Diabetes Mellitus (DM) is a prevalent, chronic metabolic condition characterized by the body’s impaired ability to metabolize carbohydrates, fats, and proteins effectively due to issues with insulin production or utilization. This dysfunction leads to hyperglycemia, or elevated blood glucose levels, which can have significant long-term health consequences if not properly managed. Understanding diabetes, formulating accurate nursing diagnoses, and implementing effective care plans are crucial skills for nurses to ensure optimal patient outcomes.
Types of Diabetes Mellitus
Diabetes is not a singular disease but rather a spectrum of conditions, each with distinct etiologies and management approaches. The primary types include:
Type 1 Diabetes: Characterized by an autoimmune reaction that destroys the insulin-producing beta cells within the pancreas. Genetic predisposition and viral infections are considered potential contributing factors. Individuals with Type 1 diabetes require exogenous insulin to survive.
Type 2 Diabetes: The most common form, Type 2 diabetes develops gradually over time. It is primarily caused by insulin resistance, where the body’s cells do not respond effectively to insulin, and eventually, the pancreas may not produce enough insulin to overcome this resistance. Lifestyle factors such as obesity, inactivity, and genetics play significant roles in its development.
Gestational Diabetes Mellitus (GDM): This type of diabetes develops during pregnancy in women who have not previously been diagnosed with diabetes. Hormonal changes during pregnancy can lead to insulin resistance. GDM typically resolves after childbirth, but it significantly increases the mother’s risk of developing Type 2 diabetes later in life and poses risks to the baby.
Prediabetes: A precursor to Type 2 diabetes, prediabetes is a condition where blood glucose levels are higher than normal but not yet high enough to be classified as Type 2 diabetes. A fasting blood glucose level between 100-125 mg/dL is indicative of prediabetes. It is a critical window for intervention to prevent or delay the onset of Type 2 diabetes through lifestyle modifications.
Understanding Hypoglycemia and Hyperglycemia
Managing diabetes effectively requires a thorough understanding of both hypoglycemia (low blood sugar) and hyperglycemia (high blood sugar), as these represent acute imbalances that can have immediate and long-term health implications.
Hypoglycemia: Low Blood Sugar
Hypoglycemia is defined as a blood glucose level below 70 mg/dL. It is a potentially dangerous condition requiring immediate intervention.
Causes of Hypoglycemia
Hypoglycemia can be triggered by various factors, including:
- Excessive insulin dosage
- Missed or delayed meals or insufficient carbohydrate intake
- Unplanned or excessive physical activity
- Alcohol consumption, especially without food
- Timing of insulin administration in relation to meals and activity
- Environmental factors like hot and humid weather
- Hormonal fluctuations related to puberty or menstruation
Hyperglycemia: High Blood Sugar
Hyperglycemia refers to elevated blood glucose levels due to insufficient insulin in the bloodstream. Hyperglycemia is diagnosed with a fasting blood glucose level exceeding 125 mg/dL or a blood glucose level of 180 mg/dL or higher one to two hours after eating.
Causes of Hyperglycemia
Hyperglycemia can result from:
- Dietary indiscretions, particularly consuming excessive carbohydrates
- Physical inactivity
- Illness or infection
- Emotional or physical stress
- Certain medications, such as steroids
- Improper use of diabetes medications (insulin or oral agents), including missed doses or incorrect dosages
Alt text: A chart illustrating normal, prediabetes, and diabetes blood sugar levels in both fasting and 2-hour postprandial states, emphasizing ranges for effective diabetes management.
Nursing Assessment for Diabetes Mellitus
The nursing assessment is the cornerstone of effective diabetes care. It involves a comprehensive evaluation of the patient’s physical, psychosocial, emotional, and diagnostic data.
Review of Health History
1. General Symptom Assessment:
Recognizing the signs and symptoms of both hypoglycemia and hyperglycemia is crucial.
Hypoglycemia Symptoms:
- Palpitations
- Tremors and shaking
- Diaphoresis (sweating)
- Anxiety and nervousness
- Confusion
- Dizziness
- Intense hunger
Hyperglycemia Symptoms:
- Polyuria (frequent urination)
- Polydipsia (increased thirst)
- Polyphagia (increased hunger)
- Blurred vision
- Burning, tingling, or numbness in the extremities (neuropathy)
- Fatigue
- Headaches
- Balanitis (inflammation of the glans penis) in men
Gestational Diabetes Symptoms:
Women with gestational diabetes may be asymptomatic; however, when symptoms are present, they often mimic hyperglycemia:
- Increased urination
- Increased hunger
- Increased thirst
- Blurred vision
- Nausea and vomiting
2. Duration of Diabetes and Treatment History:
Inquire about the duration of the patient’s diabetes diagnosis and past and current treatments. The length of time living with diabetes and the degree of glycemic control are directly linked to the risk of long-term complications.
