Cervicogenic dizziness (CGD) is a recognized clinical condition characterized by dizziness associated with neck pain. Notably, there are no definitive tests to confirm CGD, making it a diagnosis of exclusion. Distinguishing CGD from other conditions causing dizziness, such as vestibular, medical, and vascular disorders, demands significant expertise and a comprehensive understanding of appropriate diagnostic procedures. Accurate differentiation is crucial to rule in or rule out alternative diagnoses effectively. This article provides a structured, stepwise diagnostic approach designed to aid healthcare practitioners in the accurate diagnosis of cervicogenic dizziness. This guide outlines a systematic process for evaluating patients suspected of CGD and details the necessary steps to exclude conditions that mimic CGD symptoms. These mimicking conditions include central and peripheral vestibular disorders, vestibular migraine, labyrinthine concussion, cervical arterial dysfunction, and whiplash-associated disorder.
Keywords: Cervicogenic dizziness, Cervical dizziness, Disequilibrium, Vertigo, Cervical spine, Cervical proprioception, Whiplash, Diagnosis
Background
The term ‘cervical vertigo’ was first introduced by Ryan and Cope in 1955 to describe what is now known as cervicogenic dizziness (CGD). Despite its recognition, CGD has historically been a subject of debate within the medical community [1]. Other terms previously used to describe this condition include proprioceptive vertigo, cervicogenic vertigo, and cervical dizziness. However, given that true vertigo is rarely a primary symptom in CGD, the preferred term is now cervicogenic dizziness [2].
Cervicogenic dizziness is clinically defined by symptoms such as imbalance, unsteadiness, disorientation, neck pain, and restricted cervical range of motion (ROM). Headaches may also accompany these symptoms [2, 3]. A diagnosis of CGD is considered when the cervical spine is suspected as the source of dizziness after all other potential causes have been eliminated. Crucially, for a diagnosis of CGD, dizziness must be temporally linked to changes in neck position or cervical joint movement [4]. While the exact cause of CGD remains unclear, many diagnosed cases follow whiplash injuries or are linked to inflammatory, degenerative, or mechanical impairments within the cervical spine [5, 6].
The underlying mechanisms causing imbalance, unsteadiness, and disorientation in CGD are not fully understood. A prominent theory suggests that impaired cervical proprioceptive input plays a significant role [7]. It is hypothesized that disruptions in normal sensory signals from upper cervical proprioceptors to the vestibular nucleus lead to inaccurate spatial perception of head and neck orientation [8]. Pain itself is also considered a potential source of these aberrant sensory signals [6].
Currently, CGD is a diagnosis of exclusion. This type of diagnosis is applied when no single diagnostic test can confirm the condition, and its presence cannot be verified through definitive outcomes, imaging, lab results, or unique signs and symptoms [9]. Diagnoses of exclusion pose challenges for clinicians, requiring advanced clinical reasoning and a strong command of test sequencing to effectively rule out or rule in competing diagnoses. The differential diagnosis is complicated by the wide array of potential causes of dizziness, including medications, and various vestibular, cardiovascular, metabolic, neurological, psychological, and visual disorders. Therefore, a structured, stepwise approach to exclude conditions that present with symptoms similar to CGD is invaluable for accurate differential diagnosis.
Reneker and colleagues [10] conducted a Delphi study to evaluate the perceived usefulness of different clinical tests in distinguishing between cervicogenic dizziness and dizziness from other causes following sports-related concussion. Their findings revealed a lack of consensus among healthcare professionals regarding which tests are most appropriate for identifying CGD. This lack of agreement spanned across different healthcare disciplines. Given the complexity of CGD, a systematic diagnostic process is essential for effective differential diagnosis. This article aims to present a stepwise process for diagnosing CGD, utilizing a rule-out, rule-in framework. The selection and sequence of assessment tools remain at the clinician’s discretion, allowing for tailored application based on individual patient presentations.
Main Text
Our proposed stepwise clinical reasoning process for diagnosing CGD is illustrated in Figure 1. Ruling out alternative diagnoses requires tests with low negative likelihood ratios (LR-) and high sensitivity. These are crucial for minimizing the probability of missing a condition when the test result is negative. Conversely, tests with high positive likelihood ratios (LR+) and high specificity are used to rule in a condition. Table 1 provides an overview of the sensitivities, specificities, and likelihood ratios of relevant diagnostic tests. Table 2 details the descriptions and explanations of these tests. The subsequent sections provide detailed background information and explanations for each step in the diagnostic process.
Fig. 1.
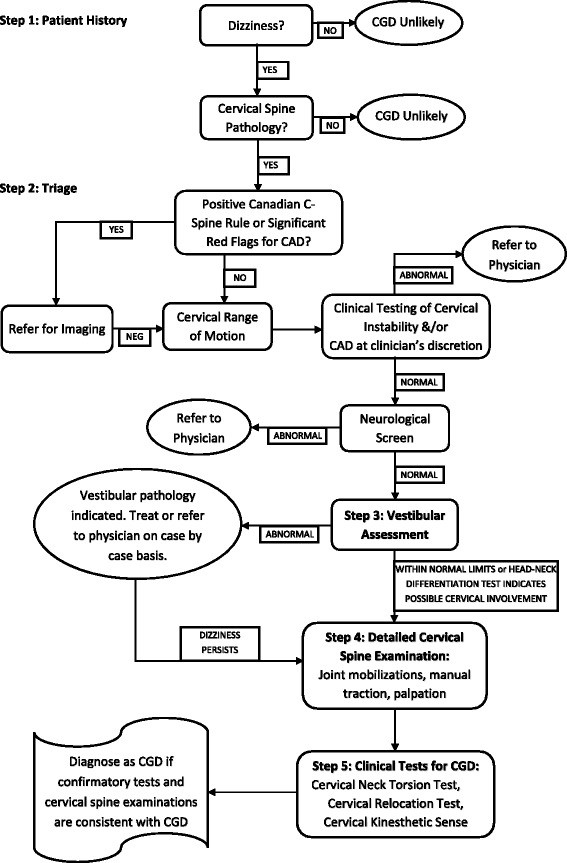 Stepwise algorithm for diagnosing cervicogenic dizziness
Stepwise algorithm for diagnosing cervicogenic dizziness
Figure 1: Stepwise algorithm designed for the diagnosis of cervicogenic dizziness, guiding clinicians through a structured process of assessment and exclusion.
Table 1.
