Introduction
Bronchiolitis obliterans-organizing pneumonia (BOOP), currently known as cryptogenic organizing pneumonia (COP), is recognized for its diverse range of radiological manifestations. Typically, hilar or mediastinal lymphadenopathy is not considered a common feature in the radiological spectrum of COP. This article presents a unique case of a patient diagnosed with idiopathic BOOP who exhibited extensive bilateral hilar and mediastinal lymphadenopathy, initially mimicking sarcoidosis and posing a significant diagnostic challenge. This case underscores the importance of considering COP in the differential diagnosis of bilateral hilar lymphadenopathy, even when clinical and radiological findings strongly suggest alternative conditions.
Case Presentation
A 37-year-old African American woman, with a history of hypertension but not on medication, presented with a six-week history of persistent dry cough, intermittent low-grade fever, night sweats, fatigue, weakness, and exertional dyspnea. She had migrated from Jamaica to the USA five years prior. Her medical history was unremarkable for orthopnea, paroxysmal nocturnal dyspnea, exposure to toxic gases or organic dust, weight loss, appetite changes, fever with joint pain, or any history of smoking, although she reported social alcohol consumption.
Upon admission, her vital signs revealed a temperature of 100.2°F, a pulse rate of 113 beats per minute, a respiratory rate of 18 breaths per minute, and a blood pressure of 150/80 mm of Hg. Her oxygen saturation was notably low, with a partial pressure of oxygen at 60 mm of Hg on room air. The rest of her physical examination was unremarkable. Initial laboratory investigations showed a white blood cell count of 11,600 cells/μL with a differential of 82% granulocytes and 13% lymphocytes. Hemoglobin was 11.6 g/dl with a mean corpuscular volume of 82 femtoliters. The platelet count was elevated at 518,000 cells/μL, and inflammatory markers were raised, with an erythrocyte sedimentation rate of 117 mm/hr and a C-reactive protein of 7 mg/dl.
A chest radiograph revealed nodular infiltrates in the bilateral upper lobes and peri-hilar fullness, prompting further investigation with a CT scan. The CT scan of the chest (Figure 1) demonstrated extensive bilateral hilar and mediastinal lymphadenopathy, along with areas of perihilar and peripheral consolidation. Pulmonary function tests indicated a mild restrictive pattern.
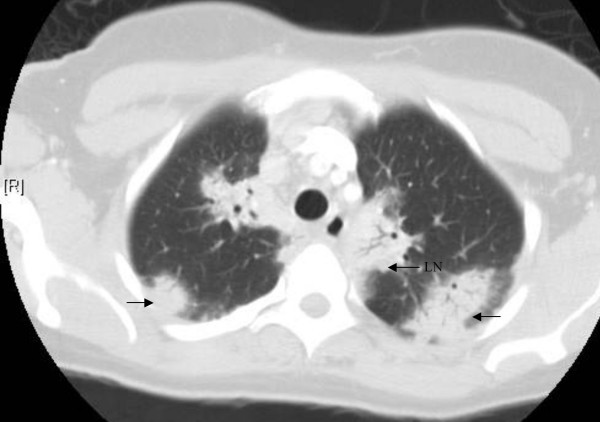 CT scan of the chest revealing bilateral hilar and mediastinal lymphadenopathy, perihilar and peripheral consolidations
CT scan of the chest revealing bilateral hilar and mediastinal lymphadenopathy, perihilar and peripheral consolidations
Differential diagnoses considered at this stage included atypical pneumonia, tuberculosis, fungal or opportunistic infections, sarcoidosis, interstitial lung disease, connective tissue and autoimmune diseases, lymphoma, and occult malignancy. The patient was initially treated with erythromycin and ceftriaxone for presumed atypical pneumonia, which was later changed to moxifloxacin due to lack of clinical improvement. However, she showed no response to these antibiotic regimens. Repeated blood and sputum cultures for bacteria, mycobacteria, and fungi were consistently negative. Tuberculin skin test (PPD) and HIV ELISA test were also negative. Further serological testing for rheumatoid factor, anti-nuclear antibodies, and anti-neutrophil cytoplasmic antibody were negative. A CT scan of the abdomen and pelvis was unremarkable, ruling out widespread malignancy or other systemic involvement.
To further investigate the lymphadenopathy, a mediastinal lymph node biopsy was performed. The biopsy revealed reactive anthracosis but no evidence of granulomas or malignant cells, which was initially not supportive of sarcoidosis, although this diagnosis remained high on the differential list given the patient’s clinical presentation, radiological findings, age, and ethnicity, as sarcoidosis is more prevalent in African Americans.
Ultimately, an open lung biopsy was performed to obtain a definitive diagnosis. Histopathological examination of the lung tissue (Figure 2) showed sharply demarcated patchy fibrosed areas with fibrotic plugs and a mixed inflammatory infiltrate composed of lymphocytes, plasma cells, macrophages, neutrophils, and foamy macrophages. These findings were consistent with Bronchiolitis obliterans organizing pneumonia (BOOP), now termed cryptogenic organizing pneumonia (COP) [1]. Following the diagnosis, the patient was commenced on oral prednisone at a dose of 1 mg/kg/day. She exhibited a dramatic clinical and radiological improvement within 8 weeks of steroid therapy. The prednisone dosage was gradually tapered and discontinued after 12 months. During a one-year follow-up period, the patient remained asymptomatic, with no recurrence of her respiratory symptoms.
