Heart failure (HF) diagnosis in primary care settings presents a significant challenge. While symptoms and signs are routinely assessed, their effectiveness in accurately identifying HF in community-based populations has been questioned. This article delves into a study that evaluated the diagnostic value of symptoms, signs, and medical history for heart failure within primary care.
The Diagnostic Dilemma in Primary Care
Early and accurate diagnosis of heart failure is crucial for timely intervention and improved patient outcomes. However, relying solely on traditional clinical assessments in primary care may lead to missed or delayed diagnoses. This is particularly relevant for patients with mild or atypical presentations of heart failure. To understand the limitations of this approach, a study was conducted in Portuguese primary care centers to assess the utility of symptoms, signs, and past medical history in diagnosing CHF.
Methods: Evaluating Diagnostic Accuracy
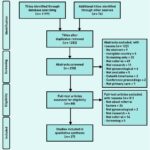
The study enrolled a large cohort of men and women attending 365 primary care centers for various health concerns, excluding acute infections, metabolic conditions, and pregnancy. Researchers used the Boston questionnaire to identify individuals at risk of heart failure. Patients scoring three or more points in specific sections of the questionnaire, along with those already receiving loop or thiazide diuretics for heart failure, were flagged for further evaluation. This evaluation included a resting echocardiogram to confirm cardiac dysfunction. The study then calculated key diagnostic metrics such as sensitivity, specificity, positive predictive value, negative predictive value, and likelihood ratios (LR) to determine the accuracy of different clinical indicators in diagnosing heart failure.
Results: Insights into Diagnostic Predictors
Out of 5434 participants, 1058 were referred for echocardiography, and 551 were confirmed to have cardiac dysfunction at rest. Notably, a significant proportion of these patients were in the early stages of heart failure, with 35.5% classified as NYHA class I.
The study revealed that certain historical factors strongly increased the likelihood of heart failure. Prior digoxin use (LR 24.9) and/or diuretic use (LR 10.6), a history of coronary artery disease (LR 7.1), and a history of pulmonary edema (LR 54.2) were all significant predictors. Among current symptoms, paroxysmal nocturnal dyspnea (LR 35.5), orthopnea (LR 39.1), and breathlessness when walking on level ground (LR 25.8) were also associated with a higher likelihood of heart failure.
However, the study highlighted a crucial point: these indicative symptoms were not commonly observed in the heart failure population within this primary care setting. This suggests that relying solely on the presence of these classic symptoms would miss a substantial number of cases, particularly those in earlier stages.
Physical signs like elevated jugular venous pressure (JVP) above 6 cm with hepatic enlargement and lower limb edema (LR 130.3), a ventricular gallop (LR 30.0), a heart rate exceeding 110 bpm (LR 26.7), and rales during lung auscultation (LR 23.3) were also strong predictors of heart failure. Similar to symptoms, these signs, while highly indicative, had low sensitivity, meaning they were infrequently present in patients with heart failure.
Conclusion: Rethinking Diagnostic Strategies in Primary Care
The findings of this study underscore the limited diagnostic value of relying solely on symptoms, signs, and clinical history for heart failure diagnosis in primary care. While certain symptoms and signs are strong predictors, they are often indicative of more advanced disease and lack the sensitivity needed to detect heart failure in its earlier stages. Over-reliance on these traditional clinical markers may lead to a significant underdiagnosis of heart failure, particularly in patients with milder symptoms.
This research emphasizes the need for a more comprehensive approach to Primary Care Diagnosis Of Heart Failure. Strategies should incorporate a lower threshold for further investigation, potentially including wider use of diagnostic tools like echocardiography, even in patients with less pronounced symptoms or signs. Focusing solely on patients with definite symptoms and signs will inevitably miss a considerable portion of individuals with heart failure, especially those who could benefit most from early intervention.