Crafting the best nursing care plan hinges on a systematic approach to accurately address patient needs. This guide provides a comprehensive walkthrough for developing effective care plans, enriched with insights and strategies for both nursing students and seasoned professionals. Utilize our extensive database of nursing care plans (NCPs) and nursing diagnosis examples to elevate your practice—all accessible for free. Delve into the essential components, objectives, and purposes of nursing care plans, alongside a detailed guide and templates to streamline your care planning process.
Table of Contents
Understanding the Nursing Care Plan
A nursing care plan (NCP) is a structured methodology used to pinpoint current health needs and anticipate potential risks for patients. It serves as a vital communication tool amongst nurses, patients, and the broader healthcare team, ensuring cohesive efforts towards achieving optimal health outcomes. The nursing care planning process is indispensable for maintaining quality and consistency in patient care, preventing fragmented or overlooked interventions.
The creation of a nursing care plan begins at the point of patient admission and is a dynamic process, continually updated to reflect changes in the patient’s condition and the evaluation of progress towards goals. This dedication to individualized, patient-centered care is the cornerstone of excellent nursing practice.
Types of Nursing Care Plans
Nursing care plans can be broadly categorized as informal or formal. An informal nursing care plan is essentially a mental strategy, a nurse’s internal roadmap for patient care. In contrast, a formal nursing care plan is a documented, either written or digital, guide that systematically organizes all relevant patient care information.
Formal care plans are further divided into standardized and individualized types. Standardized care plans are designed to address the common needs of patient groups with similar conditions, ensuring consistent baseline care. Individualized care plans are customized to meet the specific and unique needs of a particular patient, going beyond the scope of standardized plans to offer personalized care.
Standardized Care Plans
Standardized care plans are pre-established protocols developed by nursing staff and healthcare institutions to guarantee uniform care for patients with specific conditions. These plans are instrumental in setting a minimum standard of care and optimizing nurses’ efficiency by eliminating redundant planning for routine patient needs within a unit.
It’s important to note that standardized care plans are not designed to meet every patient’s unique requirements. Instead, they serve as an effective starting point for developing more tailored, individualized care plans.
The care plans featured in this resource are standardized plans, intended to provide a foundational framework for creating individualized care plans.
Individualized Care Plans
An individualized care plan involves adapting a standardized plan to precisely match the unique health goals and needs of each patient. This approach incorporates strategies known to be effective for the individual, allowing for a more personalized and holistic care experience that aligns with the patient’s specific circumstances, strengths, and objectives.
Furthermore, individualized care plans are directly linked to improved patient satisfaction. When patients perceive their care as specifically designed for them, they feel more valued and understood, which enhances their overall satisfaction with the healthcare experience. In today’s patient-centric healthcare environment, where patient satisfaction is a key indicator of quality, this personalization is increasingly crucial.
Key Tips for Individualizing Nursing Care Plans:
- Incorporate Patient Preferences: Actively seek and integrate patient preferences and values into the care plan to ensure it resonates with their personal needs and beliefs.
- Address Unique Needs: Identify and specifically address any unique physical, psychological, social, cultural, or spiritual needs that are not covered in standardized plans.
- Collaborative Goal Setting: Work together with the patient and their family to set realistic and achievable goals that are meaningful to them.
- Dynamic Adaptation: Regularly review and adjust the care plan in response to the patient’s changing condition, feedback, and new information.
- Utilize Interdisciplinary Input: Collaborate with other healthcare professionals to incorporate their expertise and create a comprehensive, patient-centered plan.
Objectives of Nursing Care Plans
The primary goals and objectives of creating a nursing care plan include:
- Promoting Evidence-Based Practice: To ensure nursing care is grounded in the latest research and best practices, fostering effective and reliable healthcare delivery in hospital and clinical settings.
- Supporting Holistic Patient Care: To address the patient as a whole person, considering their physical, psychological, social, and spiritual dimensions in the prevention and management of illness.
- Establishing Care Pathways and Bundles: To create structured, interdisciplinary approaches to care, like care pathways for standardized care protocols and care bundles for evidence-based practices in specific conditions.
- Clearly Defining Goals and Outcomes: To set distinct, measurable goals and expected outcomes that guide the care process and provide benchmarks for progress.
- Enhancing Communication and Documentation: To improve the clarity and effectiveness of care plan documentation, facilitating better communication among healthcare providers.
- Measuring Nursing Care Effectiveness: To provide a framework for evaluating the impact of nursing interventions and the overall quality of care delivered.
Purposes of a Nursing Care Plan
The creation and implementation of a nursing care plan are crucial for several reasons:
- Defining the Nurse’s Role: Care plans clarify the unique and autonomous role of nurses in addressing patients’ overall health and wellness, beyond merely following physician directives.
- Guiding Individualized Patient Care: They act as a detailed roadmap for patient care, enabling nurses to apply critical thinking to develop interventions specifically tailored to each patient’s needs.
- Ensuring Continuity of Care: By providing a consistent reference, care plans allow nurses across different shifts and departments to deliver uniform, high-quality interventions, maximizing the benefits of treatment for patients.
- Coordinating Care Among Teams: Care plans ensure that all members of the healthcare team are informed of the patient’s needs and the required actions, preventing gaps and overlaps in care.
- Facilitating Comprehensive Documentation: They serve as a structured format to document observations, nursing actions, and patient/family instructions accurately. Proper documentation in the care plan is evidence that care was indeed provided.
- Aiding Staff Assignment: Care plans help in matching patient needs with staff skills, ensuring that patients are cared for by professionals with the appropriate expertise.
- Monitoring Patient Progress: They provide a mechanism to track patient progress and make necessary adjustments to the care strategy as health conditions and goals evolve.
- Supporting Reimbursement Processes: Insurance providers often rely on medical records, including care plans, to determine the coverage and reimbursement for hospital services.
- Clarifying Patient Goals: Care plans actively involve patients in their treatment and care, promoting a collaborative approach to healthcare.