Discussion
The histopathological findings and the significant clinical and radiological response to steroid therapy strongly support the diagnosis of COP in this patient. However, the initial clinical and radiological presentation was highly suggestive of sarcoidosis. Differentiating COP from sarcoidosis can be challenging, as both conditions can present with similar clinical features, including cough, dyspnea, and fatigue. Radiologically, both conditions can manifest with bilateral perihilar and peripheral consolidations. However, extensive bilateral hilar and mediastinal lymphadenopathy is a hallmark radiological feature of sarcoidosis and is not typically associated with COP.
While COP is known to have a wide spectrum of radiological presentations, mediastinal lymphadenopathy is rarely reported. A literature review indicates that mediastinal lymphadenopathy in COP is uncommon. A study investigating the prevalence of mediastinal lymphadenopathy in BOOP at the University of British Columbia found that while COP can be associated with enlarged mediastinal lymph nodes, it usually involves only a limited number of lymph nodes, typically not more than two [2]. In contrast, the patient in this case presented with extensive mediastinal lymphadenopathy, a finding atypical for COP. Gupta et al. [3] described a case of BOOP with hilar lymphadenopathy, suggesting that these findings might represent pneumonic foci in the hilar or peri-hilar regions. However, extensive bilateral mediastinal lymphadenopathy combined with bilateral hilar lymphadenopathy, characteristic of sarcoidosis, has not been previously reported in association with COP.
The etiology of COP is largely idiopathic. While COP has been reported in association with sarcoidosis, particularly as a complication of lung transplantation in patients with end-stage pulmonary disease [4] and in alveolar sarcoidosis [5], idiopathic COP mimicking the presentation of sarcoidosis, especially with prominent bilateral hilar and mediastinal lymphadenopathy, is exceedingly rare.
Considering the negative results of extensive investigations for other etiologies, the characteristic histopathological findings of lung biopsy, the lack of response to antibiotics, the dramatic improvement with steroid treatment, and the patient’s sustained good health post-treatment, we conclude that this patient had idiopathic COP. The prominent bilateral hilar and mediastinal lymphadenopathy in this case represents an atypical and diagnostically challenging presentation of COP, initially leading to a strong consideration of sarcoidosis in the differential diagnosis of bilateral hilar lymphadenopathy.
Conclusion
This case report highlights a rare presentation of bronchiolitis obliterans-organizing pneumonia (BOOP), or cryptogenic organizing pneumonia (COP), with extensive bilateral hilar and mediastinal lymphadenopathy. This case demonstrates that COP can clinically and radiologically mimic sarcoidosis, and therefore, COP should be included in the differential diagnosis of bilateral hilar lymphadenopathy, particularly when other typical features of sarcoidosis are not definitively present or when clinical course is atypical. This report expands the known radiological spectrum of COP and emphasizes the importance of considering less common manifestations of pulmonary diseases in challenging diagnostic scenarios, especially in the context of Bilateral Hilar Lymphadenopathy Differential Diagnosis.
Abbreviations
BOOP – Bronchiolitis obliterans organizing pneumonia
COP – Cryptogenic organizing pneumonia
PPD – Purified protein derivative
HIV – Human Immunodeficiency virus
ELISA – Enzyme-linked immunosorbent assay
Competing interests
The authors declare that they have no competing interests.
Authors’ contributions
SV: Conception of the case report, data collection, literature review, and manuscript writing. SG and RE: Data collection. JT: Pathologic diagnosis and data collection. NM: Coordination and manuscript drafting. All authors read and approved the final manuscript.
Acknowledgements
Meekoo Dhar, MD. Consent was obtained from the patient for publication of this study.
Contributor Information
Seema Varma, Email: svarma@siuh.edu.
Shilpi Gupta, Email: sgupta@siuh.edu.
Raymond Elsoueidi, Email: elsoueidimd@yahoo.com.
Meekoo Dhar, Email: mdhar@siuh.edu.
Jotica Talwar, Email: jtalwar@siuh.edu.
Neville Mobarakai, Email: nmobarakai@siuh.edu.
References
- American Thoracic Society; European Respiratory Society. American Thoracic Society/European Respiratory Society international multidisciplinary consensus classification of the idiopathic interstitial pneumonias. Am J Respir Crit Care Med. 2002;165(2):277–302.
- Rademaker J, ખાન S, મિત્તલ R, et al. Mediastinal lymphadenopathy in bronchiolitis obliterans organizing pneumonia: prevalence and predictors. Eur Respir J. 2001;18(Suppl 33):239s.
- Gupta P, Guleria R, Singh N, et al. Bronchiolitis obliterans organizing pneumonia with hilar lymphadenopathy mimicking tuberculosis. Indian J Chest Dis Allied Sci. 2004;46(4):289–92.
- Verleden GM, Ruttens D, Vandecasteele SJ, et al. Organizing pneumonia after lung transplantation: a clinicopathological study. Am J Respir Crit Care Med. 2001;164(6):992–5.
- Ichikawa Y, Kinoshita M, Nishimura M, et al. Bronchiolitis obliterans organizing pneumonia associated with alveolar sarcoidosis. Intern Med. 1993;32(12):979–82.