Hemophilia is a rare, inherited bleeding disorder that impairs the blood’s ability to clot, leading to prolonged bleeding after injury, surgery, or even spontaneously. This condition, primarily affecting males, varies in severity depending on the deficiency of specific clotting factors. For nurses, understanding hemophilia and its implications is crucial for providing effective patient care. This article delves into the essential nursing diagnoses associated with hemophilia, offering a guide for healthcare professionals to deliver comprehensive and patient-centered care.
Understanding Hemophilia: Pathophysiology and Types
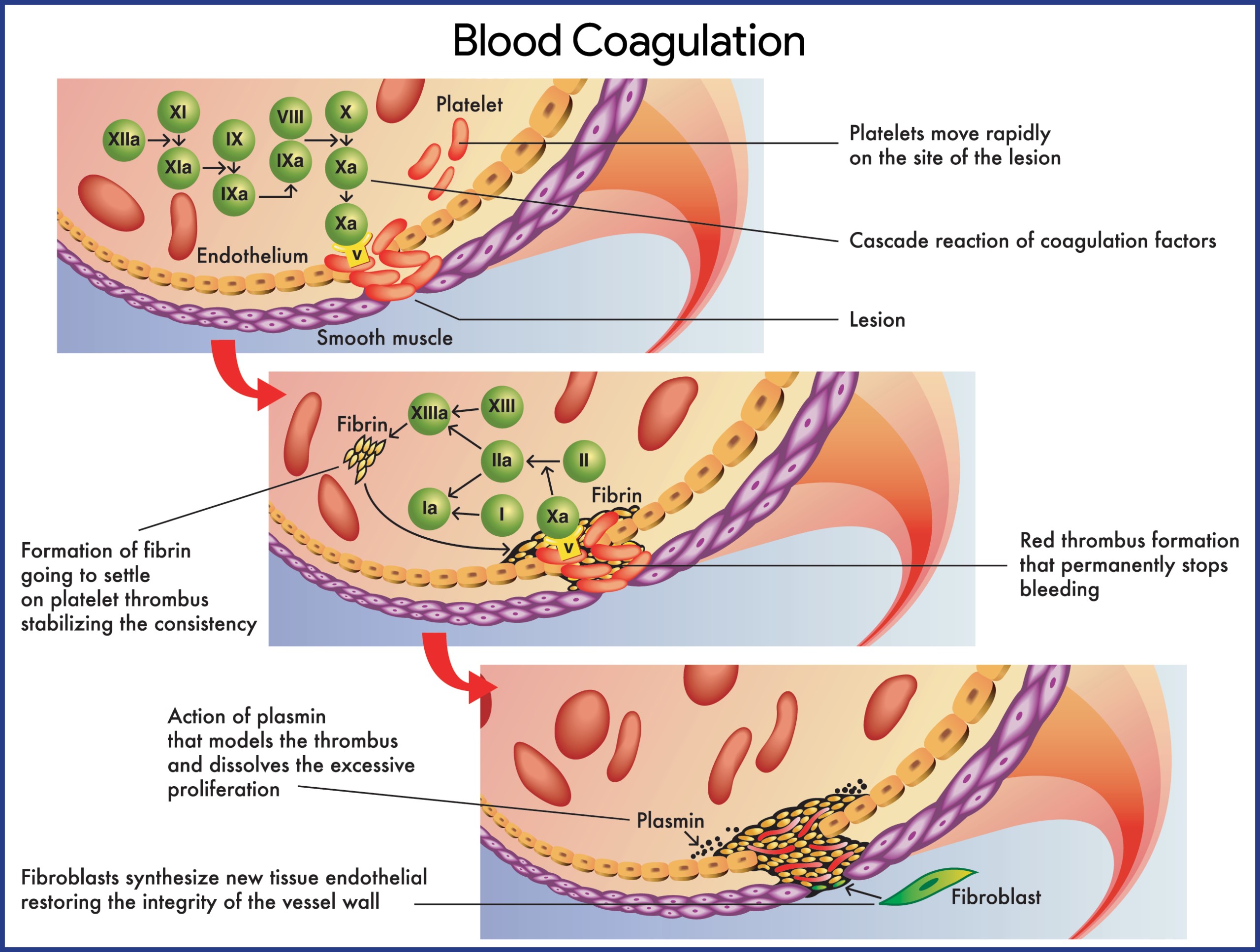
Hemophilia arises from genetic defects in genes that code for clotting factors, specifically factor VIII in hemophilia A (classic hemophilia) and factor IX in hemophilia B (Christmas disease). These factors are vital components of the coagulation cascade, a complex process that stops bleeding. Deficiencies in these factors disrupt the cascade, resulting in prolonged bleeding.