Components of a Nursing Care Plan
A typical nursing care plan (NCP) encompasses several key components, including nursing diagnoses, patient problems, expected outcomes, nursing interventions, and rationales. Each of these elements is crucial for a well-rounded and effective care strategy.
Care Plan Formats
Nursing care plans are commonly structured in formats that organize information into columns, typically ranging from three to five columns to enhance clarity and ease of use.
Three-Column Format
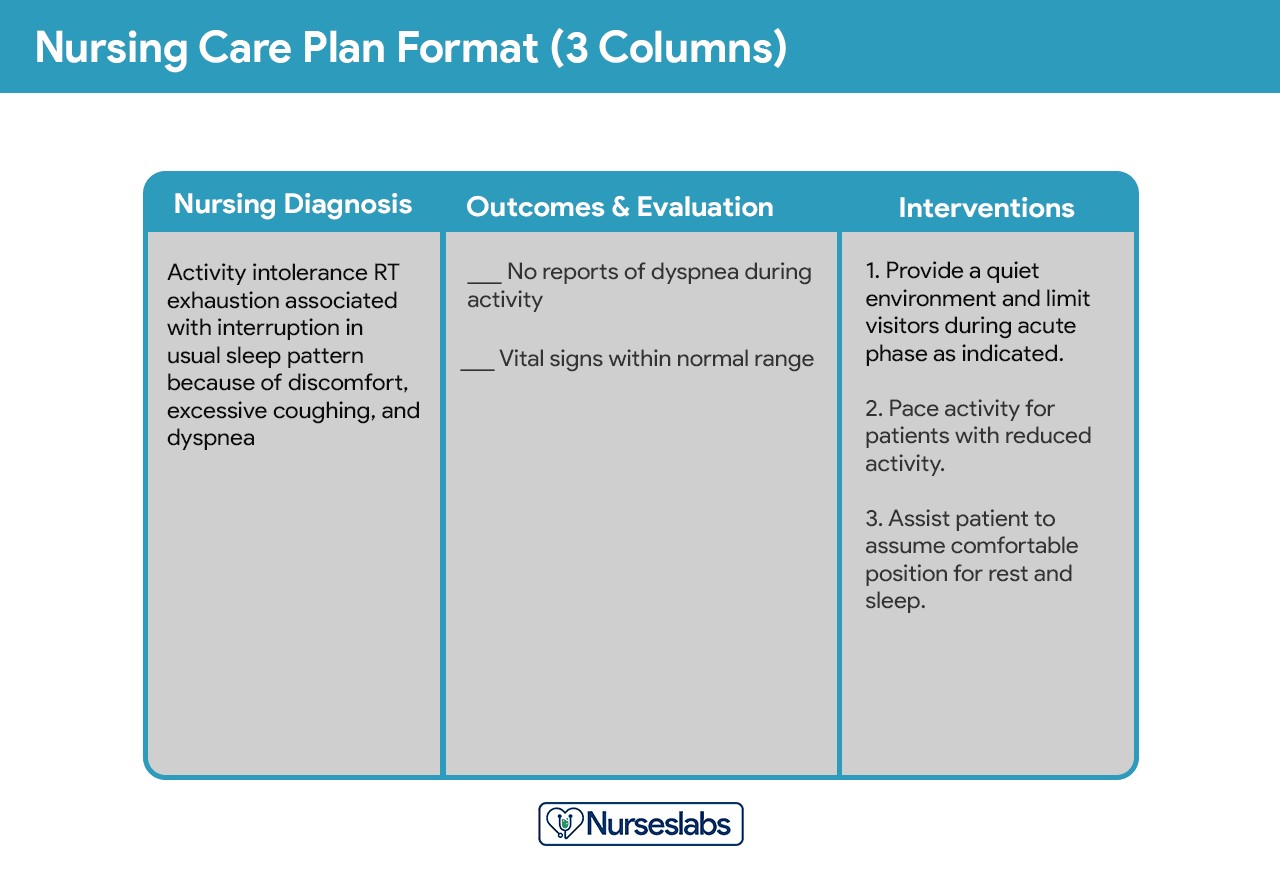
The three-column format simplifies the care plan into nursing diagnosis, outcomes and evaluation, and interventions, offering a concise overview of the care strategy.
Image alt text: Example of a three-column nursing care plan format, showing columns for Nursing Diagnosis, Outcomes/Evaluation, and Interventions.
