Placenta previa, a condition where the placenta partially or completely covers the cervix, poses significant risks during pregnancy. Primarily, it’s a major cause of postpartum hemorrhage, endangering both mother and neonate. This condition necessitates a Cesarean delivery as vaginal delivery is contraindicated. While most cases are detected through routine prenatal sonography, some present dramatically with painless vaginal bleeding, typically in the later trimesters. Furthermore, placenta previa increases the risk of placenta accreta spectrum (PAS), a severe condition involving abnormal placental invasion. Accurate and timely Placenta Previa Diagnosis is critical for managing pregnancy and planning for delivery to minimize risks. This article delves into the diagnostic process of placenta previa, emphasizing its importance in ensuring optimal maternal and fetal outcomes.
Understanding Placenta Previa: Etiology and Epidemiology
The exact cause of placenta previa remains unclear, but it’s strongly linked to endometrial damage and uterine scarring. Several factors elevate the risk, including advanced maternal age, multiple pregnancies (multiparity), smoking, cocaine use, prior uterine surgeries like suction and curettage, assisted reproductive technology (ART), previous Cesarean sections, and a history of placenta previa. These risk factors often share a common thread: disruption of the normal uterine lining, which can influence placental implantation.
Epidemiologically, placenta previa affects a notable proportion of pregnancies, ranging from 0.3% to 2% in the third trimester. The incidence has been rising, largely due to increasing rates of Cesarean deliveries. This highlights the importance of understanding and effectively managing this condition in contemporary obstetrics.
Pathophysiology and Classification of Placenta Previa
Placenta previa is defined by the placenta’s position relative to the cervix. It’s categorized based on the degree of cervical os coverage: complete previa (entire os covered), partial previa (partially covered), marginal previa (placental edge within 2cm of the os), and low-lying placenta (placental edge within 2 to 3.5 cm from the os). It’s crucial to understand that many cases initially diagnosed as low-lying placenta in early pregnancy resolve spontaneously as the pregnancy progresses. This phenomenon, known as placental migration, occurs because the placenta preferentially grows towards the better-vascularized fundus, while the portion near the cervix may atrophy. The expanding lower uterine segment also contributes to this apparent migration, increasing the distance between the placenta’s edge and the cervix.
History, Physical Examination, and Initial Suspicion
Risk factors play a crucial role in prompting suspicion for placenta previa. Advanced maternal age, multiparity, smoking, history of uterine procedures (curettage), cocaine use, and prior Cesarean births are significant indicators. Painless vaginal bleeding, especially in the second or third trimester, is the hallmark symptom. This bleeding can be spontaneous or triggered by intercourse, vaginal exams, or labor. While speculum examination may reveal the bleeding source and potentially visualize the placenta if the cervix is dilated, digital examination is strictly contraindicated due to the risk of provoking severe hemorrhage. Thus, in any case of second or third-trimester bleeding, placenta previa diagnosis should be considered and actively investigated before any digital cervical examination.
The Cornerstone of Placenta Previa Diagnosis: Sonography
Ultrasound, or sonography, is the primary and most reliable tool for placenta previa diagnosis. Routine prenatal ultrasounds in the first and second trimesters often provide the first indication of placenta previa. It’s important to note that early diagnosis, particularly before the third trimester, frequently indicates a transient condition due to placental migration. However, early detection allows for appropriate monitoring and planning.
For women presenting with vaginal bleeding in the second or third trimester, transabdominal sonography is the initial step, performed before any digital vaginal examination. If placenta previa is suspected on transabdominal ultrasound, a transvaginal sonogram is then performed for confirmation and to accurately assess the placental location relative to the internal cervical os. Transvaginal sonography is superior to transabdominal imaging in precisely determining the placental edge and is considered safe in this context. Sonography can clearly identify low-lying and marginal placenta, quantifying the distance between the placental edge and the internal os.
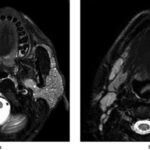
Caption: Transvaginal ultrasound is a key imaging modality in placenta previa diagnosis, offering a clear view of the placenta’s position in relation to the cervix.
Assessing Placenta Accreta Spectrum During Placenta Previa Diagnosis
Crucially, the diagnostic evaluation for placenta previa should also include an assessment for placenta accreta spectrum (PAS). The risk of PAS is significantly elevated in women with placenta previa, especially those with a history of Cesarean delivery. High suspicion for PAS should be present from the initial placenta previa diagnosis. PAS encompasses placenta accreta (abnormal adherence to the myometrium), increta (invasion into the myometrium), and percreta (invasion through the serosa and potentially into adjacent organs).
Ultrasound, particularly with Doppler studies, is highly sensitive and specific for PAS diagnosis. Specific sonographic findings suggestive of PAS include lacunae (vascular spaces) within the placenta, thinning of the myometrium overlying the placenta, and increased vascularity at the uterine-placental interface. In cases of posterior placenta previa or when bladder invasion is suspected, Magnetic Resonance Imaging (MRI) can be a valuable adjunct. While MRI can provide more detailed anatomical information, especially in challenging cases, it’s more costly and has not definitively shown to improve outcomes over ultrasound alone for PAS diagnosis. If PAS is highly suspected, planning for a Cesarean hysterectomy, where the placenta is left in situ to minimize hemorrhage, should be discussed proactively with the patient.