Hemophilia A Pathophysiology: Primarily due to a deficiency or dysfunction of factor VIII, essential for activating factor X in the coagulation cascade. This deficiency disrupts the intrinsic pathway, leading to excessive bleeding, especially in joints, muscles, and internal organs. Synovial inflammation from joint bleeds can create “target joints,” prone to repeated hemorrhages. A significant complication is the development of factor VIII inhibitors (alloantibodies), making treatment more challenging.
Hemophilia B Pathophysiology: Results from a deficiency or dysfunction of factor IX, also critical in the intrinsic coagulation pathway. Similar to Hemophilia A, this leads to impaired clot formation and increased risk of bleeding in joints, muscles, and vital organs, including the central nervous system and gastrointestinal tract.
Incidence and Genetic Basis of Hemophilia
Hemophilia A is the most common inherited bleeding disorder, affecting approximately 1 in 5,000 males worldwide. Hemophilia B is less frequent, occurring in about 1 in 25,000 to 30,000 male births. Both are X-linked recessive conditions, predominantly affecting males, while females are usually carriers. About one-third of hemophilia A cases occur in individuals with no family history, indicating spontaneous genetic mutations.
Clinical Manifestations and Diagnostic Assessment
Clinical signs of hemophilia vary with severity and can range from mild to severe bleeding tendencies. Spontaneous bleeding, bleeding disproportionate to injury, and a family history of bleeding disorders are suggestive.
Common clinical manifestations include:
- Hemarthrosis: Bleeding into joint spaces, causing pain, swelling, warmth, and stiffness. Repeated joint bleeds can lead to chronic arthropathy and disability.
- Muscle Hemorrhage: Bleeding into muscles can cause pain, swelling, and nerve compression.
- Soft Tissue Bleeding: Easy bruising and hematomas.
- Mucosal Bleeding: Nosebleeds, gum bleeding, and gastrointestinal bleeding.
- Hematuria: Blood in the urine, often painless.
- Central Nervous System Bleeding: Intracranial hemorrhage is a severe complication, presenting with headaches, stiff neck, vomiting, lethargy, and irritability.
Diagnostic findings typically involve:
- Coagulation Studies: Prolonged activated partial thromboplastin time (aPTT) is common. Prothrombin time (PT) and platelet count are usually normal.
- Factor Assays: Specific assays for factor VIII and factor IX levels confirm the diagnosis and determine the type and severity of hemophilia.
- Genetic Testing: Can identify the specific genetic mutation and carrier status.
- Imaging Studies: CT scans and MRI may be used to assess for internal bleeding, especially in the head and joints.
Medical and Nursing Management Strategies
The cornerstone of hemophilia management is factor replacement therapy. This involves infusing concentrates of factor VIII for hemophilia A and factor IX for hemophilia B to prevent or treat bleeding episodes.
Medical Management includes:
- Factor Replacement Therapy: Prophylactic or on-demand infusions of factor concentrates. Recombinant factor concentrates are preferred to minimize the risk of blood-borne infections.
- Desmopressin (DDAVP): For mild hemophilia A, DDAVP can stimulate the release of factor VIII.
- Antifibrinolytic Agents: Medications like tranexamic acid and aminocaproic acid can be used adjunctively, especially for mucosal bleeding.
- Bypassing Agents: For patients with inhibitors, bypassing agents like activated factor VIIa or prothrombin complex concentrates can promote clotting.
- Pain Management: Analgesics for acute and chronic pain associated with bleeding episodes and joint damage. NSAIDs should be used cautiously due to their potential to exacerbate bleeding.
- Gene Therapy: Emerging treatment showing promise for long-term factor production.
- Radiosynovectomy: For chronic synovitis, radioisotope injection can reduce bleeding.
Nursing Management focuses on:
- Assessment: Identifying patients at risk, monitoring for bleeding signs, and assessing pain and mobility.
