The QRS complex is a crucial component of an electrocardiogram (ECG), representing ventricular depolarization – the electrical activation of the heart’s ventricles. Analyzing the QRS complex morphology is fundamental in ECG interpretation, providing valuable insights into the heart’s electrical conduction system and overall cardiac health. While the original article provided a solid foundation on general QRS complex morphology, this article will delve deeper into a specific and clinically significant aspect: the inverted QRS complex, often manifested as pathological Q waves. Understanding inverted QRS complexes is vital for accurate diagnosis, particularly in identifying myocardial infarction and other cardiac abnormalities.
Understanding the Normal QRS Complex
Before discussing inverted QRS complexes, it’s essential to recap the normal QRS complex. As previously mentioned, it reflects ventricular depolarization. Typically, it is a predominantly positive deflection in most leads, reflecting the general direction of ventricular depolarization moving towards the positive electrode. The duration, amplitude, and morphology of the QRS complex are all critical parameters assessed in ECG analysis.
Normal QRS Complex Nomenclature. Illustrating the typical positive deflection of the QRS complex in standard ECG readings.
QRS Width and its Significance
The width of the QRS complex, normally ranging from 70-100 ms, is a primary feature to consider.
- Narrow QRS complexes (less than 100 ms) usually indicate a supraventricular origin of the electrical impulse, meaning the impulse originates above the ventricles (in the atria or AV node).
- Broad QRS complexes (greater than 100 ms) suggest either a ventricular origin or aberrant conduction of a supraventricular impulse. This could be due to conditions like bundle branch blocks, hyperkalemia, or sodium-channel blockade.
Inverted QRS Complexes: Focusing on Pathological Q Waves
An inverted QRS complex, in the context of diagnostic significance, often refers to the presence of Q waves, specifically when they are deemed pathological. While small, narrow q waves are normal in certain leads, pathological Q waves are abnormal negative deflections that can indicate significant cardiac pathology, most notably myocardial infarction (heart attack).
Physiological vs. Pathological Q Waves
It’s crucial to differentiate between physiological and pathological Q waves.
- Physiological q waves: These are small, narrow q waves (lowercase ‘q’) that are normal variants. They are typically seen in leads I, aVL, V5, and V6, representing septal depolarization from left to right. They are narrow (less than 40 ms in duration) and small in amplitude (less than 25% of the R wave amplitude).
- Pathological Q waves: These are significant Q waves (uppercase ‘Q’) that are wider (≥ 40 ms or 1 mm in width) and deeper (at least 1/3 the height of the R wave or > 1 mm deep). They indicate myocardial necrosis, often from a previous myocardial infarction.
Criteria for Pathological Q Waves
The following criteria help define pathological Q waves:
- Width: ≥ 0.04 seconds (40 milliseconds or one small square on standard ECG paper).
- Depth: At least one-third the height of the R wave in the same QRS complex, OR > 1 mm deep, OR present in more than two contiguous leads.
- Leads: Present in leads where physiological q waves are not expected (e.g., leads II, III, aVF, V1-V4). Q waves in V1-V3 are particularly concerning for anterior myocardial infarction.
Clinical Significance of Pathological Q Waves
The primary clinical significance of pathological Q waves is the indication of myocardial infarction. They represent the electrical silence of necrotic myocardial tissue. When myocardial cells die due to ischemia (lack of blood supply), they become electrically inactive and unable to depolarize. As a result, the ECG records the electrical activity moving away from the infarcted area, resulting in a negative deflection – the pathological Q wave.
Pathological Q waves are generally considered permanent markers of myocardial infarction. They may develop within hours to days after the onset of infarction and usually persist indefinitely.
Location of Infarction Based on Q Wave Leads
The location of pathological Q waves can help localize the area of myocardial infarction:
- Anterior MI: Q waves in leads V1-V4.
- Inferior MI: Q waves in leads II, III, and aVF.
- Lateral MI: Q waves in leads I, aVL, V5, and V6.
