Crafting effective nursing care plans is a cornerstone of exceptional patient care. For nurses and nursing students alike, understanding how to develop these plans, especially focusing on priority nursing diagnoses, is crucial. This guide will provide an in-depth exploration of nursing care plans, emphasizing the critical role of prioritizing nursing diagnoses to ensure patient needs are met efficiently and effectively.
Understanding Nursing Care Plans
A nursing care plan (NCP) is a systematic and dynamic tool that guides nurses in providing patient-centered care. It’s a formal, written document that outlines a patient’s current health status, identifies potential health problems or risks, and details the nursing interventions required to address these needs and achieve desired patient outcomes. Think of it as a roadmap for nursing care, ensuring consistency, quality, and individualized attention for each patient.
The nursing care planning process is not a one-time event; it’s a continuous cycle. It begins upon patient admission and is regularly updated as the patient’s condition changes and as the effectiveness of interventions is evaluated. This ongoing adaptation ensures that the care plan remains relevant and responsive to the patient’s evolving needs. At its heart, nursing care planning is about delivering personalized care, which is the gold standard of modern nursing practice.
Formal vs. Informal Nursing Care Plans
Nursing care plans can be broadly classified into two types:
- Informal Nursing Care Plans: These are mental strategies, existing in the nurse’s mind as a quick action plan. While useful for experienced nurses in routine situations, they lack the detailed structure and communication benefits of formal plans.
- Formal Nursing Care Plans: These are documented guides, either written or electronic, that meticulously organize patient information and care strategies. Formal plans are essential for ensuring comprehensive, consistent, and communicated care.
Formal care plans are further divided into:
- Standardized Care Plans: These are pre-written plans addressing common needs for patient groups with similar diagnoses. They ensure a baseline of consistent care and streamline nursing workflow by eliminating the need to reinvent the wheel for routine care activities. However, they serve as a starting point and often require individualization.
- Individualized Care Plans: These are tailored plans, adapted from standardized plans or created from scratch, to meet the specific and unique needs of each patient. They account for individual patient preferences, strengths, and goals, promoting holistic and patient-centered care. Individualized plans are vital for addressing complex patient situations or needs not covered by standardized protocols.
The Power of Individualized Care Plans
Individualized care plans are not just best practice; they are increasingly essential in today’s healthcare landscape. They contribute to:
- Enhanced Patient Satisfaction: When patients perceive their care as personalized and responsive to their specific needs, their satisfaction increases significantly. This is crucial as patient satisfaction is increasingly used as a key indicator of healthcare quality.
- Improved Holistic Care: Individualized plans allow nurses to consider the patient in their entirety – physical, psychological, social, and spiritual needs – leading to more comprehensive and effective care.
- Better Adherence to Treatment: When patients are involved in developing their care plans and feel understood, they are more likely to actively participate in their treatment and follow recommendations.
Tips for Individualizing Nursing Care Plans: (This section could be expanded with bullet points listing concrete tips)
Objectives of Nursing Care Plans
The objectives of developing and implementing nursing care plans are multifaceted and contribute significantly to quality patient care:
- Promote Evidence-Based Practice: Care plans encourage nurses to utilize current research and best practices in their care delivery, ensuring patients receive the most effective treatments and interventions.
- Support Holistic Patient Care: By considering the patient’s physical, psychological, social, and spiritual dimensions, care plans facilitate comprehensive care that addresses the whole person, not just the illness.
- Establish Care Pathways and Bundles: Care plans can serve as the foundation for developing standardized care pathways (multidisciplinary consensus on care standards and expected outcomes) and care bundles (sets of evidence-based practices for specific conditions).
- Clearly Define Goals and Outcomes: The care planning process necessitates the identification of specific, measurable, achievable, relevant, and time-bound (SMART) goals and expected outcomes, providing direction and a means to evaluate progress.
- Enhance Communication and Documentation: Care plans serve as a central communication tool for the healthcare team, ensuring everyone is informed and working towards shared goals. They also provide a structured format for documenting care provided.
- Measure and Improve Nursing Care Quality: By outlining expected outcomes and providing a framework for evaluation, care plans enable the monitoring and continuous improvement of nursing care effectiveness.
