Diagnosing a pulmonary embolism (PE), a critical condition caused by a blood clot obstructing lung arteries, can be complex, particularly if pre-existing heart or lung conditions are present. A swift and accurate Pulmonary Embolism Diagnosis is paramount for initiating timely treatment and averting potentially life-threatening complications. This detailed guide explores the array of diagnostic tests and procedures employed to identify pulmonary embolisms, offering clarity on what patients can anticipate during the diagnostic journey. Typically, healthcare providers will begin with a thorough review of your medical history and a physical examination, followed by specific diagnostic tests to either confirm or exclude the presence of a PE. Let’s examine these vital diagnostic methodologies in greater detail.
Blood Tests for Pulmonary Embolism
Blood tests play a crucial role in the initial stages of pulmonary embolism diagnosis. One key test measures D-dimer, a substance released when blood clots dissolve. Elevated D-dimer levels might indicate the presence of blood clots, suggesting a possible PE. However, it’s important to note that various other conditions can also lead to increased D-dimer levels.
Additionally, arterial blood gas tests can assess the oxygen and carbon dioxide levels in your blood. A pulmonary embolism can disrupt blood flow in the lungs, potentially causing a decrease in blood oxygen levels. Further blood tests may be conducted to investigate inherited clotting disorders, which can increase the risk of developing blood clots and subsequently, pulmonary embolisms.
Chest X-Ray in Pulmonary Embolism Diagnosis
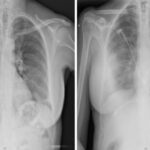
A chest X-ray is a standard, non-invasive imaging test used in the diagnostic process. It generates images of the heart and lungs. While a chest X-ray is not capable of directly diagnosing a pulmonary embolism and may even appear normal in the presence of a PE, it is invaluable for excluding other conditions that mimic PE symptoms, such as pneumonia or pneumothorax.
Ultrasound for Deep Vein Thrombosis Detection
Duplex ultrasonography, also known as a duplex scan or compression ultrasonography, is a non-invasive technique employing sound waves to examine veins, primarily to detect deep vein thrombosis (DVT), a common source of pulmonary embolisms. This ultrasound test effectively visualizes veins in the thigh, knee, and calf, and sometimes the arms.
During the procedure, a transducer, a handheld device, is moved across the skin, emitting sound waves towards the veins. These waves reflect back and are processed to create real-time images on a computer screen. The absence of blood clots in the veins significantly reduces the likelihood of DVT. If clots are detected, immediate treatment for potential pulmonary embolism is typically initiated.
CT Pulmonary Angiography: A Key Diagnostic Tool
CT pulmonary angiography (CTPA), also referred to as a CT pulmonary embolism study, is a highly effective imaging technique for pulmonary embolism diagnosis. Using X-rays and computer technology, CT scanning creates detailed cross-sectional images of the body. CTPA generates three-dimensional images of the pulmonary arteries, enabling the identification of blockages caused by pulmonary embolisms. Contrast dye, administered intravenously, is often used to enhance the visualization of blood vessels during the CT scan.
Ventilation-Perfusion (V/Q) Scan for Pulmonary Embolism
A ventilation-perfusion (V/Q) scan is an alternative diagnostic test, particularly useful when minimizing radiation exposure or avoiding contrast dye is necessary, such as in patients with kidney concerns or pregnant women where CTPA may not be preferred initially. In this procedure, a small amount of radioactive tracer is injected into a vein. The tracer maps blood flow (perfusion) and is compared to air flow (ventilation) in the lungs. A V/Q scan can help determine if blood clots are responsible for symptoms suggestive of pulmonary hypertension and PE.
Pulmonary Angiogram: The Gold Standard for Diagnosis
Pulmonary angiogram is considered the most accurate test for pulmonary embolism diagnosis, providing a clear visualization of blood flow within the lung arteries. However, due to its invasive nature, technical complexity, and potential risks, it is typically reserved for cases where other diagnostic tests are inconclusive.
The procedure involves inserting a thin, flexible catheter into a large vein, often in the groin, and guiding it through the heart and into the pulmonary arteries. A contrast dye is then injected through the catheter, and X-rays are taken as the dye moves through the arteries. While highly accurate, potential complications include temporary heart rhythm changes and, in individuals with pre-existing kidney issues, an increased risk of kidney damage from the contrast dye.
MRI for Pulmonary Embolism Diagnosis in Specific Cases
Magnetic Resonance Imaging (MRI) is an imaging technique utilizing magnetic fields and radio waves to create detailed images of body organs and tissues. In the context of pulmonary embolism diagnosis, MRI is typically employed in specific situations. It’s often favored for pregnant women to avoid fetal radiation exposure and for individuals with kidney conditions where contrast dyes used in other tests pose a risk. MRI can provide valuable diagnostic information without these concerns in select patient populations.
Conclusion
Accurate and timely pulmonary embolism diagnosis is critical for effective management and improved patient outcomes. A combination of blood tests, imaging techniques like CTPA, V/Q scans, ultrasound, and in some cases, pulmonary angiography and MRI, enables healthcare professionals to diagnose PE effectively. If you suspect you may have symptoms of a pulmonary embolism, seeking immediate medical attention is crucial to ensure prompt diagnosis and treatment.