Diagnostic Accuracy of Tests
| Test | Diagnosis | Sensitivity (%) | Specificity (%) | PV+ (%) | PV- (%) | LR+ | LR- | Reference |
|---|---|---|---|---|---|---|---|---|
| Canadian C-Spine Rule | Cervical Spine Trauma | 99 | 45 | 6.03 | 100 | 1.81 | 0.01 | Stiell et al. [36]; Duane et al. [37] |
| Cervical Arterial Dysfunction (CAD) Test | CAD | 0–57 | 87–100 | 0–100 | 26–96 | 0.22–83.3 | 0.44–1.4 | Hutting et al. [22]; Petersen et al. [38] |
| Sharp Purser Test | Transverse Ligament Stability | 69 | 96 | 85 | 90 | 15.6 | 0.33 | Uitvlugt & Indenbaum [39]; Hutting et al. [40] |
| Alar Ligament Test | Alar Ligament Stability | Right: 69Left: 72 | Right: 100Left: 96 | Right: 100Left: 93 | Right: 80Left: 81 | – | – | Kaale et al. [41] |
| Dix-Hallpike | Posterior Canal BPPV | 79.3 | 75 | 95.8 | 33.3 | 3.17 | 0.14 | Halker et al. [42] |
| Head Thrust Test | Unilateral Vestibular Hypofunction | 71 (88 for complete loss) | 82 | 87 | 65 | 4.16 | 0.3 | Schubert et al. [43] |
| Manual Spinal Examination | Cervical Facet Joint Dysfunction | 92 | 71 | – | – | 3.17 | 0.11 | Schneider et al. [30] |
| Palpation for Segmental Tenderness | Cervical Facet Joint Mediated Pain | 94 | 73 | – | – | 3.48 | 0.08 | Schneider et al. [30] |
| Cervical Neck Torsion Test | Cervicogenic Dizziness (versus BPPV) | 72 | 92 | – | – | 9 | 0.3 | L’Heureux-Leabeau et al. [14] |
| Cervical Relocation Test (with positive test defined by any of the 4 positions with JPE >4.5°) | Cervicogenic Dizziness (versus BPPV) | 92 | 54 | – | – | 2 | 0.15 | L’Heureux-Leabeau et al. [14] |
| Cervical Relocation Test (with positive test defined by mean JPE >4.5°) | Cervicogenic Dizziness (versus BPPV) | 72 | 75 | – | – | 2.9 | 0.37 | L’Heureux-Leabeau et al. [14] |
| Smooth Pursuit Neck Torsion (SPNT) Test | CGD in people with WAD and dizziness | 902756 | 915588 | 92—- | 71—- | 100.6– | 0.111.3– | L’Heureux-Leabeau et al. [14]Tjell & Rosenhall [34]Kongsted et al. [35] |
Table 1: This table summarizes the diagnostic accuracy of various clinical tests used in the differential diagnosis of cervicogenic dizziness and related conditions.
Table 2.
Test Descriptions
| Diagnosis | Test | Performance description | Explanation |
|---|---|---|---|
| Traumatic Cervical Spine Injury | CanadianC-Spine Rule[44] | 1) Any high-risk factor present: Age ≥ 65 years OR Dangerous mechanism* of injury OR Paresthesias in extremities. If YES to any, radiography should be performed. If NO to all, continue to 2.2) Any low risk factor that allows safe assessment of range of motion? If NO to all, radiography should be performed; if YES to any, continue to 3. Low risk factors defined as: Simple rear-end motor vehicle collision† OR Sitting position in emergency department OR Ambulatory at any time OR Delayed (not immediate) onset of neck pain OR Absence of midline cervical spine tenderness.3) Able to actively rotate neck 45° left and right? If unable, radiography should be performed.*Fall from elevation ≥0.9 m (3 ft)/five stairs, axial load to head, motor vehicle collision at high speed (>100 km/h), rollover, ejection, motorized recreational vehicles, bicycle struck, or bicycle collision.†Excludes: pushed into oncoming traffic, hit by bus or large truck, rollover, and hit by high speed vehicle. | Canadian C-Spine Rule is a tool to help clinicians decide if radiography should be utilized in patients following traumatic injury. It is only applicable to patients who are alert (Glasgow Coma Scale score ≥ 15) and in stable condition following trauma where cervical spine injury is a concern. Canadian C-Spine Rule is not applicable in non-trauma cases, for patients with age |
| Upper Cervical Instability | Alar Ligament Test [45] | 1) Patient assumes sitting or supine position with head slightly flexed to engage the Alar ligament. The clinician assesses the patient’s resting symptoms.2) The clinician firmly stabilizes the spinous process of C2 using a pincer grasp.3) Either lateral flexion or rotation is passively performed by the clinician (both are performed independently of each other, in either order). While performing these passive movements, the examiner attempts to feel movement of C2.4) A positive test is defined by lack of palpable movement of the C2 spinous process during lateral flexion or rotation. | The purpose of this test is to examine the integrity of the alar ligaments following traumatic injury involving the cervical spine. If the alar ligaments are intact, lateral flexion or rotation of the head should result in palpable contralateral movement of the C2 spinous process. Caution is of utmost importance when administering this test. |
| Upper Cervical Instability | Sharp Purser Test [39, 45] | 1) The patient assumes a sitting position with their head slightly flexed. The clinician assesses the patient’s resting symptoms.2) The clinician stands to one side of the patient and stabilizes the C2 spinous process using a pincer grasp.3) The clinician uses the opposite hand to gently apply an anterior to posterior translation force on the patient’s forehead.4) A positive test is defined by symptom reproduction during forward flexion, decrease in symptoms during posterior translation, or excessive displacement (>4 mm) during posterior translation. | This test assesses the integrity of the transverse ligament that maintains the position of the odontoid process relative to C1. If the transverse ligament is torn, C1 will translate forward on C2 during flexion, indicating atlantoaxial subluxation. Atlantoaxial subluxation is the most common cervical spine complication of rheumatoid arthritis. Spinal cord compression secondary to atlantoaxial subluxation can result in severe neurological damage, including quadriplegia and fatality. Extreme caution should be used when administering this test. |
| Cervical Facet Joint Dysfunction | Manual Spinal Examination [30] | Patient positioned in prone with neutral cervical spine. Clinician applies posterior to anterior directed force to the articular pillars of the cervical spine bilaterally, one joint at a time. In a study by Schneider, et al., a positive test was defined as patient report of ≥3/10 increase in concordant local or referred pain intensity when clinician rated resistance to motion as ‘moderate’ to ‘marked’. | Cervical facet joint capsules contain several sensory receptors including free nerve endings, mechanoreceptors, A-delta and C-fibers, making the joints nociceptive and sensitive to pressure and mechanical changes. |
| Cervical Facet Joint Mediated Pain | Palpation for Segmental Tenderness [30] | Patient positioned in prone. Clinician palpates deep segmental muscles overlying cervical spine facet joints bilaterally. Schneider, et al. defined a positive test as patient report of ≥3/10 increase in concordant local or referred pain intensity rating. | Segmental muscles overlying painful facet joints often react with tenderness and spasm. Cervical facet joints and the muscles overlying them are innervated by the medial branch of the dorsal rami. |
| Cervical Arterial Dysfunction | CAD Testing [22, 46] | CAD testing should include the following sequential tests:1) While seated, the patient performs end range active cervical rotation in both directions.2) While seated, the patient performs active end range combined cervical extension and rotation in both directions3) With patient supine, the clinician brings the patient into passive end range cervical rotation in both directions.4) With patient supine, the clinician brings the patient into passive end range combined cervical extension and rotation in both directions.5) Any position that the patient reports as provocative.All positions should be held for a minimum of 10 s, unless symptoms are provoked sooner. After each sustained position, the patient should return to neutral cervical spine position for at least 10 s to allow for any latent response to emerge. Throughout CAD testing, the clinician should observe the patient’s eyes for nystagmus, and the patient should report any provocation of symptoms. Positive signs and symptoms include dizziness, nystagmus, diplopia, loss of consciousness, diaphoresis, dysphagia, dysarthria, nausea, numbness around the lips, or other neurological symptoms. | CAD testing involves neck rotation and extension with a stationary body, causing decreased blood flow in the vertebrobasilar arteries with rotation alone and internal carotid arteries with combined extension and rotation. CAD testing requires cervical extension and rotation passive range of motion that is within normal limits. |