Purposes and Importance of Nursing Care Plans
Nursing care plans are not merely administrative documents; they serve vital purposes that directly impact patient care and the nursing profession:
- Defines the Nurse’s Unique Role: Care plans highlight the autonomous and crucial role of nurses in addressing patients’ overall well-being, going beyond simply following physician orders. They emphasize independent nursing interventions and critical thinking.
- Provides Direction for Individualized Care: A care plan acts as a personalized roadmap, guiding nurses to deliver care tailored to each patient’s unique needs. It encourages critical thinking in selecting and implementing appropriate interventions.
- Ensures Continuity of Care: Care plans facilitate consistent care delivery across different nursing shifts and departments. All nurses can access the plan and provide the same quality and type of interventions, maximizing treatment benefits for the patient.
- Facilitates Coordinated Care: By making patient needs and planned actions transparent, care plans ensure all members of the healthcare team are aligned and working collaboratively, preventing gaps and overlaps in care.
- Serves as Legal Documentation: Care plans are integral parts of the patient’s medical record. Accurate and thorough documentation within the care plan provides evidence of the care provided, which is vital for legal and quality assurance purposes. If care isn’t documented, it’s legally considered not to have been provided.
- Guides Staff Assignment: In situations where patients require specialized skills, care plans help in matching patient needs with appropriately skilled nursing staff.
- Monitors Patient Progress: Care plans provide a benchmark for tracking patient progress against expected outcomes. This monitoring allows for timely adjustments to the plan as needed, ensuring care remains effective.
- Supports Reimbursement: Insurance companies often review medical records, including care plans, to determine appropriate reimbursement for hospital care. Well-documented care plans can justify the necessity and scope of nursing care provided.
- Empowers Patients and Defines Patient Goals: Involving patients in the development of their care plans fosters a sense of ownership and collaboration. It clarifies patient goals and ensures care is aligned with their preferences and values.
Key Components of a Nursing Care Plan
A comprehensive nursing care plan typically includes several essential components, working together to provide a structured approach to patient care. Crucially, priority nursing diagnoses are at the heart of this structure, guiding the entire care planning process. The core components are:
- Nursing Diagnoses: These are clinical judgments about individual, family, or community responses to actual and potential health problems or life processes. They provide the foundation for the care plan, identifying the patient’s specific needs that nursing interventions can address. Prioritizing these diagnoses is the first critical step.
- Patient Problems (or Client Problems): This is a broader term encompassing health issues that may be medical diagnoses, nursing diagnoses, or collaborative problems.
- Desired Outcomes (Goals): These are specific, measurable, achievable, relevant, and time-bound statements describing the intended changes in the patient’s health status as a result of nursing care. Outcomes are directly linked to the nursing diagnoses.
- Nursing Interventions: These are the actions that nurses will implement to achieve the desired patient outcomes. Interventions should be evidence-based, patient-specific, and designed to address the identified nursing diagnoses.
- Rationales: These are the scientific reasons or evidence that support the chosen nursing interventions. Rationales are particularly important in student care plans to solidify understanding of the link between interventions and patient needs.
- Evaluation: This is the process of assessing the patient’s progress towards achieving the desired outcomes. Evaluation determines the effectiveness of the care plan and informs any necessary revisions.
