Nursing care plans (NCPs) are indispensable tools in modern healthcare, serving as formalized, step-by-step blueprints for patient care. They are meticulously designed to pinpoint both current health needs and anticipate potential health risks, ensuring a proactive and comprehensive approach to patient well-being. This guide provides an in-depth exploration of nursing care plans, emphasizing their crucial role in addressing potential diagnoses and fostering effective communication among healthcare providers, patients, and their families. For nursing students and seasoned professionals alike, understanding and skillfully implementing nursing care plans is fundamental to delivering exceptional, patient-centered care.
Understanding Nursing Care Plans
A nursing care plan (NCP) is more than just a checklist; it’s a dynamic and systematic process. It begins the moment a patient enters a healthcare facility and evolves continuously, adapting to the patient’s changing health status and the outcomes of care evaluations. At its core, the NCP facilitates clear communication among all members of the healthcare team. This shared understanding is vital for ensuring consistency and quality in patient care, preventing fragmented approaches, and promoting a unified strategy to achieve optimal healthcare outcomes. Without a structured care planning process, the very essence of consistent and high-quality patient care would be compromised. The ability to plan and deliver individualized care is the cornerstone of excellence in nursing practice.
Types of Nursing Care Plans: Formal and Informal
Nursing care plans exist on a spectrum from informal to formal. An informal nursing care plan is essentially a mental strategy, a nurse’s internal roadmap for patient care. In contrast, a formal nursing care plan is a documented, structured guide, either written or electronic, that meticulously organizes all aspects of a patient’s care.
Formal care plans are further categorized into standardized and individualized approaches:
Standardized Care Plans: Consistency and Efficiency
Standardized care plans are pre-designed frameworks developed by nursing staff and healthcare organizations. They are designed to ensure consistent care for patients with common, recurring needs. These plans are valuable for establishing a baseline of acceptable care standards and optimizing nurses’ time by streamlining routine tasks that are frequently repeated across patient populations within a nursing unit.
It is crucial to recognize that standardized care plans are not specifically tailored to each patient’s unique circumstances and goals. However, they serve as an excellent starting point, providing a solid foundation upon which to build a more personalized individualized care plan.
The care plan examples presented in this resource are standardized care plans, intended to serve as a guide for developing individualized plans tailored to specific patient needs.
Individualized Care Plans: Patient-Centered and Holistic
An individualized care plan takes the standardized framework and customizes it to address the specific needs and goals of each patient. This involves incorporating approaches that have proven effective for the particular patient, taking into account their unique medical history, preferences, and personal circumstances. This individualized approach fosters more personalized and holistic care, aligning care strategies with the patient’s individual strengths, needs, and aspirations.
Furthermore, individualized care plans significantly contribute to improved patient satisfaction. When patients perceive that their care is specifically designed for them, they feel more valued and understood, leading to greater contentment with their overall healthcare experience. In today’s healthcare environment, where patient satisfaction is increasingly recognized as a key indicator of quality care, individualized care plans are more important than ever.
Tips for Individualizing a Nursing Care Plan: (This section would be expanded in a full article with specific tips)
Objectives of Nursing Care Plans: Guiding Principles
The creation and implementation of nursing care plans serve several critical objectives:
- Promoting Evidence-Based Care: NCPs encourage the use of the latest research and best practices in nursing, fostering a consistent and reassuring environment within healthcare settings.
- Supporting Holistic Care: NCPs emphasize a holistic care approach, considering the patient as a whole person – encompassing physical, psychological, social, and spiritual dimensions – in both disease management and prevention.
- Establishing Structured Care Programs: NCPs facilitate the development of structured programs like care pathways and care bundles. Care pathways ensure a collaborative, team-based approach to standardize care and expected outcomes, while care bundles focus on implementing best practices for specific conditions.
- Clearly Defining Goals and Outcomes: NCPs distinguish and define both overarching goals and specific, measurable expected outcomes for patient care.
- Enhancing Communication and Documentation: NCPs streamline communication and ensure thorough documentation of the care plan, creating a clear record for all healthcare providers.
- Measuring Nursing Care Effectiveness: NCPs provide a framework for evaluating the effectiveness of nursing interventions and care strategies, allowing for continuous improvement and adjustments as needed.