Four-Column Format
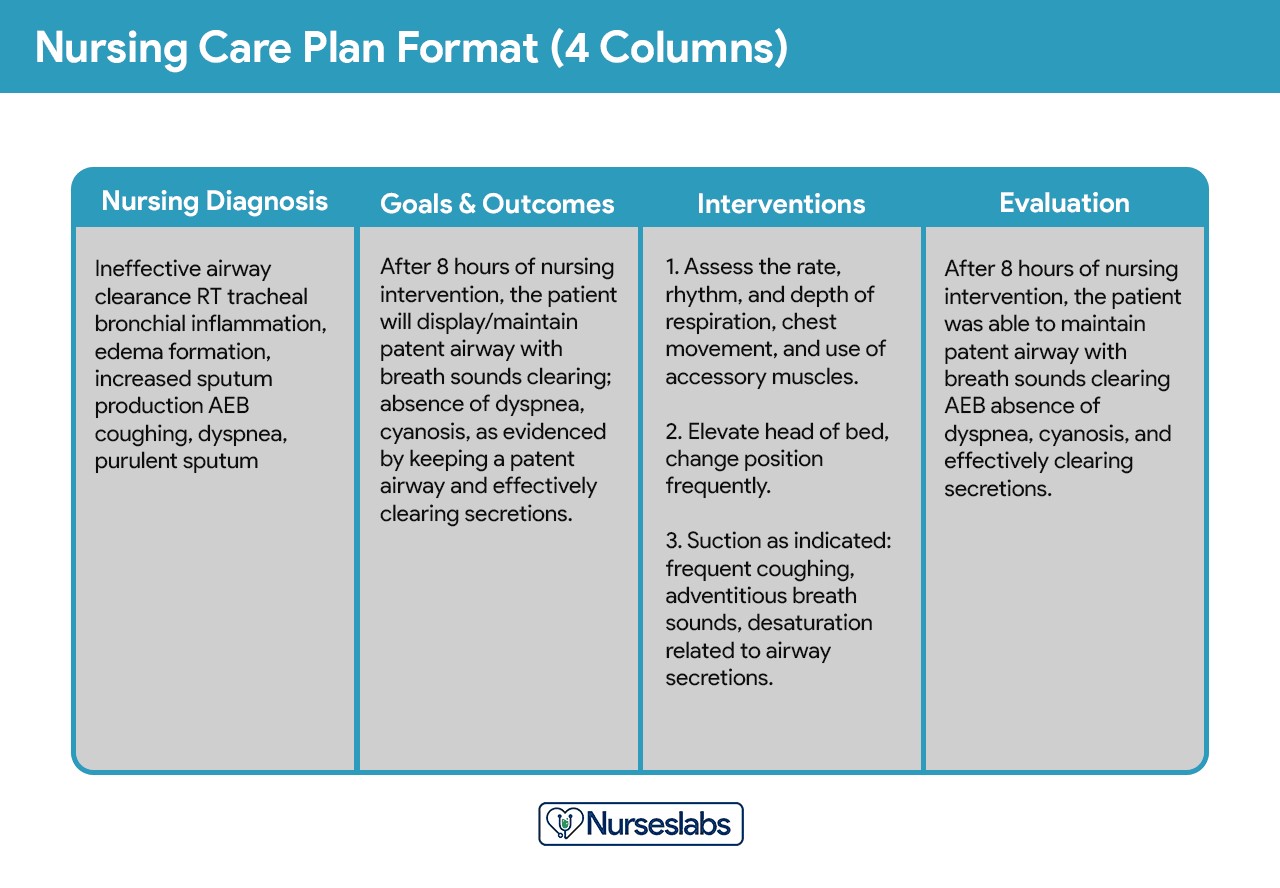
Expanding on the three-column format, the four-column plan separates outcomes and evaluation into distinct columns, providing more detailed sections for nursing diagnosis, goals and outcomes, interventions, and evaluation.
Image alt text: Sample four-column nursing care plan template, illustrating columns for Nursing Diagnosis, Goals/Outcomes, Interventions, and Evaluation.
For your convenience, we have prepared sample templates for various nursing care plan formats. These are available for download, modification, and distribution.
Download: Printable Nursing Care Plan Templates and Formats
Student Care Plans
Student care plans are designed to be more comprehensive and detailed than those used by practicing nurses. This is because they serve as a valuable learning tool for nursing students, helping them to understand the rationale behind each aspect of patient care.
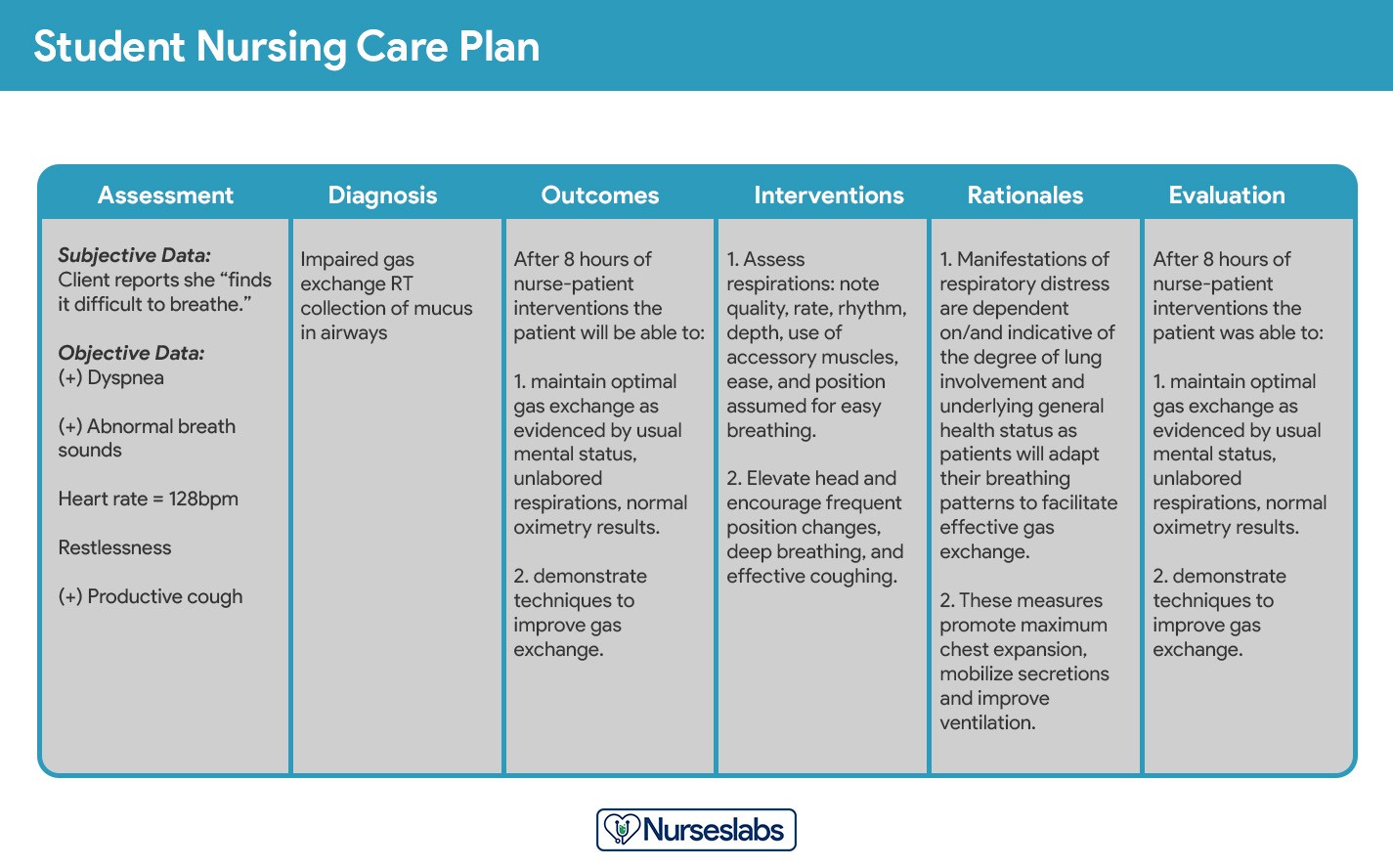
Image alt text: Example of a student nursing care plan format, highlighting the increased detail and inclusion of rationales for interventions.