Care Plan Formats: Structuring the Information
Nursing care plans can be organized in various formats, often using a columnar approach for clarity and ease of use. Common formats include:
-
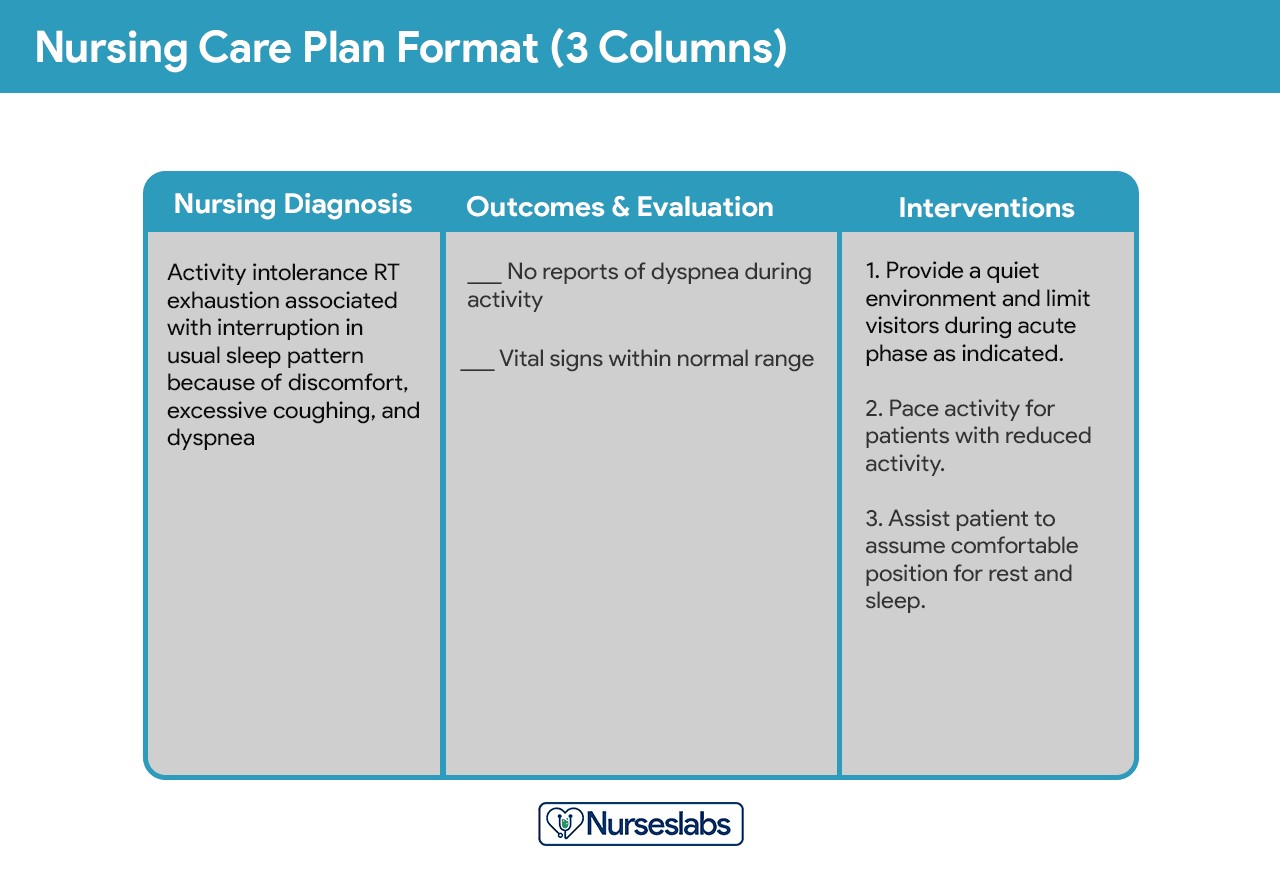
Three-Column Format: This format typically includes columns for:
- Nursing Diagnoses
- Desired Outcomes and Evaluation
- Nursing Interventions
This format is concise and integrates outcome evaluation directly with the goals.
-
Four-Column Format: This more detailed format separates outcomes and evaluation, providing distinct columns for:
- Nursing Diagnoses
- Goals and Outcomes
- Nursing Interventions
- Evaluation
This format offers greater clarity by separating the goal setting from the evaluation phase.
-
Five-Column Format: Some agencies or educational programs utilize a five-column format, adding a column for:
- Assessment Cues
- Nursing Diagnoses
- Desired Outcomes
- Nursing Interventions
- Evaluation
This format emphasizes the initial assessment data that leads to the nursing diagnoses.
Downloadable Templates: Printable Nursing Care Plan Templates and Formats
Student Care Plans: A Detailed Learning Tool
Student care plans are typically more comprehensive than those used by practicing nurses. They serve as a valuable learning exercise, requiring students to delve deeper into the rationale behind each intervention. A key feature of student care plans is often an additional column for “Rationales” or “Scientific Explanations,” placed after the nursing interventions. These rationales require students to articulate the scientific principles underpinning their chosen interventions, solidifying their understanding of the physiological and psychological basis of nursing care.
