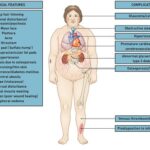
Dengue fever, a prevalent mosquito-borne viral illness, demands meticulous nursing care to manage its varied symptoms and avert potential complications. As a healthcare professional, particularly in nursing, understanding the nuances of a dengue fever diagnosis and care plan is paramount for effective patient management. This detailed nursing care plan serves as an essential guide, focusing on evidence-based interventions to accurately assess, manage symptoms, and facilitate the recovery of patients affected by dengue fever.
A Diagnosis Nursing Care Plan For Dengue Fever is intricately designed to address symptom management, complication prevention, and overall patient support throughout this mosquito-transmitted viral infection. Dengue fever, triggered by the dengue virus and propagated by Aedes mosquitoes, is a significant health concern in tropical and subtropical zones. Patients typically present with high fever, intense headaches, muscle and joint pain, and skin rashes. Severe cases can escalate to dengue hemorrhagic fever or dengue shock syndrome, underscoring the critical need for timely and comprehensive nursing interventions.
This care plan emphasizes vigilant monitoring of vital signs, ensuring optimal hydration, and providing effective pain relief, all aimed at enhancing patient comfort and promoting well-being. Furthermore, patient education plays a crucial role, focusing on mosquito bite prevention strategies and the ability to recognize early warning signs of severe dengue, essential for both individual health and public health efforts to control disease spread. This nursing care plan is structured to deliver targeted nursing actions that bolster the patient’s immune response, effectively manage distressing symptoms, and mitigate potential risks, thereby fostering a safer and more effective recovery journey.
 nursing care plan for dengue fever
nursing care plan for dengue fever
Alt text: A detailed nursing care plan chart for dengue fever diagnosis and management, outlining key assessment points, nursing interventions, and expected patient outcomes.
Patient Information:
- Name: [Patient’s Name]
- Age: [Patient’s Age]
- Gender: [Patient’s Gender]
- Medical History: [Brief summary of patient’s medical history, including pre-existing conditions like diabetes, hypertension, or any immunocompromising conditions]
- Type of Dengue: [Specify if dengue fever, dengue hemorrhagic fever (DHF), or dengue shock syndrome (DSS) if diagnosed]
- Symptoms: [Detailed description of presenting symptoms, including fever pattern, headache location and intensity, rash characteristics (macular, papular, petechial), joint and muscle pain severity, presence of gastrointestinal symptoms, and any bleeding manifestations]
- Medical Diagnosis: Dengue Fever (ICD-10 code: A90)
- Admission Date: [Date of Hospital Admission]
- Care Plan Initiated: [Date Care Plan Implementation Began]
Nursing Assessment:
A comprehensive nursing assessment is the cornerstone of effective care for patients with dengue fever. It is crucial for early symptom identification, monitoring disease progression, and guiding the implementation of targeted nursing interventions. The assessment encompasses both subjective patient reports and objective clinical findings:
Subjective Data:
- Patient’s description of symptoms: “I have a terrible headache behind my eyes,” “My muscles and joints ache all over,” “I feel extremely hot and cold,” “I’m very tired and weak.”
- Reports of symptom onset and duration: “The fever started three days ago and hasn’t gone down,” “The rash appeared yesterday on my chest and is spreading.”
- Patient concerns and anxieties: “I’m worried about bleeding because my gums bled this morning,” “I’m scared because my neighbor had severe dengue.”
Objective Data:
- Vital Signs:
- Temperature: Document elevated temperature readings (e.g., 39.5°C or 103.1°F), noting the pattern (continuous, intermittent, remittent).
- Blood Pressure: Record blood pressure, observing for hypotension (systolic BP < 90 mmHg) as a sign of potential shock.
- Heart Rate: Assess heart rate for tachycardia (HR > 100 bpm), which may indicate fever, dehydration, or early shock.