Differential Diagnosis: Ruling Out Other Causes of Bleeding
Vaginal bleeding during pregnancy can stem from various causes, and differential diagnosis is essential. The possibilities vary by trimester. In the first and second trimesters, causes include subchorionic hematoma, cervicitis, cervical cancer, threatened abortion, ectopic pregnancy, or molar pregnancy. In the third trimester, alongside placenta previa, other critical differentials include labor, placental abruption, and vasa previa.
Placental abruption, the premature separation of the placenta, is a life-threatening condition that must be differentiated from placenta previa. Abruption typically presents with severe abdominal pain, often accompanied by vaginal bleeding, and fetal heart rate abnormalities. Vasa previa, where fetal vessels traverse the membranes over the cervix, is another rare but critical condition to rule out, as rupture of these vessels during labor or membrane rupture can lead to rapid fetal exsanguination. Accurate placenta previa diagnosis is therefore not only about confirming previa but also about excluding other serious causes of third-trimester bleeding.
Management Based on Placenta Previa Diagnosis
Once placenta previa diagnosis is confirmed, management strategies are determined by gestational age, the severity of bleeding, and the presence of associated conditions like PAS. For a confirmed diagnosis without active bleeding, elective Cesarean delivery is typically scheduled between 36 to 37 weeks of gestation to balance the risks of prematurity and antepartum hemorrhage.
For patients presenting with vaginal bleeding and known placenta previa, immediate assessment includes vital signs monitoring, electronic fetal monitoring, intravenous access, and blood work (complete blood count, type and screen, coagulation studies). Significant bleeding necessitates blood transfusion. Immediate Cesarean delivery is indicated for excessive or continuous bleeding, regardless of gestational age. If bleeding subsides and gestational age is less than 36 weeks, expectant management may be considered, including hospitalization, fetal monitoring, and administration of corticosteroids for fetal lung maturity and magnesium sulfate for neuroprotection. While historically bed rest and pelvic rest were mandated, their clear benefit is not definitively established. The decision between inpatient and outpatient management depends on bleeding stability, gestational age, patient compliance, and proximity to medical care.
Delivery Planning and Team Approach
Delivery for placenta previa requires meticulous planning and a multidisciplinary team. Prenatal counseling should include a thorough discussion of the diagnosis, potential complications like postpartum hemorrhage and PAS, and the plan for Cesarean delivery, including the possibility of hysterectomy in severe cases. The surgical team, anesthesia team, nursing staff, neonatologists, and blood bank must be informed and prepared. In suspected PAS, involvement of urology, general surgery, and interventional radiology is crucial. Preoperative planning includes ensuring adequate intravenous access, cross-matched blood, and potentially prophylactic uterine artery catheter placement by interventional radiology.
Regional anesthesia (spinal-epidural) is generally preferred for non-urgent Cesarean deliveries in placenta previa due to reduced blood loss compared to general anesthesia. A vertical skin incision and potentially a high vertical uterine incision may be necessary for optimal exposure, especially in cases of complete previa. Postpartum hemorrhage is a significant risk due to lower uterine segment atony and may require various interventions, from uterotonics and uterine massage to intrauterine balloon tamponade, surgical sutures, and arterial ligation or embolization. Hysterectomy remains a last resort for uncontrolled hemorrhage. In cases of PAS, the placenta is intentionally left in situ, the uterus closed, and Cesarean hysterectomy performed to minimize blood loss.
Prognosis and Complications
Neonatal Prognosis: Placenta previa increases neonatal morbidity and mortality three to fourfold, primarily due to preterm birth. Neonates are at higher risk for prematurity, low birth weight, low Apgar scores, and respiratory distress syndrome.
Maternal Prognosis: While most cases of placenta previa resolve with delivery, maternal risks are substantial. These include postpartum hemorrhage, blood transfusion, injury to adjacent organs, Cesarean hysterectomy, ICU admission, and, rarely, maternal death. Women with anterior placenta previa may face poorer outcomes, including higher blood loss and hysterectomy rates, possibly due to increased PAS risk associated with prior uterine incisions. There is also an increased recurrence risk of placenta previa in subsequent pregnancies.
Complications: Vaginal bleeding from placenta previa can lead to severe postpartum hemorrhage, potentially requiring blood transfusion, hysterectomy, ICU care, septicemia, and maternal death. Undiagnosed or mismanaged placenta previa increases risks of preterm birth, low birth weight, prolonged hospitalization, and higher transfusion rates. The risk of PAS escalates significantly with increasing numbers of prior Cesarean sections in the presence of placenta previa.
Deterrence and Patient Education
Patient education is vital in managing placenta previa. Key points include:
- Placenta previa necessitates Cesarean delivery to avoid dangerous vaginal delivery.
- Elective Cesarean is typically planned for 36-37 weeks in uncomplicated cases.
- Pelvic rest, avoiding intercourse and digital exams, is crucial.
- Any vaginal bleeding requires immediate evaluation in the emergency room.
- Prior placenta previa and Cesarean history increase PAS risk.
- Cesarean hysterectomy may be necessary in cases of PAS.
Enhancing Healthcare Team Outcomes through Interprofessional Collaboration
Optimal management of placenta previa demands a coordinated interprofessional team. Open communication and collaboration among obstetricians, anesthesiologists, interventional radiologists, surgeons (vascular, urology, general), and nurses (labor and delivery, surgical, neonatal) are essential. Pre-delivery planning meetings, clear communication protocols, and shared awareness of patient status are crucial for anticipating and managing potential complications, ultimately improving outcomes for mothers and neonates affected by placenta previa.
Review Questions
(Please refer to the original article for review questions and figure)
References
(Please refer to the original article for the complete list of references)