Pelvic Congestion Syndrome (PCS) diagnosis presents a significant challenge for healthcare professionals across various specialties, including anesthesiology, gastroenterology, general surgery, obstetrics and gynecology, and interventional radiology. For women experiencing chronic pelvic pain where other causes have been excluded, consulting an interventional radiologist can be crucial for accurate diagnosis and effective treatment of PCS. Increased awareness of the specific symptoms and related findings associated with PCS is essential for facilitating a quicker path to appropriate treatment. For interventional radiologists specializing in PCS, Magnetic Resonance Imaging/MR Venography (MRI/MRV), diagnostic venography, and embolotherapy are central to both the diagnosis and management of this condition.
Understanding Pelvic Congestion Syndrome (PCS)
Pelvic Congestion Syndrome (PCS) is a condition characterized by chronic pelvic pain arising from the presence of varicose veins in the pelvic region. Similar to varicose veins in the legs, these pelvic varices occur when the veins become enlarged and twisted, leading to blood pooling and discomfort. Initially documented in 1949 regarding its association with pelvic varices, PCS was clinically described even earlier by French physicians in 1857. This condition predominantly affects women, particularly those between 20 and 45 years of age. While the exact causes are multifaceted, PCS is strongly linked to hormonal influences and changes associated with pregnancy.
Who is Affected by PCS?
Millions of women globally experience chronic pelvic pain at some point in their lives, with prevalence rates potentially reaching as high as 39.1%. In the United States, chronic pelvic pain accounts for a significant proportion, approximately 10% to 15%, of all outpatient gynecologic visits. While PCS can affect women of various backgrounds, certain factors increase the likelihood of developing this condition. Multiparous women, who have had multiple pregnancies, are more susceptible to PCS. This predisposition is thought to be due to the physiological changes during pregnancy that impact the pelvic veins. The role of genetics or ethnicity in PCS prevalence remains unclear and requires further research.
Pathophysiology of Pelvic Congestion Syndrome
Several factors contribute to the development of PCS. The hallmark symptom, a persistent dull ache in the pelvis, is primarily attributed to the presence of ovarian and pelvic varicosities. This pain mechanism mirrors that of leg pain caused by varicose veins in the lower extremities. A key factor is the impact of multiple pregnancies on venous function. During each pregnancy, a woman’s intravascular volume significantly increases, with vein capacity potentially expanding by as much as 60%. This repeated venous distension over time can lead to the valves within the veins becoming incompetent, hindering proper blood flow. Furthermore, the physical changes and weight gain during pregnancy can cause intermittent obstruction of pelvic veins. This obstruction, along with hormonal influences, leads to blood pooling in the pelvic and ovarian veins, resulting in engorgement, potential thrombosis, and pressure on surrounding nerves, all contributing to pelvic pain.
Image alt text: Asymmetrical vulvar varices visible under the soft tissue, indicating potential pelvic congestion syndrome.
Hormonal factors, specifically estrogen, play a significant role in PCS. The majority of women with PCS are premenopausal, suggesting a link between endogenous estrogen levels and the condition. Estrogen is known to weaken vein walls, making them more susceptible to dilation and varicosity formation.
Anatomical factors can also lead to secondary PCS. For instance, a retroaortic left renal vein can obstruct the left ovarian vein, resulting in symptomatic pelvic varices. Similarly, the left ovarian and renal veins can be compressed by the superior mesenteric artery, a condition known as Nutcracker phenomenon. Another anatomical consideration is May-Thurner syndrome, where compression of the left common iliac vein by the right common iliac artery against the spine and pelvic brim can lead to iliofemoral deep venous thrombosis and pelvic varices characteristic of PCS.
Clinical Presentation: Recognizing PCS Symptoms
The primary symptom of Pelvic Congestion Syndrome is chronic pelvic pain, defined as non-cyclical pain lasting for more than six months. This pain often exhibits specific patterns and can be aggravated by various activities and positions. Women with PCS frequently report that their pelvic pain worsens with:
- Prolonged Sitting or Standing: These positions increase pressure in the pelvic veins, exacerbating the pain.
- End of the Day: Pain intensity often increases as the day progresses, likely due to cumulative venous congestion.
- Intercourse (Dyspareunia): Pain during or after sexual activity is a common complaint, due to increased blood flow to the pelvic area.
- Pre-menstruation: Hormonal fluctuations before menstruation can worsen PCS symptoms.
In addition to chronic pelvic pain, women with PCS may experience a range of other non-specific symptoms of variable intensity. These can include:
- Generalized Lethargy and Fatigue: Persistent pelvic pain can contribute to overall fatigue and reduced energy levels.
- Depression: Chronic pain conditions are often associated with mood disorders like depression.
- Abdominal or Pelvic Tenderness: Physical examination may reveal tenderness in the lower abdomen and pelvic region.
- Vaginal Discharge: Some women may experience increased vaginal discharge.
- Dysmenorrhea: Painful menstruation can be another symptom, although PCS pain is typically non-cyclical.
- Swollen Vulva: Varicosities can extend to the vulva, causing swelling and discomfort.
