Nursing care plans (NCPs) are essential tools in healthcare, serving as a roadmap for nurses to deliver patient-centered care. Creating an effective nursing care plan involves a systematic approach, and a crucial element in this process is the use of standardized nursing language, particularly NANDA-I diagnoses. This guide will walk you through the process of developing a robust nursing care plan incorporating NANDA diagnoses, ensuring you’re equipped to provide the best possible care.
What is a Nursing Care Plan with NANDA Diagnosis?
A nursing care plan (NCP) is a formal, written or electronic document that outlines the individualized care for a patient. It’s a dynamic tool that identifies a patient’s current health status, potential problems, and sets out a plan of action to achieve specific health outcomes. Integrating NANDA-I (North American Nursing Diagnosis Association International) diagnoses into a nursing care plan provides a standardized framework for identifying, classifying, and addressing patient needs.
NANDA-I diagnoses are clinically judged human experiences/responses to health conditions and life processes. Using NANDA-I in care plans ensures clear communication among healthcare professionals, promotes evidence-based practice, and provides a consistent approach to patient care. Without a well-structured care planning process that includes standardized diagnoses like NANDA, the quality and consistency of patient care can be compromised.
Nursing care planning, especially with NANDA diagnoses, is not a static process. It begins upon patient admission and is continuously revised based on the patient’s changing condition and the evaluation of goal achievement. This dynamic, patient-centered approach is the foundation of excellent nursing practice.
Types of Nursing Care Plans Incorporating NANDA Diagnoses
Similar to general care plans, NCPs using NANDA diagnoses can be categorized as informal or formal, and further subdivided into standardized and individualized plans:
- Informal Nursing Care Plan: A mental strategy, existing in the nurse’s mind, for immediate actions. While quick, it lacks the depth and formal structure for comprehensive care and consistent communication.
- Formal Nursing Care Plan: A documented, written or computerized guide that organizes patient care information. Formal plans are essential for ensuring continuity of care and clear communication across the healthcare team.
Formal care plans are further broken down into:
- Standardized Care Plans with NANDA Diagnoses: Pre-developed guides specifying nursing care for patient groups with common needs, using standardized NANDA-I diagnoses. These plans ensure consistent care for typical conditions and improve efficiency by providing a starting point for common interventions. However, they need to be individualized to address specific patient needs.
- Individualized Care Plans with NANDA Diagnoses: Tailored plans that adapt standardized NANDA-I diagnoses and interventions to meet a specific patient’s unique needs, preferences, and goals. This approach ensures personalized and holistic care, recognizing the patient as an individual.
Standardized Care Plans and NANDA-I
Standardized care plans, enhanced with NANDA-I diagnoses, are valuable tools for ensuring a baseline level of quality care. They provide a framework for addressing common patient problems efficiently. However, it’s crucial to remember that these are starting points. Nurses must critically assess each patient and individualize the plan.
The care plans discussed in this guide utilize NANDA-I diagnoses as a foundation, providing a structured approach to develop individualized care plans.
Individualized Care Plans and NANDA-I
Individualized care plans, built upon NANDA-I diagnoses, are the gold standard for patient care. They involve selecting relevant NANDA-I diagnoses and then customizing the related goals, interventions, and evaluation criteria to the specific patient. This personalization is key to holistic care and improving patient satisfaction. When patients perceive their care as tailored to their unique circumstances, they are more likely to be engaged in their care and report higher satisfaction.
Tips to individualize a nursing care plan using NANDA diagnoses:
- Comprehensive Assessment: Conduct a thorough patient assessment to identify specific needs and responses that might not be covered in a standardized plan.
- Patient Involvement: Actively involve the patient and their family in the planning process. Their input is crucial for understanding their unique needs, values, and preferences.
- Customize NANDA Components: While using NANDA-I diagnoses as a starting point, tailor the defining characteristics, related factors, goals, and interventions to the individual patient.