3. Age at Diagnosis:
Note the patient’s age when diagnosed. Type 1 diabetes is often diagnosed in childhood or adolescence, while Type 2 diabetes is more common in adults, particularly after age 40.
4. Risk Factor Assessment:
Identify both non-modifiable and modifiable risk factors for diabetes.
Non-modifiable Risk Factors:
- Family History: A family history of diabetes increases the risk. Specific genetic mutations are associated with MODY (maturity-onset diabetes of the young) and neonatal diabetes.
- Race/Ethnicity: Certain ethnic groups, including Black, Hispanic, American Indian, and Asian Americans, have a higher prevalence of Type 2 diabetes.
- Age: The risk of prediabetes and Type 2 diabetes increases with age.
- Autoimmune Diseases: Conditions where the immune system attacks pancreatic beta cells can lead to LADA (latent autoimmune diabetes in adults) and Type 1 DM.
- Hormonal Imbalances: Can contribute to gestational diabetes and Type 2 diabetes by impacting insulin resistance.
Modifiable Risk Factors:
- Obesity and Unhealthy Diet: Diets high in fat, calories, and cholesterol, and obesity significantly increase diabetes risk.
- Smoking: Smokers have a 30-40% increased risk of Type 2 diabetes compared to non-smokers. Smoking also complicates diabetes management and increases complication risks.
- Excessive Alcohol Consumption: Can reduce insulin sensitivity, increasing the risk of Type 2 diabetes.
- Sedentary Lifestyle: Physical inactivity increases insulin resistance and the risk of prediabetes and Type 2 diabetes.
- Chronic Conditions: Conditions like hypertension and hyperlipidemia increase diabetes risk and complications.
5. History of Yeast Infections:
Assess for recurrent yeast infections, as high glucose levels promote yeast proliferation. Glycosuria (sugar in the urine) due to hyperglycemia creates an environment conducive to yeast overgrowth.
6. Diabetes-Related Complications:
Evaluate for existing complications from diabetes (Type 1 and Type 2):
- Cardiovascular Disease: Diabetes damages blood vessels and nerves, increasing the risk of hypertension, hyperlipidemia, coronary artery disease, angina, myocardial infarction, and cerebrovascular accidents.
- Neuropathy: Nerve damage from hyperglycemia leads to symptoms like tingling, numbness, burning pain, poor balance, reduced sensation, and increased risk of foot ulcers and amputations.
- Renal Disease (Nephropathy): Damage to kidney blood vessels can lead to kidney damage, potentially requiring dialysis or kidney transplant.
- Retinopathy: Damage to retinal blood vessels can cause diabetic retinopathy, increasing the risk of glaucoma, cataracts, and blindness.
- Foot Damage: Neuropathy and poor circulation in the feet increase the risk of foot ulcers, infections, and slow healing.
- Depression: The complexity of diabetes management can contribute to depression, further complicating glycemic control.
7. Blood Glucose Monitoring Records:
Review patient’s home glucose monitoring records to identify patterns of hypo- or hyperglycemia and assess overall glycemic control.
Physical Assessment
Patients with well-managed diabetes may not exhibit overt physical symptoms.
1. Vital Signs:
- Blood Pressure and Respiratory Rate: Monitor for hypertension, common in diabetes. Assess for orthostatic hypotension, indicative of autonomic neuropathy. Note Kussmaul respirations, which are deep, rapid breaths suggestive of diabetic ketoacidosis (DKA).
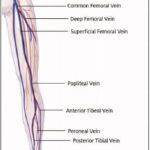
2. Peripheral Pulses:
- Lower Extremity Pulses: Palpate and document dorsalis pedis and posterior tibialis pulses to assess for vascular compromise.
3. Foot Assessment:
- Comprehensive Foot Exam: Essential to identify neuropathy and risk of ulceration. Use Semmes-Weinstein monofilament test to assess sensory neuropathy, along with reflex and vibration perception testing. Assess for existing foot ulcers.