Step-by-Step Guide to Writing a Nursing Care Plan
Creating a robust nursing care plan involves a structured, multi-step process. Prioritizing nursing diagnoses is woven throughout these steps, ensuring that the most critical patient needs are addressed first.
Step 1: Comprehensive Data Collection and Assessment
The foundation of any effective care plan is a thorough patient assessment. This initial step involves gathering comprehensive data about the patient’s health status using various methods:
- Physical Assessment: Hands-on examination to evaluate the patient’s physical condition.
- Health History: Collecting information about past and present illnesses, surgeries, medications, allergies, and family history.
- Patient Interview: Directly communicating with the patient to understand their perspective, symptoms, concerns, and goals.
- Medical Records Review: Examining existing medical documentation for relevant health information.
- Diagnostic Studies: Reviewing results of laboratory tests, imaging studies, and other diagnostic procedures.
The goal of data collection is to create a complete patient database encompassing all relevant health information. This database allows the nurse to identify patterns, risk factors, and defining characteristics that will be used to formulate nursing diagnoses. Specific assessment formats may be required by agencies or nursing schools to ensure consistency and comprehensiveness.
Critical thinking is paramount in patient assessment. Nurses must integrate knowledge from various scientific disciplines and professional guidelines to accurately evaluate patient data. This process is crucial for complex clinical decision-making, ensuring that patient healthcare needs are effectively identified and addressed in a supportive and informed environment.
Step 2: Data Analysis and Organization: Identifying Patterns
Once data is collected, the next step is to analyze and organize it. This involves:
- Clustering Data: Grouping related assessment findings together. For example, signs and symptoms related to respiratory distress might be clustered together.
- Identifying Patterns: Looking for trends and relationships within the clustered data. These patterns help to pinpoint potential health problems and form the basis for nursing diagnoses.
This step bridges the gap between raw data and actionable nursing diagnoses. It sets the stage for formulating diagnoses and prioritizing them effectively.
Step 3: Formulating Nursing Diagnoses: Naming the Needs
Nursing diagnoses are the core of the care plan. They are concise statements that:
- Identify specific patient needs and responses to health conditions.
- Focus on problems that nurses can independently address through nursing interventions.
- Provide a standardized language for communication among healthcare professionals.
Accurately formulating nursing diagnoses is essential. Resources like Nursing Diagnosis (NDx): Complete Guide and List can provide detailed guidance and examples.
This is where the concept of “priority nursing diagnosis” becomes central. After identifying all relevant nursing diagnoses, the nurse must determine which diagnoses require immediate attention and which can be addressed later.
Step 4: Setting Priorities: Addressing the Most Critical Needs First
Setting priorities is a crucial step in care planning. It involves ranking nursing diagnoses in order of importance to the patient’s immediate well-being. This prioritization guides the sequence of nursing interventions, ensuring that the most critical needs are addressed first.
Diagnoses are typically categorized by priority level:
- High Priority: Life-threatening problems or those that could cause significant harm if left untreated. These diagnoses require immediate nursing attention. Examples include compromised airway, breathing, or circulation.
- Medium Priority: Problems that are not immediately life-threatening but could cause significant discomfort, complications, or delays in recovery if not addressed in a timely manner. Examples include acute pain, risk of infection, or impaired mobility.
- Low Priority: Problems that are related to the patient’s overall well-being and long-term health, but do not pose an immediate threat. Examples include knowledge deficit, health maintenance, or altered self-esteem.
Maslow’s Hierarchy of Needs is a widely used framework for prioritizing nursing diagnoses. Developed by Abraham Maslow, this hierarchy organizes human needs into five levels, from most basic to most complex:
-
Physiological Needs (Basic Survival Needs): These are the most fundamental needs for survival. They include:
- Nutrition: Water, food
- Elimination: Toileting
- Airway, Breathing, Circulation (ABCs): Suctioning, oxygen administration, cardiac monitoring, blood pressure management
- Sleep
- Sex
- Shelter
- Exercise
Physiological needs are always the highest priority. Diagnoses related to these needs (e.g., Impaired Gas Exchange, Deficient Fluid Volume) must be addressed immediately.