- Septal MI: Q waves in leads V1 and V2 (though less specific and can be due to other causes).
It is important to note that the absence of Q waves does not rule out myocardial infarction, especially in non-ST-elevation myocardial infarction (NSTEMI) or early stages of STEMI. Furthermore, not all Q waves are pathological; hence, careful assessment of their morphology and clinical context is essential.
Differential Diagnosis of Pathological Q Waves
While myocardial infarction is the most common and clinically significant cause of pathological Q waves, other conditions can also cause them:
- Cardiomyopathies: Hypertrophic cardiomyopathy and dilated cardiomyopathy can sometimes present with Q waves.
- Myocarditis: Inflammation of the heart muscle can, in some cases, cause Q waves.
- Pulmonary Embolism: Massive pulmonary embolism can occasionally cause Q waves in inferior leads.
- Left Ventricular Hypertrophy: Severe LVH can sometimes mimic Q waves in lateral leads.
- Wolff-Parkinson-White (WPW) Syndrome: The delta wave in WPW syndrome can sometimes resemble Q waves.
- Normal Variants: In rare cases, Q waves that meet pathological criteria may be normal variants, especially in young, healthy individuals. Clinical correlation is crucial.
Diagnostic Approach to Inverted QRS Complexes (Pathological Q Waves)
When encountering inverted QRS complexes that meet the criteria for pathological Q waves, a systematic diagnostic approach is necessary:
- Clinical Correlation: Always correlate ECG findings with the patient’s clinical presentation, history, and risk factors for coronary artery disease. Chest pain, shortness of breath, and other symptoms of myocardial ischemia should raise suspicion for infarction.
- Serial ECGs: Obtain serial ECGs to assess for dynamic changes, particularly ST-segment elevation or depression, and evolution of Q waves over time. In acute MI, Q waves may not be immediately present but develop over hours.
- Cardiac Biomarkers: Measure cardiac biomarkers, such as troponin, to confirm myocardial necrosis. Elevated troponin levels in conjunction with pathological Q waves strongly support the diagnosis of myocardial infarction.
- Echocardiography: Echocardiography can assess regional wall motion abnormalities, which can further support the diagnosis of MI and assess left ventricular function.
- Coronary Angiography: In patients with suspected myocardial infarction, coronary angiography may be indicated to visualize coronary arteries and identify any blockages.
Conclusion
Inverted QRS complexes, specifically pathological Q waves, are significant ECG findings that often indicate myocardial infarction. Understanding the criteria for pathological Q waves, their clinical significance, and differential diagnoses is crucial for accurate ECG interpretation and timely management of cardiac conditions. While the presence of pathological Q waves is a valuable diagnostic clue, it should always be interpreted in the context of the patient’s clinical presentation and other diagnostic investigations. This comprehensive understanding is paramount for healthcare professionals involved in cardiac care and for anyone seeking to deepen their knowledge of ECG interpretation.
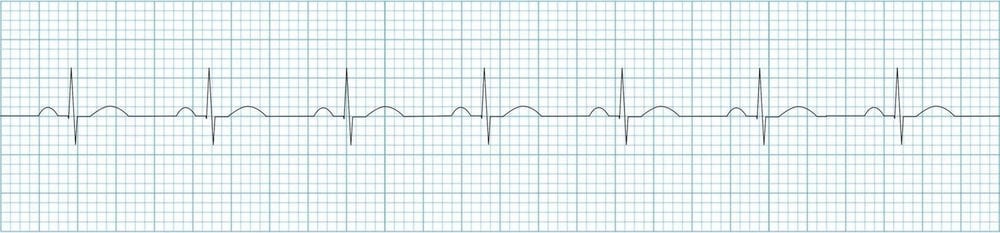 ECG Normal sinus rhythm strip
ECG Normal sinus rhythm strip
Example of a normal sinus rhythm ECG, contrasting with ECGs exhibiting pathological Q waves, to highlight the difference in QRS complex morphology.