Crafting an effective nursing care plan is a cornerstone of excellent patient care. It’s a detailed roadmap that guides nurses in addressing patient needs, managing health problems, and promoting wellness. This comprehensive guide will walk you through the essential steps of developing a robust care plan, with a particular focus on common nursing diagnoses and how to incorporate them effectively. Whether you’re a seasoned registered nurse or a student nurse just beginning your journey, this resource provides the knowledge and tools you need to excel in nursing care planning. We offer an ultimate database and extensive list of nursing care plans (NCPs) and nursing diagnosis examples readily available for both student nurses and practicing professionals – all accessible for free! Let’s delve into the components, objectives, and purposes of nursing care plans, and equip you with a detailed guide to writing exceptional plans, complete with templates you can adapt for your specific unit.
Understanding the Nursing Care Plan
A nursing care plan (NCP) is a formal, structured process that nurses use to identify a patient’s existing health needs and to recognize potential future needs or risks. Think of it as a blueprint for patient care, facilitating clear communication among nurses, patients, and the broader healthcare team. This collaborative approach ensures everyone is aligned in achieving the best possible healthcare outcomes. Without a well-defined care planning process, the consistency and quality of patient care would undoubtedly suffer.
The nursing care planning journey begins the moment a patient is admitted to a healthcare facility. It’s not a one-time event but an ongoing, dynamic process. The care plan is continuously reviewed and updated in response to changes in the patient’s condition and as progress is made towards achieving established goals. This commitment to individualized, patient-centered care is the very foundation of excellence in nursing practice.
Types of Nursing Care Plans: Formal vs. Informal, Standardized vs. Individualized
Nursing care plans can be broadly categorized as informal or formal, and further refined into standardized or individualized approaches.
Informal nursing care plans are essentially mental strategies. They represent the immediate action plans that a nurse formulates in their mind as they assess a patient’s needs and prioritize interventions. These plans are flexible and adaptable, guiding moment-to-moment decisions at the bedside.
Formal nursing care plans, in contrast, are documented guides, either written or computerized, that systematically organize a patient’s care information. These plans provide a structured framework for care delivery and ensure consistency across different nurses and shifts.
Formal care plans are further divided into two key types:
-
Standardized Care Plans: These are pre-written guides outlining nursing care for patients with common, recurring needs. They are designed to ensure consistent care for groups of patients with similar conditions and streamline nursing workflows by eliminating the need to repeatedly create plans for routine situations. These are especially helpful in addressing common nursing diagnoses.
-
Individualized Care Plans: These plans are tailored to meet the specific, unique needs of an individual patient. They are developed when a patient’s needs go beyond what a standardized plan can address, requiring a more personalized approach. Individualized plans often build upon standardized plans, adapting them to fit the patient’s particular circumstances.
Delving Deeper: Standardized and Individualized Care Plans
Standardized Care Plans are invaluable tools for healthcare agencies and nursing staff. They serve as pre-developed protocols, guaranteeing that patients with specific conditions receive a baseline of consistent, high-quality care. By establishing minimally acceptable care criteria, standardized plans also promote efficient use of nursing time, freeing nurses from repeatedly developing care steps that are common for many patients within a nursing unit.
It’s important to recognize that standardized care plans are not designed to address every nuance of a patient’s individual needs and goals. However, they provide an excellent starting point. They are often used as a foundation upon which to build a more comprehensive individualized care plan.
The care plans presented in this guide are primarily standardized care plans. They are intended to serve as a framework or direction to assist you in developing individualized care plans that are specifically tailored to your patients.
Individualized Care Plans are where the art and science of nursing truly converge. Developing an individualized care plan involves carefully modifying a standardized care plan to align with a specific patient’s unique needs and healthcare goals. This process emphasizes using approaches that have been proven effective for that particular patient, taking into account their personal preferences, strengths, and challenges. This level of personalization facilitates more holistic care, ensuring that the patient is treated not just as a diagnosis, but as a whole person.
Furthermore, individualized care plans have a significant impact on patient satisfaction. When patients perceive that their care is specifically designed for them, they feel more valued, heard, and understood. This heightened sense of engagement directly translates to increased satisfaction with their overall healthcare experience. In today’s healthcare environment, where patient satisfaction is increasingly recognized as a crucial quality metric, the ability to create effective individualized care plans is more important than ever.