| Vestibular Hypofunction | Head Thrust Test [43] | Grasp the patient’s head firmly with both hands and pitch their head forward 30° to align the horizontal semicircular canals. Instruct the patient to look at your nose. Gently move the patient’s head back and forth with intermittent high velocity, randomly timed thrusts. | While performing head thrusts, observe the patient’s eyes to determine whether they are able to maintain ocular fixation on your nose or not. A failure to maintain fixation on the visual target (nose) indicates hypofunction on the side that the thrust was directed toward. A refixation saccade will be visible for patients who are unable to maintain visual fixation. This test is most valid if the thrusts are performed with random timing that does not allow anticipatory compensation. |
| Peripheral Vestibular Dysfunction | Head Shaking Induced Nystagmus [47] | Grasp the patient’s head firmly with both hands and pitch their head forward 30° to align the horizontal semicircular canals. Instruct the patient to close their eyes. Passively oscillate the patient’s head side to side 20 times at 1–2 Hz. Instruct them to open their eyes just prior to completing the 20 side to side movements. Observe for post-headshake nystagmus. | The direction of the fast phase of nystagmus denotes the side of higher vestibular functioning. Therefore, the side of vestibular hypofunction is on the side contralateral to the direction of the fast phase. |
| Benign Paroxysmal Positional Vertigo | Dix-Hallpike Test [42] | The patient is initially sitting upright with legs extended. The clinician passively rotates the patient’s head 45° toward the side being tested. The clinician helps the patient to rapidly lie down on the table while keeping the head slightly extended. The clinician observes the patient’s eyes for nystagmus for at least 60 s; there can be a latency period of up to 15 s before the onset of nystagmus. | The direction of the nystagmus beats will be on the same side as the involved canal. With right sided BPPV, for example, the fast phase of nystagmus will beat to the right with a slow saccade back to the left. Patients with posterior canal BPPV will have a positive Dix-Hallpike test and concomitant vertigo. |
| Horizontal Canalilithiasis or Cupulolithiasis | Head Roll Test [48] | The patient is initially positioned in supine with their neck flexed 20°. The clinician quickly rotates the patient’s head 90° to either side and observes for nystagmus for at least 60 s. The clinician slowly returns the patient’s head to midline, maintaining neck flexion, then repeats the procedure on other side. | Like the Dix- Hallpike, the nystagmus will beat towards the affected ear with a slow saccade moving in the opposite direction following the fast beat of nystagmus. When the head is rolled toward the affected ear, the nystagmus beats will be in a geotropic (toward the ground) manner. If the head is maintained in this position, a burst of fast beating nystagmus will occur in an ageotropic (away from the ground) fashion. When the head is rolled away from the affected ear, the nystagmus beats will be less intense and in the geotropic fashion. |
| Vestibular Dysfunction, Cervicogenic Dizziness | Head-Neck Differentiation Test [26–28] | The patient begins seated on a swivel chair. The clinician rotates the chair both while the stabilizing patient’s head and the patient reports any provocation of dizziness. The clinician then rotates the chair without stabilizing the patient’s head and the patient again reports any provocation of dizziness. | Provocation of dizziness with trunk rotation under a stabilized head implicates the cervical spine, whereas dizziness with head and trunk rotation together (en bloc rotation) indicates a vestibular component to the patient’s symptoms. If symptoms are provoked in both scenarios, it is likely that CGD and vestibular dysfunction are comorbid. Dizziness of vertebral origin should be ruled out prior to administration of the Head-Neck Differentiation Test. |
| Cervicogenic Dizziness | Cervical Neck Torsion Test [14] | The patient begins seated on a swivel chair and turns their trunk 90° to the either the right or left, holding for 30 s, then returns their trunk to center. The patient then repeats the same process in the opposite direction. Each position, including the center positions, is maintained for 30 s. Throughout the test, the head is stabilized by the clinician and therefore motionless. The clinician also must continuously observe for nystagmus. | Considered positive if nystagmus (excluding spontaneous nystagmus) of more than 2° per second is observed in any of the four positions (left trunk rotation, neutral rotation, right trunk rotation, neutral rotation). |
| Cervicogenic Dizziness, Whiplash Associated Disorder | Smooth Pursuit Neck Torsion Test (SPNT) [34, 49] | Surface electrodes are placed on the subject’s skin just lateral to the eyes bilaterally to record the corneo-retinal potential. The subject begins seated with their cervical spine in neutral position. The subject watches a visual target (LED or laser light) that moves through a 40° arc at a frequency of 0.2 Hz with a peak velocity of 20° per second. The subject is instructed to keep their head still and try not to blink while following the light closely with their eyes. The examiner gently holds the subject’s head in place. This process is then repeated with the subject’s body rotated 45° to one side with the head remaining in the same position to create cervical torsion. If 45° of trunk rotation causes discomfort, the angle can be decreased to symptom free range (minimum of 30°). The examiner gently holds the subject’s head and trunk in the position. The test is performed to the left and right sides. The mean gain (i.e. the ratio between eye velocity and target velocity) is calculated in all three positions. | There is a lack of consensus in the description of proper performance methodology of the SPNT. The methods described are based on the initial study of the SPNT performed by Tjell and Rosenhall in 1998. The SPNT is a test of smooth pursuit eye movement with cervical neck torsion. The SPNT is the average value of the smooth pursuit in both the right and left trunk-rotation positions. The difference between the smooth pursuit and the smooth pursuit with neck torsion values is called the smooth pursuit neck torsion difference. The larger the difference between smooth pursuit with neck torsion and smooth pursuit in neutral, the more likely the patient is suffering from a whiplash associated disorder. The utility of the SPNT as a diagnostic tool for differentiating CGD from WAD has been studied in controlled laboratory trials, with mixed results, but has not yet been studied in a clinical setting. |
| Cervicocephalic Proprioception and Neck Reposition Sense | Cervical Relocation Test [32] | The patient begins seated, facing a wall 90 cm away, and wearing a head-mounted laser pointer that is centered on a target on the wall. The patient keeps their eyes closed while moving their neck in a specified direction, then back to what they believe to be centered starting position. The patient verbally indicates when they believe they are back to center. The patient repeats this process for right rotation, left rotation, flexion, and extension (in no particular order). | The mean distance from the actual center to the subjective center is used to calculate the joint position error (JPE) for each movement. An error of 4.5° is the cutoff point suggesting a failure of head and neck relocalization precision. |
Table 2: Detailed descriptions of tests used in the diagnosis of cervicogenic dizziness, including procedures, positive test criteria, and clinical relevance.
