Peptic ulcer disease (PUD) is a common gastrointestinal disorder characterized by sores on the lining of the stomach, duodenum, or esophagus. Understanding the Nursing Diagnosis For Peptic Ulcer Disease is crucial for effective patient care and management. This guide provides an in-depth look at nursing diagnoses related to PUD, enhancing the original article with a focus on nursing care and SEO optimization for an English-speaking audience.
Understanding Peptic Ulcer Disease
A peptic ulcer is a lesion in the mucosal lining of the upper gastrointestinal tract. These ulcers are classified based on their location:
- Gastric Ulcers: Located in the stomach, most commonly on the lesser curvature near the pylorus.
- Duodenal Ulcers: Occur in the duodenum, the first part of the small intestine. Duodenal ulcers are more prevalent than gastric ulcers.
- Esophageal Ulcers: Develop in the esophagus due to the reflux of hydrochloric acid (HCl) from the stomach.
Pathophysiology of Peptic Ulcers
Peptic ulcer disease arises from an imbalance between aggressive factors and defensive mechanisms in the gastroduodenal mucosa.
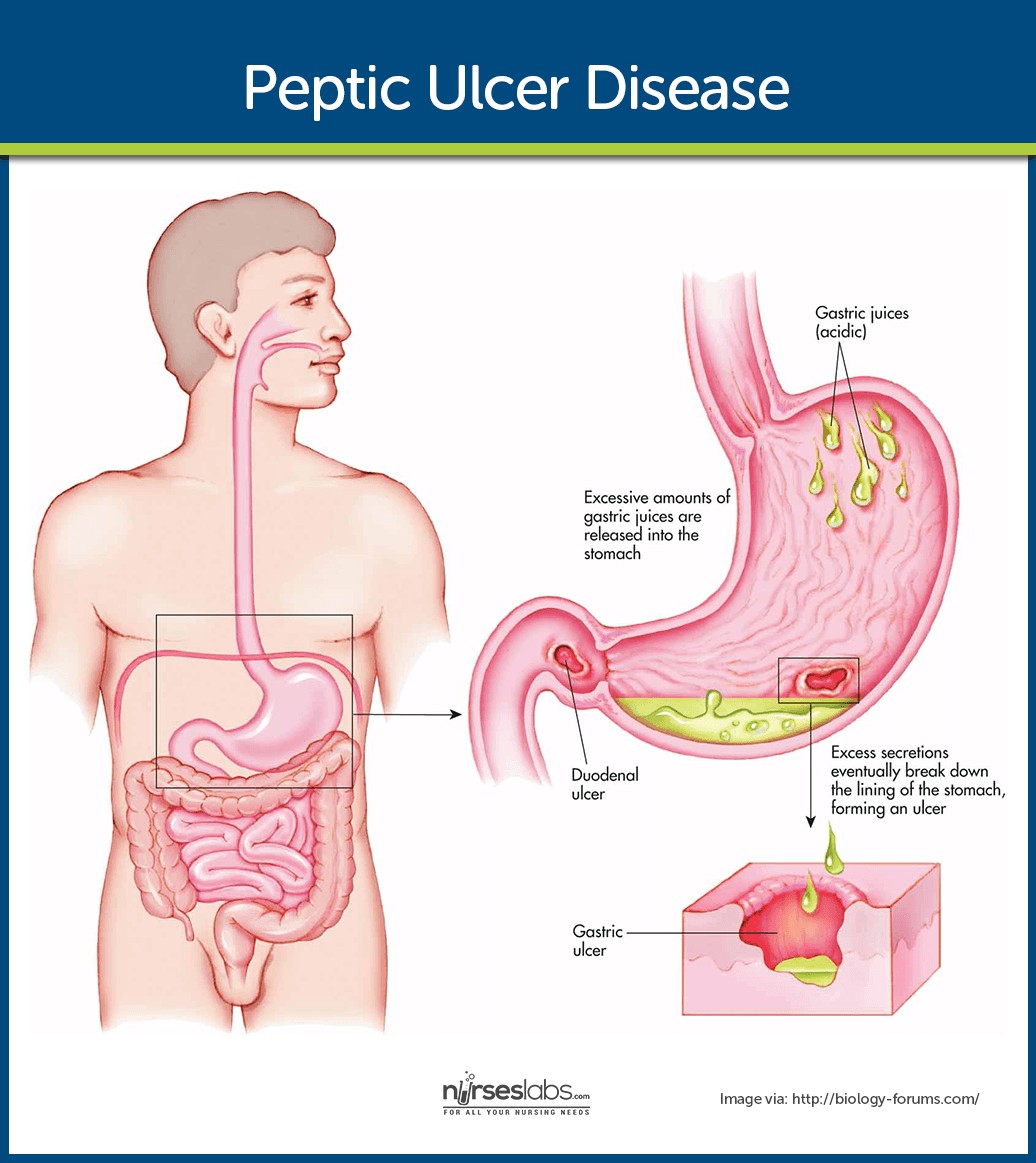 Visual representation of peptic ulcer pathophysiology showing erosion, damage, acid secretion and decreased resistance
Visual representation of peptic ulcer pathophysiology showing erosion, damage, acid secretion and decreased resistance
- Mucosal Erosion: Increased acid-pepsin activity or decreased mucosal resistance leads to erosion of the protective mucosal layer.
