parotid lymphoma and mediastinal mass.
Warthin’s Tumor
Warthin’s tumor (papillary cystadenoma lymphomatosum) is a benign epithelial tumor and the most common salivary neoplasm to present bilaterally (up to 10% of cases). It manifests as a painless, slow-growing mass. Ultrasound shows a well-defined hypoechoic mass, often cystic. MRI reveals a partially cystic mass with characteristic signal intensities. Bilateral or multiple parotid masses are highly suggestive of Warthin’s tumor.
Figure 13: Axial T1-weighted and T2-weighted MRI images showing multiple well-defined focal lesions involving bilateral parotid glands, consistent with bilateral Warthin’s tumors. Alt text: MRI of bilateral Warthin’s tumors.
Pseudolesion
Benign Masseteric Hypertrophy
Bilateral masseteric hypertrophy, enlargement of the masseter muscles, can mimic parotid enlargement. Clinically, it gives the face a rectangular appearance. Radiographically, bony hyperplasia at the mandibular angle may be seen. Sialography may show lateral displacement and narrowing of Stensen’s duct. Cross-sectional imaging reveals enlarged masseter muscles with normal tissue characteristics.
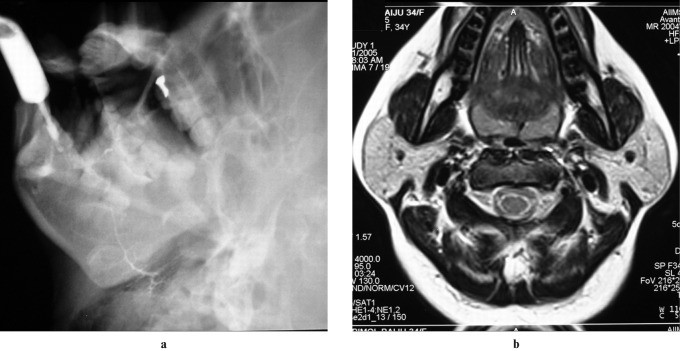
Figure 14: Clinical photograph, digital sialogram, and axial CT showing bilateral masseteric hypertrophy. Sialogram shows narrowing of the parotid duct, and CT shows enlarged masseter muscles. Alt text: Imaging of masseteric hypertrophy mimicking parotid swelling.
Conclusion
Bilateral parotid swelling encompasses a wide range of differential diagnoses, from common infections like mumps to rarer conditions such as sarcoidosis and lymphoma. Imaging plays a crucial role in the diagnostic process, often suggesting the nature of the underlying pathology. Conditions like chronic recurrent parotitis, Sjögren’s syndrome, HIV sialopathy, Warthin’s tumor, lymphoma, and sarcoidosis can often be suggested based on distinctive imaging features. Pseudolesions like masseteric hypertrophy can be confidently identified with imaging. While imaging findings may be less specific in conditions like sialadenosis and Wegener’s granulomatosis, they remain a valuable tool in conjunction with clinical evaluation and laboratory findings.
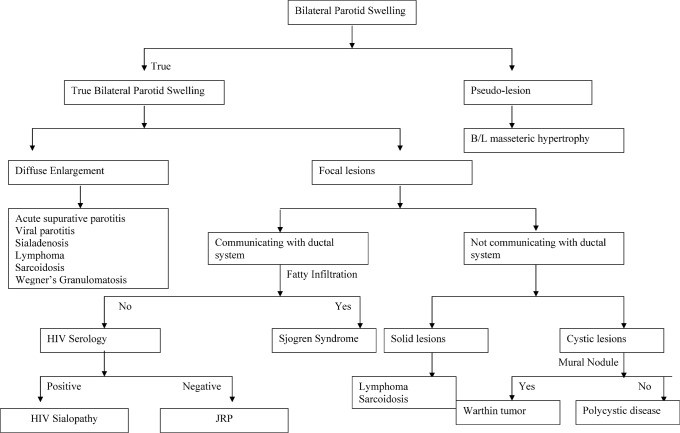
The algorithmic approach to bilateral parotid swelling, incorporating clinical history, physical examination, and appropriate imaging, is essential for accurate diagnosis and management.
Figure 15: Algorithmic approach to diagnosing bilateral parotid swelling, emphasizing the role of clinical evaluation and imaging modalities. Alt text: Diagnostic algorithm for bilateral parotid swelling.