Choroidal neovascularization (CNV) is a serious eye condition that can severely impact vision. Often associated with wet Age-related Macular Degeneration (AMD), CNV involves the growth of abnormal blood vessels in the retina. Early and accurate Cnv Eye Diagnosis is critical to prevent vision loss and manage this condition effectively. This article will explore what CNV is, how it’s diagnosed, its symptoms, and available treatments.
What is Choroidal Neovascularization?
Neovascularization, in medical terms, refers to the development of new blood vessels. In the context of CNV, these new, unhealthy blood vessels originate from the choroid, a layer rich in blood vessels located beneath the retina. In individuals with conditions like AMD, the eye may produce excessive vascular endothelial growth factor (VEGF). This excess VEGF triggers the growth of new blood vessels from the choroid, extending into the retina. Unlike healthy blood vessels, these new ones are fragile and leaky. This leakage causes fluid and sometimes blood to seep into the retina. This accumulation of fluid disrupts the normally flat structure of the retina, creating a blister-like effect and immediately distorting vision. If left untreated, this fluid leakage can cause lasting damage to the photoreceptors, the light-sensing cells of the retina, leading to permanent vision impairment.
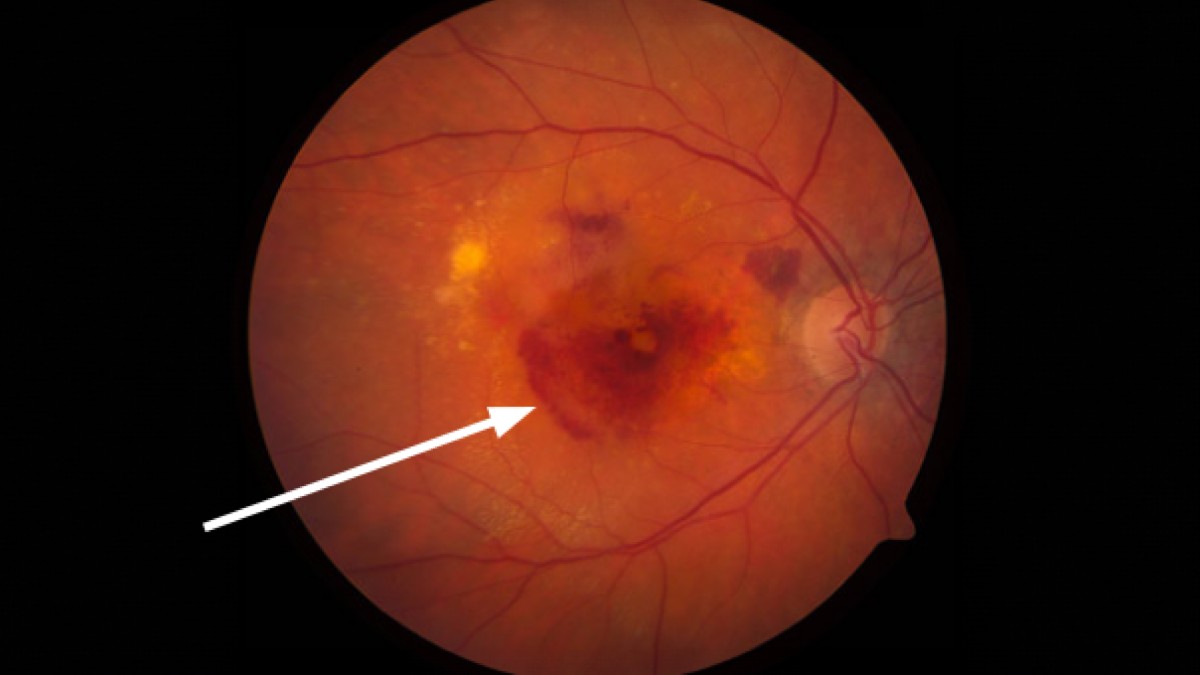 Close-up image of a human retina displaying signs of diabetic retinopathy, with an arrow pointing to an area of hemorrhage and abnormal vessels.
