Crafting effective nursing care plans is a cornerstone of excellent patient care. It’s a systematic process that involves identifying patient needs, formulating nursing diagnoses, setting goals, and planning interventions to achieve desired outcomes. For nursing students and practicing professionals alike, mastering this skill is crucial. Fortunately, numerous resources are available to guide and enhance your understanding of nursing diagnosis and care planning, and books remain an invaluable tool in this learning journey.
This guide will explore the significance of nursing care plans, delve into their components, and highlight the best books available to help you excel in creating comprehensive and patient-centered care plans. Whether you are a student just beginning your nursing education or a seasoned nurse looking to refine your skills, understanding and utilizing the right resources, particularly books focused on nursing diagnosis and care plans, can significantly elevate your practice.
Understanding Nursing Care Plans
A nursing care plan (NCP) is a formalized, written document that outlines the individualized care for a patient. It serves as a blueprint for nursing actions, ensuring consistent, quality care and effective communication among healthcare team members. Without well-structured care plans, patient care can become fragmented, potentially compromising patient outcomes.
Nursing care planning is a dynamic process, starting at patient admission and continuously evolving as the patient’s condition changes. It’s the bedrock of patient-centered care, emphasizing individualized approaches based on each patient’s unique needs and circumstances.
Types of Nursing Care Plans: Formal vs. Informal, Standardized vs. Individualized
Nursing care plans can be broadly categorized as informal or formal. An informal care plan is a mental strategy, existing in the nurse’s mind, guiding immediate actions. In contrast, a formal care plan is a written or electronic document, providing a structured guide to patient care information.
Formal care plans are further divided into standardized and individualized plans. Standardized care plans are pre-written guides for patients with common needs, ensuring consistent care for routine conditions. Individualized care plans are tailored to meet the specific and unique needs of a particular patient, adapting standardized plans or creating new strategies where necessary.
Standardized Care Plans: Efficiency and Consistency
Standardized care plans are developed by healthcare agencies to provide consistent care for patients with similar conditions. They ensure a minimum standard of care is met efficiently, saving nurses time by eliminating the need to create plans from scratch for common patient needs.
It’s important to remember that standardized care plans are a starting point. They are not designed to address every patient’s unique situation, and often require adaptation to become truly patient-centered. Many resources, including books on nursing diagnosis and care plans, offer standardized care plans as templates, emphasizing their role as frameworks for individualization.
Individualized Care Plans: Patient-Centered Approach
An individualized care plan takes a standardized plan and modifies it to address the specific needs and goals of an individual patient. This personalization is crucial for providing holistic care, considering the patient’s unique strengths, preferences, and circumstances.
Individualized care plans are directly linked to improved patient satisfaction. When patients feel their care is tailored to them, they are more likely to feel valued and understood, leading to a more positive healthcare experience. In today’s healthcare landscape, where patient satisfaction is a key indicator of quality, individualized care planning is paramount.
Tips for Individualizing Nursing Care Plans: (This section could be expanded with specific examples from Nursing Diagnosis And Care Plans Books)
Objectives of Nursing Care Plans
The primary objectives of nursing care plans are multifaceted:
- Promote Evidence-Based Care: Care plans encourage the use of current best practices and research findings in patient care.
- Support Holistic Care: They ensure consideration of the patient’s physical, psychological, social, and spiritual needs, promoting a whole-person approach to care.
- Establish Care Pathways and Bundles: Care plans can facilitate the development of standardized care pathways for consistent treatment and care bundles for specific conditions based on best practices.
- Define Goals and Expected Outcomes: They clearly identify specific, measurable goals and outcomes to guide care and evaluate progress.
- Enhance Communication and Documentation: Care plans improve communication among healthcare providers and provide a documented record of planned and delivered care.
- Measure Nursing Care Effectiveness: They provide a framework for evaluating the effectiveness of nursing interventions and adjusting care as needed.
Purposes of Nursing Care Plans: Why They Matter
Nursing care plans serve several vital purposes in patient care and nursing practice:
- Define the Nurse’s Role: Care plans highlight the unique, independent role of nurses in addressing patients’ overall health and well-being, beyond simply following physician orders.
- Provide Direction for Individualized Care: They act as a roadmap for patient care, guiding nurses to think critically and tailor interventions to individual needs.
- Ensure Continuity of Care: Care plans enable consistent care across different shifts and departments, ensuring patients receive seamless and beneficial treatment.
- Coordinate Care: They facilitate communication and collaboration among the healthcare team, preventing gaps in care and ensuring everyone is working towards the same goals.
