Introduction
Cryptorchidism, commonly known as undescended testes, is a prevalent congenital condition in male infants where one or both testicles fail to descend into the scrotum before birth. Instead, the testicle(s) may remain in the abdomen or along the inguinal canal. While spontaneous descent can occur within the first few months of life, medical intervention is often necessary to ensure proper testicular development and function. Early detection and management are crucial to mitigate potential complications and promote long-term reproductive health. This article provides a comprehensive overview of cryptorchidism, with a specific focus on NANDA nursing diagnosis care plans designed to guide nurses in providing optimal care for infants and children with this condition and their families.
Understanding Cryptorchidism
What is Cryptorchidism?
Cryptorchidism, derived from the Greek words “kryptos” (hidden) and “orchis” (testis), is the most common abnormality of male sexual development. Typically, the testes descend from the abdominal cavity into the scrotum shortly before or after birth. Cryptorchidism occurs when this natural descent is interrupted, leaving one or both testes undescended. This condition was first documented in 1786 by British anatomist Sir John Hunter, and the first successful orchidopexy, a surgical correction, was performed in 1877 by Annandale.
Pathophysiology
The exact pathophysiology of cryptorchidism is multifactorial and not fully understood, but several theories exist. These include:
- Gubernacular Abnormalities: The gubernaculum testis is a crucial structure that guides testicular descent by attaching the testis to the scrotum and widening the inguinal canal. Anomalies in its development or function can hinder descent.
- Reduced Intra-abdominal Pressure: Adequate intra-abdominal pressure may be necessary for testicular descent. Conditions affecting this pressure could contribute to cryptorchidism.
- Intrinsic Testicular or Epididymal Abnormalities: Some research suggests that inherent abnormalities within the testicle or epididymis itself may prevent descent. Studies have shown histological abnormalities in the germinal epithelium of undescended testes. Furthermore, epididymal abnormalities are frequently observed in cases of cryptorchidism, with a higher incidence in intra-abdominal testes compared to less severe cases.
- Endocrine Abnormalities: Hormonal imbalances, particularly involving androgens and anti-Müllerian hormone, are suspected to play a role in testicular descent.
- Anatomic Anomalies: Physical obstructions or anatomical variations in the inguinal canal can impede testicular passage.
Statistics and Incidences
Cryptorchidism is a relatively common condition, affecting approximately 3-5% of newborn males. Bilateral cryptorchidism occurs in about 15% of these cases.
- Spontaneous descent occurs in a significant proportion of infants, particularly within the first four months of life. By one year of age, the prevalence of persistent undescended testis decreases to 0.7-1%.
- Nonpalpable testes account for approximately 20% of all cryptorchidism cases. Of these, roughly 40% are located intra-abdominally, 40% in the inguinal canal, and 20% are atrophic or absent, a condition known as vanishing testis syndrome.
- Prematurity is a significant risk factor, with cryptorchidism observed in up to 30% of premature infants. Other predisposing factors include low birth weight, small size for gestational age, twin pregnancies, and maternal estrogen exposure.
- There is a familial component, with a higher incidence of cryptorchidism in siblings (7%) and fathers (2%) of affected infants.
- Cryptorchidism is exclusive to males and has no reported racial predilection.
Clinical Manifestations
A thorough physical examination is essential for identifying cryptorchidism. Key clinical signs include:
- Hemiscrotal Asymmetry: Visual inspection often reveals an asymmetrical scrotum, with the affected side appearing smaller or less developed due to the absence of the testis.
- Nonpalpable Testis: The primary finding is the inability to palpate one or both testes within the scrotum upon physical examination.
- Contralateral Testicular Hypertrophy: In cases of unilateral cryptorchidism or absent testis, compensatory hypertrophy (enlargement) of the descended testis may occur.
- Empty Scrotal Sac: The affected side of the scrotum may feel empty upon palpation.
Assessment and Diagnosis of Cryptorchidism
Diagnosis of cryptorchidism primarily relies on physical examination. In most cases, laboratory tests and imaging studies are not routinely necessary.