Tips for Individualizing Nursing Care Plans: (This section would be expanded with practical tips, but is omitted for brevity as per instructions).
Objectives of Nursing Care Plans
The creation and implementation of nursing care plans serve several vital objectives:
- Promote Evidence-Based Care: Care plans are designed to ensure that nursing care is grounded in the best available evidence and tailored to create a comfortable and familiar environment within healthcare settings.
- Support Holistic Care: Nursing care plans champion holistic care, addressing the patient as a whole person, encompassing their physical, psychological, social, and spiritual dimensions. This comprehensive approach is essential for both managing and preventing disease effectively.
- Establish Care Programs: Care plans facilitate the development of structured programs like care pathways and care bundles. Care pathways promote team consensus on standards of care and desired outcomes, while care bundles focus on implementing best practices for specific conditions.
- Clearly Define Goals and Outcomes: A key objective is to precisely identify and differentiate between broad goals and specific, measurable expected outcomes for patient care.
- Enhance Communication and Documentation: Care plans improve communication among healthcare providers and provide a structured format for documenting all aspects of patient care.
- Measure Nursing Care Effectiveness: Care plans provide a framework for evaluating the effectiveness of nursing interventions and making necessary adjustments to optimize patient outcomes.
Purposes and Importance of Nursing Care Plans
Nursing care plans are not merely procedural documents; they serve profound purposes that are critical to effective healthcare delivery:
- Defines the Nurse’s Role: Care plans clearly delineate the unique and independent role of nurses in addressing patients’ overall health and well-being. They empower nurses to act proactively, beyond simply following physician orders.
- Provides Direction for Individualized Care: A care plan acts as a personalized roadmap, guiding nurses in delivering care that is specifically tailored to each patient’s unique needs. It encourages critical thinking in developing interventions that directly address individual circumstances.
- Ensures Continuity of Care: Care plans are essential for maintaining consistent care across different nursing shifts and departments. By providing a shared source of patient data and planned interventions, they ensure that all nurses deliver the same high-quality care, maximizing treatment benefits for patients.
- Coordinates Care Across Teams: Care plans facilitate seamless coordination among all members of the healthcare team. By ensuring everyone is aware of the patient’s needs and planned actions, care plans prevent fragmentation and gaps in service delivery.
- Serves as a Vital Documentation Tool: Care plans are crucial for accurate documentation. They outline specific observations to be made, nursing actions to be implemented, and instructions required for the patient and their family members. Proper documentation within the care plan serves as evidence that care was provided, which is essential for legal and quality assurance purposes.
- Guides Staff Assignment: In situations where patients require specialized skills, care plans assist in appropriately assigning staff with the necessary expertise to meet specific patient needs.
- Monitors Patient Progress: Care plans are dynamic tools that enable healthcare providers to track a patient’s progress systematically. They allow for timely adjustments to the care plan in response to evolving health status and changing goals.
- Supports Reimbursement Processes: Insurance companies rely on medical records, including care plans, to determine appropriate reimbursement for hospital care. Comprehensive care plans justify the medical necessity and scope of services provided.
- Defines Patient Goals and Promotes Engagement: Care plans benefit both nurses and patients by actively involving patients in their treatment journey. This collaborative approach ensures that care is aligned with patient preferences and promotes a sense of ownership in their health outcomes.
Key Components of a Nursing Care Plan
A typical nursing care plan (NCP) comprises several essential components, including nursing diagnoses, patient problems, expected outcomes, nursing interventions, and rationales. Let’s explore each of these in more detail:
- (1) Nursing Diagnoses: These are clinical judgments about individual, family, or community responses to actual or potential health problems and life processes. Nursing diagnoses provide the foundation for selecting nursing interventions to achieve patient outcomes. They are based on data gathered during patient assessment.
- (2) Patient Problems/Needs: This component expands upon the nursing diagnoses, detailing specific issues or challenges the patient is facing. It provides a more descriptive picture of the patient’s condition.
- (3) Expected Outcomes: These are specific, measurable, achievable, relevant, and time-bound (SMART) statements describing the desired changes in patient health status as a result of nursing care. They define what the nurse hopes to achieve.