Typically, student care plans are handwritten and include an additional column for “Rationale” or “Scientific Explanation” following the nursing interventions. These rationales provide the scientific basis for each selected nursing intervention, reinforcing the student’s understanding of evidence-based practice.
Writing an Effective Nursing Care Plan
How can you create a robust nursing care plan (NCP)? Follow these essential steps to develop a client-centered care plan.
Step 1: Comprehensive Data Collection and Assessment
The initial step in formulating a nursing care plan is to compile a thorough patient database. This involves employing various assessment techniques and data collection methods, including physical examinations, health history interviews, reviews of medical records, and diagnostic studies. A complete patient database encompasses all relevant health information gathered. During this phase, nurses identify related or risk factors and defining characteristics that are crucial for formulating accurate nursing diagnoses. Many institutions and nursing programs provide specific assessment formats to guide this process.
Critical thinking is paramount in patient assessment, integrating scientific knowledge and professional guidelines to inform evaluations. This process is essential for complex clinical decision-making and aims to effectively identify patients’ healthcare needs within a supportive and informed environment.
Step 2: Data Analysis and Organization
Once patient data is collected, the next step is to analyze, cluster, and organize this information. This structured analysis is vital for formulating nursing diagnoses, setting priorities, and defining desired patient outcomes.
Step 3: Formulating Accurate Nursing Diagnoses
Nursing diagnoses provide a standardized language for identifying and addressing specific patient needs and responses to both actual and potential health issues. These diagnoses are statements of health problems that nurses are qualified and licensed to treat independently. They focus on conditions that nursing interventions can prevent or resolve.
For a detailed guide on formulating nursing diagnoses, refer to our comprehensive resource: Nursing Diagnosis (NDx): Complete Guide and List.
Step 4: Prioritizing Nursing Diagnoses
Setting priorities involves ranking nursing diagnoses to determine the order in which they will be addressed. This step requires collaboration between the nurse and patient to decide which problems require immediate attention. Diagnoses are typically categorized as high, medium, or low priority, with life-threatening issues taking precedence.
Maslow’s Hierarchy of Needs provides a useful framework for prioritizing nursing diagnoses and planning patient care based on fundamental human needs. Introduced by Abraham Maslow in 1943, this hierarchy posits that basic physiological needs must be satisfied before higher-level needs, such as self-esteem and self-actualization, can be addressed. Physiological and safety needs form the foundation of nursing care and interventions, residing at the base of Maslow’s pyramid as essential prerequisites for physical and emotional well-being.
Maslow’s Hierarchy of Needs:
- Basic Physiological Needs: These include the essentials for survival: nutrition (water and food), elimination, airway management (suction), breathing (oxygen administration), circulation (monitoring pulse, cardiac function, blood pressure), sleep, sexual health, shelter, and exercise.
- Safety and Security Needs: Focus on preventing harm and ensuring security through injury prevention (using side rails, call lights, practicing hand hygiene, implementing isolation protocols, suicide precautions, fall prevention, car seats, helmets, seat belts), fostering trust and safety through therapeutic relationships, and patient education on modifiable risk factors (e.g., for stroke, heart disease).
- Love and Belonging Needs: Address the need for social connection and support by fostering supportive relationships, preventing social isolation, employing active listening and therapeutic communication techniques, and addressing needs for sexual intimacy.
- Self-Esteem Needs: Involve building confidence and self-respect through community acceptance, workplace recognition, personal achievements, a sense of control, and positive body image.
- Self-Actualization Needs: Represent the highest level of personal growth, facilitated by empowering environments, spiritual development, the ability to consider diverse perspectives, and striving to reach one’s full potential.
Image alt text: Diagram illustrating Virginia Henderson’s 14 Basic Needs applied to Maslow’s Hierarchy of Needs, showing the correlation between fundamental nursing needs and Maslow’s levels.
Patient values, beliefs, available resources, and the urgency of the health issue are critical factors in determining priorities. Engaging patients in this process enhances their cooperation and commitment to the care plan.
Step 5: Setting Patient Goals and Desired Outcomes
Following the prioritization of nursing diagnoses, nurses collaborate with patients to establish goals for each priority. Goals or desired outcomes define the intended results of nursing interventions, derived from the patient’s nursing diagnoses. These goals guide the planning of interventions, provide criteria for evaluating patient progress, help in determining when problems are resolved, and motivate both patient and nurse by providing a sense of accomplishment.
Image alt text: Examples of well-written nursing care plan goals and desired outcomes, demonstrating specific, measurable, and patient-centered criteria.
A primary goal is set for each nursing diagnosis. The terms “goal outcomes” and “expected outcomes” are often used interchangeably.
Effective goals should be SMART, an acronym for Specific, Measurable, Attainable, Realistic, and Time-oriented.
- Specific: Goals should be clear, significant, and focused to be effective.
- Measurable: Goals must be quantifiable to allow for progress monitoring and determination of achievement.