-
Safety and Security Needs: Once physiological needs are met, safety and security become the next priority. These include:
- Injury Prevention: Side rails, call lights, hand hygiene, isolation precautions, suicide precautions, fall precautions, car seats, helmets, seat belts
- Fostering Trust and Safety: Therapeutic relationship, patient education on modifiable risk factors (e.g., stroke, heart disease)
Diagnoses related to safety (e.g., Risk for Falls, Risk for Infection) are also high priority, especially in vulnerable patient populations.
-
Love and Belonging Needs: After physiological and safety needs are addressed, the focus shifts to social and emotional needs:
- Supportive Relationships: Fostering positive relationships, addressing social isolation (e.g., bullying)
- Communication: Active listening, therapeutic communication, addressing sexual intimacy
Diagnoses related to love and belonging (e.g., Social Isolation, Impaired Social Interaction) are medium to low priority, depending on the patient’s overall situation.
-
Self-Esteem Needs: These relate to feelings of confidence, worth, and achievement:
- Acceptance in Community/Workforce
- Personal Achievement
- Sense of Control/Empowerment
- Acceptance of Physical Appearance
Diagnoses related to self-esteem (e.g., Disturbed Body Image, Chronic Low Self-Esteem) are typically medium to low priority.
-
Self-Actualization Needs: This is the highest level of need, relating to personal growth, fulfillment, and reaching one’s full potential:
- Empowering Environment
- Spiritual Growth
- Recognizing Others’ Perspectives
- Reaching Maximum Potential
Diagnoses related to self-actualization (e.g., Readiness for Enhanced Spiritual Well-being) are generally low priority in acute care settings but may become more relevant in long-term care or rehabilitation.
Factors Influencing Priority Setting:
- Patient Values and Beliefs: Patient preferences and cultural values should be considered when prioritizing care.
- Available Resources: Realistic resource availability (staffing, equipment, time) must be factored into prioritization.
- Urgency of the Problem: Life-threatening or rapidly deteriorating conditions take precedence.
- Medical Treatment Plan: Nursing priorities should align with the overall medical plan of care.
Patient Involvement: Whenever possible, involve the patient in the priority-setting process. This enhances patient cooperation and ensures that care aligns with their priorities.
Step 5: Establishing Client Goals and Desired Outcomes: Defining Success
Once priorities are set, the next step is to establish goals and desired outcomes for each priority nursing diagnosis. Goals are broad statements describing the overall aim of nursing care, while desired outcomes are specific, measurable criteria that indicate goal achievement.
Goals and desired outcomes are crucial because they:
- Provide direction for nursing interventions.
- Serve as criteria for evaluating patient progress.
- Enable nurses and patients to track problem resolution.
- Motivate patients and nurses by providing a sense of accomplishment.
Typically, one overall goal is established for each nursing diagnosis. The terms “goal outcomes” and “expected outcomes” are often used interchangeably.
SMART Goal Framework: Goals and outcomes should ideally be SMART:
- Specific: Clearly defined and focused.
- Measurable: Quantifiable and able to be tracked.
- Attainable: Realistic and achievable for the patient.
- Relevant: Aligned with patient needs and priorities.
- Time-bound: With a defined timeframe for achievement.
REEPIG Standards: For high-quality care plans, Hogston (2011) suggests using the REEPIG standards:
- Realistic: Achievable given available resources.
- Explicitly Stated: Clear and unambiguous, leaving no room for misinterpretation.
- Evidence-Based: Supported by research and best practices.
- Prioritized: Addressing the most urgent problems first.
- Involve Patient and Team: Collaborative, involving the patient and multidisciplinary team members.
- Goal-Centered: Directly contributing to goal achievement.
Short-Term and Long-Term Goals:
- Short-Term Goals: Outcomes achievable in a short period (hours to days), common in acute care settings focusing on immediate needs.
- Long-Term Goals: Outcomes requiring longer timeframes (weeks to months), typical for chronic conditions, home care, or rehabilitation settings. Discharge planning often involves setting long-term goals.
Components of Goals and Desired Outcomes: A well-written outcome statement usually includes:
-
Subject: The patient (often implied).
-
Verb: Action the patient will perform (e.g., “will demonstrate,” “will verbalize”).
-
Conditions/Modifiers: Circumstances under which the behavior will occur (e.g., “using proper technique,” “with assistance”).