- Mucosal Damage: Damaged mucosa cannot produce sufficient mucus, which normally acts as a barrier against HCl.
- Acid Secretion Imbalance: Patients with duodenal ulcers often have increased acid secretion, while those with gastric ulcers may have normal or decreased acid levels.
- Reduced Mucosal Resistance: Damage weakens the mucosa’s defense, increasing susceptibility to bacterial infection, particularly by Helicobacter pylori (H. pylori).
Epidemiology and Statistics
Peptic ulcer disease affects individuals across all ages and genders.
- Age Distribution: The highest incidence of PUD is observed in individuals aged 40 to 60 years.
- Gender Differences: Before menopause, women have a lower incidence compared to men. However, after menopause, the incidence in women becomes nearly equal to that in men.
- Pediatric Cases: While less common, PUD can occur in children and infants.
Etiology of Peptic Ulcer Disease
Several factors contribute to the development of peptic ulcers:
- Helicobacter pylori (H. pylori) Infection: This gram-negative bacterium is a primary cause of PUD. H. pylori, often acquired through contaminated food or water, disrupts the mucosal barrier, making the stomach and duodenum vulnerable to acid damage.
- Nonsteroidal Anti-inflammatory Drugs (NSAIDs): Chronic NSAID use inhibits prostaglandin production, which is vital for mucosal protection, thereby promoting ulcer formation.
- Pathological Hypersecretory Disorders: Conditions like Zollinger-Ellison syndrome lead to excessive gastric acid secretion, overwhelming mucosal defenses.
- Other Illnesses: Conditions such as pancreatitis, liver disease, Crohn’s disease, and gastritis are associated with increased PUD risk.
- Excessive HCl Secretion: While not always the primary cause, overproduction of HCl contributes to ulcer development.
- Lifestyle Irritants: Certain substances, including caffeinated beverages, alcohol, and milk (in some individuals), can stimulate HCl secretion and gastric emptying, potentially exacerbating mucosal breakdown.
- Blood Type Predisposition: Individuals with blood type A are more prone to gastric ulcers, while duodenal ulcers are more common in those with blood type O.
Clinical Manifestations of Peptic Ulcers
Peptic ulcer symptoms are varied and can fluctuate in intensity and duration.
- Pain: The hallmark symptom is abdominal pain, often described as burning or gnawing. Pain location can vary depending on ulcer location:
- Gastric Ulcer Pain: May worsen with eating, typically occurring shortly after meals.
- Duodenal Ulcer Pain: Often relieved by food or antacids, frequently occurring 2-3 hours after meals and during the night.
- Bloating and Fullness: A sensation of fullness or bloating can accompany ulcer pain.
- Heartburn: Acid reflux and heartburn are common, especially with esophageal ulcers.
- Nausea and Vomiting: These symptoms can occur, particularly if the ulcer is causing gastric outlet obstruction.
- Weight Loss: Unintentional weight loss may occur due to pain-induced reduced food intake or malabsorption.
Potential Complications of PUD
Untreated peptic ulcers can lead to serious complications:
- Hemorrhage: The most frequent complication, occurring in 10-20% of PUD patients. Bleeding can manifest as hematemesis (vomiting blood) or melena (dark, tarry stools).
- Perforation: Ulcer erosion through the stomach or duodenal wall into the peritoneal cavity. This is a surgical emergency presenting with sudden, severe abdominal pain.
- Penetration: Ulcer erosion into adjacent organs, such as the pancreas or liver, causing referred pain and potential organ damage.