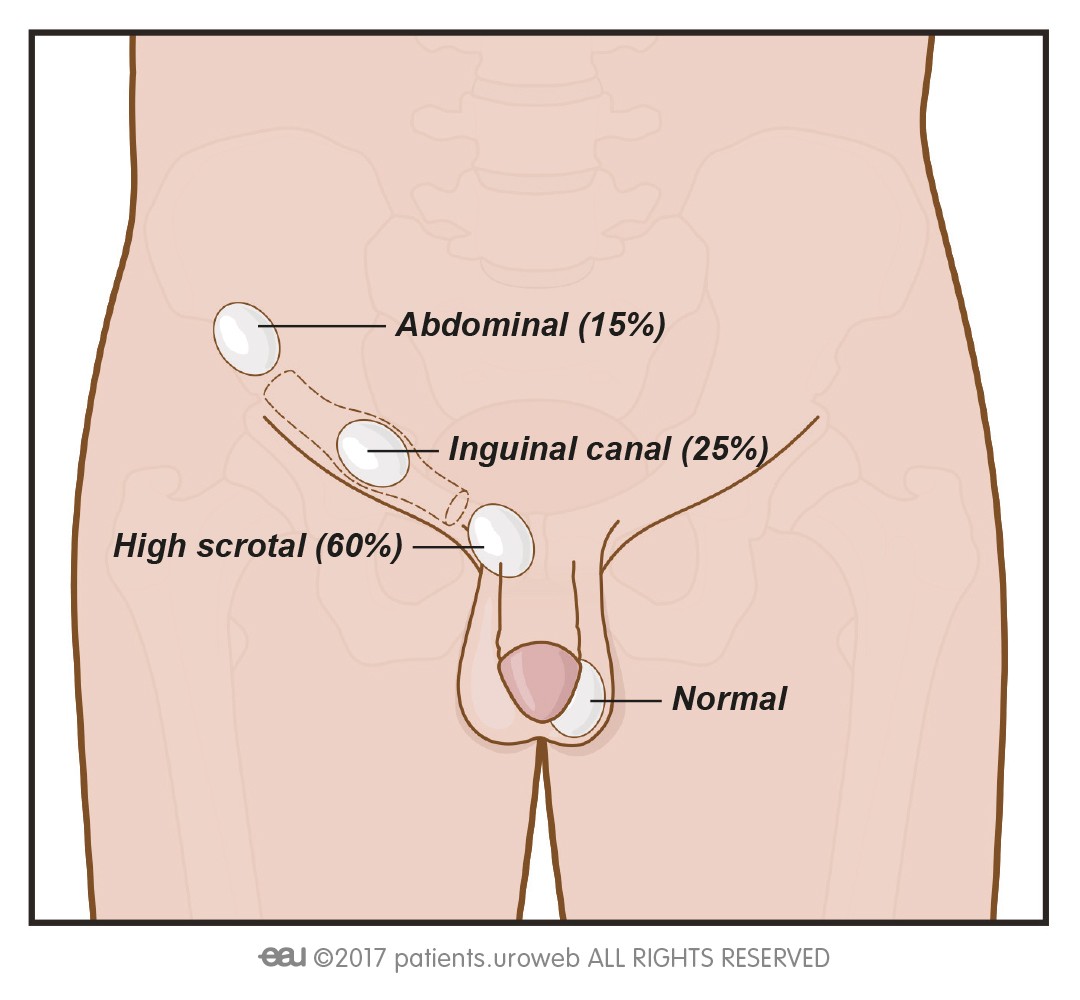 Examination position for cryptorchidism
Examination position for cryptorchidism
Via: https://patients.uroweb.org/
- Physical Examination: Careful palpation of the scrotum and inguinal canal, ideally in a warm environment and with the child in a relaxed position (e.g., frog-legged or cross-legged), is the cornerstone of diagnosis.
- Diagnostic Laparoscopy: For nonpalpable testes, diagnostic laparoscopy is the most accurate method for locating the testis. This minimally invasive surgical procedure allows visualization of the abdominal cavity and inguinal region. Laparoscopy is often performed concurrently with surgical correction (orchiopexy).
- Histologic Findings: Microscopic examination of undescended testes may reveal a range of histological changes, from normal tissue to germ cell hypoplasia and Leydig cell hyperplasia. The severity of these changes is often associated with intra-abdominal location and delayed treatment.
Medical Management of Cryptorchidism
The primary goals of medical management are to facilitate testicular descent, preserve fertility and hormone production, and enable early detection of potential testicular malignancies. Treatment options include hormonal therapy and surgical intervention.
- Hormonal Therapy: Human chorionic gonadotropin (hCG) or gonadotropin-releasing hormone (GnRH) analogs may be used to stimulate testicular descent in some cases, particularly for palpable undescended testes. Hormonal therapy is generally less effective than surgery and is not typically recommended for nonpalpable testes or in cases where anatomical abnormalities are suspected.
- Surgical Intervention (Orchiopexy): Orchiopexy, the surgical fixation of the testis in the scrotum, is the gold standard treatment for cryptorchidism. It is typically recommended for infants between 6 and 18 months of age. Orchiopexy can be performed via open surgery or laparoscopically, depending on the location of the testis and surgeon preference. Early surgical correction significantly improves the chances of fertility and reduces the risk of long-term complications.
NANDA Nursing Diagnosis Care Plans for Cryptorchidism
Nursing care is integral to the management of cryptorchidism, encompassing assessment, pre- and post-operative care, parental education, and emotional support. Utilizing NANDA nursing diagnoses provides a standardized framework for planning and delivering patient-centered care.