Purposes of Nursing Care Plans: Why They Matter
Nursing care plans are essential for a multitude of reasons, significantly impacting both the quality of patient care and the efficiency of healthcare delivery:
- Defining the Nurse’s Role: NCPs clearly delineate the unique and independent role of nurses in addressing patients’ comprehensive health and well-being. They empower nurses to act autonomously, not solely relying on physician directives but utilizing their expertise to provide holistic care.
- Providing Direction for Individualized Care: An NCP serves as a personalized roadmap, guiding the nursing care tailored to each patient’s specific needs. It encourages nurses to think critically and develop interventions that directly address the individual patient’s health challenges and goals.
- Ensuring Continuity of Care: NCPs are vital for maintaining consistent care across different nursing shifts and departments. By providing a shared source of patient data and planned interventions, they ensure that all nurses deliver the same high standard of care, maximizing the benefits of treatment for the patient.
- Coordinating Care Among Teams: NCPs promote effective care coordination by ensuring that all members of the healthcare team are informed about the patient’s needs and the required actions. This collaborative approach prevents gaps in care and ensures a unified, patient-centered strategy.
- Facilitating Comprehensive Documentation: NCPs serve as a structured format for documenting critical aspects of patient care, including observations, nursing actions, and instructions for the patient and family members. Accurate documentation within the NCP provides evidence that care was delivered and meets professional and legal standards.
- Guiding Staff Assignments: NCPs can inform staff assignments by highlighting patients with complex needs that require nurses with specific skills and expertise.
- Monitoring Patient Progress: NCPs provide a framework for tracking a patient’s progress against established goals. This monitoring allows for timely adjustments to the care plan as the patient’s condition evolves, ensuring the plan remains relevant and effective.
- Supporting Reimbursement Processes: Insurance companies often utilize medical records, including NCPs, to assess and determine appropriate reimbursement for healthcare services. Well-documented NCPs can support accurate and timely claims processing.
- Defining Patient Goals and Engagement: NCPs actively involve patients in their care planning, promoting a collaborative approach to treatment. This engagement empowers patients, making them active participants in their healthcare journey and fostering a sense of ownership and commitment to their health goals.
Key Components of a Nursing Care Plan
A standard nursing care plan (NCP) typically encompasses several core components, each playing a vital role in guiding patient care: nursing diagnoses, patient problems, expected outcomes, nursing interventions, and the rationales behind these interventions.