- Pyloric Obstruction: Scarring and stenosis near the pyloric sphincter can obstruct gastric outflow, leading to nausea, vomiting, and abdominal distention.
Diagnostic Assessment for Peptic Ulcer Disease
Accurate diagnosis is essential for effective PUD management. Diagnostic procedures include:
- Esophagogastroduodenoscopy (EGD): The gold standard for diagnosis. EGD allows direct visualization of the esophagus, stomach, and duodenum, confirming ulcer presence and enabling biopsy and cytology to detect H. pylori or rule out malignancy.
- Physical Examination: May reveal epigastric tenderness, pain upon palpation, or abdominal distention.
- Barium Swallow (Upper GI Series): Radiographic imaging using barium contrast can identify ulcers, although it is less sensitive than endoscopy.
- H. pylori Testing: Various tests detect H. pylori infection:
- Urea Breath Test: Non-invasive test measuring urea breakdown products to indicate active H. pylori infection.
- Stool Antigen Test: Detects H. pylori antigens in stool samples.
- Biopsy during EGD: Tissue samples can be tested for H. pylori using histology, culture, or rapid urease tests.
- Occult Blood Test: Stool samples are tested to detect microscopic blood, indicating potential bleeding from an ulcer.
Medical and Surgical Management of PUD
Treatment aims to eradicate H. pylori, reduce gastric acidity, and promote ulcer healing.
- Pharmacological Therapy:
- Proton Pump Inhibitors (PPIs): Potent acid suppressants, e.g., omeprazole, lansoprazole.
- H2 Receptor Antagonists: Reduce acid secretion, e.g., ranitidine, famotidine.
- Antibiotics: Used in combination to eradicate H. pylori infection, typically a triple or quadruple therapy regimen.
- Mucosal Protectants: Sucralfate and bismuth subsalicylate protect the ulcer site and promote healing.
- Antacids: Neutralize stomach acid for symptomatic relief.
- Surgical Interventions: Less common due to effective medical therapies, surgery may be necessary for complications like perforation, uncontrolled bleeding, or obstruction.
- Pyloroplasty: Surgical widening of the pyloric sphincter.
- Antrectomy: Removal of the antrum of the stomach, which produces gastrin.
- Vagotomy: Severing the vagus nerve to reduce gastric acid secretion.
Nursing Management: Nursing Diagnoses for Peptic Ulcer Disease
Nursing care is integral to managing patients with PUD. Based on assessment data, common nursing diagnoses for peptic ulcer disease include:
-
Acute Pain related to gastric mucosal irritation secondary to peptic ulcer disease, as evidenced by patient report of epigastric pain, guarding behavior, and changes in vital signs.
- Nursing Interventions:
- Assess pain characteristics (location, intensity, duration, aggravating/relieving factors).
- Administer prescribed analgesics and antacids as ordered.
- Encourage the patient to eat small, frequent meals.
- Advise avoidance of foods and beverages that exacerbate pain (e.g., spicy foods, caffeine, alcohol).
- Promote relaxation techniques (e.g., deep breathing, meditation).
- Nursing Interventions:
-
Risk for Bleeding related to peptic ulcer erosion into blood vessels.
- Nursing Interventions:
- Monitor vital signs for signs of hypovolemia (hypotension, tachycardia).
- Assess for signs of bleeding (hematemesis, melena, pallor, dizziness).
- Monitor hemoglobin and hematocrit levels.
- Administer prescribed medications to reduce acid and promote healing.
- Prepare for potential blood transfusion or endoscopic intervention if bleeding occurs.
- Nursing Interventions:
-
Imbalanced Nutrition: Less Than Body Requirements related to pain and discomfort associated with eating, as evidenced by reported decreased food intake, weight loss, and aversion to food.
- Nursing Interventions:
- Assess nutritional status and dietary intake.
- Encourage small, frequent meals as tolerated.
- Advise on easily digestible, non-irritating foods.
- Monitor weight regularly.
- Consult with a dietitian for nutritional support and meal planning.
- Nursing Interventions:
-
Anxiety related to the diagnosis of chronic illness and potential complications, as evidenced by patient expressions of worry, restlessness, and changes in sleep patterns.
- Nursing Interventions:
- Assess the patient’s level of anxiety and coping mechanisms.
- Provide clear and accurate information about PUD, treatment, and prognosis.
- Encourage the patient to express feelings and concerns.
- Offer emotional support and reassurance.