- (4) Nursing Interventions: These are the actions that nurses will perform to achieve the expected outcomes. Interventions should be evidence-based, patient-centered, and tailored to address the identified nursing diagnoses and patient problems.
- (5) Rationales: For each nursing intervention, a rationale explains the scientific basis or evidence supporting its use. Rationales are particularly important in student care plans as they reinforce the link between nursing actions and underlying principles.
Care Plan Formats: Three-Column, Four-Column, and Student Plans
Nursing care plans are often organized into structured formats to enhance clarity and ease of use. Common formats include three-column and four-column plans, with student care plans often having additional elements. The organization typically facilitates a logical flow from problem identification to outcome evaluation.
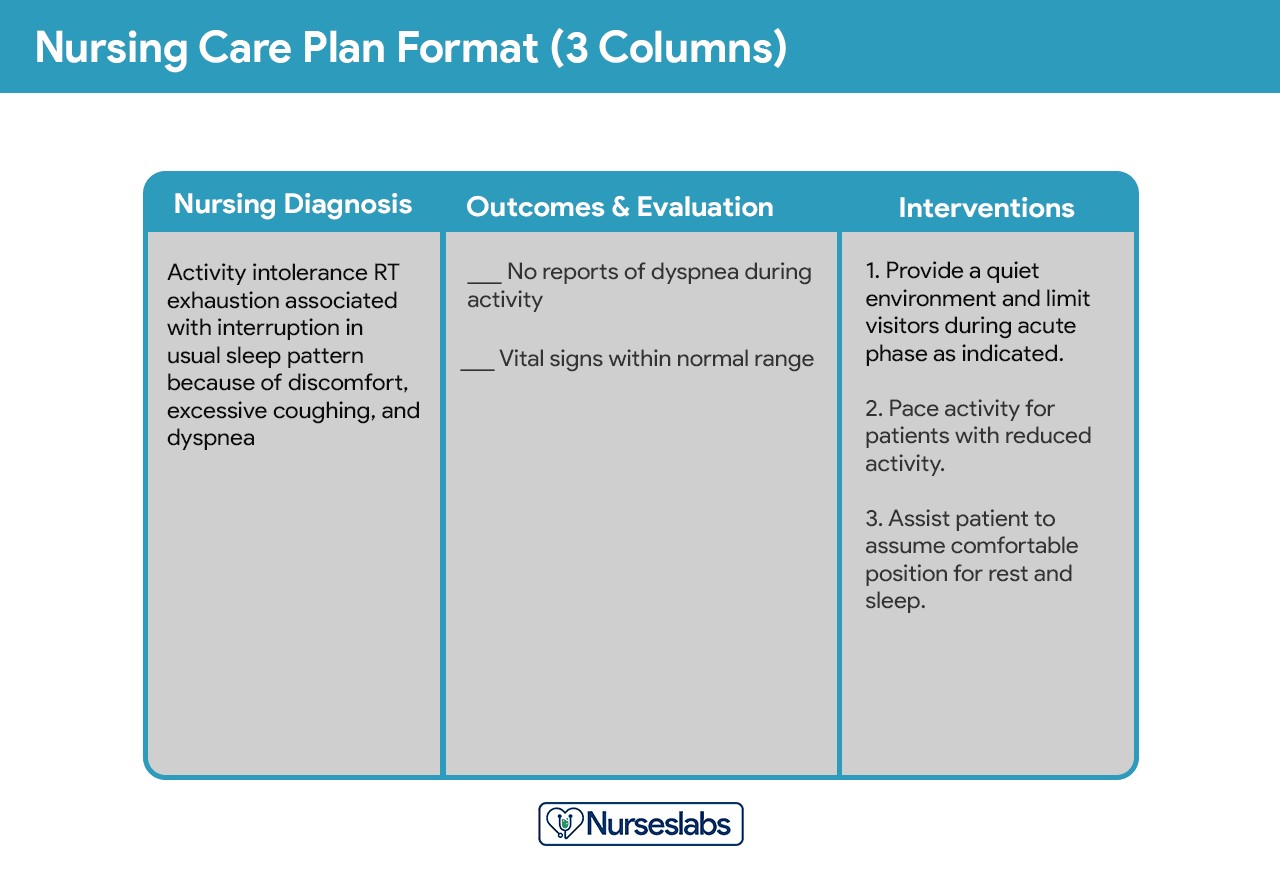
Three-Column Format
The three-column plan is a streamlined format that efficiently presents key information. It typically includes columns for:
- Nursing Diagnosis: The identified nursing diagnosis.