- Consider Patient Strengths: Focus not only on problems but also on patient strengths and resources that can be utilized in the care plan.
- Regular Review and Revision: Continuously evaluate the effectiveness of the plan and revise it based on the patient’s progress and changing needs.
Objectives of Nursing Care Plans with NANDA Diagnosis
The objectives of writing nursing care plans incorporating NANDA diagnoses are multifaceted:
- Promote Standardized, Evidence-Based Care: NANDA-I provides a common language for nurses, promoting consistency and allowing for the implementation of evidence-based interventions associated with specific diagnoses.
- Support Holistic and Patient-Centered Care: By using NANDA-I diagnoses to identify patient responses across physical, psychological, social, and spiritual dimensions, care plans can be designed to address the whole person.
- Establish Care Pathways and Bundles: NANDA diagnoses can be used to develop standardized care pathways for specific patient populations or conditions, ensuring consistent and best-practice care delivery.
- Clearly Define Goals and Expected Outcomes: NANDA diagnoses help in formulating specific, measurable, achievable, relevant, and time-bound (SMART) goals and outcomes that are directly linked to the identified patient needs.
- Enhance Communication and Documentation: Using standardized NANDA-I language improves clarity and precision in care plan documentation, facilitating effective communication among the healthcare team.
- Measure and Evaluate Nursing Care Effectiveness: Clearly defined goals and outcomes linked to NANDA diagnoses provide a framework for evaluating the effectiveness of nursing interventions and making necessary adjustments to the care plan.
Purposes of Nursing Care Plans with NANDA Diagnosis
Nursing care plans with NANDA diagnoses serve several critical purposes in patient care:
- Define the Nurse’s Role: Care plans highlight the unique and independent role of nurses in addressing patients’ health and well-being. NANDA diagnoses empower nurses to articulate their professional judgments and contributions to patient care.
- Provide Direction for Individualized Care: They serve as a detailed guide for delivering personalized care, ensuring that interventions are tailored to the patient’s specific NANDA-I diagnoses and needs.
- Ensure Continuity of Care: Standardized NANDA language facilitates seamless transitions and consistent care across different shifts, departments, and healthcare settings.
- Coordinate Care Among Healthcare Team Members: Care plans with NANDA diagnoses ensure that all members of the healthcare team understand the patient’s nursing diagnoses, goals, and planned interventions, fostering collaboration and preventing gaps in care.
- Documentation and Legal Record: Care plans document the nursing process, including assessment, diagnosis (using NANDA-I), planning, implementation, and evaluation. Accurate documentation is essential for legal and professional accountability.
- Guide Staff Assignment: Care plans can help in assigning nurses with specific expertise to patients with complex needs based on their NANDA diagnoses.
- Monitor Patient Progress: Care plans facilitate the tracking of patient progress toward achieving goals related to their NANDA diagnoses, allowing for timely adjustments to the care plan.
- Support Reimbursement: Insurers often review medical records, including care plans, to determine coverage. Well-documented care plans with clear NANDA diagnoses and interventions can support reimbursement claims.
- Define Patient Goals and Promote Engagement: Involving patients in the care planning process, including discussing their NANDA diagnoses and related goals, promotes patient engagement and shared decision-making.
Components of a Nursing Care Plan with NANDA Diagnosis
A comprehensive nursing care plan incorporating NANDA diagnoses typically includes the following components:
- Nursing Diagnoses (NANDA-I): These are the core of the care plan, identifying the patient’s health problems or risks using standardized NANDA-I terminology.
- Defining Characteristics: The assessment findings (signs and symptoms) that provide evidence for the selected NANDA diagnosis.
- Related Factors/Risk Factors: The factors contributing to or causing the nursing diagnosis. For risk diagnoses, these are the factors that increase the patient’s vulnerability.
- Goals and Desired Outcomes: Measurable, patient-centered statements describing the expected changes in the patient’s health status as a result of nursing care. These should directly address the NANDA diagnosis.
