Chronic Kidney Disease (CKD) is a significant global health issue, recognized as the 16th leading cause of years of life lost worldwide. Early and accurate diagnosis of CKD is paramount for effective management and preventing severe health outcomes, including cardiovascular disease, end-stage kidney disease (ESKD), and premature death. For primary care clinicians, understanding and applying the Ckd Diagnosis Criteria is essential to improve patient outcomes and reduce the global burden of this condition.
Understanding the Definition and Diagnostic Thresholds for CKD
Chronic Kidney Disease is defined by persistent abnormalities in kidney structure or function lasting for more than three months. The diagnosis of CKD hinges on specific criteria, primarily focusing on glomerular filtration rate (GFR) and albuminuria, alongside other indicators of kidney damage. These criteria are crucial for identifying CKD, staging its severity, and guiding appropriate clinical actions.
According to established guidelines, CKD diagnosis is confirmed by meeting one or more of the following criteria for a duration exceeding three months:
- Glomerular Filtration Rate (GFR) below 60 mL/min/1.73 m2: GFR is the gold standard measure of kidney function, reflecting the rate at which kidneys filter waste from the blood. A GFR below 60 mL/min/1.73 m2 indicates a significant reduction in kidney function and is a primary diagnostic criterion for CKD.
- Albuminuria (≥30 mg per 24 hours or urine albumin-to-creatinine ratio [ACR] ≥30 mg/g): Albuminuria, the presence of excessive albumin in the urine, is a key indicator of kidney damage. Even with a normal GFR, albuminuria signifies kidney dysfunction and is an independent criterion for CKD diagnosis. The level of albuminuria helps in staging CKD and assessing prognosis.
- Markers of Kidney Damage: Beyond GFR and albuminuria, other markers of kidney damage can establish a CKD diagnosis. These include abnormalities in urine sediment (e.g., hematuria), kidney histology (obtained through biopsy), or structural abnormalities detected through imaging (e.g., polycystic kidneys). Renal tubular disorders also fall under this category, as does a history of kidney transplantation.
It is important to differentiate CKD from acute kidney injury (AKI) and acute kidney disease (AKD). AKI is characterized by a sudden decline in kidney function over a few days, while AKD refers to kidney damage or reduced function lasting up to 3 months. If the duration of kidney issues is unclear, repeated assessments are necessary to accurately classify the condition as acute or chronic.
Clinical Presentation and Initial Evaluation for CKD
CKD often progresses silently, particularly in its early stages. Many individuals with CKD are asymptomatic, and the condition is frequently detected through routine laboratory tests. However, some patients may present with non-specific symptoms, or symptoms that only appear in advanced stages.
Common Clinical Presentations:
- Early Stages: Often asymptomatic; detection through routine serum chemistry profiles and urine tests.
- Less Common Initial Symptoms: Gross hematuria, foamy urine (indicating albuminuria), nocturia, flank pain, decreased urine output.
- Advanced Stages: Fatigue, poor appetite, nausea, vomiting, metallic taste, unintentional weight loss, pruritus, changes in mental status, dyspnea, peripheral edema.
Comprehensive Evaluation:
When CKD is suspected or diagnosed, a thorough evaluation is essential to determine the underlying cause, stage the disease, and guide management. This evaluation should include:
- Detailed Medical History: Assess for risk factors such as diabetes, hypertension, autoimmune diseases, systemic infections, nephrotoxic medication exposure (NSAIDs, herbal remedies, certain antibiotics), kidney stones, recurrent UTIs, family history of kidney disease, and genetic risk factors.
- Physical Examination: Evaluate volume status, check for signs of systemic diseases (rash, lymphadenopathy), and assess for indicators of potential causes like renovascular disease (carotid or abdominal bruits) or polycystic kidney disease (enlarged kidneys). In advanced CKD, signs may include pallor, skin excoriations, muscle wasting, and neurological changes.