- Outcomes and Evaluation: Desired patient outcomes and space for documenting evaluation of goal achievement.
- Interventions: Specific nursing interventions planned to address the diagnosis and achieve outcomes.
Example of a three-column nursing care plan format, demonstrating the concise organization of nursing diagnosis, desired outcomes/evaluation, and interventions.
Four-Column Format
The four-column format provides a slightly more detailed structure, separating outcomes and evaluation into distinct columns:
- Nursing Diagnosis: The nursing diagnosis.
- Goals and Outcomes: Desired patient goals and specific, measurable outcomes.
- Interventions: Nursing interventions.
- Evaluation: Assessment of goal achievement and plan effectiveness.
Example of a four-column nursing care plan template, illustrating the clear separation of nursing diagnosis, goals/outcomes, interventions, and evaluation.
Below is a downloadable document containing sample templates for various nursing care plan formats. Feel free to adapt, modify, and share these templates for your use:
Download: Printable Nursing Care Plan Templates and Formats
Student Care Plans: Emphasizing Learning and Rationales
Student care plans are intentionally designed to be more comprehensive and detailed than those used by practicing nurses. Their primary purpose is to serve as a robust learning tool for nursing students, reinforcing critical thinking and the application of nursing principles.
A student nursing care plan example, highlighting the greater detail and inclusion of rationales for interventions, crucial for the learning process.
Typically, student care plans are handwritten and include an additional column for “Rationale” or “Scientific Explanation.” This rationale column is placed after the nursing interventions column and requires students to articulate the scientific principles that justify each selected nursing intervention. This element is key to deepening understanding and linking theory to practice.
Step-by-Step Guide: Writing a Nursing Care Plan
How do you effectively write a nursing care plan (NCP)? Follow these steps to develop a well-structured and patient-centered plan for your client.
Step 1: Data Collection and Comprehensive Assessment
The initial step in crafting a nursing care plan is to build a comprehensive patient database through thorough assessment and data collection. This involves employing a range of techniques and methods, including:
- Physical Assessment: A systematic physical assessment to gather objective data about the patient’s current health status.
- Health History: Obtaining a detailed health history to understand the patient’s past medical experiences, current concerns, and relevant lifestyle factors.
- Patient Interview: Conducting a structured interview to gather subjective data directly from the patient about their symptoms, perceptions, and needs.
- Medical Records Review: Examining existing medical records to access previous diagnoses, treatments, and relevant clinical information.
- Diagnostic Studies: Reviewing results from laboratory tests, imaging studies, and other diagnostic procedures to gain further insight into the patient’s condition.
This comprehensive patient database encompasses all relevant health information gathered. During this stage, the nurse analyzes the collected data to identify related or risk factors and defining characteristics. These elements are crucial for formulating accurate and relevant nursing diagnoses. Many healthcare agencies and nursing schools provide specific assessment formats to guide this data collection process, ensuring consistency and completeness.
Critical thinking is paramount in patient assessment. It involves integrating knowledge from various scientific disciplines and professional guidelines to inform clinical judgments. This process is fundamental for complex clinical decision-making. The ultimate goal is to effectively identify patients’ healthcare needs within a supportive environment that values reliable information and collaborative approaches.
Step 2: Data Analysis and Organization for Nursing Diagnoses
Once you have compiled a robust dataset of patient health information, the next step is to analyze, cluster, and organize this data. This analytical process is essential for formulating accurate nursing diagnoses, establishing priorities for care, and defining desired patient outcomes.
Step 3: Formulating Precise Nursing Diagnoses
Nursing diagnoses represent a standardized and precise way to identify, focus on, and address specific patient needs and responses to both actual and potential health problems. They are clinical judgments about a patient’s health status that nurses are qualified and licensed to treat independently. Nursing diagnoses focus on health problems that can be prevented or resolved through independent nursing interventions.