- Nursing Interventions: Specific actions that nurses will implement to achieve the patient’s goals and address the NANDA diagnosis. Interventions should be evidence-based and tailored to the individual patient.
- Rationales: The scientific principles or evidence that support the chosen nursing interventions. These explain why specific interventions are expected to be effective for the identified NANDA diagnosis.
- Evaluation: A method for assessing the patient’s progress toward achieving the stated goals and the effectiveness of the nursing care plan. Evaluation is ongoing and leads to revisions of the care plan as needed.
Care Plan Formats with NANDA Diagnosis
Nursing care plans with NANDA diagnoses can be organized in various formats. The most common are three-column and four-column formats:
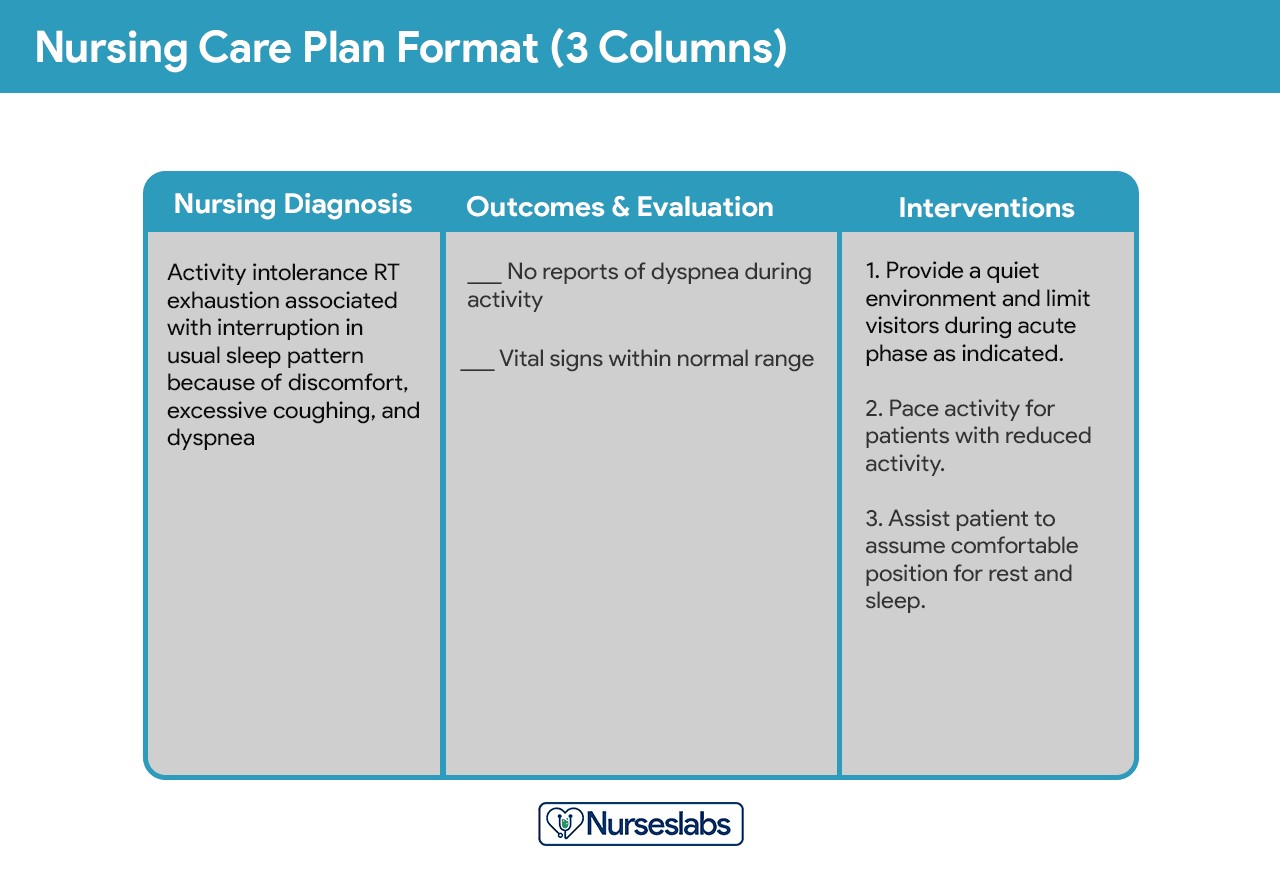
Three-Column Format (NANDA-I NCP)
This format typically includes:
- NANDA Nursing Diagnosis: The identified NANDA-I diagnosis.