4. Weight Assessment:
- Weight Changes: In Type 1 diabetes, weight loss may occur due to glucose loss and dehydration. In Type 2 diabetes, assess for overweight or obesity, as these exacerbate insulin resistance.
Diagnostic Procedures
1. Blood Glucose Testing:
Blood glucose levels are fundamental in diagnosing diabetes.
Diagnostic Criteria:
- Type 1 DM:
- Fasting glucose ≥ 126 mg/dL
- Random glucose ≥ 200 mg/dL
- HbA1c ≥ 6.5%
- Type 2 DM:
- Fasting glucose levels and HbA1c testing are used for diagnosis and monitoring.
- Prediabetes:
- Fasting blood sugar (FBS) 100 to 125 mg/dL
- 2-hour post-oral glucose tolerance test (post-OGTT) glucose level of 140 to 200 mg/dL
- Gestational Diabetes:
- Screening at 24-28 weeks gestation: 1-hour glucose challenge test.
- Diagnostic 3-hour glucose tolerance test if 1-hour test is ≥ 140 mg/dL.
2. Additional Lab Tests:
- Urine Albumin: To detect early diabetic nephropathy, especially in Type 1 DM.
- Serum Lipid Profile: Assessed at diagnosis and regularly thereafter due to increased cardiovascular risk in diabetic patients.
- Thyroid Function Tests: Annual testing recommended due to higher prevalence of hypothyroidism in individuals with diabetes.
Alt text: A close-up image of a glucometer displaying a blood glucose reading, highlighting the importance of regular monitoring in diabetes management.
Nursing Interventions for Diabetes Management
Effective nursing interventions are crucial for managing diabetes, controlling glycemia, and preventing complications.
Glycemic Control Strategies
1. Promote Patient Adherence:
Patient participation is paramount. Encourage adherence to specialist appointments, including endocrinologists or primary care providers managing their diabetes. Emphasize the impact of lifestyle choices on glycemic control and reinforce diet and exercise adherence.
2. Diabetes Education:
Comprehensive education is critical. Educate patients about treatment options and how diet, stress, medications, and exercise affect glucose levels. Refer to a certified diabetes nurse educator for personalized education.
3. Home Glucose Monitoring:
Teach patients to use a home glucose monitoring device and record results, often up to four times daily, to maintain optimal glucose ranges. Continuous glucose monitors (CGMs) are also an option, especially for children or those using insulin pumps, providing real-time glucose data.
4. Maintain Target Glucose Levels:
Aim for an HbA1c below 7% and blood sugar levels between 90 and 130 mg/dL to minimize long-term complications.
5. Tailored Treatment Plans:
Recognize differences in treatment for Type 1 and Type 2 DM.
Type 1 DM Treatments:
- Insulin injections or insulin pump therapy
- Regular blood sugar monitoring
- Carbohydrate counting
- In select cases, islet cell or pancreas transplantation
Type 2 DM Treatments:
- Lifestyle modifications (diet and exercise)
- Blood sugar monitoring
- Oral diabetic medications
- Insulin therapy may be required
6. Insulin Administration Education:
Educate patients on proper insulin administration techniques, including different types of insulin (rapid-acting, short-acting, intermediate-acting, long-acting), drawing up insulin, using insulin pens, and assess return demonstrations.
7. Insulin Pump Management:
Provide training and support for patients using wearable insulin pumps, which deliver continuous rapid-acting insulin and can be programmed for bolus doses for meals.
8. Closed-Loop Insulin Delivery Systems:
Explain closed-loop systems (artificial pancreas), which integrate a CGM with an insulin pump to automatically adjust insulin delivery based on real-time glucose readings.
9. Oral Diabetes Medications Education:
Educate patients on various classes of oral diabetes medications for Type 2 DM, prediabetes, and gestational diabetes:
- Alpha-glucosidase inhibitors: Delay carbohydrate absorption.
- Biguanides (metformin): Reduce hepatic glucose production and improve insulin sensitivity.
- Bile acid sequestrants (BASs): Lower cholesterol and may modestly reduce blood sugar.
- Dopamine-2 agonists: Affect circadian rhythms to reduce hepatic glucose production and improve insulin resistance.
- DPP-4 inhibitors (gliptins): Enhance incretin hormones to increase insulin release and decrease glucagon secretion.
- Meglitinides (glinides): Stimulate rapid insulin secretion from the pancreas.
- SGLT2 inhibitors: Increase glucose excretion in the urine.
- Sulfonylureas: Stimulate insulin release from the pancreas.