For a detailed guide on formulating effective nursing diagnoses, refer to this resource: Nursing Diagnosis (NDx): Complete Guide and List. This guide provides comprehensive steps and examples to help you master the art of nursing diagnosis.
Step 4: Setting Priorities for Nursing Care
Setting priorities involves establishing a logical and preferential order for addressing identified nursing diagnoses and planning subsequent interventions. In this step, the nurse collaborates with the patient to determine which problems require immediate attention and which can be addressed subsequently. Nursing diagnoses are typically ranked according to their urgency, often categorized as high, medium, or low priority. Life-threatening problems always take precedence and are designated as high priority.
A crucial framework for prioritizing nursing diagnoses is Maslow’s Hierarchy of Needs. This theory helps nurses to prioritize care based on fundamental human needs, progressing from basic physiological needs to higher-level needs like self-esteem and self-actualization. Developed in 1943 by Abraham Maslow, this hierarchy posits that basic physiological needs must be met before higher needs can be effectively addressed. Physiological and safety needs form the foundation of nursing care and interventions. They are positioned at the base of Maslow’s pyramid, providing the bedrock for physical and emotional well-being.
Maslow’s Hierarchy of Needs in Nursing Practice:
- Basic Physiological Needs: These are the most fundamental needs for survival and include: Nutrition (water and food), Elimination (Toileting), Airway (suctioning), Breathing (oxygen administration), Circulation (monitoring pulse, cardiac rhythm, and blood pressure), Sleep, Sex, Shelter, and Exercise. These are often referred to as the ABCs – Airway, Breathing, and Circulation – representing the highest priorities in immediate patient care.
- Safety and Security Needs: Once physiological needs are met, safety and security become paramount. These needs encompass: Injury prevention (using side rails, ensuring call lights are within reach, practicing hand hygiene, implementing isolation protocols when necessary, initiating suicide precautions, applying fall precautions, using car seats for infants and children, promoting helmet use, and ensuring seat belt use). Creating a climate of trust and safety is also crucial, fostering a therapeutic relationship and providing effective patient education on modifiable risk factors for conditions like stroke and heart disease.
- Love and Belonging Needs: Addressing social and emotional needs is essential for overall well-being. This includes: Fostering supportive relationships, implementing strategies to avoid social isolation (especially addressing issues like bullying), employing active listening techniques, using therapeutic communication, and supporting healthy expressions of sexual intimacy.
- Self-Esteem Needs: These needs relate to feelings of self-worth and accomplishment. They involve: Achieving acceptance within the community and workplace, experiencing personal achievements, fostering a sense of control or empowerment, and promoting acceptance of one’s physical appearance and body image.
- Self-Actualization Needs: Representing the highest level of human needs, self-actualization focuses on personal growth and fulfillment. This includes: Creating an empowering environment, supporting spiritual growth, developing the ability to understand and appreciate diverse perspectives, and facilitating the patient’s journey toward reaching their maximum potential.
Visual representation of Virginia Henderson’s 14 Needs integrated with Maslow’s Hierarchy, illustrating the interconnectedness of fundamental human needs in nursing care prioritization. Learn more about it here.
When prioritizing care, nurses must consider a range of factors, including the patient’s health values and beliefs, their own priorities, available resources, and the overall urgency of the situation. Actively involving the patient in this prioritization process is crucial to enhance their cooperation and ensure that care aligns with their values and preferences.
Step 5: Establishing Client-Centered Goals and Desired Outcomes
Following the prioritization of nursing diagnoses, the next crucial step involves collaborative goal setting. The nurse and the patient work together to establish goals for each prioritized diagnosis. Goals or desired outcomes are statements that describe what the nurse aims to achieve through the implementation of nursing interventions. These outcomes are directly derived from the patient’s nursing diagnoses. Well-defined goals serve several essential functions:
- Provide clear direction for planning targeted nursing interventions.
- Establish measurable criteria for evaluating patient progress and the effectiveness of care.
- Enable both the patient and the nurse to determine when problems have been successfully resolved.
- Enhance motivation for both the patient and the nurse by providing a sense of progress and achievement.