- Outcomes and Evaluation Criteria: Patient-centered goals and measurable criteria to evaluate goal achievement.
- Nursing Interventions: Actions to be taken by the nurse, often implied to be related to the NANDA diagnosis and outcomes.
Example of a three-column nursing care plan format, designed for clarity and ease of use.
Four-Column Format (Comprehensive NANDA-I NCP)
This more detailed format includes:
- NANDA Nursing Diagnosis: The identified NANDA-I diagnosis, including related factors and defining characteristics.
- Goals and Desired Outcomes: SMART goals and expected outcomes that are patient-centered and measurable.
- Nursing Interventions: Specific, detailed actions to be taken by the nurse to address the NANDA diagnosis and achieve the goals.
- Evaluation: Methods and criteria for evaluating the effectiveness of interventions and the patient’s progress towards goals.
A four-column nursing care plan template, providing a structured approach for detailed and comprehensive care planning.
Downloadable Templates:
For your convenience, sample templates for different NANDA nursing care plan formats are available for download:
Download: Printable Nursing Care Plan Templates and Formats
Student Care Plans and NANDA Diagnosis
Student care plans often require a more detailed approach to facilitate learning. When using NANDA diagnoses in student care plans, it’s common to include an additional column for “Rationales” or “Scientific Explanation.” This column helps students connect the chosen nursing interventions to the underlying scientific principles and the specific NANDA diagnosis. Student care plans are valuable learning tools for mastering the nursing process and the application of NANDA-I.
Student nursing care plans are designed to be more detailed, enhancing the learning process and critical thinking skills.
Writing a Nursing Care Plan with NANDA Diagnosis: Step-by-Step
Developing a nursing care plan with NANDA diagnoses involves a systematic process, following the steps of the nursing process:
Step 1: Assessment and Data Collection
The first step is to gather comprehensive patient data. Use various assessment techniques, including:
- Physical Assessment: Head-to-toe examination to identify physical signs and symptoms.
- Health History: Gathering information about past medical conditions, surgeries, medications, allergies, and psychosocial history.
- Patient Interview: Directly communicating with the patient to understand their perspective, concerns, and health goals.
- Medical Records Review: Examining existing medical documentation for relevant information.
- Diagnostic Studies: Reviewing laboratory results, imaging reports, and other diagnostic findings.
The goal is to create a complete patient database, identifying relevant health information, including defining characteristics and potential related or risk factors that will be used to formulate NANDA nursing diagnoses.
Critical thinking is paramount during assessment. Integrate knowledge from various sciences and professional guidelines to inform your evaluation. This process, essential for complex clinical decision-making, aims to effectively identify patients’ healthcare needs within a supportive and informative environment.
Step 2: Data Analysis and Organization
Once data is collected, analyze and organize it to identify patterns and clusters of cues. Group related data to identify potential health problems and patient responses. This step sets the stage for selecting appropriate NANDA nursing diagnoses.
Step 3: Formulating NANDA Nursing Diagnoses
This crucial step involves selecting the most appropriate NANDA-I diagnoses that accurately represent the patient’s health problems or risks. Refer to a NANDA-I handbook or resource to select diagnoses based on the identified defining characteristics and related/risk factors from your assessment data.
Key Considerations for NANDA Diagnosis Formulation:
- Diagnostic Accuracy: Ensure the selected NANDA diagnosis accurately reflects the patient’s condition.
