As experts in automotive repair at xentrydiagnosis.store, understanding diagnostic processes is crucial. While our primary focus is vehicles, the principles of differential diagnosis are universal. This article delves into the differential diagnosis of testicular masses, a critical area in men’s health, drawing parallels to the systematic approach we use in automotive troubleshooting. Just as we differentiate between engine problems and transmission issues, medical professionals must distinguish between various causes of testicular masses. This guide aims to provide a comprehensive overview for better understanding and awareness.
Understanding Scrotal Lumps and Testicular Masses
A scrotal lump refers to any abnormal mass or swelling within the scrotum. These can originate from the testicles themselves (testicular) or from surrounding structures (extra-testicular). It’s vital to recognize that while many scrotal lumps are benign, some, particularly those originating from the testis, can be malignant, most notably testicular cancer. Therefore, prompt and accurate differential diagnosis is paramount.
Clinical Assessment: Key to Initial Differential Diagnosis
Similar to a vehicle inspection, the initial diagnosis of a testicular mass heavily relies on a thorough clinical examination. This involves taking a detailed patient history, focusing on the onset, duration, pain level, and any associated symptoms. Crucially, a physical examination using inspection and palpation provides vital clues.
Inspection: Employ the “6 S’s” framework – Site, Size, Shape, Symmetry, Skin changes, and Scars – to systematically document visual characteristics of the scrotal lump.
Palpation: Utilizing the acronym CAMPFIRE – Consistency, Attachments, Mobility, Pulsation, Fluctuation, Irreducibility, Regional lymph nodes, and Edge, alongside Tenderness and Temperature, allows for a structured assessment of the mass’s physical properties. Specifically within the scrotum, it’s essential to meticulously identify and palpate the testis, epididymis, and vas deferens separately to pinpoint the origin of the mass.
Investigations: Ultrasound as First-Line for Testicular Mass Differential Diagnosis
In most cases of scrotal lumps, and especially when a testicular origin is suspected, an ultrasound scan of the scrotum is the primary investigative tool. This is akin to using diagnostic tools in automotive repair to pinpoint the source of a problem. Depending on the ultrasound findings and the suspected underlying cause, further investigations like blood tests or advanced imaging may be necessary.
Investigating Suspected Testicular Cancer: A Critical Aspect of Testicular Mass Differential Diagnosis
Any mass directly arising from the testis necessitates urgent ultrasound evaluation to rule out testicular cancer. Unlike many other cancers, biopsy is contraindicated in suspected testicular cancer due to the risk of tumor seeding. Diagnosis is based on clinical findings, ultrasound imaging, and histopathological examination after orchidectomy (surgical removal of the testis).
When testicular cancer is a concern, blood tests for tumor markers, including lactate dehydrogenase (LDH), alpha-fetoprotein (AFP), and beta-human chorionic gonadotrophin (beta-hCG), are crucial for diagnosis, staging, and monitoring treatment response.
Differential Diagnoses of Testicular Masses: Testicular vs. Extra-testicular
Scrotal lumps can be broadly categorized as either testicular or extra-testicular in origin, which forms the foundation of the differential diagnosis. Understanding this distinction is crucial for accurate diagnosis and management.
Figure 2 – Schematic representation of the differential diagnoses for scrotal lumps, highlighting testicular and extra-testicular origins, essential for diagnosis.Extra-testicular Causes Mimicking Testicular Masses
While focusing on testicular masses, it’s important to consider extra-testicular conditions that can present as scrotal lumps and need to be differentiated.
Hydrocele: Fluid Accumulation Around the Testis
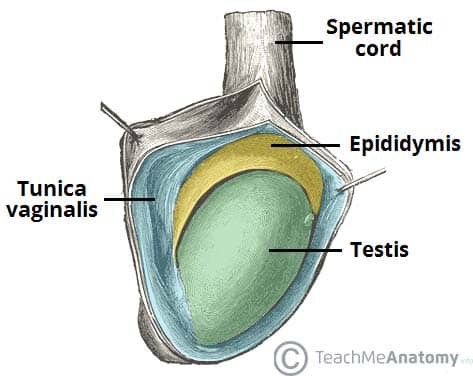
A hydrocele is an abnormal collection of serous fluid within the tunica vaginalis, the sac surrounding the testis. It typically manifests as a painless, fluctuant swelling that transilluminates readily. Hydroceles can be unilateral or bilateral and may enlarge to cause discomfort. In infants, congenital hydroceles are common and often resolve spontaneously. In adults, they can be primary (idiopathic) or secondary to trauma, infection, or malignancy. Urgent ultrasound is recommended for hydroceles in men aged 20-40 or when the testis cannot be palpated.