- Respiratory Rate: Monitor respiratory rate for tachypnea (RR > 20 breaths/min), which could suggest respiratory distress or compensation for shock.
- Oxygen Saturation (SpO2): Measure SpO2 to detect hypoxemia, especially in severe cases or those with respiratory symptoms.
- Physical Examination:
- Skin: Observe for dengue rash (maculopapular, petechial), noting distribution, characteristics, and any signs of bleeding (petechiae, purpura, ecchymosis). Assess skin turgor for dehydration.
- Mucous Membranes: Evaluate for dryness, indicating dehydration. Check for bleeding gums or oral mucosal bleeding.
- Lymph Nodes: Palpate for lymphadenopathy, which may be present in dengue fever.
- Abdomen: Assess for abdominal tenderness, particularly in the right upper quadrant, which can indicate liver involvement. Palpate for hepatomegaly.
- Laboratory Findings:
- Complete Blood Count (CBC): Review platelet count for thrombocytopenia (platelets < 150,000/µL), a hallmark of dengue. Monitor hematocrit levels for hemoconcentration (increased hematocrit > 20% baseline), suggesting plasma leakage. Assess white blood cell count, which may initially be low or normal.
- Dengue Serology/PCR: Check results of dengue NS1 antigen test, IgM/IgG antibody tests, or RT-PCR for dengue virus RNA to confirm diagnosis.
- Liver Function Tests (LFTs): Evaluate liver enzymes (AST, ALT) for elevation, indicating liver involvement (dengue hepatitis).
- Electrolytes: Monitor serum electrolytes (sodium, potassium) as imbalances can occur, especially with dehydration or intravenous fluid therapy.
- Coagulation Studies: In severe cases, review prothrombin time (PT) and activated partial thromboplastin time (aPTT) to assess for coagulopathy.
- Urine Specific Gravity: Assess urine specific gravity as an indicator of hydration status.
Detailed Assessment Categories:
1. Vital Signs Monitoring:
- Temperature Pattern: Chart the fever curve to identify typical dengue fever patterns (biphasic fever).
- Blood Pressure Trends: Track blood pressure readings to detect trends toward hypotension, indicative of worsening condition.
- Pulse Pressure: Note narrowing pulse pressure (difference between systolic and diastolic BP), which can be an early sign of shock.
2. Hydration Status Evaluation:
- Fluid Balance Chart: Maintain accurate records of oral and intravenous fluid intake and all outputs (urine, vomit, diarrhea, insensible losses).
- Capillary Refill Time: Assess capillary refill time (>2 seconds suggests dehydration or poor perfusion).
- Urine Output: Monitor hourly urine output if critically ill; decreased output (< 0.5 mL/kg/hour) suggests inadequate renal perfusion.
3. Pain and Symptom Assessment:
- Pain Scales: Use standardized pain scales (numerical rating scale, visual analog scale) to quantify pain intensity (headache, myalgia, arthralgia).
- Pain Characteristics: Document location, quality (throbbing, aching), radiation, and aggravating/relieving factors of pain.
- Non-Pain Symptoms: Inquire about and document associated symptoms like nausea, vomiting, anorexia, and altered taste.
4. Bleeding Risk Assessment:
- Tourniquet Test: Perform tourniquet test (if indicated and as per local guidelines) to assess capillary fragility.
- Bleeding History: Inquire about any history of bleeding disorders or anticoagulant use.
- Early Bleeding Signs: Actively look for and document early signs of bleeding such as epistaxis, gingival bleeding, easy bruising, and menorrhagia in women.
5. Skin and Mucosal Membrane Integrity:
- Rash Progression: Document the evolution of the dengue rash, from initial appearance to resolution. Note any blistering or secondary skin infections.
- Pruritus Assessment: Evaluate the severity of itching associated with the rash and its impact on patient comfort and skin integrity.
6. Neurological Status:
- Glasgow Coma Scale (GCS): Assess level of consciousness using GCS, especially if there are signs of encephalopathy or severe dengue.