- Use of NANDA-I Terminology: Phrase the diagnosis using the standardized NANDA-I terminology.
- “Related to” Statement: For actual diagnoses, link the diagnosis to related factors (etiology) using “related to” (R/T).
- “As evidenced by” Statement: Support the diagnosis with defining characteristics from your assessment data using “as evidenced by” (AEB).
- Risk Diagnoses: For risk diagnoses, identify risk factors using “as evidenced by” risk factors.
For a detailed guide on formulating nursing diagnoses, refer to: Nursing Diagnosis (NDx): Complete Guide and List.
Step 4: Setting Priorities
Prioritize the NANDA nursing diagnoses based on their urgency and potential impact on the patient’s well-being. Use frameworks like Maslow’s Hierarchy of Needs to guide prioritization. Physiological needs (like airway, breathing, circulation) typically take precedence over safety, love/belonging, esteem, and self-actualization needs.
Maslow’s Hierarchy of Needs and NANDA Diagnosis Prioritization:
- Physiological Needs (Highest Priority): Diagnoses related to basic survival needs (e.g., Ineffective Airway Clearance, Deficient Fluid Volume).
- Safety and Security Needs: Diagnoses related to safety and security (e.g., Risk for Falls, Risk for Infection).
- Love and Belonging Needs: Diagnoses related to social interaction and belonging (e.g., Social Isolation).
- Self-Esteem Needs: Diagnoses related to self-worth and confidence (e.g., Disturbed Body Image).
- Self-Actualization Needs (Lowest Priority): Diagnoses related to personal growth and fulfillment (often less directly addressed in acute care settings).
Abraham Maslow’s hierarchy emphasizes meeting basic physiological needs before addressing higher-level needs. This framework is crucial for prioritizing nursing care and interventions based on patient-centered outcomes.
Virginia Henderson’s 14 Needs applied to Maslow’s Hierarchy, illustrating the interconnectedness of basic needs and holistic patient care. Learn more about it here.
Consider patient values, beliefs, available resources, and the urgency of the problem when setting priorities. Involve the patient in this process to foster collaboration and adherence to the care plan.
Step 5: Establishing Patient Goals and Desired Outcomes
For each prioritized NANDA nursing diagnosis, develop patient-centered goals and desired outcomes. Goals describe the desired change in patient health status, directly addressing the NANDA diagnosis. Outcomes are specific, measurable criteria that indicate goal achievement.
SMART Goal Framework:
- Specific: Clearly defined and focused.
- Measurable: Quantifiable and observable.
- Attainable: Realistic and achievable for the patient.
- Relevant: Meaningful and important to the patient’s needs.
- Time-bound: With a specific timeframe for achievement.
Examples of well-written goals and desired outcomes, demonstrating the SMART criteria for effective care planning.
REEPIG Standards for High-Quality Goals:
- Realistic: Achievable with available resources.
- Explicitly Stated: Clear and unambiguous.
- Evidence-Based: Supported by research or best practices.
- Prioritized: Addressing the most urgent needs first.
- Involve Patient: Collaboratively developed with the patient.
- Goal-Centered: Directly related to the NANDA diagnosis and desired outcomes.
Goals can be short-term (achievable within hours to days) or long-term (achievable over weeks to months), depending on the care setting and patient condition.
Components of Goal Statements:
- Subject: The patient (often implied).
- Verb: Action the patient will perform (e.g., “will demonstrate,” “will verbalize,” “will maintain”).
- Conditions/Modifiers: Circumstances under which the behavior will be performed (e.g., “within 24 hours,” “before discharge”).
- Criterion of Performance: Standard for evaluating performance (e.g., “pain level less than 3 on a scale of 0-10”).
Tips for Writing Effective Goals:
- Focus on patient responses, not nurse activities. Start with “Patient will…”
- Focus on what the patient will do, not what the nurse hopes to achieve.
- Use observable and measurable terms. Avoid vague language.