- Attainable: Goals should be challenging yet realistically achievable, promoting progress without being discouraging.
- Realistic: Goals need to be practical and consider available resources and patient circumstances to ensure successful outcomes.
- Time-Oriented: Each goal should have a defined timeframe, creating a sense of urgency and a target for achievement.
Additionally, utilizing the REEPIG standards ensures high-quality care planning. REEPIG stands for:
- Realistic: Goals are feasible within the context of available resources.
- Explicitly stated: Care plans are clear and unambiguous, leaving no room for misinterpretation.
- Evidence-based: Interventions are supported by research and best practices.
- Prioritized: The most critical issues are addressed first.
- Involve: Patients and the multidisciplinary team are actively involved in the planning process.
- Goal-centered: The planned care is directly aimed at achieving the set goals.
Short-Term and Long-Term Goals
Goals and expected outcomes must be measurable and patient-centered, focusing on problem prevention, resolution, and rehabilitation. Goals are classified as short-term or long-term. In acute care settings, short-term goals are more common due to the immediate focus on patients’ urgent needs. Long-term goals are typically used for patients with chronic conditions or those in long-term care facilities.
- Short-term goals: These are achievable within a short period, typically hours to days, representing immediate improvements in patient behavior or condition.
- Long-term goals: These are broader objectives expected to be achieved over weeks or months, suitable for ongoing care and chronic conditions.
- Discharge planning: Primarily involves setting long-term goals that facilitate continued recovery and problem resolution through home health services, physical therapy, and other referrals.
Components of Effective Goals and Desired Outcomes
Goal statements generally include four essential components: a subject, a verb, conditions or modifiers, and a criterion of desired performance.
Image alt text: Breakdown of the components of desired outcomes and goals in a nursing care plan, including subject, verb, conditions/modifiers, and criterion of performance.
- Subject: Usually the patient, or a specific aspect of the patient (e.g., pulse, temperature, urinary output). Often implied to be the patient unless otherwise specified (e.g., family, caregiver).
- Verb: Specifies the action the patient is expected to perform, learn, or experience.
- Conditions or modifiers: Detail the circumstances under which the behavior should occur (what, when, where, how).
- Criterion of desired performance: Defines the standard for evaluating performance or the level at which the patient should perform the specified behavior. This component is optional but enhances goal measurability.
Tips for Writing Effective Goals and Desired Outcomes:
- Frame goals and outcomes in terms of patient responses rather than nurse activities. Start each goal with “Patient will […]” to maintain patient-centered focus.
- Avoid stating goals based on nursing actions or hopes; instead, concentrate on observable patient behaviors.
- Use measurable, observable terms for outcomes, avoiding vague language that is open to interpretation.
- Ensure outcomes are realistic considering the patient’s resources, abilities, limitations, and the care timeframe.
- Verify that goals are consistent with other therapeutic interventions from the healthcare team.
- Derive each goal from a single nursing diagnosis to facilitate clear evaluation of care and ensure interventions are directly linked to the diagnosis.
- Confirm that the patient values and considers the goals important to encourage their active participation and cooperation.
Step 6: Selecting Appropriate Nursing Interventions
Nursing interventions are the specific actions nurses take to help patients achieve their goals. These interventions should aim to eliminate or reduce the underlying causes of the nursing diagnosis. For risk diagnoses, interventions focus on mitigating risk factors. Although identified and planned during the planning phase of the nursing process, interventions are implemented during the implementation phase.
Types of Nursing Interventions
Nursing interventions can be categorized as independent, dependent, or collaborative.
Image alt text: Diagram illustrating the types of nursing interventions: Independent, Dependent, and Collaborative, with examples of each.
- Independent nursing interventions are actions nurses are authorized to initiate based on their professional judgment and expertise. These include ongoing assessments, emotional support, comfort measures, patient education, physical care, and referrals to other healthcare professionals.
- Dependent nursing interventions are carried out under the direction of a physician’s orders or supervision. This category includes administering medications, IV therapy, diagnostic tests, treatments, diet modifications, and activity or rest regimens. Nurses also provide assessments and explanations related to these medical orders.
- Collaborative interventions involve actions undertaken in cooperation with other healthcare team members, such as physicians, social workers, dietitians, and therapists. These interventions are developed through interdisciplinary consultation to integrate diverse professional perspectives.
Nursing interventions should be:
- Safe and suitable for the patient’s age, health status, and condition.
- Achievable with available resources and time constraints.
- Consistent with the patient’s values, cultural background, and beliefs.
- Compatible with other therapies the patient is receiving.
- Based on established nursing knowledge, experience, and relevant scientific principles.
Guidelines for Writing Nursing Interventions:
- Date and sign the care plan to ensure accountability and to provide a timeframe for review and evaluation.
- Interventions should be specific and clearly articulated, beginning with an action verb that describes the nurse’s expected action. Include qualifiers detailing how, when, where, and how often the intervention should be performed. For example: “Educate parents on how to measure temperature and report any changes,” or “Assess urine for color, volume, odor, and turbidity.”
- Use only institution-approved abbreviations to maintain clarity and avoid confusion.