- Documentation and Legal Record: Care plans document the planned care, observations, nursing actions, and patient/family instructions. Proper documentation is essential; if care isn’t documented, it’s legally considered not provided.
- Guide Staff Assignment: Care plans can help in assigning staff with appropriate skills to patients with specific needs.
- Monitor Patient Progress: They provide a mechanism to track patient progress and adjust the care plan in response to changes in health status.
- Support Reimbursement: Insurance companies often use medical records, including care plans, to determine reimbursement for hospital care.
- Define Patient Goals and Engagement: Care plans involve patients in their care, promoting understanding, cooperation, and a sense of ownership in their treatment journey.
Components of a Nursing Care Plan
A comprehensive nursing care plan typically includes several key components:
- Nursing Diagnoses: Identifies the patient’s health problems or potential risks that nurses are qualified and licensed to treat.
- Patient Problems/Needs: A broader description of the patient’s health issues and care requirements.
- Expected Outcomes/Goals: Specific, measurable, achievable, relevant, and time-bound (SMART) statements describing the desired changes in patient health status.
- Nursing Interventions: Actions nurses will take to achieve the expected outcomes.
- Rationales: Scientific principles or evidence supporting the chosen nursing interventions.
- Evaluation: Assessment of the patient’s progress toward achieving goals and the effectiveness of the care plan.
These components are often organized into structured formats to facilitate clarity and ease of use. Books on nursing diagnosis and care plans provide detailed explanations of each component and offer examples to guide students and professionals in their development.
Care Plan Formats: Structuring for Clarity
Nursing care plans are often formatted in columns to organize information logically. Common formats include three-column and four-column plans.
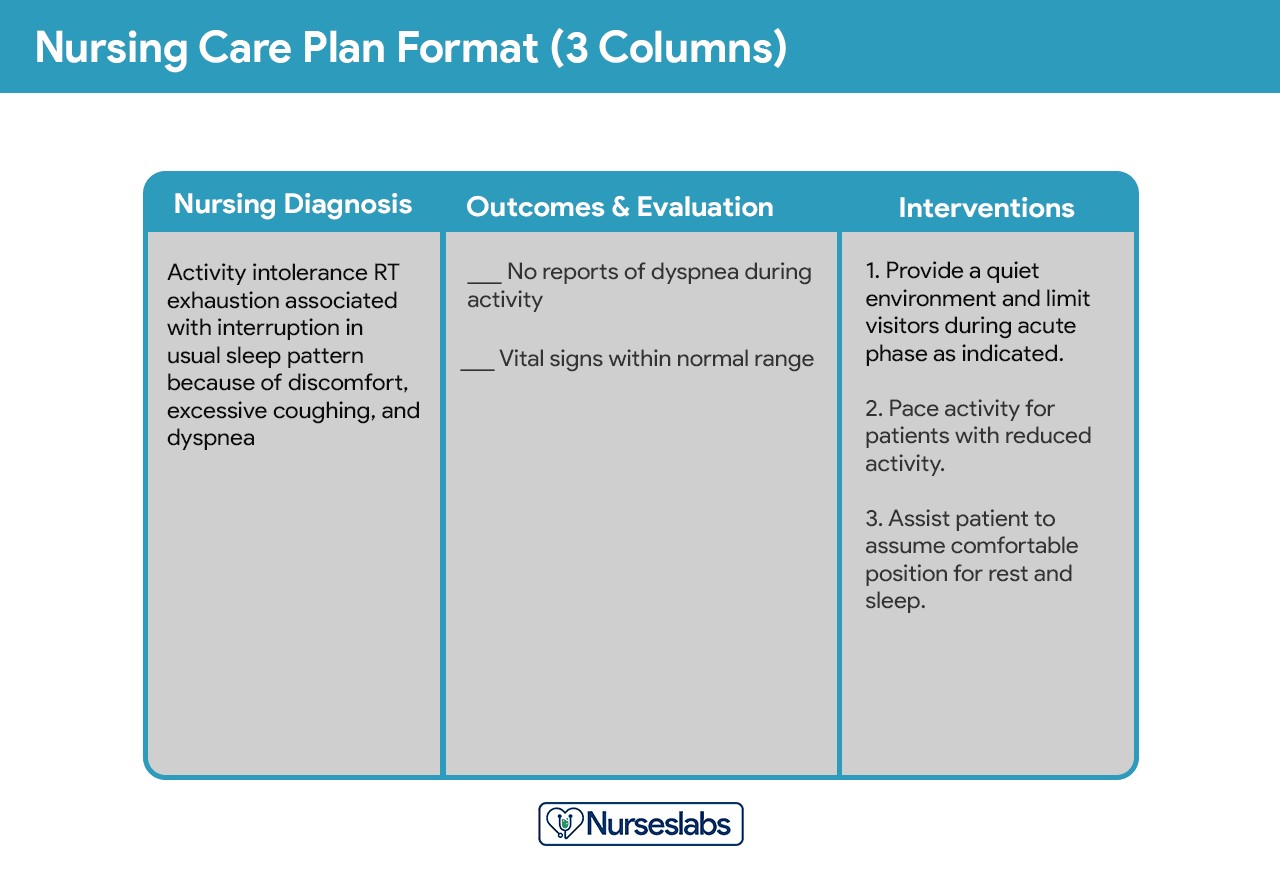
Three-Column Format
The three-column format typically includes:
- Nursing Diagnosis: The identified nursing diagnosis.