- Ensure goals are realistic for the patient’s situation and resources.
- Ensure compatibility with other therapies.
- Each goal should be derived from only one NANDA diagnosis for clear evaluation.
- Involve the patient in goal setting to ensure value and cooperation.
Step 6: Selecting Nursing Interventions
Nursing interventions are specific actions nurses will take to achieve patient goals and address the NANDA nursing diagnoses. Interventions should be aimed at reducing or eliminating the etiology (related factors) of the diagnosis.
Types of Nursing Interventions:
- Independent Interventions: Actions nurses are licensed to initiate based on their own judgment and skills (e.g., patient education, emotional support, positioning).
- Dependent Interventions: Actions requiring a physician’s order (e.g., medication administration, wound care treatments).
- Collaborative Interventions: Actions implemented in conjunction with other healthcare team members (e.g., physical therapy, dietary consults).
Different types of nursing interventions, highlighting the scope of nursing actions in patient care.
Criteria for Selecting Interventions:
- Safe and Appropriate: For patient’s age, health condition, and diagnosis.
- Achievable: With available resources and time.
- Congruent with Patient Values: Respecting culture, beliefs, and preferences.
- Compatible with Other Therapies: Coordinated with the overall treatment plan.
- Evidence-Based: Supported by nursing knowledge, research, or best practices.
Tips for Writing Nursing Interventions:
- Date and sign the care plan to indicate accountability.
- Be specific and clear, starting with an action verb (e.g., “Assess,” “Administer,” “Educate,” “Monitor”).
- Include qualifiers (how, when, where, frequency, amount) for clarity.
- Use only approved abbreviations within your institution.
Step 7: Providing Rationales (for Student NCPs)
Rationales are scientific explanations for why each nursing intervention is selected. They connect the intervention to the NANDA diagnosis and desired outcome, demonstrating the student’s understanding of the underlying principles. Rationales are typically required in student care plans to enhance learning.
Example of nursing interventions paired with rationales, illustrating the scientific basis for nursing actions in a care plan.
Step 8: Evaluation
Evaluation is the ongoing process of assessing the patient’s progress toward achieving goals and the effectiveness of the nursing care plan. It involves:
- Data Collection: Gathering data to determine if desired outcomes have been met.
- Outcome Comparison: Comparing patient data to the established outcome criteria.
- Judgment: Determining the extent to which goals have been achieved (met, partially met, not met).
- Care Plan Modification: Revising the care plan based on the evaluation findings. Interventions may need to be continued, adjusted, or discontinued.
Evaluation is a continuous cycle, ensuring the care plan remains relevant and effective throughout the patient’s care.
Step 9: Documentation
Document the completed nursing care plan, including NANDA diagnoses, goals, interventions, and evaluation findings, according to institutional policy. The care plan becomes part of the patient’s permanent medical record.
Nursing Care Plan Examples Using NANDA Diagnoses
The following sections provide lists of nursing care plans categorized by various health conditions and specialties. These examples can serve as a starting point for developing your own Nanda Diagnosis Nursing Care Plans.
(The extensive list of Nursing Care Plan examples from the original article follows here, categorized as in the original, but without repeating the full lists for brevity in this rewritten example. In a full rewrite, these lists would be included.)
Recommended Resources for NANDA Diagnosis and Nursing Care Plans
(The list of recommended books from the original article follows here, as it provides valuable resources.)
Disclosure: Included below are affiliate links from Amazon at no additional cost from you. We may earn a small commission from your purchase. For more information, check out our privacy policy.
Ackley and Ladwig’s Nursing Diagnosis Handbook: An Evidence-Based Guide to Planning Care
Nursing Care Plans – Nursing Diagnosis & Intervention (10th Edition)
Nurse’s Pocket Guide: Diagnoses, Prioritized Interventions, and Rationales
Nursing Diagnosis Manual: Planning, Individualizing, and Documenting Client Care
References and Sources
(The original reference and social sharing links follow here.)