- Urinary Analysis: Urinalysis is crucial. “Foamy urine” may suggest albuminuria. Urine dipstick and microscopic examination can detect hematuria and other abnormalities. Quantitative measurement of albuminuria, preferably using urine ACR, is essential for diagnosis and staging.
- Blood Tests: Serum creatinine is used to estimate GFR. Electrolyte levels, bicarbonate, calcium, phosphate, parathyroid hormone, vitamin D, and hemoglobin levels are important for monitoring complications of CKD.
Staging CKD Based on GFR and Albuminuria: KDIGO Guidelines
Once CKD is diagnosed, staging is crucial for prognosis and management. The Kidney Disease Improving Global Outcomes (KDIGO) guidelines provide a standardized staging system based on GFR and albuminuria categories. This system helps clinicians assess the severity of CKD and the risk of progression.
GFR Categories:
| GFR Category | GFR (mL/min/1.73 m2) | Description |
|---|---|---|
| G1 | ≥90 | Normal or High |
| G2 | 60-89 | Mildly Decreased |
| G3a | 45-59 | Mildly to Moderately Decreased |
| G3b | 30-44 | Moderately to Severely Decreased |
| G4 | 15-29 | Severely Decreased |
| G5 | <15 (or dialysis) | Kidney Failure |
Albuminuria Categories (Urine ACR):
| Albuminuria Category | Urine ACR (mg/g) | Description |
|---|---|---|
| A1 | <30 | Normal to Mildly Increased |
| A2 | 30-300 | Moderately Increased |
| A3 | >300 | Severely Increased |
Risk Stratification using GFR and Albuminuria Categories:
The KDIGO guidelines combine GFR and albuminuria categories to define the prognosis of CKD, stratifying risk into green (low), yellow (moderate), orange (high), and red (very high) risk of CKD progression and adverse outcomes.
Figure 2. KDIGO 2012 risk stratification for CKD based on GFR and albuminuria categories, illustrating the increasing risk of CKD progression and adverse outcomes as categories worsen. This matrix is essential for guiding management and referral strategies.
This risk stratification chart is a critical tool for clinicians to understand the prognosis and guide management intensity. Patients in higher risk categories (orange and red) require more aggressive management and closer monitoring.
Screening Strategies for Early CKD Detection
Given the asymptomatic nature of early CKD, screening is vital for early detection, especially in high-risk populations. A risk-based screening approach is widely recommended.
Target Populations for CKD Screening:
- Individuals aged 60 years or older.
- Those with diabetes mellitus.
- Individuals with hypertension.
- People with autoimmune diseases.
- Those with systemic infections (HIV, hepatitis B, hepatitis C).
- Patients with a history of cardiovascular disease.
- Individuals with family history of kidney disease.
- Those exposed to nephrotoxic medications (NSAIDs, lithium, etc.).
- Individuals with recurrent urinary tract infections or kidney stones.
- Patients with reduced kidney mass or history of acute kidney injury.
Screening Tests:
The National Kidney Foundation recommends a “kidney profile test” which includes:
- Serum Creatinine Measurement: Used to estimate GFR, typically using the CKD-EPI equation, which is more accurate than older equations, especially at higher GFR levels. Online calculators are readily available (https://www.kidney.org/professionals/kdoqi/gfr_calculator). Cystatin C may be considered in specific situations for increased accuracy.
- Urine Albumin-to-Creatinine Ratio (ACR): Preferred method for quantifying albuminuria due to better standardization and precision, especially at lower levels. First morning void or 24-hour urine collection are most accurate, but random samples are acceptable for initial screening.
While screening guidelines are well-established, it’s important to note that randomized controlled trials demonstrating improved outcomes from screening asymptomatic individuals are still lacking. However, the consensus is that risk-based screening is a prudent approach to identify CKD early.
Diagnostic Algorithm and Referral Considerations
For primary care clinicians, a clear diagnostic algorithm is crucial for managing patients with suspected or confirmed CKD.
Diagnostic Steps:
- Identify Risk Factors: Assess patients for clinical, sociodemographic, and genetic risk factors for CKD.