- Outcomes and Evaluation: Desired patient outcomes and space for evaluation of goal achievement.
- Interventions: Nursing actions to achieve the outcomes.
This format streamlines the plan, combining outcomes and evaluation into a single column.
Three-column nursing care plan format
Four-Column Format
The four-column format provides more detailed organization:
- Nursing Diagnosis: The identified nursing diagnosis.
- Goals and Outcomes: Specific, measurable goals and expected outcomes for the patient.
- Interventions: Nursing actions planned to achieve the goals and outcomes.
- Evaluation: Assessment of patient progress and care plan effectiveness.
This format clearly separates goals/outcomes from evaluation, offering a more granular view of the care planning process.
Four-column nursing care plan template
Download Printable Nursing Care Plan Templates and Formats
Student Care Plans: Detailed Learning Tools
Student care plans are typically more detailed and comprehensive than those used by practicing nurses. This is because they serve as a crucial learning tool for nursing students, helping them to develop critical thinking and care planning skills.
Student nursing care plans are more detailed.
Often, student care plans are handwritten and include an additional column for “Rationales” or “Scientific Explanation.” These rationales require students to articulate the scientific basis for their chosen interventions, reinforcing their understanding of the underlying principles of nursing care. Many nursing diagnosis and care plans books are specifically designed for students, providing detailed rationales and examples tailored to the learning process.
Writing a Nursing Care Plan: A Step-by-Step Guide
Developing a robust nursing care plan involves a systematic, multi-step process. Here’s a breakdown of the key steps:
Step 1: Data Collection or Assessment
The first step is comprehensive data collection. This involves gathering patient information through various methods, including:
- Physical Assessment: Hands-on examination of the patient’s physical condition.
- Health History: Obtaining information about the patient’s past and present health status, including medical history, symptoms, and treatments.
- Interviews: Direct communication with the patient and/or family to gather subjective data.
- Medical Records Review: Examining existing medical documentation for relevant information.
- Diagnostic Studies: Reviewing results of laboratory tests, imaging, and other diagnostic procedures.
The goal of data collection is to create a complete patient database, encompassing all relevant health information. This information is then used to identify related or risk factors and defining characteristics that form the basis for nursing diagnoses. Some institutions and nursing programs provide specific assessment formats to guide this process.
Critical thinking is paramount in patient assessment. It involves integrating knowledge from various sciences and professional guidelines to effectively evaluate patient needs. This process is vital for complex clinical decision-making, aiming to accurately identify patient healthcare needs within a supportive and informative environment.
Step 2: Data Analysis and Organization
Once data is collected, the next step is analysis and organization. This involves:
- Analyzing Data: Examining the collected data to identify patterns, trends, and significant findings.
- Clustering Data: Grouping related data points together to identify potential problem areas.
- Organizing Data: Structuring the data in a logical manner to facilitate the formulation of nursing diagnoses, priorities, and desired outcomes.
This step bridges the gap between raw data and actionable nursing diagnoses.
Step 3: Formulating Nursing Diagnoses
Nursing diagnoses are standardized statements that describe a patient’s health problems or potential risks that nurses can independently address. They provide a common language for nurses to communicate about patient needs. Nursing diagnoses focus on patient responses to health conditions and life processes.
For a detailed guide on formulating nursing diagnoses, resources like nursing diagnosis and care plans books are invaluable. Nursing Diagnosis (NDx): Complete Guide and List provides a comprehensive overview of this crucial step.
Step 4: Setting Priorities
Setting priorities involves ranking nursing diagnoses in order of importance. This ensures that the most critical patient needs are addressed first. Prioritization is a collaborative process involving the nurse and the patient, whenever possible. Diagnoses are often categorized as high, medium, or low priority. Life-threatening problems always take top priority.