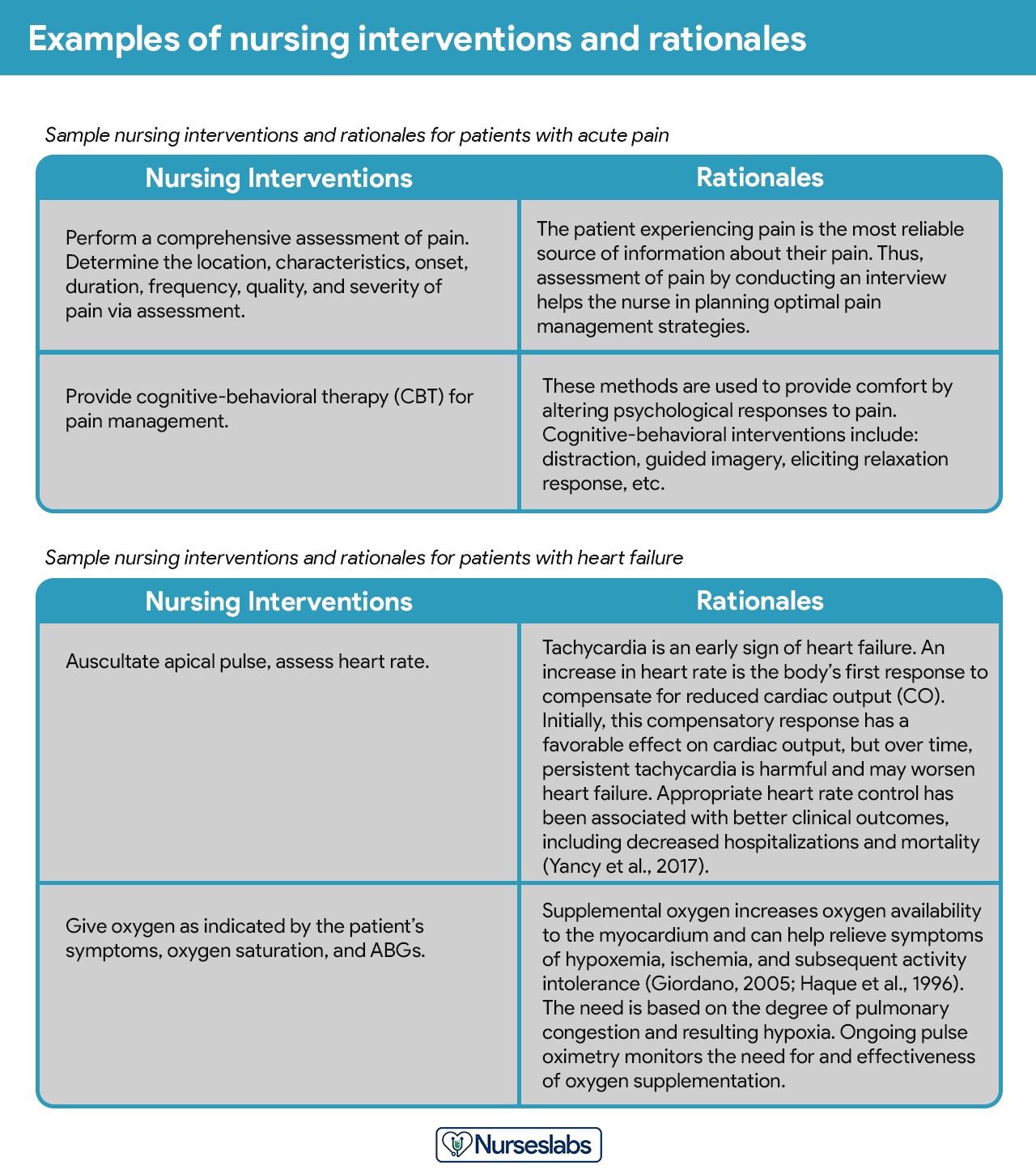
Step 7: Providing Rationale for Interventions
Rationales, or scientific explanations, justify why each nursing intervention is selected for the care plan.
Image alt text: Example of nursing interventions with corresponding rationales in a care plan, showing the scientific basis for each action.
Rationales are typically included in student care plans to help students link pathophysiological and psychological principles to the chosen interventions, enhancing their understanding of the evidence-based practice.
Step 8: Evaluation of the Care Plan
Evaluation is a continuous, planned, and purposeful process to assess the patient’s progress toward achieving goals and to determine the effectiveness of the nursing care plan. This step is critical in the nursing process as it informs decisions about whether to continue, modify, or terminate specific nursing interventions.
Step 9: Documenting the Care Plan
The patient’s care plan is documented according to hospital policy and becomes a part of their permanent medical record, accessible for review by all members of the healthcare team. Nursing programs often use varied care plan formats, many following a five-column structure that systematically guides students through the interrelated steps of the nursing process.
Comprehensive Nursing Care Plan List
This section provides a categorized list of sample nursing care plans (NCPs) and nursing diagnoses for various health conditions and diseases, offering a broad spectrum of resources for clinical practice and study.