- Perform Screening Tests: For at-risk individuals, conduct serum creatinine measurement for eGFR estimation and urine ACR testing.
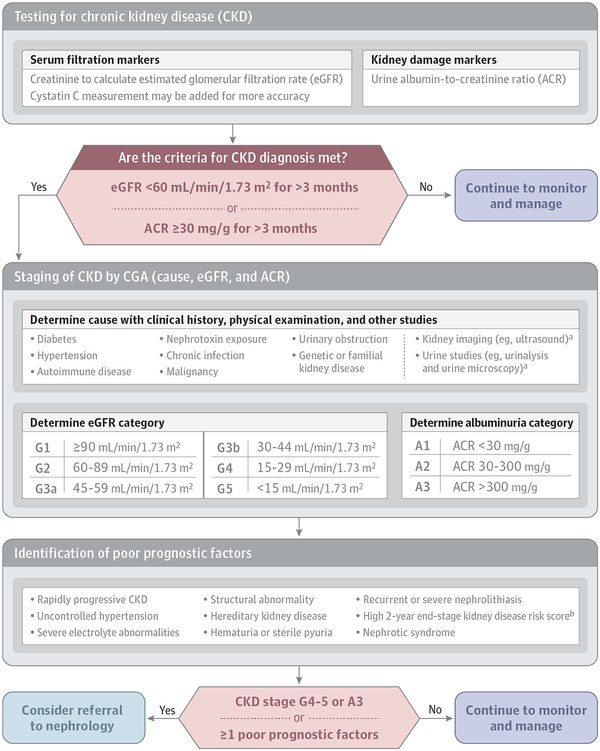
- Confirm CKD Diagnosis: If eGFR is <60 mL/min/1.73 m2, or urine ACR is ≥30 mg/g, or other markers of kidney damage are present for >3 months, confirm CKD diagnosis.
- Determine Etiology: Investigate potential causes of CKD based on history, physical exam, and initial lab findings. Consider systemic diseases, urinary tract obstruction, nephrotoxin exposure, etc.
- Stage CKD: Use KDIGO guidelines to stage CKD based on GFR and albuminuria categories.
- Assess Risk of Progression: Utilize risk calculators like the Kidney Failure Risk Equation (KFRE) (https://kidneyfailurerisk.com/) to estimate the risk of ESKD.
Figure 1. A diagnostic and management algorithm for CKD, outlining key steps from initial suspicion to referral, emphasizing the integration of GFR, albuminuria, and risk assessment tools for optimal patient care.
Referral to Nephrologist:
Prompt referral to a nephrologist is essential for certain CKD patients. KDIGO guidelines recommend referral in the following scenarios:
- eGFR <30 mL/min/1.73 m2 (Stage G4 or G5).
- Urine ACR >300 mg/g (Stage A3).
- Albuminuria >2200 mg per 24 hours (consider nephrotic syndrome).
- Rapid progression of CKD (eGFR decline ≥25% or >5 mL/min/1.73 m2 per year).
- Uncontrolled hypertension despite ≥4 antihypertensive medications.
- Persistent hyperkalemia or hypokalemia.
- Recurrent or extensive kidney stones.
- Hereditary kidney disease.
- Unexplained hematuria or red cell casts.
- CKD of unclear etiology.
Early nephrology referral improves CKD management, facilitates timely planning for kidney replacement therapy, and optimizes patient outcomes.
Conclusion: Improving CKD Care Through Accurate Diagnosis
Accurate and timely diagnosis of Chronic Kidney Disease is the cornerstone of effective management and reducing its global impact. Primary care clinicians play a pivotal role in identifying individuals at risk, applying CKD diagnosis criteria, staging the disease, and initiating appropriate management and referral strategies. By adhering to established guidelines and utilizing available tools for risk assessment and staging, clinicians can significantly improve the care and outcomes for patients with CKD, ultimately mitigating the burden of this widespread and serious condition.