- Thiazolidinediones (TZDs): Improve insulin sensitivity in muscle and fat tissue.
10. Pancreas Transplant Considerations:
Discuss pancreas transplantation as an option for select individuals with Type 1 DM who struggle with glycemic control or require a kidney transplant. Highlight the risks and the need for lifelong immunosuppression.
11. Meal Planning Guidance:
Educate patients on diabetic diets, emphasizing reduced carbohydrates, processed foods, and sugars. Focus on increasing intake of fruits, vegetables, lean proteins, and whole grains. Involve patients in meal planning to enhance adherence.
12. Nutritionist/Dietitian Referral:
Refer patients to registered dietitians or nutritionists for personalized meal planning, carbohydrate counting education (especially for Type 1 DM or insulin users), and dietary guidance tailored to their lifestyle and preferences.
13. Promote Physical Activity:
Encourage at least 150 minutes of moderate physical activity per week. Exercise improves insulin sensitivity and lowers blood glucose. Advise patients to obtain medical clearance before starting new exercise programs.
14. Weight Management:
For overweight or obese patients with Type 2 DM or prediabetes, even a modest weight loss (e.g., 7%) can significantly improve glycemic control.
15. Gestational Diabetes Management:
Manage gestational diabetes through blood sugar monitoring, dietary modifications, and potentially oral hypoglycemic agents or insulin. Monitor blood sugar during labor and postpartum due to the risk of neonatal hypoglycemia.
16. Diabetes Prevention Strategies:
For prediabetes, emphasize lifestyle changes including healthy diet, exercise, and weight management to prevent progression to Type 2 diabetes. Metformin and other medications may be considered in some high-risk individuals.
17. Endocrinologist Referral:
Refer patients to endocrinologists or diabetologists for specialized diabetes care and management of complex cases.
Prevention of Diabetes Complications
1. Medical Alert Identification:
Advise patients to wear a medical alert ID to provide crucial medical information in emergencies, such as DKA or severe hypoglycemia.
2. Ophthalmologist Referrals:
Recommend annual eye exams by an ophthalmologist to screen for retinopathy, cataracts, and glaucoma.
3. Vaccination Recommendations:
Promote recommended vaccinations, as diabetes can impair immune function.
4. Foot Care Education:
Educate on daily foot inspection, proper washing and drying (especially between toes), avoiding lotion between toes, and regular podiatry visits for nail care and neuropathy management.
5. Blood Pressure and Cholesterol Management:
Educate on lifestyle modifications and medications to manage blood pressure and cholesterol to reduce cardiovascular risk.
6. Oral Hygiene Education:
Emphasize twice-daily brushing and flossing, and regular dental exams to prevent gum disease.
7. Smoking Cessation Counseling:
Strongly encourage smoking cessation due to the significantly increased risk of diabetes complications and cardiovascular disease.
8. Moderate Alcohol Consumption:
Advise on moderate alcohol intake (no more than one drink per day for women, two for men) and to consume alcohol with food due to its effects on blood glucose.
9. Stress Management Techniques:
Teach stress-reduction techniques, as chronic stress can negatively impact blood glucose levels.
10. Diabetes Nurse Educator Coordination:
Coordinate with diabetes nurse educators to provide comprehensive and ongoing diabetes self-management education and support.
11. DSMES Program Referrals:
Refer patients to Diabetes Self-Management Education and Support (DSMES) programs to improve self-efficacy, coping skills, healthy behaviors, and overall health outcomes.
Diabetes Nursing Care Plans Examples
Nursing care plans provide structured frameworks for addressing patient needs and prioritizing interventions. Here are examples of nursing diagnoses and associated care plans relevant to diabetes mellitus.
Decreased Cardiac Output
Nursing Diagnosis: Decreased Cardiac Output related to cellular dysfunction secondary to insulin resistance or uncontrolled blood glucose levels.
Related Factors:
- Elevated blood glucose levels
- Impaired myocardial contractility
- Increased afterload
- Decreased myocardial oxygenation
- Increased cardiac inflammation
Evidenced by:
- Tachycardia
- Tachypnea
- Dyspnea
- Orthopnea
- Reduced oxygen saturation
- Hypotension
- Decreased central venous pressure
- Dysrhythmia
- Fatigue
- Change in level of consciousness
- Anxiety/Restlessness
- Decreased activity tolerance
- Edema
- Decreased peripheral pulses
- Decreased urine output
Expected Outcomes:
- Patient will demonstrate adequate cardiac output as evidenced by stable vital signs, strong peripheral pulses, and appropriate urine output.