- Education: Patient and family education on hemophilia, self-infusion techniques, recognizing bleeding signs, and preventive measures.
- Care during Bleeding Episodes: Administering factor replacement therapy, pain management, and joint immobilization.
- Preventing Injury: Educating patients about safe activities and home modifications to reduce the risk of trauma.
- Psychosocial Support: Addressing the emotional and social challenges of living with a chronic bleeding disorder.
Ryan White, a prominent advocate for hemophilia awareness, emphasizing the importance of comprehensive care and support.
Key Nursing Diagnoses for Hemophilia
Based on the comprehensive assessment and understanding of hemophilia, several nursing diagnoses are pertinent to patient care. These diagnoses guide the development of individualized care plans to address the specific needs of individuals with hemophilia.
1. Risk for Bleeding related to deficiency of clotting factors (Factor VIII or IX).
- Defining Characteristics: History of prolonged bleeding, spontaneous bleeding, easy bruising, hemarthrosis, hematuria, and prolonged aPTT.
- Nursing Interventions:
- Administer factor replacement therapy as prescribed and monitor for effectiveness.
- Educate patient and family on recognizing early signs of bleeding and when to seek treatment.
- Implement bleeding precautions: avoid intramuscular injections, minimize venipunctures, use soft toothbrushes, and pad crib rails for children.
- Monitor for signs of internal bleeding: changes in vital signs, abdominal pain, headache, and neurological changes.
2. Acute Pain related to hemarthrosis, muscle hemorrhage, or injury.
- Defining Characteristics: Reports of pain, guarding behavior, joint swelling, limited range of motion, and elevated pain scores.
- Nursing Interventions:
- Assess pain using a validated pain scale regularly.
- Administer prescribed analgesics, including factor replacement therapy, and non-opioid or opioid pain relievers as needed.
- Apply ice packs to affected joints or muscles to reduce swelling and pain.
- Elevate and immobilize the affected limb to reduce pain and promote healing.
- Teach relaxation techniques and distraction methods for pain management.
3. Impaired Physical Mobility related to joint pain, swelling, and muscle weakness secondary to hemarthrosis and muscle bleeds.
- Defining Characteristics: Limited range of motion, reluctance to move affected joints, muscle weakness, and difficulty performing activities of daily living.
- Nursing Interventions:
- Assess range of motion and functional abilities.
- Encourage gentle range-of-motion exercises within pain tolerance during periods of remission.
- Collaborate with physical therapy for tailored exercise programs and assistive devices.
- Promote weight management to reduce stress on joints.
- Educate on the importance of maintaining muscle strength and joint mobility.
4. Risk for Injury related to decreased clotting factors and potential for bleeding.
- Defining Characteristics: Known diagnosis of hemophilia, history of bleeding episodes, and potential exposure to trauma.
- Nursing Interventions:
- Educate patient and family on injury prevention strategies: avoiding contact sports, using protective gear, and creating a safe home environment.
- Assess home environment for safety hazards and recommend modifications.
- Encourage participation in non-contact activities to maintain physical fitness.
- Provide guidance on managing minor injuries at home and when to seek medical attention.
5. Compromised Family Coping related to chronic illness of a family member and the complexities of hemophilia management.
- Defining Characteristics: Expressed concerns about managing hemophilia, difficulty understanding the condition, anxiety, and changes in family roles or dynamics.
- Nursing Interventions:
- Assess family coping mechanisms and support systems.
- Provide comprehensive education about hemophilia, its management, and potential complications.
- Offer resources for emotional and financial support, such as hemophilia organizations and support groups.
- Facilitate communication between family members and the healthcare team.
- Encourage respite care and self-care strategies for caregivers.
Conclusion: Enhancing Nursing Care for Hemophilia
Effective nursing care for patients with hemophilia requires a thorough understanding of the disease, its complications, and the nursing diagnoses that guide patient-centered care. By focusing on preventing bleeding, managing pain, promoting mobility, preventing injury, and supporting families, nurses play a vital role in improving the quality of life for individuals living with hemophilia. Continuous education and collaboration within a multidisciplinary team are essential to provide optimal care and support for this complex and chronic condition.
References:
- (Include relevant medical and nursing resources on hemophilia and nursing diagnoses here)