- Neurological Signs: Monitor for restlessness, irritability, confusion, lethargy, seizures, or focal neurological deficits.
7. Psychosocial Assessment:
- Anxiety and Fear: Assess the patient’s and family’s anxiety levels related to the illness and potential complications.
- Coping Mechanisms: Evaluate the patient’s usual coping strategies and support systems.
- Educational Needs: Determine the patient’s and family’s understanding of dengue fever, treatment, and home care.
This detailed and systematic nursing assessment is crucial for identifying specific patient needs and formulating individualized nursing diagnoses and interventions. Regular reassessments are essential to monitor disease progression and adjust the care plan as needed.
Nursing Diagnosis:
Based on the comprehensive assessment, several nursing diagnoses may be pertinent for a patient with dengue fever. These diagnoses address the patient’s actual and potential health problems:
1. Hyperthermia related to dengue viral infection, as evidenced by elevated body temperature (39°C/102.2°F), flushed skin, and patient report of feeling hot.
- Supporting Data: Temperature of 39°C orally, skin warm to touch, patient states “I feel like I’m burning up.”
- Desired Outcome: Patient will achieve and maintain a normal body temperature (36.5°C-37.5°C / 97.7°F-99.5°F) within 24-48 hours, as evidenced by temperature readings within normal limits and patient reports of thermal comfort.
2. Deficient Fluid Volume related to fever, increased capillary permeability, and reduced oral intake, as evidenced by dry mucous membranes, decreased urine output (less than 30 mL/hour), and increased heart rate (110 bpm).
- Supporting Data: Dry oral mucosa, urine output 25 mL/hour for the past 2 hours, heart rate 110 bpm, patient reports nausea and difficulty drinking fluids.
- Desired Outcome: Patient will demonstrate adequate fluid volume balance, as evidenced by moist mucous membranes, urine output greater than 30 mL/hour, heart rate within normal limits (60-100 bpm), and stable blood pressure within 24-48 hours.
3. Acute Pain related to headache, muscle aches (myalgia), and joint pain (arthralgia) associated with dengue infection, as evidenced by patient report of pain rated 8/10 on a numerical pain scale, facial grimacing, and guarding behavior.
- Supporting Data: Patient rates pain 8/10, describes pain as “throbbing headache” and “aching muscles all over,” observed to be restless and avoiding movement.
- Desired Outcome: Patient will report a reduction in pain intensity to a manageable level (e.g., pain rating ≤ 3/10) within 1-2 hours after intervention, as evidenced by verbal reports of pain relief and decreased nonverbal pain cues.
4. Risk for Bleeding related to thrombocytopenia and increased capillary fragility secondary to dengue fever.
- Risk Factors: Platelet count 90,000/µL, positive tourniquet test, potential for mucosal damage from viral infection.
- Desired Outcome: Patient will remain free from signs of bleeding throughout hospitalization, as evidenced by absence of petechiae, ecchymosis, gingival bleeding, hematuria, hematemesis, and stable platelet counts within safe limits for dengue management.
5. Risk for Impaired Skin Integrity related to dengue rash and pruritus.
- Risk Factors: Presence of maculopapular rash covering trunk and limbs, patient reports intense itching, potential for scratching.
- Desired Outcome: Patient will maintain skin integrity, as evidenced by absence of skin breakdown, infection, and reports of reduced itching and effective management of pruritus throughout the illness.
6. Fatigue related to physiological effects of dengue infection (fever, pain, inflammatory response), as evidenced by patient report of overwhelming exhaustion, weakness, and inability to perform usual activities.
- Supporting Data: Patient states “I’m so tired I can barely lift my head,” observed to be lethargic and requiring assistance with basic activities of daily living.
- Desired Outcome: Patient will report improved energy levels and ability to perform activities of daily living within limitations of illness, as evidenced by increased participation in self-care and verbalization of feeling less fatigued by discharge.