Nursing Assessment
A comprehensive nursing assessment for a child with cryptorchidism includes:
- History:
- Gestational age and birth weight (to identify prematurity and low birth weight).
- Family history of cryptorchidism or other congenital anomalies.
- History of palpation of testes in the scrotum at birth or during subsequent well-child visits.
- Parental concerns and understanding of the condition.
- Physical Examination:
- Inspection and palpation of the scrotum to assess for asymmetry, presence, and location of testes.
- Assessment for other congenital anomalies.
- Vital signs and overall health status.
- Developmental stage and age-appropriate responses to examination.
- Psychosocial Assessment:
- Parental anxiety and coping mechanisms related to the child’s condition and planned interventions.
- Family support systems and resources.
NANDA Nursing Diagnoses
Based on the assessment data, relevant NANDA nursing diagnoses for a child with cryptorchidism may include:
- Risk for Injury related to malpositioned testis and potential complications (e.g., testicular torsion, infertility, malignancy).
- Pain related to surgical intervention (post-operative pain).
- Risk for Infection related to surgical procedure.
- Anxiety (Parental) related to child’s diagnosis, planned surgery, and potential outcomes.
- Knowledge Deficit (Parents/Caregivers) related to cryptorchidism, treatment options, and post-operative care.
- Disturbed Body Image (Later Childhood/Adolescence) related to perceived physical difference and potential impact on self-esteem (less common in infancy but relevant for older children diagnosed later or with complications).
Nursing Care Planning and Goals
The major goals of nursing care for a child with cryptorchidism and their family are to:
- Prevent injury and complications associated with undescended testes.
- Manage post-operative pain effectively.
- Prevent infection at the surgical site.
- Reduce parental anxiety and provide emotional support.
- Educate parents/caregivers about cryptorchidism, treatment, and home care.
- Promote positive body image in the child as they grow.
Nursing Interventions
Nursing interventions are tailored to address the identified NANDA nursing diagnoses and achieve the established goals. Key interventions include:
- Pre-operative Care:
- Provide age-appropriate education to the child and parents about the surgical procedure, expected outcomes, and post-operative care.
- Address parental anxieties and concerns, providing emotional support and reassurance.
- Ensure pre-operative assessments and laboratory tests are completed as ordered.
- Prepare the child and family for the hospital experience.
- Post-operative Pain Management:
- Assess pain level regularly using age-appropriate pain scales.
- Administer analgesics as prescribed, ensuring timely and effective pain relief.
- Utilize non-pharmacological pain management techniques, such as positioning, comfort measures, and distraction.
- Educate parents on pain management strategies at home.
- Infection Prevention:
- Maintain a clean and dry surgical site.
- Monitor for signs and symptoms of infection (redness, swelling, drainage, fever).
- Administer prophylactic antibiotics as prescribed.
- Educate parents on wound care and signs of infection to report.
- Parental Anxiety Reduction:
- Provide clear and consistent information about the child’s condition, treatment plan, and progress.
- Encourage parents to express their concerns and ask questions.
- Offer emotional support and reassurance throughout the perioperative period.
- Connect parents with support resources if needed.
- Education and Discharge Planning:
- Provide comprehensive discharge instructions to parents, including wound care, pain management, activity restrictions, and follow-up appointments.
- Educate parents about the importance of long-term follow-up and testicular self-examination as the child reaches puberty.
- Ensure parents understand potential complications and when to seek medical attention.
Evaluation
Evaluation of nursing care involves assessing the achievement of patient goals, as evidenced by:
- The child recovering from surgery without complications (e.g., infection, bleeding).
- Effective pain management, with the child appearing comfortable and pain-free.
- Parents demonstrating reduced anxiety and expressing understanding of the condition and care plan.
- Parents verbalizing understanding of discharge instructions and follow-up care.
- Age-appropriate understanding and acceptance of body image as the child develops.
Documentation Guidelines
Accurate and thorough documentation is essential for continuity of care and legal purposes. Documentation for a child with cryptorchidism should include:
- Baseline assessment findings, including testicular palpation and scrotal appearance.
- NANDA nursing diagnoses identified.
- Nursing care plan and interventions implemented.
- Pain assessments and pain management interventions.
- Wound assessments and infection monitoring.
- Parental education provided and their level of understanding.
- Child’s response to interventions and progress towards goals.
- Discharge instructions provided to parents/caregivers.
Conclusion
NANDA nursing diagnosis care plans provide a valuable framework for nurses caring for infants and children with cryptorchidism. By utilizing this structured approach, nurses can effectively assess patient needs, formulate appropriate diagnoses, implement targeted interventions, and evaluate outcomes. Comprehensive nursing care, encompassing physical, emotional, and educational support, is essential to optimize outcomes for children with cryptorchidism and their families, promoting long-term health and well-being.