Maslow’s Hierarchy of Needs is a useful framework for setting priorities. This hierarchy, developed by Abraham Maslow, organizes human needs into a pyramid, with basic physiological needs at the base and self-actualization at the peak. Physiological and safety needs must be met before higher-level needs can be addressed.
Maslow’s Hierarchy of Needs:
-
Basic Physiological Needs: These are the most fundamental needs for survival, including:
- Nutrition (water, food)
- Elimination (toileting)
- Airway, Breathing, Circulation (ABCs) (suction, oxygen, pulse, cardiac monitoring, blood pressure)
- Sleep
- Sex
- Shelter
- Exercise
-
Safety and Security Needs: Once physiological needs are met, safety and security become paramount. These include:
- Injury prevention (side rails, call lights, hand hygiene, isolation, suicide precautions, fall precautions, car seats, helmets, seat belts)
- Fostering a climate of trust and safety (therapeutic relationships)
- Patient education (modifiable risk factors for stroke, heart disease)
-
Love and Belonging Needs: These involve social connection and acceptance:
- Foster supportive relationships
- Methods to avoid social isolation (addressing bullying)
- Active listening, therapeutic communication
- Sexual intimacy
-
Self-Esteem Needs: Relate to feelings of self-worth and accomplishment:
- Acceptance in the community, workforce
- Personal achievement
- Sense of control or empowerment
- Accepting one’s physical appearance
-
Self-Actualization Needs: The highest level of needs, focused on personal growth and fulfillment:
- Empowering environment
- Spiritual growth
- Ability to recognize others’ perspectives
- Reaching one’s maximum potential
*Virginia Henderson’s 14 Needs as applied to Maslow’s Hierarchy of Needs. Learn more about it here. *
Patient values, beliefs, available resources, and urgency all influence priority setting. Patient involvement in this process enhances cooperation and adherence to the care plan.
Step 5: Establishing Client Goals and Desired Outcomes
After prioritizing diagnoses, the nurse and patient collaborate to set goals for each priority. Goals or desired outcomes describe the intended results of nursing interventions. They provide direction for planning interventions, serve as evaluation criteria, and motivate both the patient and nurse.
Examples of goals and desired outcomes. Notice how they’re formatted and written.
One overall goal is typically established for each nursing diagnosis. Goals should be SMART:
- Specific: Clearly defined and focused.
- Measurable: Quantifiable and able to be tracked.
- Attainable: Achievable given the patient’s circumstances and resources.
- Realistic: Relevant to the patient’s needs and priorities.
- Time-Oriented: With a defined timeframe for achievement.
The REEPIG standards also provide guidance for high-quality goal setting:
- Realistic: Achievable with available resources.
- Explicitly stated: Clearly and unambiguously written.
- Evidence-based: Supported by research and best practices.
- Prioritized: Addressing the most urgent problems first.
- Involve: Including the patient and multidisciplinary team members.
- Goal-centered: Focused on achieving the desired outcomes.
Short-Term and Long-Term Goals
Goals can be short-term or long-term. Short-term goals are achievable within hours or days, common in acute care settings. Long-term goals are achieved over weeks or months, often used for chronic conditions or home care. Discharge planning involves setting long-term goals to ensure continued recovery and problem resolution.
Components of Goals and Desired Outcomes
Goal statements typically include four components:
- Subject: The patient or part of the patient (often implied).
- Verb: Action the patient will perform.
- Conditions/Modifiers: Circumstances under which the behavior will be performed.
- Criterion of Desired Performance: Standard for evaluating performance (optional).
Components of goals and desired outcomes in a nursing care plan.
Tips for Writing Goals and Desired Outcomes:
- Focus on patient responses, not nurse activities. Start with “Client will…”
- Focus on what the patient will do, not nurse hopes.
- Use observable, measurable terms. Avoid vague language.
- Ensure outcomes are realistic given patient resources and timeframe.
- Ensure compatibility with other therapies.
- Each goal should relate to only one nursing diagnosis.
- Ensure goals are important and valued by the patient.
Step 6: Selecting Nursing Interventions
Nursing interventions are the specific actions nurses will perform to help patients achieve their goals. Interventions should address the etiology of the nursing diagnosis or reduce risk factors for risk diagnoses. Interventions are planned in this step but implemented in the implementation phase of the nursing process.
Types of Nursing Interventions
Nursing interventions can be independent, dependent, or collaborative:
Types of nursing interventions in a care plan.