-
Criterion of Performance: Standard for evaluation (optional, but enhances measurability).
Tips for Writing Goals and Desired Outcomes:
- Focus on patient responses, not nurse activities. Start with “Client will…”
- Focus on what the patient will do, not what the nurse hopes to achieve.
- Use observable, measurable terms. Avoid vague language.
- Ensure outcomes are realistic given patient resources and timeframe.
- Ensure goals are compatible with other therapies.
- Each goal should be derived from only one nursing diagnosis for clear evaluation.
- Ensure goals are important and valued by the patient to promote cooperation.
Step 6: Selecting Nursing Interventions: Actionable Strategies
Nursing interventions are the specific actions nurses will take to help patients achieve their goals and desired outcomes. Interventions should be:
- Directly linked to the etiology of the nursing diagnosis. They aim to reduce or eliminate the factors contributing to the problem. For risk diagnoses, interventions focus on reducing risk factors.
- Evidence-based and supported by research or best practices.
- Patient-centered and tailored to individual needs, preferences, and values.
Nursing interventions are planned during the planning phase of the nursing process but are actually implemented during the implementation phase.
Types of Nursing Interventions:
-
Independent Nursing Interventions: Actions nurses are licensed to initiate based on their own judgment and skills. Examples: patient education, emotional support, comfort measures, ongoing assessment, referrals.
-
Dependent Nursing Interventions: Actions carried out under physician orders or supervision. Examples: medication administration, IV therapy, diagnostic tests, dietary orders, activity orders. Nurses still play a crucial role in assessment and patient education related to dependent interventions.
-
Collaborative Interventions: Actions carried out in coordination with other healthcare team members (physicians, social workers, dietitians, therapists). These interventions require interprofessional consultation and teamwork.
Criteria for Selecting Nursing Interventions:
- Safe and appropriate for patient’s age, health, and condition.
- Achievable with available resources and time.
- Aligned with patient’s values, culture, and beliefs.
- Compatible with other therapies.
- Based on nursing knowledge, experience, and relevant scientific principles.
Tips for Writing Nursing Interventions:
- Date and sign the plan for accountability and tracking.
- Be specific and clear. Start with an action verb describing what the nurse will do. Include qualifiers (how, when, where, frequency, amount) for clarity. Examples: “Educate parents on…”, “Assess urine for…”.
- Use only accepted abbreviations within the institution.
Step 7: Providing Rationales: Explaining the “Why”
Rationales (scientific explanations) are included primarily in student care plans. They explain the scientific basis for each nursing intervention, linking interventions to underlying pathophysiology and psychological principles. Rationales are not typically included in care plans used by practicing nurses but are invaluable for student learning.
Step 8: Evaluation: Assessing Effectiveness and Making Adjustments
Evaluation is a critical, ongoing process to determine the effectiveness of the nursing care plan. It involves:
- Assessing patient progress towards achieving desired outcomes.
- Comparing actual patient outcomes to expected outcomes.
- Determining the effectiveness of nursing interventions.
- Deciding whether to continue, modify, or terminate interventions.
Evaluation is integral to the nursing process, as it provides feedback to refine the care plan and ensure it remains effective.
Step 9: Documentation: Putting it on Paper (or Screen)
The final step is documenting the care plan according to agency policy. The care plan becomes part of the patient’s permanent medical record, ensuring communication and continuity of care. Different nursing programs and healthcare agencies may have specific care plan formats, but most follow the steps of the nursing process.
Nursing Care Plan Examples: A Comprehensive List
This section of the original article provides a valuable list of nursing care plans categorized by medical specialties. This list could be retained and even expanded upon, as it offers a practical resource for nurses seeking examples of care plans for various conditions. It demonstrates the breadth of conditions for which nursing care plans are relevant. (The detailed lists of care plans from the original article would be included here).
Recommended Resources
(The recommended resources section from the original article, including book recommendations and affiliate links, would be included here).
References and Sources
(The references and sources section from the original article would be included here).
By prioritizing nursing diagnoses within a well-structured care plan, nurses can ensure they are addressing the most critical patient needs first, providing focused, effective, and patient-centered care. Mastering the art of nursing care planning, with a strong emphasis on priority setting, is essential for all nurses committed to excellence in patient care.