Stepwise Process for Diagnosing Cervicogenic Dizziness
Step 1: Patient History – Unraveling the Narrative
Taking a detailed patient history is the crucial first step in determining the likelihood of CGD. It is essential to thoroughly explore the patient’s symptoms and the circumstances of their onset. For CGD to be considered, the patient should typically present with a history of neck problems alongside dizziness that emerges in close temporal proximity to the neck symptoms. It is important to note that CGD is unlikely in the absence of neck pain. This neck pain can be present at rest, during movement, or upon palpation. Symptoms related to CGD should be aggravated by movements that provoke neck pain and relieved by interventions that alleviate neck pain.
A comprehensive patient history serves multiple critical purposes: identifying red flags, initiating the process of ruling out alternative diagnoses, and prioritizing conditions that best align with the patient’s reported onset, signs, and symptoms. Table 3 outlines the typical clinical presentations of CGD and other conditions that may present with similar symptoms. Key information to gather from patients experiencing both dizziness and neck pain includes cardiovascular risk factors, history of migraines, symptoms of tinnitus or aural fullness, oscillopsia, and symptom exacerbation related to exertion, positional changes, busy environments, or specific activities.
Table 3.
Differentiating Cervicogenic Dizziness from Competing Diagnoses
| Diagnosis | Duration | Signs and symptoms |
|---|---|---|
| Acute Vestibular Loss | Single attack, several attacks, or persistent for several weeks. | Sudden vertigo or dizziness possibly accompanied by tinnitus, diplopia, nausea, vomiting [15]. |
| Benign ParoxysmalPositional Vertigo | A few seconds to several minutes. | Vertigo. Occurs with changes in position relative to gravity [50]. |
| Central Vestibular Disorders | Several days to weeks. | Constant vertigo, facial asymmetry, swallowing or speech problems, ptosis, ataxia, sensation changes, upper motor neuron signs, abnormal head thrust test, direction changing nystagmus, pure vertical nystagmus, pure torsional nystagmus, a skew deviation, and other neurological symptoms [23, 51]. |
| Cervical Arterial Dysfunction | Several minutes. | Dizziness that is typically accompanied by diplopia, numbness around the lips, nystagmus, ataxia, bilateral neurological symptoms, dysphagia, dysarthria and headaches. Associated with nausea and vomiting [19]. |
| Cervicogenic Dizziness | Several minutes to hours [3]. | Dizziness and disequilibrium due to changes in cervical spine position [3]. |
| Labyrinthine Concussion | Episodically over hours to days [26]. | Cervical neck pain is common. Hearing loss, tinnitus, and dizziness [18]. |
| Ménière’s Disease | Minutes to hours, rarely longer than 24 h [12]. | Presents with episodic, intense vertigo, accompanied by aural fullness, tinnitusand fluctuating hearing loss. Attacks are typically preceded by aura and followed by a period of exhaustion and generalized dizziness. As Ménière’s disease progresses, the hearing loss and tinnitus intensify and become more persistent, and the acute attacks of vertigo may be replaced by more chronic problems with dizziness and imbalance [12, 13]. |
| Vestibular Migraine | 4–72 h. | Vestibular Migraine Diagnostic Criteria (International Headache Society) [17]. A. At least five episodes involving criteria C and D. B. A current or past history of Migraine without aura or Migraine with aura. C. Vestibular symptoms* of moderate or severe intensity, lasting between 5 min and 72 h. D. At least 50% of episodes are associated with at least one of the following three migrainous features: 1) headache with at least two of the following four characteristics: unilateral location, pulsating quality, moderate or severe intensity, aggravation by routine physical activity; 2) photophobia and phonophobia; 3) visual aura. E. Not better accounted for by another ICHD-3 diagnosis or by another vestibular disorder.*Barany Society’s Classification of Vestibular Symptoms:a. spontaneous vertigo: i. internal vertigo (a false sensation of self-motion) ii. external vertigo (a false sensation of visual surroundings spinning or flowing)b. positional vertigo, triggered by a complex or large moving stimulusc. visually induced vertigo, triggered by a complex or large moving visual stimulusd. head motion-induced vertigo, occurring during head motione. head motion-induced dizziness with nausea |
| Whiplash Associated Disorder | Variable. Days to weeks and in some cases months. | Cervical neck pain and hypersensitivity, decreased cervical range of motion, dizziness, tinnitus, and headache. Associated with psychological factors, such as low pain tolerance and fear avoidance [21]. |
Table 3: Clinical presentations of cervicogenic dizziness compared with other conditions that can cause similar symptoms, aiding in differential diagnosis.
The nature of the patient’s symptoms provides critical clues to the underlying cause of dizziness. It is crucial to clarify the patient’s perception of “vertigo” or “dizziness,” as these terms are often used inconsistently. Dorland’s Illustrated Medical Dictionary [11] defines vertigo as an illusion of motion, either of the external environment revolving around the individual (objective vertigo) or of the individual rotating in space (subjective vertigo). True vertigo is typically associated with peripheral vestibular disorders or lesions within the central nervous system’s vestibular pathways, not primarily from cervical spine issues.
Symptom duration is another vital aspect of the patient history that helps differentiate CGD from other conditions. CGD symptoms can persist from minutes to hours within an episode, and these episodes can recur over days, months, or even years [3]. Table 3 provides typical symptom durations for various conditions associated with dizziness.
Several vestibular conditions present with characteristic symptoms that can help distinguish them from CGD. Ménière’s disease, a chronic vestibular disorder, is marked by episodic attacks of aural fullness, intense vertigo, and fluctuating hearing loss [12, 13]. In contrast, CGD typically does not involve aural fullness, tinnitus, or hearing loss. While these symptoms do not definitively confirm Ménière’s disease, their presence reduces the likelihood of CGD.
Benign paroxysmal positional vertigo (BPPV) is the most prevalent vestibular disorder. BPPV occurs when otoconia (calcium carbonate crystals) dislodge from the utricle and migrate into one of the semicircular canals of the inner ear. BPPV is characterized by vertigo triggered by changes in head position relative to gravity, accompanied by nystagmus. The nystagmus pattern in BPPV is typically mixed up-beating and torsional, with the direction varying based on the affected semicircular canal. If a patient experiences vertigo with nystagmus in response to head position changes, BPPV is more likely than CGD. A comparative study between BPPV and CGD revealed that sensations of “drunkenness” and “fainting” were reported in both groups, but significantly more often in the CGD group. Conversely, rotatory sensations and symptom durations lasting only seconds were more common in the BPPV group [14]. Cervical neck movements, fatigue, anxiety, and stress were also identified as more frequent triggers for symptom exacerbation in CGD compared to BPPV.