- Lumbosacral Neuropathy: Pain may radiate to the lower back and sacral region.
- Rectal Discomfort: Pressure from pelvic varices can cause discomfort in the rectal area.
- Urinary Frequency: Increased pressure on the bladder can lead to more frequent urination.
Physical examination findings in women with PCS can include cervical motion tenderness or localized tenderness over the ovaries or uterus during a bimanual exam. Visible signs such as hemorrhoids and varicose veins in the perineum, buttocks, or lower extremities may also be present, further supporting the diagnosis. It’s important to note that PCS can coexist with other pelvic pathologies, making diagnosis and treatment more complex.
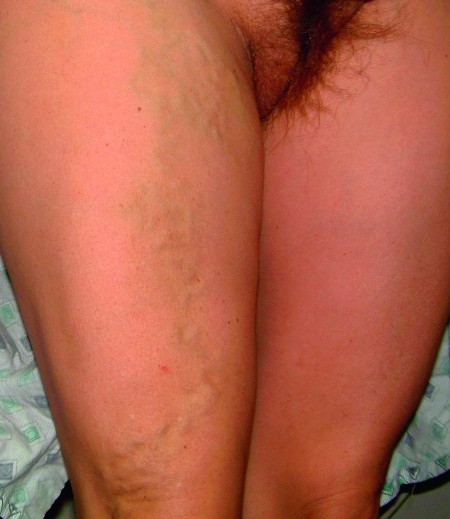
Image alt text: Varicose veins extending into the leg, a potential sign of pelvic congestion syndrome contributing to broader venous insufficiency.
The Diagnostic Journey: How is PCS Diagnosed?
For many women, achieving a definitive Pelvic Congestion Syndrome Diagnosis is a lengthy and challenging process. The diagnosis of PCS remains complex and requires careful consideration by all physicians involved. However, a heightened clinical suspicion for PCS, guided by specific symptoms and associated findings, can significantly expedite the diagnostic process and lead to timely treatment.
When other potential pelvic pathologies have been ruled out, consultation with an interventional radiologist is often recommended for further evaluation and management of suspected PCS. By the time a patient is referred to an interventional radiologist, several imaging modalities may have already been utilized. However, PCS is frequently missed during initial imaging, largely because standard imaging is often performed with the patient in a supine (lying down) position. In this position, pelvic venous distension, a key indicator of PCS, may be underestimated or even absent.
Imaging Modalities for PCS Diagnosis
Several imaging techniques play a crucial role in the pelvic congestion syndrome diagnosis process.
Ultrasound (US) and CT Scans
Pelvic ultrasound (US) and computed tomography (CT) scans are commonly the initial imaging modalities used in evaluating chronic pelvic pain. Both US and CT provide excellent visualization of the uterus and other pelvic organs, helping to rule out various gynecological conditions. CT scans are particularly sensitive in detecting varicosities throughout the lower pelvis. However, ultrasound, especially with Doppler examination, offers dynamic information about blood flow within the veins, which is valuable in assessing venous insufficiency.
Sonographic criteria for diagnosing pelvic varices include:
- Dilated Ovarian Veins: Visualization of ovarian veins with a diameter greater than 4mm.
- Dilated Arcuate Veins: Presence of dilated and tortuous arcuate veins within the myometrium (uterine muscle), communicating with pelvic varices.
- Slow or Reversed Blood Flow: Reduced blood flow velocity (less than 3 cm/s) or retrograde (reversed) venous blood flow, particularly in the left ovarian vein, indicative of venous reflux.
Interestingly, cystic ovaries are frequently observed in women with PCS, with over 50% exhibiting this finding. The ultrasound appearance can range from classic polycystic ovarian syndrome to clusters of cysts in bilaterally enlarged ovaries (typically 4 to 6 cysts, 5 to 15 mm in diameter). The clinical significance of these cystic changes in PCS patients is not fully understood, especially as most women with PCS do not present with hirsutism or amenorrhea, typical of polycystic ovary syndrome. However, the association does reinforce the suspected role of estrogen overstimulation in PCS.
While US and CT scans are readily accessible and relatively quick (20-30 minutes for outpatients), they have lower sensitivity for PCS compared to Magnetic Resonance Imaging/MR Venography (MRI/MRV) or diagnostic venography. Nevertheless, their primary value lies in effectively excluding other pelvic pathologies, particularly underlying malignancies that can mimic PCS symptoms.
MRI/MRV: The Preferred Imaging
For interventional radiologists specializing in PCS treatment, MRI/MRV is often considered the optimal primary imaging modality for pelvic congestion syndrome diagnosis. MRI/MRV offers several advantages: it is an outpatient procedure, non-invasive, radiation-free, and highly sensitive in detecting pelvic varices.
Typical MRI findings indicative of PCS include:
- Dilated, Tortuous Tubular Structures: Presence of enlarged, winding, and interconnected vessels near the uterus and ovaries, potentially extending into the broad ligament and pelvic sidewall.
- Signal Intensity on Different Sequences:
- T1-weighted images: Varices appear as flow voids (areas of signal absence).
- Gradient-echo (GRE): Varices show high signal intensity.