Examples of well-formulated goals and desired outcomes in a nursing care plan, demonstrating the use of specific, measurable, and patient-centered language.
For each nursing diagnosis, an overarching goal is typically established. The terms “goal outcomes” and “expected outcomes” are often used interchangeably in practice.
According to Hamilton and Price (2013), effective goals should adhere to the SMART criteria. SMART is an acronym that stands for:
- Specific: Goals should be clearly defined, significant to the patient’s needs, and sensible within the context of their health situation.
- Measurable or Meaningful: Measurable goals allow for objective tracking of progress and provide a clear indication of when the desired result has been achieved.
- Attainable or Action-Oriented: Goals should be challenging yet realistically achievable, focusing on actions the patient can take and changes that are within their capacity.
- Realistic or Results-Oriented: Goals should be relevant to the patient’s overall health priorities and achievable given available resources and the patient’s current capabilities.
- Timely or Time-Oriented: Every goal needs a defined timeframe, including a target date or period for achievement. This adds structure and promotes focused effort.
Hogston (2011) proposes the REEPIG standards as a complementary framework to ensure the highest quality of care planning. REEPIG emphasizes that nursing care plans should be:
- Realistic: Feasible and achievable given available resources, staffing, and the patient’s circumstances.
- Explicitly stated: Clearly and unambiguously written, leaving no room for misinterpretation of instructions or expected actions.
- Evidence-based: Grounded in current research and best practices, ensuring that interventions are supported by scientific evidence.
- Prioritized: Addressing the most urgent problems first, reflecting the prioritization of nursing diagnoses.
- Involve: Developed collaboratively, actively involving the patient and all relevant members of the multidisciplinary healthcare team.
- Goal-centered: Focused on achieving the established patient goals, with all planned interventions directly contributing to goal attainment.
Short-Term and Long-Term Goal Setting
Goals and expected outcomes must be both measurable and client-centered. Goal setting should focus on problem prevention, active problem resolution, and effective rehabilitation strategies. Goals are generally categorized as either short-term or long-term. In acute care settings, the majority of goals are short-term due to the emphasis on addressing immediate patient needs and acute conditions. Long-term goals are more commonly utilized for patients with chronic health problems or those receiving care in home settings, nursing homes, or extended-care facilities.
- Short-term goal: A statement that describes an anticipated change in patient behavior or health status that can be realistically achieved in a short timeframe, typically within a few hours or days.
- Long-term goal: An objective that is expected to be achieved over a more extended period, usually spanning weeks or months. Long-term goals are particularly relevant for patients managing chronic conditions or undergoing rehabilitation.
- Discharge planning: Primarily involves establishing long-term goals that extend beyond the acute care setting. Effective discharge planning promotes continued restorative care and ongoing problem resolution through home health services, physical therapy, and other appropriate referral sources.
Essential Components of Goals and Desired Outcomes
Well-formulated goals and desired outcome statements typically include four key components: a subject, a verb, conditions or modifiers, and a criterion of desired performance.
Breakdown of the components of effective goals and desired outcomes in a nursing care plan, emphasizing clarity and measurability.
- Subject: The subject is the focus of the goal and is typically the patient. It can also refer to a specific part of the patient (e.g., leg, wound), or a measurable attribute (e.g., pulse rate, temperature, urinary output). In most cases, the subject is implicitly understood to be the patient and is often omitted for brevity, unless the goal pertains to family members or a significant other.
- Verb: The verb specifies the action or behavior that the patient is expected to perform, demonstrate, learn, or experience. It should be an action-oriented verb.
- Conditions or modifiers: These elements provide context and detail by specifying the “what, when, where, or how” of the expected behavior. They clarify the circumstances under which the behavior is to be performed.
- Criterion of desired performance: The criterion sets the standard for evaluating performance or the level at which the patient will perform the specified behavior. Criteria are often expressed in quantifiable terms (e.g., “walk 50 feet,” “verbalize pain level less than 3/10”). While criteria enhance measurability, they are considered optional in some goal statements if the desired performance is inherently clear.
Key Tips for Writing Effective Goals and Desired Outcomes:
- Frame goals and outcomes in terms of observable patient responses, not as nursing activities. Start each goal statement with “Client will […]” to maintain a patient-centered focus on behavior and responses.