Patients with acute, unilateral peripheral vestibular loss, such as from labyrinthitis or vestibular neuritis, usually present with pronounced vertigo and imbalance, accompanied by nausea and possibly vomiting. Acutely, they exhibit spontaneous horizontal, direction-fixed nystagmus observable in room light. As acute symptoms subside, patients may experience residual dizziness, motion sensitivity, imbalance, concentration difficulties, tinnitus, and hearing loss [15]. This symptom profile aids in differentiating vestibular loss from CGD, as CGD typically does not include tinnitus, hearing loss, or true vertigo.
Vestibular migraines are recognized as a common cause of recurrent vertigo [16]. The International Headache Society criteria for diagnosing vestibular migraine are detailed in Table 3. Key symptoms more indicative of vestibular migraine than CGD include aura, true vertigo, throbbing headaches, sensitivity to auditory or visual stimuli, and oculomotor changes [17]. Dizziness in vestibular migraine is not typically associated with mechanical neck pain or cervical dysfunction.
Labyrinthine concussion, a vestibular disorder, can mimic CGD symptoms due to the overlap of dizziness and neck pain [3]. Differentiating between CGD and labyrinthine concussion is challenging because both can result from trauma. Labyrinthine concussion often shares symptoms with peripheral vestibular loss, including hearing loss, tinnitus, and dizziness [18].
Cervical arterial dysfunction (CAD) and whiplash-associated disorder (WAD) are non-vestibular conditions that can resemble CGD. Cervical arterial dysfunction, sometimes incorrectly used interchangeably with vertebrobasilar insufficiency (VBI), actually refers to restricted blood flow in any cervical artery, including the internal carotid arteries, not just the vertebrobasilar arteries [19]. VBI specifically denotes reduced blood flow in the vertebrobasilar arteries. CAD can arise from various underlying conditions such as atherosclerosis, thrombosis, anatomical anomalies, cervical arterial dissection, vasospasm, and external compression. Clinicians should assess patients for cardiovascular risk factors that increase CAD likelihood, such as hypertension, hypercholesterolemia, blood clotting disorders, diabetes mellitus, smoking, vessel trauma, or a history of cardiac or vascular disease [19]. CAD-related dizziness typically lasts minutes and is associated with head and trunk movements [19]. Isolated dizziness without other CAD symptoms is rare; CAD-related dizziness presents as a sole symptom in less than 1% of cases [20]. Other CAD symptoms include severe headache, diplopia, nystagmus, perioral numbness, dysphagia, dysarthria, and upper motor neuron signs [19].
Whiplash-associated disorder (WAD) develops following rapid acceleration/deceleration trauma, commonly from motor vehicle accidents. WAD patients often exhibit low pain tolerance and high scores on fear-avoidance measures like the Fear Avoidance Belief Questionnaire (FABQ). Common WAD symptoms include neck pain and hypersensitivity, reduced cervical ROM, dizziness, tinnitus, and headache [21]. Dizziness in WAD can sometimes be cervicogenic. WAD may also coincide with concussion from the same trauma. Thus, WAD, concussion, and CGD are not mutually exclusive diagnoses. Dizziness experienced as a symptom of concussion or WAD may originate from cervical structures.
Step 2: Triage – Prioritizing Safety and Ruling Out Critical Conditions
In cases where the patient history includes blunt trauma, cervical spine triage should begin with the Canadian C-Spine Rule to determine the necessity for radiography. The criteria for this rule are detailed in Table 2. The Canadian C-Spine Rule is highly sensitive, effectively minimizing the risk of incorrectly clearing a patient with a significant cervical spine injury from radiographic evaluation. If the patient reports significant red-flag symptoms suggestive of CAD, referral for diagnostic imaging is necessary to rule out cervical artery involvement as a cause of dizziness. Clinical tests for cervical instability and CAD are inherently provocative and should be performed cautiously and judiciously. Positive findings on these tests necessitate immediate medical attention and imaging [22].
If imaging is not indicated based on the Canadian C-Spine Rule or CAD red flags, the next step is to assess cervical range of motion (ROM). Cervical ROM assessment at this stage is practical because several subsequent vestibular tests (Step 3) require a minimum degree of cervical mobility. Furthermore, identifying ROM limitations or symptom provocation during active or passive cervical movements provides valuable early diagnostic information. For instance, if dizziness is provoked by cervical extension rather than rotation, the Cervical Neck Torsion Test, which primarily uses rotation, might be deprioritized in favor of other clinical tests more relevant to extension-related dizziness.
Given that patients being evaluated for CGD often present with dizziness of unknown origin and may have a history of trauma, a neurological screening is generally warranted. This screen should include assessment for radicular symptoms, myotomes, dermatomes, deep tendon reflexes, upper motor neuron signs, and cranial nerve function. Abnormal neurological findings may necessitate referral to a neurologist or emergency care, depending on the severity and nature of the findings. Central vestibular disorders can manifest with diverse symptoms, from persistent vertigo to non-specific dizziness, often accompanied by red-flag signs that require medical referral [23].
Once cervical instability, CAD, and neurological dysfunction are effectively ruled out, the clinician should proceed with clinical tests aimed at excluding vestibular pathologies.
Step 3: Vestibular Assessment – Evaluating the Inner Ear System
Following a history suggestive of CGD and appropriate triage, the vestibular system should be evaluated. Prior to vestibular testing, a basic cervical spine assessment is necessary, including confirmation of neck pain from Step 1 and ROM and radicular symptom assessment from Step 2. Vestibular tests can be adapted to accommodate any limitations in cervical ROM. A comprehensive cervical spine evaluation is optimally performed in Step 4. Ruling out vestibular dysfunction first increases the probability that the cervical spine is the source of dizziness. However, Steps 3 and 4 may overlap depending on the patient’s presentation. For example, in cases of clear vestibular causes of dizziness (e.g., BPPV, vestibular hypofunction) without acute cervical involvement, vestibular pathology treatment would precede Step 4. Conversely, significant cervical ROM restrictions hindering vestibular pathology treatment would necessitate cervical spine assessment and treatment before or concurrently with addressing the vestibular issue.
Vestibular function assessment should include oculomotor evaluations, specifically nystagmus, skew deviation, smooth pursuit, saccades, Dix-Hallpike test, static and dynamic visual acuity, and the vestibulo-ocular reflex (VOR), including VOR cancellation and the head thrust test. Observing nystagmus is clinically significant for determining vestibular system involvement; its presence during testing can help rule out CGD.