- Teach stress-reduction techniques.
- Refer to counseling or support groups if needed.
- Nursing Interventions:
-
Deficient Knowledge related to peptic ulcer disease management and prevention of recurrence, as evidenced by patient questions about the condition, lack of adherence to treatment plan, and expressed misinformation.
- Nursing Interventions:
- Assess the patient’s understanding of PUD, medications, and lifestyle modifications.
- Provide patient education on:
- Medications (name, dosage, frequency, side effects, importance of adherence).
- Dietary modifications (foods to avoid, meal timing, portion control).
- Lifestyle changes (smoking cessation, stress management, alcohol limitation).
- Signs and symptoms of complications requiring immediate medical attention.
- Utilize various teaching methods (verbal, written materials, demonstrations).
- Encourage patient questions and provide clear, understandable answers.
- Nursing Interventions:
Nursing Care Planning and Goals
The primary goals for nursing care of patients with peptic ulcer disease are:
- Pain relief and comfort.
- Prevention and management of complications.
- Attainment of adequate nutritional intake.
- Reduction of anxiety and emotional support.
- Patient education and self-management skills for long-term health.
Nursing Interventions: Implementation
Nursing interventions are tailored to address the identified nursing diagnoses and achieve patient goals. Key interventions include:
Pain Management and Nutritional Support:
- Administer prescribed analgesics, antacids, and other medications promptly.
- Educate patients about avoiding NSAIDs, aspirin, caffeine, alcohol, and acidic foods.
- Encourage regular, small, well-spaced meals in a relaxed environment.
- Monitor weight and dietary intake regularly.
- Teach relaxation and stress-reduction techniques.
Anxiety Reduction:
- Assess anxiety levels and coping mechanisms.
- Provide patient education about the disease, diagnostic tests, and treatment plan.
- Create a calm and supportive environment.
- Encourage open communication and address patient fears and concerns.
- Involve family members in care and support, as appropriate.
Complication Monitoring and Management:
- Vigilantly monitor for signs and symptoms of hemorrhage, perforation, and obstruction.
- Report any changes in patient condition promptly.
- Implement emergency protocols as needed (e.g., for hemorrhage or perforation).
- Educate patients about warning signs and when to seek immediate medical attention.
Home Management and Self-Care Education:
- Provide comprehensive discharge instructions, including medication regimens, dietary guidelines, and lifestyle modifications.
- Emphasize the importance of medication adherence, even after symptom improvement.
- Educate on foods and substances that can aggravate PUD.
- Encourage smoking cessation and stress management.
- Instruct on recognizing and reporting signs of complications.
- Ensure the patient understands follow-up appointments and resources.
Evaluation of Nursing Care
Patient outcomes are evaluated based on the established goals. Expected outcomes include:
- Patient reports adequate pain relief.
- Patient demonstrates no signs or symptoms of complications.
- Patient maintains adequate nutritional intake and stable weight.
- Patient expresses reduced anxiety and improved coping.
- Patient verbalizes understanding of PUD management and prevention strategies.
Discharge and Home Care Guidelines
Prior to discharge, patients should receive thorough self-care instructions.
- Understanding the Condition: Explain factors that relieve and aggravate PUD symptoms.
- Medication Education: Review medication names, dosages, frequency, side effects, and the importance of continued medication use.
- Dietary Instructions: Provide specific dietary guidelines, emphasizing foods to avoid and those that are beneficial.
- Lifestyle Recommendations: Counsel on lifestyle modifications, such as regular meal times, stress reduction, and smoking cessation.
Documentation in Nursing Care
Accurate and thorough documentation is essential. Key documentation points include:
- Patient’s pain assessment and response to pain management interventions.
- Anxiety level and coping mechanisms.
- Nutritional intake and any dietary restrictions or preferences.
- Patient education provided and their understanding of the information.
- Patient’s progress towards desired outcomes and any modifications to the care plan.
- Any complications and interventions implemented.
Conclusion
Understanding nursing diagnoses for peptic ulcer disease is fundamental for providing holistic and effective care. By focusing on pain management, preventing complications, ensuring nutritional support, addressing anxiety, and empowering patients through education, nurses play a vital role in improving outcomes and enhancing the quality of life for individuals with PUD. This comprehensive guide aims to equip healthcare professionals with the knowledge to deliver optimal nursing care for patients with peptic ulcer disease.
See Also
Related resources for further study:
- Pancreatitis
- Risk for Bleeding