7. Knowledge Deficit related to dengue fever disease process, transmission, management, and prevention, as evidenced by patient and family questions about dengue, lack of awareness of mosquito bite prevention strategies, and expressed uncertainty about home care.
- Supporting Data: Patient asks “How did I get dengue?”, family unsure about how to prevent mosquito bites at home, expresses concern about what to do after discharge.
- Desired Outcome: Patient and family will demonstrate understanding of dengue fever disease process, transmission, management, and prevention strategies prior to discharge, as evidenced by verbalization of key information and active participation in education sessions.
These nursing diagnoses provide a framework for planning and delivering patient-centered care, addressing the multifaceted needs of individuals with dengue fever.
Nursing Interventions and Rationales:
Nursing interventions for dengue fever are aimed at managing symptoms, preventing complications, and supporting the patient’s recovery. Rationales are provided to explain the scientific basis for each intervention.
For Hyperthermia:
- Monitor temperature regularly (every 2-4 hours and PRN).
- Rationale: Frequent monitoring allows for timely detection of fever spikes and evaluation of intervention effectiveness.
- Administer antipyretics as prescribed (e.g., paracetamol/acetaminophen). Avoid NSAIDs (e.g., ibuprofen, aspirin).
- Rationale: Paracetamol reduces fever by inhibiting prostaglandin synthesis in the central nervous system. NSAIDs are contraindicated due to their antiplatelet effects, which can increase bleeding risk in dengue.
- Apply tepid sponge baths.
- Rationale: Evaporative cooling from tepid water helps reduce body temperature through conduction and evaporation. Avoid cold water, which can cause shivering and increase metabolic rate, thus raising body temperature.
- Encourage light clothing and maintain a comfortable room temperature.
- Rationale: Light clothing facilitates heat loss through convection and radiation. A comfortable room temperature prevents overheating.
- Promote adequate fluid intake.
- Rationale: Fever increases metabolic rate and fluid loss through perspiration. Adequate hydration is essential to prevent dehydration and support thermoregulation.
For Deficient Fluid Volume:
- Monitor fluid intake and output accurately.
- Rationale: Precise measurement of intake and output helps assess fluid balance and guide fluid replacement therapy.
- Encourage oral rehydration with oral rehydration solutions (ORS) or clear fluids (water, juice, broth) if tolerated.
- Rationale: Oral rehydration is the preferred route for fluid replacement in mild to moderate dehydration. ORS provides balanced electrolytes.
- Administer intravenous fluids as prescribed (e.g., isotonic saline, Ringer’s lactate) for severe dehydration or inability to tolerate oral fluids.
- Rationale: IV fluids rapidly replenish fluid volume and electrolytes in cases of significant dehydration or when oral intake is insufficient. Isotonic solutions help restore intravascular volume.
- Assess for signs of dehydration (dry mucous membranes, poor skin turgor, decreased urine output, concentrated urine, hypotension, tachycardia).
- Rationale: Early recognition of dehydration allows for prompt intervention to prevent hypovolemic shock and organ damage.
- Monitor hematocrit and electrolyte levels.
- Rationale: Hematocrit can increase with dehydration due to hemoconcentration. Electrolyte imbalances can occur with fluid loss or replacement therapy.
For Acute Pain:
- Assess pain characteristics (location, intensity, quality, aggravating/relieving factors) regularly.
- Rationale: Comprehensive pain assessment guides individualized pain management strategies.
- Administer analgesics as prescribed (paracetamol is usually first-line).
- Rationale: Paracetamol provides pain relief by inhibiting prostaglandin synthesis.
- Encourage rest and promote comfort measures (e.g., positioning, gentle massage, cool compresses to forehead).
- Rationale: Rest reduces metabolic demands and can alleviate pain. Comfort measures enhance relaxation and pain tolerance.
- Provide distraction techniques (e.g., reading, listening to music, watching movies).
- Rationale: Distraction can divert attention away from pain and reduce pain perception.
For Risk for Bleeding:
- Monitor platelet count and coagulation studies regularly.