- Avoid phrasing goals in terms of what the nurse hopes to accomplish. Instead, focus on what the patient will actively do or achieve.
- Use observable and measurable terms for outcomes. Avoid vague words that require subjective interpretation or judgment.
- Ensure desired outcomes are realistic and achievable given the patient’s resources, capabilities, limitations, and the designated timeframe for care.
- Verify that goals are compatible with the overall treatment plan and therapies prescribed by other healthcare professionals.
- Ensure that each goal is derived from only one nursing diagnosis to facilitate clear evaluation of care and ensure interventions are directly linked to the diagnosed problem.
- Finally, confirm that the patient considers the goals important and values them. Patient buy-in is crucial for ensuring cooperation and active participation in achieving desired outcomes.
Step 6: Selecting and Implementing Nursing Interventions
Nursing interventions are the specific actions and activities that nurses implement to help patients achieve their established goals and desired outcomes. The interventions chosen should directly address the underlying cause (etiology) of the prioritized nursing problem or diagnosis. For risk diagnoses, interventions should focus on mitigating or reducing the patient’s identified risk factors. While nursing interventions are identified and documented during the planning phase of the nursing process, they are actively carried out during the implementation phase.
Types of Nursing Interventions: Independent, Dependent, and Collaborative
Nursing interventions can be broadly categorized into three types: independent, dependent, and collaborative.
Visual representation of the three types of nursing interventions – independent, dependent, and collaborative – illustrating the scope of nursing actions in patient care plans.
- Independent Nursing Interventions: These are actions that nurses are authorized and competent to initiate based on their professional knowledge, judgment, and skills. Independent interventions encompass a wide range of nursing activities, including: ongoing patient assessment, providing emotional support, offering comfort measures, patient education, delivering physical care, and making referrals to other healthcare professionals or community resources.
- Dependent Nursing Interventions: These are actions that require a physician’s order or supervision to be implemented. Dependent interventions typically include: administering medications, managing intravenous therapy, performing diagnostic tests, providing specific treatments, implementing dietary orders, and managing activity or rest prescriptions. Nurses play a crucial role in dependent interventions by conducting assessments related to the ordered intervention and providing patient education and explanations.
- Collaborative Interventions: These are actions that nurses carry out in partnership and consultation with other members of the healthcare team. Collaborative interventions involve working with physicians, social workers, dietitians, physical therapists, and other specialists to develop a comprehensive and integrated care plan. These interventions leverage the expertise of different disciplines to address complex patient needs holistically.
Key Criteria for Effective Nursing Interventions:
- Safe and Appropriate: Interventions must be safe and suitable for the patient’s age, overall health status, and specific condition.
- Achievable and Realistic: Interventions should be realistically achievable given available resources, staffing levels, and the time constraints of the care setting.
- Aligned with Patient Values: Interventions should be consistent with the patient’s personal values, cultural background, and beliefs to promote patient engagement and adherence.
- Integrated with Other Therapies: Interventions should be coordinated and compatible with other therapies the patient is receiving from different healthcare providers.
- Evidence-Based: Interventions should be grounded in established nursing knowledge, clinical experience, and relevant scientific evidence or knowledge from related disciplines.
Essential Tips for Documenting Nursing Interventions:
- Date and Sign the Plan: Always date the care plan when it is written. The date is crucial for tracking plan implementation, evaluation timelines, and future reviews. The nurse’s signature demonstrates professional accountability for the plan of care.
- Specificity and Clarity: Nursing interventions should be written with specificity and clarity. Begin each intervention statement with an action verb that clearly indicates what the nurse is expected to do. Action verbs provide precision and direction. Include qualifiers that specify how, when, where, at what time, with what frequency, and in what amount the intervention should be carried out. For example: “Educate parents on the proper technique for taking their child’s temperature and instruct them to notify the healthcare provider of any significant changes,” or “Assess the patient’s urine for color, amount, odor, and turbidity every shift.”
- Use Approved Abbreviations: Use only abbreviations that are officially accepted and recognized by the healthcare institution to ensure clear communication and avoid potential misunderstandings.