Nursing Care Plan Formats: Structuring for Clarity
Nursing care plans can be structured in various formats, often organized into columns to enhance clarity and ease of use. The most common formats include three-column and four-column plans. Some institutions may also utilize a five-column format.
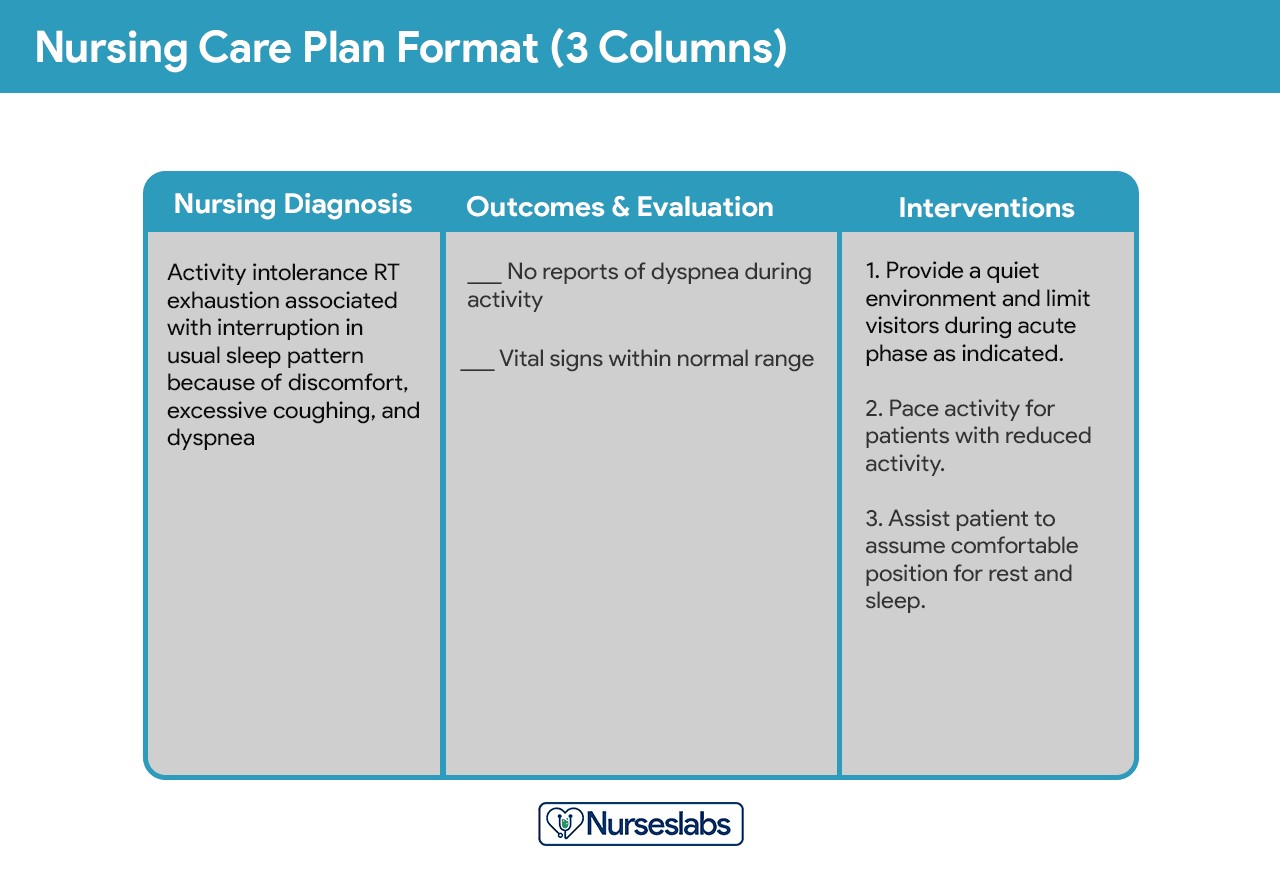
Three-Column Format: Concise and Efficient
The three-column format is a streamlined approach, typically including columns for:
- Nursing Diagnosis: Clearly stated patient health issues or potential risks.
- Outcomes and Evaluation: Desired patient outcomes and criteria for evaluating progress.
- Interventions: Specific nursing actions to achieve the desired outcomes.
Three-column nursing care plan format
Four-Column Format: Detailed and Comprehensive
The four-column format expands on the three-column structure, providing additional space for detailed planning:
- Nursing Diagnosis: Patient health issues or potential risks.
- Goals and Outcomes: Desired patient outcomes and measurable goals.
- Interventions: Detailed nursing actions, including frequency and specific instructions.
- Evaluation: Criteria and methods for evaluating the effectiveness of interventions and patient progress toward goals.
Four-column nursing care plan template
Sample templates for various nursing care plan formats are readily available for download and adaptation:
Download: Printable Nursing Care Plan Templates and Formats
Student Care Plans: In-Depth Learning Tools
Student care plans are intentionally more detailed and extensive than those used by practicing nurses. They serve as a critical learning tool for nursing students, fostering a deep understanding of the care planning process.
Student nursing care plans are more detailed.
Often, student care plans are required to be handwritten and include an additional column for “Rationale” or “Scientific Explanation.” This column necessitates students to articulate the scientific principles that justify each nursing intervention, strengthening their critical thinking and evidence-based practice skills.
Step-by-Step Guide to Writing a Nursing Care Plan
Creating an effective nursing care plan involves a systematic, step-by-step approach:
Step 1: Comprehensive Data Collection and Assessment
The initial step in crafting a nursing care plan is to establish a thorough patient database. This is achieved through meticulous assessment techniques and data collection methods, including physical assessments, detailed health histories, patient interviews, reviews of medical records, and diagnostic studies. This comprehensive client database encompasses all pertinent health information gathered. During this phase, nurses identify related or risk factors and defining characteristics that will inform the formulation of nursing diagnoses, including potential diagnoses. Many healthcare institutions and nursing programs provide specific assessment formats to guide this process.