- Rationale: Serial monitoring of platelet count helps detect and manage thrombocytopenia progression. Coagulation studies assess clotting function in severe cases.
- Implement bleeding precautions:
- Avoid invasive procedures (IM injections, venipunctures if possible; use smallest gauge needle if necessary).
- Rationale: Minimizing invasive procedures reduces the risk of bleeding in thrombocytopenic patients.
- Use soft toothbrush and advise gentle oral hygiene.
- Rationale: Prevents gum trauma and bleeding.
- Avoid rectal temperatures and suppositories.
- Rationale: Prevents rectal mucosal trauma and bleeding.
- Apply pressure to venipuncture/injection sites for 5-10 minutes.
- Rationale: Prolonged pressure promotes hemostasis at puncture sites.
- Instruct patient to avoid forceful nose blowing and straining during bowel movements.
- Rationale: Reduces risk of mucosal bleeding.
- Avoid invasive procedures (IM injections, venipunctures if possible; use smallest gauge needle if necessary).
- Monitor for signs of bleeding (petechiae, ecchymosis, gingival bleeding, epistaxis, hematuria, melena, hematemesis).
- Rationale: Early detection of bleeding allows for prompt intervention, such as platelet transfusion if severe bleeding occurs or platelet count is critically low.
- Educate patient and family about bleeding precautions and to report any signs of bleeding immediately.
- Rationale: Patient and family involvement in bleeding precautions enhances safety and early detection of complications.
For Risk for Impaired Skin Integrity:
- Assess skin for rash characteristics and signs of breakdown regularly.
- Rationale: Early detection of skin changes allows for timely interventions to prevent complications.
- Encourage patient to avoid scratching.
- Rationale: Scratching can lead to skin excoriation, secondary infection, and delayed healing.
- Keep skin clean and dry.
- Rationale: Prevents secondary bacterial or fungal infections.
- Apply cool compresses or calamine lotion for pruritus relief, if prescribed.
- Rationale: Cool compresses and calamine lotion can soothe itching and provide symptomatic relief.
- Consider antihistamines if itching is severe, as prescribed.
- Rationale: Antihistamines can reduce pruritus by blocking histamine effects.
For Fatigue:
- Encourage rest periods and prioritize activities.
- Rationale: Rest reduces metabolic demands and conserves energy. Prioritizing activities helps manage fatigue effectively.
- Assist with activities of daily living (ADLs) as needed.
- Rationale: Reduces energy expenditure and supports patient comfort and hygiene.
- Provide a quiet and comfortable environment.
- Rationale: Promotes restful sleep and reduces sensory overload.
- Monitor patient’s response to activity and adjust activity levels accordingly.
- Rationale: Prevents overexertion and allows for individualized activity planning based on patient tolerance.
For Knowledge Deficit:
- Assess patient’s and family’s current understanding of dengue fever.
- Rationale: Identifies learning needs and guides educational content.
- Provide education on dengue fever:
- Disease process and transmission (mosquito bites).
- Rationale: Empowers patient to understand the illness and mode of transmission.
- Signs and symptoms of dengue fever and warning signs of severe dengue (severe abdominal pain, persistent vomiting, bleeding, lethargy/restlessness).
- Rationale: Enables early recognition of complications requiring immediate medical attention.
- Importance of mosquito bite prevention measures (using mosquito repellent, wearing long sleeves and pants, using mosquito nets, eliminating breeding sites).
- Rationale: Promotes preventive behaviors to reduce risk of future dengue infection and transmission to others.
- Medication regimen, symptom management, and follow-up care.
- Rationale: Ensures adherence to treatment plan and appropriate symptom management at home.
- Disease process and transmission (mosquito bites).
- Use various teaching methods (verbal explanation, written materials, visual aids).
- Rationale: Accommodates different learning styles and enhances comprehension.
- Encourage questions and provide clear, concise answers.
- Rationale: Facilitates active learning and addresses patient and family concerns.