Close-up image of a human retina displaying signs of diabetic retinopathy, with an arrow pointing to an area of hemorrhage and abnormal vessels.
Alt text: Detailed retinal image showing choroidal neovascularization, highlighting abnormal blood vessel growth and hemorrhage area, crucial for cnv eye diagnosis.
Recognizing the Symptoms of CNV
Identifying the symptoms of CNV promptly is vital for preserving vision. The primary symptoms include:
- Distortion or waviness in central vision: Straight lines may appear bent or irregular.
- A gray, black, or blank spot in central vision: This can obscure the center of your visual field.
Experiencing these symptoms warrants immediate consultation with an ophthalmologist. Urgent medical attention is necessary because timely intervention, ideally within hours or days of symptom onset, is crucial. Ophthalmologists can administer treatments, such as VEGF-blocking drugs, to halt the progression of CNV and fluid leakage, but their effectiveness is significantly higher with early administration. Remember, in the case of CNV, delayed diagnosis and treatment can lead to irreversible vision loss.
Methods for CNV Eye Diagnosis
A comprehensive cnv eye diagnosis involves several techniques employed by ophthalmologists. Initially, a dilated eye exam is performed, allowing the ophthalmologist to directly observe the retina. During this examination, signs of CNV, such as fluid buildup or bleeding within the retina, may be visible.
To gain a more detailed view, specialized imaging techniques are used:
-
Optical Coherence Tomography (OCT): OCT provides cross-sectional images of the retina. This technology can detect even minute amounts of fluid leakage caused by CNV, offering a precise assessment of retinal structure.
-
Fluorescein and Indocyanine Green (ICG) Angiography: These procedures involve injecting a dye into a vein, which then circulates to the blood vessels in the eye. Retinal imaging is performed as the dye passes through the eye’s blood vessels. Leakage of the dye from abnormal blood vessels into the retina, visualized in these images, can confirm CNV and provide further details about the condition. These angiography techniques offer supplementary information that aids in a complete cnv eye diagnosis.
Underlying Conditions Contributing to CNV
While age-related macular degeneration is the most prevalent cause of CNV, several other conditions can also trigger its development. These conditions generally share a common pathway: they either stress the retina, leading to increased VEGF production, or disrupt the barrier between the retina and the choroid. Other conditions include:
-
Pathologic Myopia (Extreme Nearsightedness): In individuals with severe myopia, the elongated shape of the eye can stretch the retina, making it more susceptible to CNV.
-
Ocular Histoplasmosis: This fungal infection can affect the eye and is another known cause of CNV.
-
Eye Trauma and Angioid Streaks: Physical trauma to the eye or angioid streaks (small cracks in the Bruch’s membrane, a layer of the retina) can disrupt the barrier between the retina and choroid, facilitating CNV.
-
Severe Ocular Inflammation (Uveitis): Inflammatory conditions affecting the eye, such as uveitis, can also contribute to the development of CNV.
Treatment Strategies for Choroidal Neovascularization
For most patients diagnosed with CNV stemming from these various conditions, intravitreal injections of anti-VEGF drugs have become the standard of care. Medications like brolucizumab (Beovu®), aflibercept (Eylea®), and ranibizumab (Lucentis®) are effective in targeting VEGF, the protein that drives the growth and leakage of CNV blood vessels. By inhibiting VEGF, these drugs can slow down or halt the progression of CNV, helping to preserve vision.
Ongoing research is focused on developing next-generation anti-VEGF therapies that offer longer-lasting effects. This includes newer anti-VEGF drugs and gene therapy approaches. The goal of these advancements is to reduce the frequency of injections required, improving patient convenience and long-term outcomes in managing CNV. Early cnv eye diagnosis coupled with timely treatment offers the best chance of managing this condition and maintaining vision.