Basic Nursing and General Care Plans
A collection of diverse nursing care plan examples applicable across various healthcare settings:
| Basic Nursing & General Care Plans |
|---|
| Acute Confusion (Delirium) and Altered Mental Status |
| Acute Pain and Pain Management |
| Activity Intolerance and Generalized Weakness |
| Cancer (Oncology Nursing) |
| Caregiver Role Strain and Family Caregiver Support Systems |
| Chronic Confusion (Dementia) |
| End-of-Life Care (Hospice Care or Palliative) |
| Fall Risk and Fall Prevention |
| Fatigue and Lethargy |
| Geriatric Nursing (Older Adult) |
| Grieving and Loss |
| Hypothermia and Cold Injuries |
| Hyperthermia (Fever) |
| Impaired Swallowing (Dysphagia) |
| Insomnia and Sleep Deprivation |
| Prolonged Bed Rest |
| Risk for Injury and Patient Safety |
| Self-Care and Activities of Daily Living (ADLs) |
| Surgery (Perioperative Client) |
| Systemic Lupus Erythematosus |
| Total Parenteral Nutrition |




Surgery and Perioperative Care Plans
Care plans tailored for patients undergoing surgical procedures and perioperative care:
| Surgery and Perioperative Care Plans |
|---|
| Amputation |
| Appendectomy |
| Cholecystectomy |
| Fracture UPDATED! |
| Hemorrhoids |
| Hysterectomy |
| Ileostomy & Colostomy |
| Laminectomy (Disc Surgery) |
| Mastectomy |
| Subtotal Gastrectomy |
| Surgery (Perioperative Client) |
| Thyroidectomy |
| Total Joint (Knee, Hip) Replacement |
Cardiac Care Plans
Nursing care plans focused on managing conditions of the cardiovascular system:
| Cardiac Care Plans |
|---|
| Angina Pectoris (Coronary Artery Disease) |
| Cardiac Arrhythmia (Digitalis Toxicity) |
| Cardiac Catheterization |
| Cardiogenic Shock |
| Congenital Heart Disease |
| Decreased Cardiac Output & Cardiac Support |
| Heart Failure UPDATED! |
| Hypertension UPDATED! |
| Hypovolemic Shock |
| Impaired Tissue Perfusion & Ischemia |
| Myocardial Infarction |
| Pacemaker Therapy |
Endocrine and Metabolic Care Plans
Care plans addressing disorders of the endocrine system and metabolic processes:
| Endocrine and Metabolic Care Plans |
|---|
| Addison’s Disease |
| Cushing’s Disease |
| Diabetes Mellitus (Type 1, Type 2) UPDATED! |
| Diabetic Ketoacidosis (DKA) and Hyperglycemic Hyperosmolar Nonketotic Syndrome (HHNS) |
| Eating Disorders: Anorexia & Bulimia Nervosa |
| Fluid Volume Deficit (Dehydration & Hypovolemia) |
| Fluid Volume Excess (Hypervolemia) |
| Gestational Diabetes Mellitus |
| Hyperthyroidism |
| Hypothyroidism |
| Imbalanced Nutrition (Malnutrition) |
| Obesity & Overweight |
| Thyroidectomy |
| Unstable Blood Glucose Levels (Hyperglycemia & Hypoglycemia) |
| Acid-Base Imbalances |
|---|
| Metabolic Acidosis |
| Metabolic Alkalosis |
| Respiratory Acidosis |
| Respiratory Alkalosis |
| Electrolyte Imbalances |
|---|
| Calcium (Ca) Imbalances: Hypercalcemia and Hypocalcemia |
| Magnesium (Mg) Imbalances: Hypermagnesemia and Hypomagnesemia |
| Potassium (K) Imbalances: Hyperkalemia and Hypokalemia |
| Sodium (Na) Imbalances: Hypernatremia and Hyponatremia |
Gastrointestinal Care Plans
Care plans addressing disorders of the gastrointestinal and digestive system:
| Gastrointestinal Care Plans |
|---|
| Appendectomy |
| Bowel Incontinence (Fecal Incontinence) |
| Cholecystectomy |
| Constipation |
| Diarrhea Nursing Care Plan and Management |
| Cholecystitis and Cholelithiasis |
| Gastroenteritis |
| Gastroesophageal Reflux Disease (GERD) |
| Hemorrhoids |
| Hepatitis |
| Ileostomy & Colostomy |
| Inflammatory Bowel Disease (IBD) |
| Intussusception |
| Liver Cirrhosis |
| Nausea & Vomiting |
| Pancreatitis |
| Peritonitis |
| Peptic Ulcer Disease |
| Subtotal Gastrectomy |
| Umbilical and Inguinal Hernia |
Hematologic and Lymphatic Care Plans
Care plans related to disorders of the hematologic and lymphatic systems:
| Hematologic & Lymphatic Care Plans |
|---|
| Anaphylactic Shock |
| Anemia UPDATED! |
| Aortic Aneurysm |
| Bleeding Risk & Hemophilia |
| Deep Vein Thrombosis |
| Disseminated Intravascular Coagulation |
| Hemophilia |
| Kawasaki Disease |
| Leukemia |
| Lymphoma |
| Sepsis and Septicemia |
| Sickle Cell Anemia Crisis |
Infectious Diseases Care Plans
Care plans for managing communicable and infectious diseases:
| Infectious Diseases Care Plans |
|---|
| Acquired Immunodeficiency Syndrome (AIDS) (HIV Positive) |
| Acute Rheumatic Fever |
| Dengue Hemorrhagic Fever |
| Herpes Zoster (Shingles) |
| Influenza (Flu) |
| Pulmonary Tuberculosis |
| Risk for Infection & Infection Control |
Integumentary Care Plans
Care plans focusing on conditions affecting the integumentary system:
| Integumentary Care Plans |
|---|
| Burn Injury |
| Dermatitis |
| Herpes Zoster (Shingles) |
| Pressure Ulcer (Bedsores) |
| Wound Care and Skin/Tissue Integrity |
Maternal and Newborn Care Plans
Nursing care plans for the care of pregnant mothers and newborns:
| Maternal and Newborn Care Plans |
|---|
| Abortion (Termination of Pregnancy) |
| Cervical Insufficiency (Premature Dilation of the Cervix) |
| Cesarean Birth |
| Cleft Palate and Cleft Lip |
| Gestational Diabetes Mellitus |
| Hyperbilirubinemia (Jaundice) |
| Labor Stages, Induced, Augmented, Dysfunctional, Precipitous Labor |
| Neonatal Sepsis |
| Perinatal Loss (Miscarriage, Stillbirth) |
| Placental Abruption |
| Placenta Previa |
| Postpartum Hemorrhage |
| Postpartum Thrombophlebitis |
| Prenatal Hemorrhage |
| Preeclampsia and Gestational Hypertension |
| Prenatal Infection |
| Preterm Labor |
| Puerperal & Postpartum Infections |
| Substance (Alcohol and Drug) Abuse in Pregnancy |
Mental Health and Psychiatric Care Plans
Care plans for mental health and psychiatric nursing:
| Mental Health and Psychiatric Care Plans |
|---|
| Alcohol Withdrawal |
| Anxiety & Fear |