- T2-weighted images: Varices typically appear low in signal intensity.
- 3D T1-weighted GRE with Gadolinium: Contrast enhancement with gadolinium highlights varices with high signal intensity.
Contrast enhancement with gadolinium improves the visualization of pelvic varices and may increase diagnostic sensitivity, especially if images are acquired while the patient performs a Valsalva maneuver (holding breath and straining). MRV images are particularly valuable in mapping the complete pelvic venous anatomy and delineating the extent of varicosities.
Diagnostic Venogram: The Gold Standard
Diagnostic venography remains the minimally invasive gold standard for pelvic congestion syndrome diagnosis. This procedure, performed under fluoroscopy, involves accessing the venous system, typically through the common femoral vein. A catheter is then guided to selectively catheterize the ovarian and pelvic veins, allowing for contrast injection at each site.
PCS diagnosis is confirmed venographically based on the following criteria:
- Ovarian Vein Diameter > 6mm: Enlargement of the ovarian vein beyond 6mm in diameter.
- Retrograde Venous Flow: Backward (retrograde) flow of contrast in the ovarian or pelvic veins, indicating venous reflux.
- Tortuous Collateral Pathways: Presence of multiple, winding collateral venous pathways in the pelvis, indicative of abnormal venous drainage.
- Delayed Contrast Clearance: Slow or stagnant clearing of contrast from the veins at the end of injection, suggesting venous congestion.
While diagnostic venography involves radiation exposure, contrast administration, and is an invasive procedure, it offers distinct advantages over other imaging methods. It provides immediate, dynamic information about venous flow and allows for precise measurements of ovarian and pelvic vein diameters. Furthermore, patient positioning can be adjusted during the procedure (e.g., using a tilt table) to assess the influence of gravity on venous congestion. Venography can also be performed with balloon occlusion in the pelvis to further evaluate venous reflux. Crucially, diagnostic venography can seamlessly transition into embolotherapy, allowing for immediate treatment by the interventional radiologist.
Laparoscopy: Limited Role in PCS Diagnosis
Laparoscopy, a minimally invasive surgical procedure involving direct visualization of the pelvic organs, is frequently used in women with chronic pelvic pain to investigate potential causes. It is excellent for excluding conditions like endometriosis, which can mimic PCS symptoms. However, laparoscopy has limitations in diagnosing PCS itself. The procedure is performed with the patient supine and with insufflation of carbon dioxide (CO2) gas into the abdomen. This position and CO2 insufflation can compress pelvic varices, potentially masking the presence of PCS during the examination. While some gynecologists now perform an initial laparoscopic view of the pelvis before CO2 insufflation to try and visualize varices, laparoscopy can still yield false negative results in a significant proportion (80-90%) of women who actually have PCS.
Transfundal Pelvic Venogram
Transfundal pelvic venography is an alternative diagnostic technique used by some physicians. This involves directly placing a catheter 0.5 to 1 cm into the myometrium under fluoroscopic guidance and injecting contrast. This technique can visualize venous abnormalities associated with the uterus but provides incomplete evaluation of the ovarian veins and other potential causes of pelvic varices.
Differential Diagnosis: Ruling Out Other Conditions
A crucial step in pelvic congestion syndrome diagnosis is differentiating it from other conditions that can cause chronic pelvic pain. The differential diagnosis for chronic pelvic pain is extensive and varied, necessitating a multidisciplinary approach to patient evaluation. Obstetrics and Gynecology (Ob/Gyn) specialists play a fundamental role in this assessment, and input from other specialties such as anesthesiology, gastroenterology, general surgery, neurology, hematology/oncology, psychiatry, and urology may be required depending on the individual case. Routine workup typically includes abdominal and pelvic examinations, Pap smear tests, routine laboratory blood work, and cross-sectional imaging to exclude other potential causes of pelvic pain.
Table 1. Chronic Pelvic Pain Differential Diagnosis
| Bowel pathology |
|---|
| Cancer/metastases |
| Endometriosis |
| Fibroids |
| Fibromyalgia |
| Neurologic pathology |
| Orthopedic pathology |
| Ovarian cyst |
| Pelvic congestion syndrome |
| Pelvic inflammatory disorder |
| Porphyria |
| Urologic pathology |
| Uterine prolapse |

Conclusion: Achieving Accurate PCS Diagnosis
Diagnosing Pelvic Congestion Syndrome remains a complex process, requiring a thorough and systematic approach. While challenging, accurate PCS diagnosis is achievable with increased awareness of the condition, recognition of its characteristic symptoms, and the strategic utilization of appropriate diagnostic modalities. Imaging techniques, particularly MRI/MRV and diagnostic venography, are pivotal in confirming PCS and guiding treatment strategies. Interventional radiology plays a central role in both the diagnostic and therapeutic pathways for PCS, offering minimally invasive solutions like embolotherapy that can significantly improve the quality of life for women suffering from this often-overlooked condition. Continued research and clinical vigilance are essential to further refine diagnostic approaches and optimize patient care for pelvic congestion syndrome.
REFERENCES
References are the same as the original article. (To be added if needed, as per original article).