Varicocele: Dilated Veins in the Spermatic Cord
A varicocele is characterized by the abnormal dilation of the pampiniform venous plexus within the spermatic cord. Clinically, it feels like a “bag of worms” and may cause a dragging sensation. Varicoceles often diminish when lying down. They are more common on the left side and can contribute to infertility. Red flag signs include acute onset, right-sided presentation, or persistence when supine, requiring urgent investigation.
Figure 4 – Ultrasound with and without Doppler showing a varicocele, demonstrating venous dilation.Epididymal Cysts (Spermatoceles): Benign Fluid-Filled Sacs
Epididymal cysts, or spermatoceles, are benign, fluid-filled sacs originating from the epididymis. They present as smooth, fluctuant nodules, separate from the testis, and transilluminate. Common in middle-aged men, they are typically asymptomatic and require no treatment unless large or painful.
Epididymitis: Inflammation of the Epididymis
Epididymitis is inflammation of the epididymis, often causing acute scrotal pain, swelling, and tenderness. It’s frequently bacterial in origin, either sexually transmitted infections in younger men or enteric bacteria in older men. Pain relief upon testicular elevation (Prehn’s sign) may be present.
Inguinal Hernia Extending into the Scrotum
An inguinal hernia can descend into the scrotum, running alongside the spermatic cord. Crucially, you cannot “get above” an inguinal hernia on examination. Coughing may exacerbate the swelling, and it may reduce when lying down.
Testicular Causes of Testicular Masses: Primary Concerns
Now focusing on masses originating directly from the testis, the differential diagnosis becomes critical, particularly in ruling out malignancy.
Testicular Tumors: The Primary Malignancy to Exclude
Testicular tumors, predominantly cancerous, are a primary concern when evaluating a testicular mass. They are often painless, firm, and irregular masses within the testis that do not transilluminate. Testicular cancer is the most common malignancy in men aged 20-40. Urgent ultrasound and tumor markers are essential for diagnosis. Radical inguinal orchidectomy is often necessary, followed by chemotherapy in many cases, with high survival rates depending on tumor stage and grade.
Testicular Torsion: A Surgical Emergency
Testicular torsion involves the twisting of the testis on the spermatic cord, leading to ischemia and sudden, severe scrotal pain, often with nausea and vomiting. It’s a surgical emergency requiring immediate scrotal exploration and fixation of both testes to prevent irreversible damage. Time is critical, as salvage rates decrease significantly after 6 hours of symptom onset.
Benign Testicular Lesions: Less Common Causes
Benign testicular lesions, though less frequent, include Leydig cell tumors, Sertoli cell tumors, lipomas, and fibromas. These are typically diagnosed after excluding malignancy.
Orchitis: Inflammation of the Testis
Orchitis, inflammation of the testis, is rare in isolation and most commonly caused by the mumps virus. It often presents with testicular pain and swelling, sometimes following parotid swelling. Treatment is usually conservative with rest and analgesia.
Key Points for Differential Diagnosis of Testicular Masses
- A scrotal lump, especially a testicular mass, requires a systematic approach to differential diagnosis to rule out serious conditions like testicular cancer and testicular torsion.
- Ultrasound of the scrotum is the first-line investigation for most scrotal lumps and is crucial in differentiating testicular from extra-testicular masses and identifying specific pathologies.
- Clinical examination, combined with ultrasound and tumor markers when indicated, is essential for accurate diagnosis and timely management.
- Always consider testicular cancer in the differential diagnosis of any testicular mass, particularly in men aged 20-40.
This guide provides a framework for understanding the differential diagnosis of testicular masses. Just as in automotive repair, a systematic and thorough approach, utilizing the right tools (clinical examination and investigations), is key to accurate diagnosis and effective management in the medical field.