| Anxiety and Panic Disorders |
| Bipolar Disorders |
| Body Image Disturbance & Self-Esteem |
| Impaired Thought Processes & Cognitive Impairment |
| Major Depression |
| Personality Disorders |
| Schizophrenia |
| Sexual Assault |
| Substance Dependence and Abuse |
| Suicide Behaviors |
Musculoskeletal Care Plans
Care plans related to the musculoskeletal system:
| Musculoskeletal Care Plans |
|---|
| Amputation |
| Congenital Hip Dysplasia |
| Fracture UPDATED! |
| Impaired Physical Mobility & Immobility |
| Juvenile Rheumatoid Arthritis |
| Laminectomy (Disc Surgery) |
| Osteoarthritis |
| Osteogenic Sarcoma (Osteosarcoma) |
| Osteoporosis |
| Rheumatoid Arthritis |
| Scoliosis |
| Spinal Cord Injury |
| Total Joint (Knee, Hip) Replacement |
Neurological Care Plans
Nursing care plans for disorders of the nervous system:
| Neurological Care Plans |
|---|
| Alzheimer’s Disease UPDATED! |
| Brain Tumor |
| Cerebral Palsy |
| Cerebrovascular Accident (Stroke) UPDATED! |
| Guillain-Barre Syndrome |
| Meningitis |
| Multiple Sclerosis |
| Parkinson’s Disease |
| Seizure Disorder |
| Spinal Cord Injury |
Ophthalmic Care Plans
Care plans related to eye disorders:
| Ophthalmic Care Plans |
|---|
| Cataracts |
| Glaucoma |
| Macular Degeneration |
Pediatric Nursing Care Plans
Nursing care plans for pediatric conditions and diseases:
| Pediatric Nursing Care Plans |
|---|
| Child Abuse |
| Cleft Lip and Cleft Palate |
| Dying Child |
| Febrile Seizure |
| Hospitalized Child |
| Hydrocephalus |
| Otitis Media |
| Spina Bifida |
| Tonsillitis and Adenoiditis |
Reproductive Care Plans
Care plans addressing reproductive and sexual function disorders:
| Reproductive Care Plans |
|---|
| Cryptorchidism (Undescended Testes) |
| Hysterectomy |
| Hypospadias and Epispadias |
| Mastectomy |
| Menopause |
| Prostatectomy |
Respiratory Care Plans
Care plans for disorders of the respiratory system:
| Respiratory Care Plans |
|---|
| Airway Clearance Therapy & Coughing |
| Apnea |
| Asthma UPDATED! |
| Aspiration Risk & Aspiration Pneumonia |
| Bronchiolitis UPDATED! |
| Bronchopulmonary Dysplasia (BPD) UPDATED! |
| Chronic Obstructive Pulmonary Disease (COPD) UPDATED! |
| Croup Syndrome |
| Cystic Fibrosis UPDATED! |
| Epiglottitis |
| Hemothorax and Pneumothorax UPDATED! |
| Ineffective Breathing Pattern (Dyspnea) |
| Impairment of Gas Exchange |
| Influenza (Flu) UPDATED! |
| Lung Cancer UPDATED! |
| Mechanical Ventilation |
| Near-Drowning |
| Pleural Effusion |
| Pneumonia |
| Pulmonary Embolism |
| Pulmonary Tuberculosis |
| Tracheostomy |
Urinary Care Plans
Care plans related to kidney and urinary system disorders:
| Urinary Care Plans |
|---|
| Acute Glomerulonephritis |
| Acute Renal Failure |
| Benign Prostatic Hyperplasia (BPH) |
| Chronic Renal Failure |
| Hemodialysis |
| Nephrotic Syndrome |
| Peritoneal Dialysis |
| Urolithiasis (Renal Calculi) |
| Urinary Elimination (Urinary Incontinence & Urinary Retention) |
| Urinary Tract Infection |
| Vesicoureteral Reflux (VUR) |
| Wilms Tumor (Nephroblastoma) |
Recommended Resources for Nursing Care Plans
Enhance your understanding and skills in nursing care planning with these highly recommended books and resources.
Disclosure: The following are affiliate links from Amazon. As an affiliate, we may earn a small commission from qualifying purchases at no extra cost to you. For more details, please refer to our privacy policy.
Ackley and Ladwig’s Nursing Diagnosis Handbook: An Evidence-Based Guide to Planning Care
This handbook is invaluable for its evidence-based approach to nursing interventions. It employs a user-friendly, three-step system to guide you through patient assessment, nursing diagnosis, and care plan development. It includes detailed instructions on implementing care and evaluating outcomes, thereby enhancing your diagnostic reasoning and critical thinking skills.
Nursing Care Plans – Nursing Diagnosis & Intervention (10th Edition)
Featuring over 200 care plans, this resource reflects the latest evidence-based guidelines. The newest edition includes ICNP diagnoses, care plans addressing LGBTQ health issues, and comprehensive coverage of electrolyte and acid-base balance.
Image alt text: Cover image of the “Nursing Care Plans – Nursing Diagnosis & Intervention” 10th Edition book, showcasing its value as a resource for nursing students and professionals.
Nurse’s Pocket Guide: Diagnoses, Prioritized Interventions, and Rationales
This quick-reference tool provides essential information for accurate diagnoses and efficient care planning. The 16th edition features the most current nursing diagnoses and interventions, with an alphabetized listing covering over 400 disorders.
Nursing Diagnosis Manual: Planning, Individualizing, and Documenting Client Care
This manual helps you identify interventions to plan, personalize, and document care for over 800 diseases and disorders. It uniquely offers subjective and objective data for each diagnosis, sample clinical applications, prioritized interventions with rationales, and dedicated documentation sections.
Image alt text: Cover image of the “Nursing Diagnosis Manual: Planning, Individualizing, and Documenting Client Care” book, highlighting its focus on detailed diagnosis and care planning.
All-in-One Nursing Care Planning Resource – E-Book: Medical-Surgical, Pediatric, Maternity, and Psychiatric-Mental Health
This comprehensive e-book includes over 100 care plans spanning medical-surgical, maternity/OB, pediatrics, and psychiatric and mental health nursing. Its interprofessional “patient problems” focus familiarizes you with effective patient communication.
References and Sources
List of original article references/sources if available, or general citation if not.