- Evaluate learning through teach-back methods.
- Rationale: Confirms understanding of key information and identifies areas needing further clarification.
Nursing Goals:
- Patient will achieve and maintain normothermia (36.5°C-37.5°C / 97.7°F-99.5°F) throughout hospitalization.
- Patient will maintain adequate fluid volume, evidenced by stable vital signs, appropriate urine output, and moist mucous membranes.
- Patient will report pain reduced to a tolerable level (≤ 3/10 on pain scale) with effective pain management strategies.
- Patient will remain free from bleeding complications throughout hospitalization.
- Patient will maintain skin integrity without signs of breakdown or secondary infection.
- Patient will report reduced fatigue levels and participate in self-care activities as tolerated.
- Patient and family will verbalize understanding of dengue fever, its management, prevention strategies, and discharge instructions prior to discharge.
- Patient will demonstrate reduced anxiety related to dengue fever and hospitalization.
Evaluation and Expected Outcomes:
Patient outcomes are evaluated based on the achievement of the nursing goals set. Expected outcomes indicate the desired patient status following implementation of the nursing care plan.
- Temperature Regulation: Patient maintains normothermia (36.5°C-37.5°C / 97.7°F-99.5°F) consistently during hospital stay.
- Fluid Balance: Patient exhibits balanced fluid volume, evidenced by:
- Stable vital signs (BP and HR within normal limits for age).
- Adequate urine output (≥ 0.5 mL/kg/hour).
- Moist mucous membranes and good skin turgor.
- Hematocrit and electrolyte levels within normal limits.
- Pain Management: Patient reports pain is managed effectively, with pain scores consistently ≤ 3/10 on pain scale. Patient is able to rest comfortably and engage in minimal activities without significant pain exacerbation.
- Bleeding Prevention: Patient exhibits no signs of bleeding throughout hospitalization. Platelet counts are monitored and managed appropriately.
- Skin Integrity: Patient’s skin remains intact without signs of breakdown, infection, or excessive scratching. Dengue rash resolves without complications.
- Fatigue Management: Patient reports improved energy levels and is able to participate in self-care activities to the extent possible given illness severity. Patient verbalizes understanding of the need for continued rest and gradual activity increase during convalescence.
- Knowledge and Understanding: Patient and family accurately verbalize key information about dengue fever, its transmission, management, prevention, and discharge instructions. They demonstrate understanding of warning signs requiring medical attention and mosquito bite prevention strategies.
- Anxiety Reduction: Patient expresses reduced anxiety and demonstrates improved coping mechanisms related to dengue fever and hospitalization. Patient and family actively participate in care and ask appropriate questions.
Documentation:
Meticulous documentation is essential for effective nursing care. Document the following:
- Initial and ongoing nursing assessments, including vital signs, hydration status, pain assessments, bleeding risk assessments, skin condition, neurological status, and psychosocial status.
- Nursing diagnoses identified based on assessment data.
- Nursing interventions implemented, including medication administration, fluid therapy, comfort measures, bleeding precautions, skin care, patient education, and any consultations or referrals.
- Patient’s response to interventions, including changes in symptoms, vital signs, pain levels, bleeding signs, and overall condition.
- Patient and family education provided and their understanding of information.
- Evaluation of patient outcomes and progress towards goals.
- Any modifications to the care plan based on reassessment and patient needs.
- Communication with the interdisciplinary healthcare team and any collaborative care planning.
This nursing care plan is a dynamic guide that should be individualized and adapted based on the patient’s unique presentation, disease progression, and response to treatment. Continuous assessment, evaluation, and interdisciplinary collaboration are crucial for providing optimal care to patients with dengue fever.
Note: This nursing care plan is intended as a general guideline and should be adapted to meet the specific needs of individual patients and according to institutional protocols and healthcare provider orders. It is crucial to consult with the healthcare team and modify the care plan as necessary based on the patient’s condition and evolving clinical situation.