Critical thinking is paramount in patient assessment. It involves integrating knowledge from various scientific disciplines and professional guidelines to inform evaluations. This process is crucial for complex clinical decision-making, aiming to effectively identify patients’ healthcare needs within a supportive environment and utilizing reliable information.
Step 2: Data Analysis and Organization for Potential Diagnoses
Once comprehensive patient data is collected, the next step involves rigorous analysis, clustering, and organization of this information. This process is crucial for formulating accurate nursing diagnoses, setting priorities, and defining desired outcomes, particularly when considering potential diagnoses. By carefully analyzing patterns and risk factors in the collected data, nurses can identify potential health problems before they fully manifest, allowing for proactive intervention and preventative care planning.
Step 3: Formulating Nursing Diagnoses, Including Potential Risks
Nursing diagnoses provide a standardized language for identifying, focusing on, and addressing specific patient needs and responses to both actual and high-risk health problems. These diagnoses encompass actual health issues as well as potential health problems that nursing interventions can prevent or resolve independently. The inclusion of potential diagnoses is a key aspect of proactive care planning, allowing nurses to address vulnerabilities and risks before they escalate into significant health concerns.
A detailed guide on formulating nursing diagnoses is available here: Nursing Diagnosis (NDx): Complete Guide and List.
Step 4: Prioritizing Diagnoses: Addressing Potential Issues Proactively
Prioritization involves establishing a strategic sequence for addressing nursing diagnoses and interventions. In this step, the nurse and patient collaboratively determine which identified problems, including potential diagnoses, require immediate attention. Diagnoses can be categorized by priority level: high, medium, or low. Life-threatening problems and those posing immediate risks are naturally assigned high priority. However, proactively addressing potential diagnoses is also a critical aspect of prioritization, as early intervention can prevent more serious issues from developing.
Nursing diagnosis prioritization often incorporates Maslow’s Hierarchy of Needs, a framework that organizes human needs into a pyramid, starting with basic physiological needs at the base and progressing to higher-level needs like self-esteem and self-actualization. Developed by Abraham Maslow in 1943, this hierarchy underscores that basic physiological needs must be met before higher needs can be addressed. In nursing, physiological and safety needs form the foundation of care and interventions.
Maslow’s Hierarchy of Needs:
- Basic Physiological Needs: These include the essentials for survival: nutrition (water and food), elimination, airway management (suction), breathing (oxygen), circulation (pulse, cardiac monitoring, blood pressure) (ABCs), sleep, sex, shelter, and exercise.
- Safety and Security Needs: Focus on protection from harm and establishing stability: injury prevention (side rails, call lights, hand hygiene, isolation, suicide precautions, fall precautions, car seats, helmets, seat belts), fostering trust and safety (therapeutic relationships), and patient education regarding modifiable risk factors (e.g., for stroke, heart disease).
- Love and Belonging Needs: Relate to social connection and acceptance: fostering supportive relationships, strategies to prevent social isolation (addressing bullying), active listening, therapeutic communication, and addressing needs for sexual intimacy.
- Self-Esteem Needs: Involve feelings of accomplishment and self-worth: community acceptance, professional achievements, personal accomplishments, a sense of control, and positive self-perception.
- Self-Actualization Needs: Represent reaching one’s full potential: empowering environments, spiritual growth, embracing diverse perspectives, and maximizing personal capabilities.
*Virginia Henderson’s 14 Needs as applied to Maslow’s Hierarchy of Needs. Learn more about it here. *
Patient values, beliefs, available resources, and the urgency of the situation are critical factors nurses consider when prioritizing diagnoses, including potential diagnoses. Patient involvement in this process is essential to foster cooperation and ensure the care plan aligns with their needs and preferences.
Step 5: Setting Client Goals and Desired Outcomes, Including Prevention of Potential Problems
Following diagnosis prioritization, nurses and patients collaboratively establish goals for each priority diagnosis, including goals related to preventing potential diagnoses from becoming actual problems. Goals or desired outcomes articulate what the nursing team aims to achieve through the implementation of nursing interventions derived from the patient’s nursing diagnoses. Goals provide direction for planning interventions, serve as benchmarks for evaluating patient progress, and enable both the patient and nurse to recognize problem resolution and experience a sense of accomplishment.