- Patient will report absence of dyspnea, palpitations, and altered mentation.
- Patient will maintain intact skin without breakdown.
Nursing Assessments:
- Monitor heart rate and blood pressure: Assess for tachycardia and hypotension.
- Assess EKG: Monitor for arrhythmias via telemetry.
- Daily weights: Monitor for fluid retention.
- Cardiac history: Assess for pre-existing cardiac conditions exacerbated by diabetes.
Nursing Interventions:
- Oxygen administration: Provide supplemental oxygen as needed.
- Promote rest: Encourage physical and emotional rest to reduce cardiac workload.
- Assist with echocardiography: Prepare patient for diagnostic echocardiogram.
- Medication administration: Administer prescribed medications, such as SGLT2 inhibitors, which can improve cardiac outcomes in diabetes.
- Diabetes education: Emphasize the link between diabetes and cardiac dysfunction to enhance treatment adherence.
Ineffective Peripheral Tissue Perfusion
Nursing Diagnosis: Ineffective Tissue Perfusion related to endothelial damage from chronic hyperglycemia.
Related Factors:
- Impaired oxygen transport
- Interrupted blood flow
- Elevated blood glucose levels
- Neuropathy
- Peripheral vascular disease
- Insufficient knowledge of diabetes management
Evidenced by:
- Weak or absent peripheral pulses
- Numbness
- Pain in extremities
- Cool, clammy skin
- Discrepancy in BP between extremities
- Prolonged capillary refill
- Delayed wound healing
- Altered sensation
Expected Outcomes:
- Patient will maintain optimal peripheral tissue perfusion, evidenced by strong pulses, warm extremities, and normal capillary refill.
- Patient will report absence of burning or numbness in extremities.
Nursing Assessments:
- Orthostatic blood pressure: Monitor for orthostatic hypotension.
- Doppler ultrasound: Assess peripheral pulses with Doppler if needed.
- Skin assessment: Evaluate skin texture, color, and presence of ulcers, noting signs of arterial or venous insufficiency.
Nursing Interventions:
- Glycemic control: Maintain blood glucose within target range through medication and education.
- Compression stockings: Encourage use to improve venous return.
- Foot care: Provide comprehensive foot care and refer to podiatry.
- Smoking cessation: Counsel on smoking cessation.
- Lifestyle education: Educate on diet and exercise to improve perfusion and manage diabetes risk factors.
Risk for Unstable Blood Glucose Level
Nursing Diagnosis: Risk For Unstable Blood Glucose Level related to factors affecting glucose regulation.
Related Factors:
- Alterations in physical activity
- New diagnosis and unfamiliarity with management
- Weight changes
- Inadequate glucose monitoring
- Incorrect insulin administration
- Non-adherence to antidiabetic medications
- Inconsistent dietary intake
- Pregnancy
- Illness
Evidenced by:
- Risk diagnosis, evidenced by risk factors, not signs and symptoms.
Expected Outcomes:
- Patient will achieve and maintain blood glucose levels within acceptable range.
- Patient will verbalize factors that influence glucose levels.
- Patient will describe symptoms of hypoglycemia and hyperglycemia and appropriate actions.
Nursing Assessments:
- Hypo/hyperglycemia symptoms: Monitor for signs and symptoms of both conditions.
- Activity level: Assess patient’s physical activity patterns.
- HbA1c levels: Review HbA1c for long-term glucose control assessment.
- Diabetes knowledge: Evaluate patient’s understanding of diabetes management.
- Support system: Assess available support for diabetes management.
Nursing Interventions:
- Medication administration: Administer prescribed oral and injectable diabetes medications as ordered.
- Carbohydrate counting education: Instruct on carbohydrate counting.
- Glucose monitoring education: Train patient on blood glucose monitoring techniques.
- Hypoglycemia management education: Teach patients how to recognize and treat hypoglycemia.
- DSME referral: Refer to Diabetes Self-Management Education programs.
References
- American Diabetes Association. (2023). Standards of medical care in diabetes—2023 abridged for primary care providers. Clinical Diabetes, 41(1), 4-31.
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). (2022). Diabetes mellitus.
- Smeltzer, S. C., Bare, B. G., Hinkle, J. L., & Cheever, K. H. (2022). Brunner & Suddarth’s textbook of medical-surgical nursing (15th ed.). Wolters Kluwer.