Horizontal, direction-fixed nystagmus is indicative of unilateral peripheral vestibular hypofunction. Patients with this condition typically exhibit oculomotor signs like a positive head thrust test or head-shaking induced nystagmus and may have abnormal dynamic visual acuity—findings not typical in CGD. The absence of spontaneous or gaze-evoked nystagmus in room light does not exclude peripheral vestibular deficit, as visual fixation can suppress nystagmus in these cases. Frenzel lenses can enhance detection of unilateral peripheral vestibular hypofunction by removing visual fixation. Individuals compensated for unilateral loss may show no nystagmus in room light, while those with bilateral vestibular loss generally show no nystagmus even with visual fixation removed. Nystagmus from central pathology presents differently, being present in room light and persisting or diminishing with removal of visual fixation. Direction-changing, purely vertical, or torsional nystagmus suggests a central vestibular deficit.
Other oculomotor abnormalities, such as saccadic smooth pursuit or saccadic intrusions, may indicate central vestibular and oculomotor deficits. While some studies report abnormal eye movements in WAD, findings vary significantly [24, 25]. No single oculomotor test definitively diagnoses CGD.
The Head-Neck Differentiation Test, a variation of the Cervical Neck Torsion Test, can differentiate between CGD and vestibular dizziness [26–28]. This test involves rotating a seated patient’s trunk while stabilizing their head and noting dizziness provocation. Dizziness during trunk rotation with a stabilized head points to cervical spine involvement, whereas dizziness with en bloc head and trunk rotation suggests a vestibular component. If symptoms are provoked in both scenarios, CGD and vestibular dysfunction may coexist, requiring management of both.
While static and dynamic balance tests are not diagnostic for vestibular dysfunction, they are often abnormal in vestibular disorders [28, 29]. Studies also show cervical pain can impair balance and postural control [8]. Patients with vestibular dysfunction or CGD may show increased symptoms during dynamic balance assessments. Although not diagnostic for either condition, balance assessment is important for functional evaluation.
Positive vestibular test results do not exclude CGD, as patients can have both. If vestibular dysfunction is found, treatment may be initiated, and referral to an otolaryngologist or neurologist may be considered based on the patient’s presentation. If vestibular treatment does not fully resolve dizziness, or if the Head-Neck Differentiation Test suggests both cervical and vestibular involvement, CGD should be considered, and Step 4 should be pursued.
Step 4: Detailed Cervical Spine Evaluation – Pinpointing Cervical Involvement
While cervical ROM and instability testing are part of triage, a thorough cervical spine evaluation ideally follows vestibular testing to rule out vestibular dysfunction and narrow down potential dizziness causes. Cervical evaluation includes Manual Spinal Examination (MSE) for facet joint dysfunction, Palpation for Segmental Tenderness (PST), postural assessment, and traction.
No single test definitively diagnoses cervical facet joints as a pain source. However, MSE and PST have shown high sensitivity (92% and 94%, respectively) as screening tools for cervical facet joint-mediated pain [30]. MSE involves unilateral posterior-to-anterior mobilization of cervical facet joints, assessing pain provocation and motion resistance. PST involves palpating muscles over cervical facet joints, assessing for tenderness. CGD patients often present with tight posterior neck muscles and tenderness in posterior neck muscles and cervical facet joints. A study by L’Heureux-Leabeau et al. [14] found CGD patients more likely to experience pain during upper cervical spine and paravertebral muscle examination compared to BPPV patients.
Postural alignment and control assessment is important as postural impairments are common in CGD, especially post-whiplash neck pain [8]. Dizziness symptom reduction with cervical traction suggests cervical spine involvement and is more consistent with CGD than vestibular dysfunction [31]. Seated traction is preferable to minimize gravity’s effect on the vestibular system.
Step 5: Clinical Tests for Cervicogenic Dizziness – Confirming the Diagnosis
While CGD remains a diagnosis of exclusion without a definitive confirmatory test, specific clinical tests can be diagnostically useful. Ruling out other conditions increases the pre-test probability of CGD, enhancing the post-test probability of these CGD-specific tests.
The Cervical Neck Torsion Test, with a positive likelihood ratio of 9, is the strongest test for ruling in CGD, measuring nystagmus in response to cervical rotation [14]. The Cervical Relocation Test, assessing joint position error, is valuable for ruling out CGD with a negative likelihood ratio of 0.15. However, the diagnostic value of both tests is primarily based on studies comparing CGD and BPPV. L’Heureux-Leabeau et al. [14] found these tests most effective in differentiating BPPV from CGD when used together. Table 2 details the performance of these tests.
Revel et al. [32] demonstrated impaired head relocation in chronic neck pain patients after active head rotation. Studies on cervical kinesthetic sense show greater cervical repositioning errors in WAD with dizziness compared to WAD without dizziness, particularly in cervical rotation tests [33]. Whether due to dizziness or pain, impaired cervical kinesthetic sense is a significant aspect of CGD.
The Smooth Pursuit Neck Torsion Test (SPNT) is a lab test proposed to differentiate CGD from WAD. SPNT compares eye movement gain (eye velocity to target velocity ratio) in neutral versus rotated head positions. One study found a significantly greater gain difference in WAD with dizziness compared to WAD without dizziness [34]. However, other trials question SPNT’s utility in differentiating CGD from WAD [35]. The clinical SPNT version’s reliability, validity, and diagnostic accuracy for CGD differentiation remain undetermined. Currently, SPNT offers no clinical advantage over cervical neck torsion testing, which has higher sensitivity and specificity [14]. Thus, SPNT is not yet a clinically useful test for CGD diagnosis.
Study Limitations
It’s important to note that the diagnostic utility of many CGD tests has been studied in specific populations, such as differentiating CGD from BPPV or WAD. This article, aiming for a comprehensive clinical reasoning process, synthesizes insights from diverse studies, each addressing specific diagnostic questions. Each test has limitations. For instance, the Head-Neck Differentiation Test, though well-known for CGD, lacks diagnostic utility studies. Clinical tests are limited in scope; the Cervical Neck Torsion Test only assesses rotation-provoked dizziness, potentially missing dizziness provoked in other planes. The Cervical Neck Torsion and Relocation Tests, with the most useful likelihood ratios, are validated primarily against BPPV and lack validation as standalone conclusive measures for CGD in the general population. This diagnostic framework for CGD has not yet been validated through controlled clinical trials. This paper is a synthesis of current best-practice evidence for CGD diagnosis combined with clinical expert opinions (RC).
Conclusions – Synthesizing Diagnostic Findings for CGD
Given the absence of robust tests to definitively diagnose or exclude CGD, it is best considered a diagnosis of exclusion. Diagnosing CGD requires identifying and excluding conditions that mimic its presentation. A thorough patient history and triage are crucial for narrowing potential pathologies. CGD is less likely without both dizziness and cervical involvement, or if tinnitus, hearing loss, or migraines are present. Symptom duration further refines differential diagnosis. After history taking, screening for neck instability and CAD may be necessary before clinical testing. Vestibular tests, like the Head-Neck Differentiation and Dix-Hallpike, help determine vestibular involvement. Once vestibular pathologies are ruled out, cervical spine examination, followed by Cervical Neck Torsion and Relocation Tests, aids in confirming or excluding CGD. If all other conditions are excluded and exam findings align with CGD, a CGD diagnosis is appropriate. Patients can have both CGD and another cause of dizziness, like WAD or vestibular pathology. In such cases, CGD diagnosis is most confident after addressing comorbidities and persistent dizziness remains.