Examples of goals and desired outcomes. Notice how they’re formatted and written.
Typically, one overarching goal is defined for each nursing diagnosis. The terms “goal outcomes” and “expected outcomes” are often used interchangeably.
Effective goal setting follows the SMART criteria, as outlined by Hamilton and Price (2013):
- Specific: Goals should be clear, well-defined, and directly relevant to the patient’s needs.
- Measurable: Goals must be quantifiable, allowing for objective assessment of progress and achievement.
- Attainable: Goals should be realistic and achievable given the patient’s current condition, resources, and limitations.
- Realistic: Goals should be relevant to the patient’s overall health status and align with their values and priorities.
- Time-Oriented: Goals should include a specific timeframe for achievement, providing structure and a sense of urgency to the care plan.
Hogston (2011) proposes the REEPIG standards to further ensure high-quality care plans:
- Realistic: Goals and interventions must be feasible within available resources.
- Explicitly stated: Care plan components should be clearly and unambiguously defined to avoid misinterpretations.
- Evidence-based: Interventions should be supported by current research and best practices.
- Prioritized: The care plan should address the most urgent needs and potential risks first.
- Involve: Planning should be a collaborative process involving the patient and all relevant members of the multidisciplinary healthcare team.
- Goal-centered: All planned care should directly contribute to achieving the established patient goals.
Short-Term and Long-Term Goals: Addressing Immediate and Future Needs
Goals and expected outcomes must be measurable and patient-centered. They are framed around problem prevention, resolution, and rehabilitation. Goals are classified as either short-term or long-term. In acute care settings, most goals are short-term, focusing on immediate needs. Long-term goals are more relevant for patients with chronic conditions or those receiving care at home, in nursing homes, or in extended care facilities. Crucially, both short-term and long-term goals should address both actual and potential diagnoses.
- Short-term goal: Describes an achievable change in patient behavior or status that can be accomplished relatively quickly, typically within hours or days.
- Long-term goal: Indicates a broader objective to be achieved over a longer duration, such as weeks or months.
- Discharge planning: Primarily involves setting long-term goals that promote ongoing restorative care and problem resolution through home health services, physical therapy, or other referral sources. Discharge planning should also consider strategies for managing potential future health issues.
Components of Effective Goals and Desired Outcomes
Goal and desired outcome statements typically include four key components:
Components of goals and desired outcomes in a nursing care plan.
- Subject: The focus of the goal, typically the patient, a part of the patient (e.g., limb), or a patient attribute (e.g., vital sign). Often implied to be the patient unless otherwise specified.
- Verb: Specifies the action the patient is expected to perform, learn, or experience.
- Conditions or modifiers: Clarify the circumstances under which the behavior should occur, including “what,” “when,” “where,” and “how.”
- Criterion of desired performance: Defines the standard for evaluating performance or the level at which the patient will perform the behavior. This component is optional but adds specificity.
Key tips for writing effective goals and desired outcomes:
- Frame goals and outcomes in terms of patient responses, not nurse activities. Begin each goal with “Client will […],” emphasizing patient-centered outcomes.
- Focus on what the patient will achieve, not what the nurse hopes to accomplish.
- Utilize observable and measurable terms for outcomes, avoiding vague language that requires subjective interpretation.
- Ensure desired outcomes are realistic considering the patient’s resources, capabilities, limitations, and the timeframe of care.
- Verify that goals are compatible with therapies prescribed by other healthcare professionals.
- Ensure each goal is derived from only one nursing diagnosis, maintaining a clear link between diagnoses and planned interventions.
- Prioritize goals that are meaningful and valued by the patient to enhance cooperation and adherence to the care plan.
Step 6: Selecting Nursing Interventions: Addressing Potential Diagnoses
Nursing interventions are specific actions nurses undertake to help patients achieve their goals. Interventions should be carefully chosen to eliminate or reduce the underlying cause (etiology) of the prioritized nursing problem or diagnosis, including potential diagnoses. For risk diagnoses, interventions focus on mitigating the patient’s risk factors and preventing the potential problem from developing. While interventions are identified and documented during the planning phase of the nursing process, they are actually implemented during the implementation phase. For potential diagnoses, interventions are often preventative and educational in nature.
