Introduction
Hemophagocytic lymphohistiocytosis (HLH) is not a standalone disease but a severe hyperinflammatory syndrome that can be life-threatening. Central nervous system involvement in HLH (CNS-HLH) is a critical complication, frequently observed in both primary and secondary HLH cases. A significant number of HLH patients, whether their condition is primary or secondary, experience CNS involvement, highlighting the importance of recognizing and addressing this aspect of the disease. Reactivation within the CNS is a common concern during HLH treatment, occurring alongside or independently of systemic relapses. Furthermore, primary HLH should be considered as a potential underlying cause in cases of unexplained CNS inflammation, as some patients may initially present with symptoms solely related to CNS disease. Accurate and timely Cns Hlh Diagnosis is paramount for initiating appropriate treatment and preventing severe neurological outcomes. This article provides a detailed overview of CNS-HLH diagnosis, emphasizing the critical steps for auto repair experts in understanding this complex condition within the broader context of HLH.
Understanding CNS Involvement in HLH
Defining CNS-HLH
The definition of CNS involvement in HLH lacks standardization, yet the consensus among HLH experts is that CNS-HLH is characterized by abnormal Cerebrospinal Fluid (CSF) findings and/or Magnetic Resonance Imaging (MRI) of the brain. These abnormalities may or may not be accompanied by overt neurological signs or symptoms. Despite ongoing discussions about the precise definition, there is agreement that CNS-HLH involves the infiltration of activated lymphocytes and macrophages into the meninges and brain tissue. Neuropathologically, CNS-HLH is categorized into stages: stage I involves leptomeningeal inflammation, stage II is marked by perivascular infiltration, and stage III is characterized by massive tissue infiltration, blood vessel destruction, and tissue necrosis. This aggressive infiltration can lead to devastating brain lesions, making CNS involvement a major contributor to mortality and morbidity in HLH.
Prevalence and Significance of CNS-HLH
CNS involvement is frequently observed at the onset of both primary and secondary HLH. Moreover, reactivation of the disease within the CNS is a common occurrence during or after treatment. Overall, studies indicate that CNS disease is reported in 30–73% of all HLH patients, either at the time of diagnosis or during the disease course. Given the diagnostic challenges associated with HLH, a high degree of clinical suspicion is essential when evaluating patients, especially those presenting with systemic HLH. While the systemic manifestations of HLH are similar across primary and secondary cases—characterized by systemic inflammation, elevated cytokine levels, and immune-mediated organ damage—the clinical presentation of CNS disease in HLH is highly variable. Neurological symptoms are not part of the systemic HLH diagnostic criteria. However, it is vital to consider HLH in children exhibiting unexplained neurological manifestations, particularly when accompanied by fever, pancytopenia, and hepatosplenomegaly.
Long-Term Neurological Sequelae
Improvements in HLH survival rates have shifted focus towards the long-term consequences of the disease, with neurological sequelae being particularly significant. Unfortunately, HLH can result in substantial motor and cognitive deficits. Early recognition and prompt treatment of CNS disease are crucial for preventing irreversible CNS injury, thereby improving long-term outcomes. However, data on neurological outcomes following different treatment approaches remain limited, as clinical trials have primarily focused on survival rates.
Diagnostic Approach to CNS-HLH
To achieve accurate cns hlh diagnosis, a multifaceted approach is necessary. This includes a thorough clinical evaluation, detailed neurological examination, CSF analysis, and neuroimaging. The diagnostic process is crucial even in the absence of obvious neurological symptoms, as early detection significantly impacts treatment strategies and patient outcomes.
Clinical Evaluation and Neurological Examination
A detailed patient history and neurological examination are fundamental first steps in suspecting cns hlh diagnosis. While prospective neurological evaluations in HLH are limited, studies indicate that neurological involvement occurs in a substantial proportion of HLH patients, ranging from 18% to 73%. Larger, more systematic studies suggest that approximately two-thirds of HLH patients, encompassing both primary and secondary forms, will exhibit neurological manifestations. It is crucial to note that CNS inflammation can be the primary and sole clinical presentation of HLH.
Neurological symptoms in CNS-HLH can be severe and even life-threatening, often appearing early in the disease course. Seizures are the most frequently reported neurological sign, occurring in 33–83% of children with CNS-HLH. Altered mental status, encompassing irritability, disturbed consciousness, and encephalopathy, is also common, affecting 31–47% of patients, indicating frequent gray matter dysfunction. Meningism is observed in about one-third of patients with neurological findings. Focal neurological signs, such as hemiparesis, cranial neuropathies, and ataxia, are less frequent, occurring in 10–20% of cohorts. However, inconsistencies in reporting neurological symptoms across different studies make direct comparisons challenging.