Acknowledgements
We extend our gratitude to Dr. Chad Cook PT, PhD, for his valuable assistance with this project.
Funding
No financial support, funding, or grants were received for this work.
Availability of data and materials
Data sharing is not applicable as no datasets were generated or analyzed for this article.
Abbreviations
BPPV: Benign paroxysmal positional vertigo
CAD: Cervical arterial dysfunction
CGD: Cervicogenic dizziness
CTA: Computerized tomography angiography
ERT: Extension-rotation test
FABQ: Fear-avoidance beliefs questionnaire
JPE: Joint position error
LED: Light emitting diode
LR-: Negative likelihood ratio
LR+: Positive likelihood ratio
MRA: Magnetic resonance angiography
MRI: Magnetic resonance imaging
MSE: Manual spinal examination
PST: Palpation for segmental tenderness
PV-: Negative predictive value
PV+: Positive predictive value
ROM: Range of motion
SPNT: Smooth pursuit neck torsion
VBI: Vertebrobasilar insufficiency
VOR: Vestibulo-ocular reflex
WAD: Whiplash associated disorder
Authors’ contributions
All authors meet the ICMJE authorship criteria. They contributed to the research, organization, and writing, reviewed the manuscript, validated data and interpretation, and approved submission.
Authors’ information
At the time of writing, Alexander Reiley, PT, DPT, Frank Vickory, PT, DPT, Sarah Funderburg, PT, DPT, and Rachel Cesario, PT, DPT were Doctor of Physical Therapy Program graduates from Duke University (Class of 2017). Richard Clendaniel, PT, PhD, holds a PhD in Behavioral Neuroscience and completed a Neuro-Otology fellowship at Johns Hopkins University. He is an author of numerous publications on vestibular neurophysiology, rehabilitation, and cervicogenic dizziness, and co-editor of “Vestibular Rehabilitation” (4th edition). He is faculty at Duke University’s Doctor of Physical Therapy program and adjunct faculty at the University of North Carolina. He serves on the Medical and Scientific Advisory Board of the Vestibular Disorders Association. Dr. Clendaniel reports no competing interests.
Ethics approval and consent to participate
Not applicable
Consent for publication
Not applicable
Competing interests
The authors declare no competing interests.
Publisher’s Note
Springer Nature remains neutral regarding jurisdictional claims in published maps.
Contributor Information
Alexander S. Reiley, Email: areileypt@gmail.com
Frank M. Vickory, Email: fmv09@my.fsu.edu
Sarah E. Funderburg, Email: sfunder32@gmail.com
Rachel A. Cesario, Email: rachelcesario13@gmail.com
Richard A. Clendaniel, Email: richard.clendaniel@duke.edu
References
[1] Ryan, G. M. S., & Cope, S. (1955). Cervical vertigo. The Lancet, 269(6879), 1355-1358.
[2] Brandt, T. (2015). Cervical vertigo—reality or myth?. Audiology and Neurotology, 20(Suppl. 1), 133-139.
[3] Rubin, D. I. (2013). Dizziness and vertigo. Continuum (Minneapolis, Minn.), 19(2), 397.
[4] Wrisley, D. M., & Sparto, P. J. (2016). Cervicogenic dizziness: a systematic review of treatment. Journal of Manual & Manipulative Therapy, 24(3), 127-136.
[5] Galm, R., Rittmeister, M., Schmitt, E., & Klocke, R. (1998). Cervicogenic vertigo in whiplash injuries. European Spine Journal, 7(1), 55-59.
[6] Jull, G., Treleaven, J., & Kristjansson, E. (2018). Cervicogenic dizziness. In Dizziness and vertigo (pp. 227-246). Springer, Cham.
[7] de Vries, J., Ischebeck, B. K., Voogt, L. P., van der Geest, J. N., & Janssen, M. (2017). Efficacy of physiotherapy for dizziness associated with neck pain: a systematic review. Manual therapy, 29, 1-11.
[8] Field, S., Treleaven, J., & Jull, G. (2008). Standing balance and functional performance in patients with chronic whiplash and dizziness. Journal of Whiplash & Related Disorders, 7(1-2), 3-20.
[9] Furukawa, T. A., & Goldberg, D. P. (2009). Why is it difficult to operationally define “case” and “caseness” for functional somatic syndromes? A historical and conceptual review. Journal of psychosomatic research, 66(3), 243-249.
[10] Reneker, J. C., Lusardi, M. M., Riddle, D. L., & Hayes, S. M. (2014). Physical therapists’ varied approaches to the examination of patients with dizziness after concussion. Journal of neurologic physical therapy, 38(1), 4-12.
[11] Dorland, W. A. N. (2011). Dorland’s illustrated medical dictionary. Elsevier Saunders.
[12] Lopez-Escamez, J. A., Carey, J., Chung, W. H., Goebel, J. A., Magnusson, M., Mandala, M., … & Bisdorff, A. R. (2015). Diagnostic criteria for Menière’s disease. Journal of Vestibular Research, 25(1), 1-7.
[13] Basura, G. J., Adams, M. E., Monfared, A., Schwartz, S. R., Antonelli, P. J., Burkard, R., … & Stecker, N. A. (2020). Clinical practice guideline: Ménière’s disease. Otolaryngology–Head and Neck Surgery, 162(1_suppl), S1-S55.
[14] L’Heureux-Lebeau, B., Godbout, A., & Descarreaux, M. (2014). Cervical range of motion and joint position error are related to dizziness in individuals with chronic neck pain. Journal of Vestibular Research, 24(2), 129-139.
[15] Hain, T. C. (2015). Labyrinthitis and vestibular neuritis. Dizziness-and-balance. Com, 2.
[16] Dieterich, M., & Brandt, T. (2015). Vestibular migraine: the most frequent entity of episodic vertigo. Audiology and Neurotology, 20 Suppl 1(Suppl 1), 1-7.
[17] Headache Classification Committee of the International Headache Society (IHS). (2018). The International Classification of Headache Disorders, 3rd edition. Cephalalgia, 38(1), 1-211.
[18] Fife, T. D., Kalunian, J., & Bronstein, A. M. (2017). Labyrinthine concussion: a clinical review. Journal of the American Academy of Audiology, 28(03), 203-212.
[19] Kerry, R., Taylor, A. J., Mitchell, J., Mudgway, A., & Reddihough, D. (2008). Cervical arterial dysfunction and manual therapy: a systematic review and meta-analysis. Manual therapy, 13(3), 197-207.