Types of Nursing Interventions: Independent, Dependent, and Collaborative
Nursing interventions can be categorized into three types: independent, dependent, and collaborative:
Types of nursing interventions in a care plan.
- Independent nursing interventions are actions nurses are authorized to initiate based on their professional judgment and expertise. These include ongoing assessments, emotional support, comfort measures (comfort), patient education, physical care, and referrals to other healthcare professionals. Many interventions for potential diagnoses, such as preventative education, are independent nursing actions.
- Dependent nursing interventions are carried out under the direction or supervision of a physician. These include administering medications, intravenous therapy, diagnostic tests, treatments, dietary orders, and activity or rest orders. Nurses remain responsible for assessment and patient education related to these dependent interventions.
- Collaborative interventions involve actions undertaken in coordination with other members of the healthcare team, such as physicians, social workers, dietitians, and therapists. These interventions are developed through consultation to leverage the diverse expertise within the team and provide holistic patient care, particularly when addressing complex potential diagnoses.
Effective nursing interventions should be:
- Safe and appropriate for the patient’s age, overall health, and specific condition, including any potential diagnoses.
- Achievable given available resources, time constraints, and staffing levels.
- Consistent with the patient’s values, cultural background, and beliefs.
- Integrated and compatible with other therapies the patient is receiving.
- Grounded in established nursing knowledge, clinical experience, and relevant scientific principles.
Key tips for writing effective nursing interventions:
- Date and sign the care plan upon completion. Dating is crucial for tracking plan reviews and updates. Nurse signatures ensure accountability.
- Interventions should be specific, clear, and action-oriented, beginning with an action verb that precisely describes the nurse’s expected action. Include qualifiers specifying how, when, where, frequency, duration, and amount to provide complete instructions. For example: “Educate parents on proper temperature measurement and when to report changes,” or “Assess urine characteristics including color, amount, odor, and turbidity every shift.”
- Use only standard abbreviations approved by the healthcare institution to ensure clarity and prevent errors.
Step 7: Providing Rationales: Justifying Interventions
Rationales, also known as scientific explanations, articulate the evidence base and underlying principles that justify each chosen nursing intervention in the NCP. Rationales are particularly valuable in student care plans, helping students connect pathophysiological and psychological concepts to practical nursing actions.
While rationales are not always included in routine care plans used by practicing nurses, understanding the scientific basis for interventions is crucial for all nurses to ensure evidence-based and effective care, especially when addressing potential diagnoses and implementing preventative measures.
Step 8: Evaluation: Assessing Progress and Plan Effectiveness
Evaluation is a systematic, ongoing process of assessing a patient’s progress toward achieving the established goals and desired outcomes. It also involves evaluating the overall effectiveness of the nursing care plan (NCP). Evaluation is a critical component of the nursing process because its findings determine whether interventions should be continued, modified, or discontinued. In the context of potential diagnoses, evaluation focuses on whether preventative interventions are effectively mitigating risks and preventing the potential problem from developing.
Step 9: Documenting the Care Plan: Creating a Living Record
The patient’s care plan is formally documented according to hospital policy and becomes an integral part of their permanent medical record. This documentation is essential for communication among healthcare providers, particularly during shift changes and handovers. Different nursing programs and healthcare institutions may utilize varying care plan formats. Most formats are designed to guide nurses and students through the logical steps of the nursing process. Many student care plans and some practice settings utilize a five-column format to include rationales.
Comprehensive Nursing Care Plan Resources
This section provides a categorized list of sample nursing care plans (NCPs) and nursing diagnoses for a wide range of diseases and health conditions, offering valuable resources for nurses in various specialties.
(The extensive list of Nursing Care Plans from the original article would be included here, categorized as in the original, but potentially with added sections or emphasis related to “potential diagnoses” where relevant.)
Recommended Resources for Nursing Care Planning
(The recommended books and resources from the original article would be included here, maintaining affiliate links and disclosures.)
References and Sources
(The references and sources section from the original article would be included here.)
(Social sharing buttons and other website elements from the original article would be omitted as per instructions.)