Step 7: Providing Rationales: The “Why” Behind Interventions
Rationales, also known as scientific explanations or supporting evidence, are essential for justifying the selection of specific nursing interventions in the NCP. They articulate why a particular intervention is chosen and how it is expected to address the patient’s nursing diagnosis and achieve the desired outcome.
Example of nursing interventions paired with their corresponding rationales in a care plan, demonstrating the scientific basis for nursing actions.
While rationales are typically not included in routine care plans used by practicing nurses, they are a critical component of student care plans. Rationales serve as a valuable learning tool, helping nursing students connect pathophysiological and psychological principles to the practical application of nursing interventions. They bridge the gap between theoretical knowledge and clinical practice.
Step 8: Evaluation: Assessing Progress and Plan Effectiveness
Evaluation is a systematic, ongoing, and purposeful process in which the patient’s progress toward achieving the established goals and desired outcomes is rigorously assessed. It also involves evaluating the overall effectiveness of the nursing care plan (NCP). Evaluation is an indispensable aspect of the nursing process because the conclusions drawn from this step directly inform future care decisions. The evaluation determines whether the current nursing interventions should be:
- Terminated: If the patient has fully achieved the desired outcomes and the problem is resolved.
- Continued: If the patient is making satisfactory progress, and the plan remains effective.
- Modified: If the patient is not progressing as expected, or if new needs or challenges have emerged, requiring adjustments to the care plan.
Step 9: Documenting the Care Plan
The patient’s care plan is a crucial part of their permanent medical record. It is formally documented according to the policies and procedures of the healthcare facility. The documented care plan serves as a vital communication tool for the entire healthcare team, including oncoming nurses who rely on it to ensure continuity of care. Different nursing programs and healthcare settings may utilize various care plan formats. However, most formats are designed to guide nurses (and especially students) through the logical and interconnected steps of the nursing process. The five-column format is a commonly used structure in many educational settings and healthcare agencies.
Comprehensive Nursing Care Plan List
This section provides an extensive list of sample nursing care plans (NCPs) and nursing diagnoses categorized by medical specialties and health conditions. These resources offer valuable examples and templates to guide your care planning process.
(The extensive list of care plans from the original article is included here, categorized as in the original, but is omitted in this response for brevity, as per instructions.)
Recommended Resources for Nursing Care Planning
To further enhance your skills in nursing diagnosis and care planning, consider these highly recommended books and resources:
Disclosure: The following are affiliate links from Amazon. Purchases made through these links may generate a small commission for us, at no additional cost to you. For more details, please review our privacy policy.
Ackley and Ladwig’s Nursing Diagnosis Handbook: An Evidence-Based Guide to Planning Care Highly favored for its evidence-based approach to nursing interventions. This handbook offers a user-friendly, three-step system to guide you through patient assessment, nursing diagnosis formulation, and care plan development. It provides step-by-step instructions on implementing care and evaluating outcomes, effectively building your diagnostic reasoning and critical thinking skills.
Nursing Care Plans – Nursing Diagnosis & Intervention (10th Edition) Features over two hundred care plans reflecting the latest evidence-based guidelines. This edition includes new ICNP diagnoses, care plans addressing LGBTQ health issues, and expanded content on electrolytes and acid-base balance.
Nurse’s Pocket Guide: Diagnoses, Prioritized Interventions, and Rationales A quick and practical reference tool that includes essential information for accurate diagnosis and efficient care planning. The sixteenth edition features the most current nursing diagnoses and interventions, with an alphabetized listing covering over 400 disorders.
Nursing Diagnosis Manual: Planning, Individualizing, and Documenting Client Care An essential manual for identifying interventions to effectively plan, individualize, and document care for over 800 diseases and disorders. This manual uniquely provides, for each diagnosis, subjective and objective data, sample clinical applications, prioritized action/interventions with rationales, documentation guidance, and much more.
All-in-One Nursing Care Planning Resource – E-Book: Medical-Surgical, Pediatric, Maternity, and Psychiatric-Mental Health This comprehensive e-book includes over 100 care plans spanning medical-surgical, maternity/OB, pediatrics, and psychiatric-mental health nursing. It utilizes interprofessional “patient problems” to familiarize you with effective patient communication strategies.
References and Sources
(The original article’s references/sources section would be included here.)