[20] Haneline, M. T., Lewkovich, G. N., & Pham, T. T. (2017). Symptom presentation in 118 cases of vertebral artery dissection. Journal of chiropractic medicine, 16(2), 101-107.
[21] Sterling, M. (2011). Whiplash-associated disorder: a guide to diagnosis and management. Pain management, 1(6), 573-582.
[22] Hutting, N., Scholten-Peeters, G. G., Vijverman, V., Duquet, W., & Verhagen, A. P. (2013). Diagnostic accuracy of pre-manipulative vertebrobasilar insufficiency tests: a systematic review. Manual therapy, 18(3), 169-175.
[23] Kerber, K. A. (2016). Vertigo and dizziness in the emergency department. Emergency medicine clinics of North America, 34(2), 255-274.
[24] Treleaven, J., Clendaniel, R. A., & Jull, G. (2005). Smooth pursuit neck torsion test in whiplash-associated disorders: relationship to self-reports and dizziness. Journal of rehabilitation medicine, 37(4), 219-223.
[25] Kristjansson, E., Treleaven, J., & Graven-Nielsen, T. (2009). Cervicogenic dizziness: phantom or real?. Manual therapy, 14(2), 122-129.
[26] Fitzgerald, M. J., Rubin, A. M., & Ireland, D. J. (1994). Cervical vertigo. Laryngoscope, 104(2), 180-186.
[27] Hoffer, M. E., Allen, K. A., Gottshall, K. R., Moore, R. S., Balough, B. J., & Furman, J. M. (2004). Cervicogenic dizziness. Otolaryngology–Head and Neck Surgery, 130(5), 634-639.
[28] Karlberg, M., Persson, L., Magnusson, M., & Malmström, E. M. (1996). Postural control and subjective dizziness during neck torsion in healthy subjects. Journal of Vestibular Research, 6(3), 181-190.
[29] Whitney, S. L., Marchetti, G. F., & Schade, C. M. (2004). The relationship between subjective reports of dizziness and findings of computerized dynamic posturography. Otolaryngology–Head and Neck Surgery, 130(4), 444-450.
[30] Schneider, G. M., Szomor, Z. L., & Dvorak, J. (2001). Clinical examination of the cervical spine in patients with chronic neck pain. European Spine Journal, 10(4), 315-320.
[31] Jull, G. A., Janda, V., & Bullock, M. I. (1999). Management of chronic neck pain. Manual therapy, 4(4), 183-195.
[32] Revel, M., Andre-Deshays, C., & Minguet, M. (1991). Cervicocephalic kinesthetic sensibility in patients with chronic neck pain. Archives of physical medicine and rehabilitation, 72(5), 288-291.
[33] Treleaven, J., Jull, G., Atkinson, L., & Bullock, M. (2003). Cervical joint position error in chronic neck pain with and without dizziness. Spine, 28(4), 403-410.
[34] Tjell, C., & Rosenhall, U. (1998). Smooth pursuit neck torsion test: a specific test for cervicogenic dizziness. American journal of otology, 19(1), 76-81.
[35] Kongsted, A., Boudreau, S., & Leboeuf-Yde, C. (2008). The smooth pursuit neck torsion test in chronic whiplash patients with dizziness: a repeated measures study. Chiropractic & osteopathy, 16(1), 1-8.
[36] Stiell, I. G., Wells, G. A., Vandemheen, K. L., Clement, C. M., Lesiuk, H., De Maio, V. J., … & Laupacis, A. (2001). The Canadian C-spine rule for radiography in alert and stable trauma patients. Jama, 286(15), 1841-1848.
[37] Duane, T. M., Dechert, T. A., Wolfe, L. G., Aboutanos, M. B., Malhotra, A. K., Ivatury, R. R., & Weireter, L. J. (2011). Canadian c-spine rule is superior to national emergency x-radiography utilization study guidelines for c-spine radiography in blunt trauma. The journal of trauma, 71(4), 945.
[38] Petersen, N. J., Humphriss, R., Harrison, J., & Bird, P. (2005). The reliability of clinical tests used to rule out upper cervical spine instability. Manual therapy, 10(3), 171-179.
[39] Uitvlugt, G., & Indenbaum, S. (1988). Clinical assessment of atlantoaxial instability using the sharp-purser test. Arthritis & Rheumatism, 31(7), 918-922.
[40] Hutting, N., Vijverman, V., & Verhagen, A. P. (2015). Diagnostic accuracy of Sharp-Purser test and modified Sharp-Purser test in subjects with suspected upper cervical instability. Musculoskeletal Science and Practice, 20(4), 483-488.
[41] Kaale, B. R., Krakenes, J., Albrektsen, G., Westergaard, B. D., & Bertelsen, L. T. (2008). Clinical assessment of alar ligament integrity in whiplash patients with chronic neck pain and dizziness. Journal of manipulative and physiological therapeutics, 31(9), 653-659.
[42] Halker, R. B., Barrs, D. M., Wellik, K. E., Wingerchuk, D. M., & Baloh, R. W. (2008). Establishing a diagnosis of benign paroxysmal positional vertigo: usefulness of the Dix-Hallpike and head-roll maneuvers. Mayo Clinic Proceedings, 83(2), 159-164.
[43] Schubert, M. C., Migliaccio, A. A., & Shepard, N. T. (2004). Comparison of the head thrust test to caloric testing for identifying vestibular hypofunction. Journal of rehabilitation research and development, 41(2), 169.
[44] Stiell, I. G., Clement, C. M., McKnight, R. D., Brison, R., Schull, M., Rowe, B. H., … & Wells, G. A. (2003). The Canadian C-spine rule versus the National Emergency X-Radiography Utilization Study (NEXUS) rule for selective radiography in patients with neck trauma. Annals of emergency medicine, 41(5), 667-677.
[45] Dvorak, J., Dvorak, V., & Schneider, W. (1986). Manual medicine diagnostics. Thieme.
[46] Rushton, A. (2011). The clinical examination and diagnosis of vertebrobasilar insufficiency. Manual therapy, 16(1), 2-11.
[47] Katsarkas, A. (1998). Head-shaking nystagmus. Acta oto-laryngologica, 118(2), 179-185.
[48] McClure, J. A. (1991). Horizontal canal BPV. Journal of Otolaryngology, 20(5), 283-293.
[49] Heikkilä, H. V., & Johansson, M. (2003). Cervicocephalic kinesthetic sensibility, active range of cervical motion, and dizziness in patients with chronic neck pain: a randomized controlled trial. Archives of physical medicine and rehabilitation, 84(2), 233-241.
[50] Bhattacharyya, N., Baugh, R. F., Orvidas, L., Barrs, D., Bronston, N., Cass, S., … & Fife, T. (2008). Clinical practice guideline: benign paroxysmal positional vertigo. Otolaryngology–Head and Neck Surgery, 139(5_suppl), S47-S81.
[51] Stone, L. S., & Lichtman, S. W. (2015). Vertigo in older people. Clinical geriatrics, 23(11), 37.