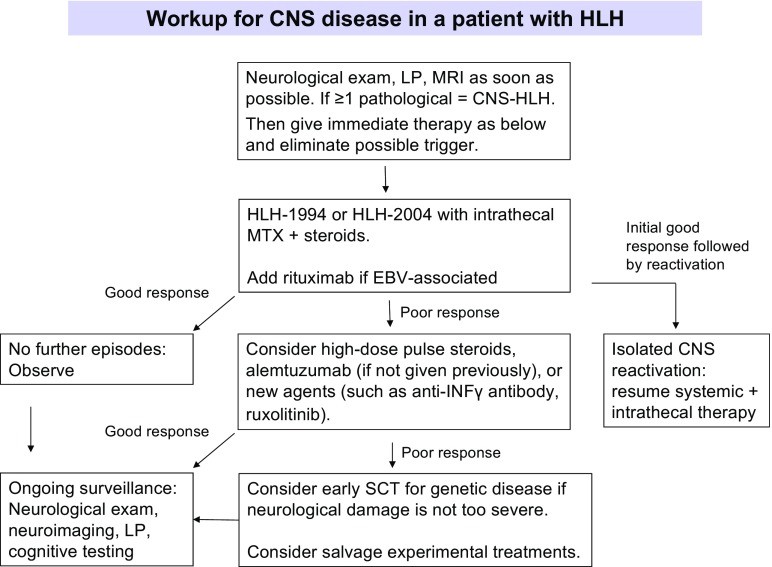 Fig. 1
Fig. 1
Caption: Diagnostic workflow for CNS disease in HLH patients, illustrating the sequential steps from initial suspicion to treatment initiation.
Cerebrospinal Fluid (CSF) Analysis: A Key Diagnostic Tool
CSF analysis is indispensable for cns hlh diagnosis, even in the absence of neurological symptoms. A lumbar puncture should be performed routinely in all patients suspected of having HLH, provided there are no contraindications. Standard CSF analysis should include cell counts, protein levels (including fractions), glucose, lactate, microbiology, and cytospin examination for hemophagocytosis.
CSF abnormalities are common in HLH. Pleocytosis, an increased number of cells in the CSF, is seen in 10–47% of HLH patients. It is important to note that pleocytosis may be a late finding, and repeat lumbar punctures may be necessary if clinical suspicion remains high. Elevated CSF protein levels are also frequent, observed in 11–41% of HLH patients. While typically moderately elevated (500–1000 mg/L, normal range 150–400 mg/L), levels can reach as high as 10,000 mg/L. Protein levels exceeding 2500 mg/L have been associated with stage III neuropathological abnormalities, though their prognostic value is uncertain. Significantly elevated CSF protein in an encephalopathic child of unknown etiology should raise suspicion for neuroinflammatory conditions, including HLH.
“Abnormal CSF” is often defined as the presence of pleocytosis, increased CSF protein, or both. Using this definition, CSF abnormalities are found in 16–76% of HLH cases. The presence of neurological symptoms combined with any CSF abnormality is considered a negative prognostic marker. CSF abnormalities can resolve quickly with treatment, with some studies showing resolution in all children within 6 weeks of initiating therapy.
Hemophagocytosis, while highly prevalent in brain biopsies (91%) and bone marrow samples (92%), is less commonly observed in CSF (39%) in pediatric HLH cases. The clinical significance of CSF hemophagocytosis and its correlation with disease severity and duration, as seen in brain tissue, remains unclear. Research into novel biomarkers in CSF, such as neopterin, CXCL13, and neurofilament light chain, is warranted to improve diagnostic sensitivity and specificity for CNS-HLH.
Neuroimaging: MRI as Modality of Choice
MRI of the brain with gadolinium contrast is the preferred neuroimaging technique when CNS involvement in HLH is suspected. If MRI is not readily available, CT scans can provide valuable structural information but lack the detailed assessment offered by MRI. Neuroimaging findings in CNS-HLH are diverse. Multifocal and bilateral abnormalities on T2-weighted MRI are almost universally present in primary HLH (89%), often with symmetric involvement (53%), which can help differentiate it from conditions like acute disseminated encephalomyelitis (ADEM). Large, poorly defined, confluent lesions are seen in up to two-thirds of HLH patients. CNS hemorrhage is less common but has been reported. Chronic changes such as atrophy and calcifications have also been noted, though their timing in relation to disease onset and treatment is not well-documented. Gadolinium contrast administration is beneficial, often revealing nodular or ring enhancement (6/9) and/or leptomeningeal enhancement (5/9) in many cases.
Caption: Neuroradiological MRI findings in HLH patients. (a) T2-weighted image showing bilateral hyperintense lesions in the cerebellum. (b) T2-weighted image with hyperintense signal and edema in the left posterior hemisphere and brainstem abnormalities. (c) Diffusion-weighted imaging of the same region as (b) with lesions mimicking cerebral infarction.
Differential Diagnosis
The differential diagnosis for CNS-HLH is broad, encompassing various neuroinflammatory and neurological conditions. These include acute disseminated encephalomyelitis (ADEM), acute necrotizing encephalopathy (ANE), CNS vasculitis, multiple sclerosis, encephalitis, CNS manifestations of rheumatologic diseases like systemic lupus erythematosus, and other genetic CNS inflammatory disorders such as interferonopathies. Careful clinical and paraclinical evaluation is crucial to differentiate CNS-HLH from these conditions and ensure accurate cns hlh diagnosis.
Conclusion
Accurate and timely cns hlh diagnosis is critical for effective management of this severe complication of HLH. A comprehensive diagnostic approach incorporating clinical assessment, neurological examination, CSF analysis, and neuroimaging, particularly MRI, is essential. Early diagnosis and prompt initiation of treatment are vital to mitigate neurological damage and improve long-term outcomes for patients with CNS-HLH. Given the complexity and severity of CNS-HLH, early consultation with specialists experienced in HLH diagnosis and management is highly recommended.
References
[References] (as in original article)