-
Independent Interventions: Actions nurses are licensed to initiate based on their own judgment, such as:
- Ongoing assessment
- Emotional support
- Comfort measures
- Teaching
- Physical care
- Referrals
-
Dependent Interventions: Actions carried out under physician orders or supervision, including:
- Medication administration
- IV therapy
- Diagnostic tests
- Treatments
- Diet orders
- Activity/rest orders
-
Collaborative Interventions: Actions carried out in collaboration with other healthcare team members, such as:
- Physical therapy
- Dietary consults
- Social work referrals
Nursing interventions should be:
- Safe and appropriate for the patient’s age, health, and condition.
- Achievable with available resources and time.
- Consistent with patient values, culture, and beliefs.
- Compatible with other therapies.
- Based on nursing knowledge and evidence.
Tips for Writing Nursing Interventions:
- Date and sign the plan for accountability and future reference.
- Be specific and clear, starting with an action verb. Include qualifiers (how, when, where, frequency, amount). Examples: “Educate parents on temperature taking and when to notify changes,” “Assess urine for color, amount, odor, and turbidity.”
- Use only accepted abbreviations.
Step 7: Providing Rationales
Rationales are scientific explanations for why specific interventions are chosen. They explain the underlying principles supporting the intervention.
Rationales are typically included in student care plans to enhance learning and connect interventions to scientific principles. They are not always included in care plans used by practicing nurses. Books focused on nursing diagnosis and care plans often provide rationales to aid understanding.
Step 8: Evaluation
Evaluation is an ongoing process of assessing patient progress toward goals and the effectiveness of the care plan. It’s a crucial step in the nursing process, determining whether to continue, modify, or terminate interventions.
Step 9: Documentation
The completed care plan is documented according to institutional policy and becomes part of the patient’s medical record. Different nursing programs and institutions may have specific care plan formats. Most formats are designed to guide users through the steps of the nursing process.
Nursing Care Plan Resources: Books for Success
To further enhance your skills in nursing diagnosis and care planning, consider utilizing dedicated books. These resources offer in-depth guidance, examples, and templates to support your learning and practice. Here are some recommended books, particularly valuable for their focus on nursing diagnosis and care plans:
Recommended Nursing Diagnosis and Care Plan Books
These books are highly recommended for nursing students and professionals seeking to master care planning. They provide comprehensive information, evidence-based approaches, and practical guidance.
Ackley and Ladwig’s Nursing Diagnosis Handbook: An Evidence-Based Guide to Planning Care
This handbook is highly praised for its evidence-based approach to nursing interventions. It uses a clear, three-step system to guide you through assessment, diagnosis, and care planning. It includes step-by-step instructions for implementing care and evaluating outcomes, fostering diagnostic reasoning and critical thinking skills. Its evidence-based rationales are particularly helpful in understanding the ‘why’ behind nursing interventions, making it a valuable resource for learning and applying nursing diagnosis and care plans.
Nursing Care Plans – Nursing Diagnosis & Intervention (10th Edition)
This comprehensive text features over 200 care plans reflecting the latest evidence-based guidelines. The 10th edition includes ICNP diagnoses, care plans addressing LGBTQ health issues, and expanded content on electrolytes and acid-base balance. Its extensive collection of care plans makes it an excellent resource for both students and practicing nurses looking for practical examples and templates for nursing diagnosis and care plans.
Nurse’s Pocket Guide: Diagnoses, Prioritized Interventions, and Rationales
This quick-reference guide is ideal for rapid access to essential information for patient care planning. It includes current nursing diagnoses and interventions, with an alphabetized listing of diagnoses covering over 400 disorders. The pocket-size format makes it convenient for clinical use, providing on-the-spot support for formulating nursing diagnosis and care plans.
Nursing Diagnosis Manual: Planning, Individualizing, and Documenting Client Care
This manual is specifically designed to help nurses plan, individualize, and document care for over 800 diseases and disorders. For each diagnosis, it includes subjective and objective data, sample clinical applications, prioritized actions/interventions with rationales, and a documentation section. Its focus on individualization and documentation makes it a crucial tool for developing patient-centered nursing diagnosis and care plans.
This resource offers over 100 care plans across various specialties, including medical-surgical, maternity/OB, pediatrics, and psychiatric-mental health. Its interprofessional “patient problems” approach helps users understand patient care from a holistic perspective. The broad coverage across specialties makes it a versatile resource for learning about nursing diagnosis and care plans in diverse clinical settings.
By utilizing these recommended books and diligently practicing the steps outlined in this guide, nursing students and professionals can significantly enhance their ability to create effective, patient-centered nursing care plans. Mastering this skill is not only essential for providing high-quality patient care but also for professional growth and success in the nursing field.