Establishing an accurate pulpal and periapical diagnosis is paramount in dentistry, serving as the cornerstone for determining the most appropriate clinical treatment. In endodontics, a precise diagnosis is not merely a formality; it is the critical step that dictates whether a tooth requires root canal therapy (RCT), conservative management, or an entirely different approach. Incorrect diagnoses can lead to mistreatment, such as unnecessary procedures or, conversely, neglecting a tooth in dire need of intervention.
Beyond individual patient care, a standardized diagnostic system is crucial for effective communication within the dental community. Educators, clinicians, students, and researchers all benefit from a common language when discussing endodontic conditions. A clear, clinically-oriented system facilitates a shared understanding of pulpal and periapical diseases, guiding practitioners toward the best treatment strategies for each unique situation.
Recognizing this need for uniformity, the American Association of Endodontists (AAE) convened a consensus conference in 2008 to establish standardized diagnostic terms in endodontics. This initiative aimed to create universal recommendations and definitions that would be widely accepted across all facets of dentistry. The AAE and the American Board of Endodontics have since endorsed these terms, advocating for their consistent use throughout dental practice and education.
This article delves into these standardized diagnostic terms, outlining the clinical and radiographic characteristics of each condition. By providing clear definitions and illustrative examples, we aim to enhance your understanding of endodontic diagnosis and its vital role in modern dental practice. Remember, diseases of the pulp and periapical tissues are dynamic, and their presentation can vary based on the stage of the disease and individual patient factors. Accurate diagnosis requires a comprehensive approach, combining clinical examination, radiographic assessment, and pulp testing. For each tooth evaluated, a complete endodontic diagnosis must include both a pulpal and periapical component to ensure appropriate and effective treatment planning.
Examination and Diagnostic Procedures for RCT Diagnosis
Endodontic diagnosis is not a straightforward process; it is akin to assembling a jigsaw puzzle. A definitive diagnosis cannot be reached by relying on a single piece of information in isolation. Instead, clinicians must systematically gather data from various sources to formulate a “probable” diagnosis. The diagnostic journey begins with a thorough review of the patient’s medical and dental history. This initial step often provides valuable clues, allowing the clinician to start forming a preliminary, logical diagnosis, especially when the patient presents with a chief complaint.
Clinical and radiographic examinations are essential components of the diagnostic process. These examinations, combined with a comprehensive periodontal evaluation and specific clinical tests (such as pulp and periapical tests), serve to either confirm or refine the preliminary diagnosis. However, it’s important to acknowledge that clinical and radiographic findings can sometimes be inconclusive or even contradictory. In such instances, reaching a definitive pulpal and periapical diagnosis may not be immediately possible. It is crucial to emphasize that treatment should never be initiated without a clear diagnosis. In ambiguous cases, it may be necessary to postpone treatment, reassess the patient at a later appointment, or refer them to an endodontist for specialized evaluation.
Diagnostic Terminology Approved by the American Association of Endodontists and American Board of Endodontics
Pulpal Diagnoses Explained
Normal Pulp: This diagnostic category describes a pulp that is free of symptoms and responds normally to pulp testing. While histologically, the pulp might not be perfectly “normal,” a clinically normal pulp exhibits a mild and transient response to thermal (cold) testing. This response typically lasts for only one to two seconds after the stimulus is removed. Crucially, determining a “normal” diagnosis requires comparison with adjacent and contralateral teeth. It is recommended to test these teeth first to establish a baseline of normal response for the patient, facilitating more accurate interpretation of the test results on the tooth in question.
Reversible Pulpitis: This diagnosis is made when subjective and objective findings suggest that the pulpal inflammation is mild and should resolve, allowing the pulp to return to its normal state once the cause is addressed. Patients with reversible pulpitis typically experience discomfort when exposed to stimuli like cold or sweets, but the pain subsides quickly, usually within seconds after the stimulus is removed. Common causes include exposed dentin (dentinal sensitivity), dental caries, or deep restorations. Radiographically, there are usually no significant changes in the periapical region of the affected tooth. The pain associated with reversible pulpitis is stimulus-induced and not spontaneous. After addressing the underlying cause (e.g., removing caries and placing a restoration or covering exposed dentin), the tooth needs to be re-evaluated to confirm that the pulp has returned to a normal, healthy status. It’s worth noting that while dentinal sensitivity itself is not an inflammatory process, its symptoms closely mimic those of reversible pulpitis.
Symptomatic Irreversible Pulpitis: This condition is characterized by a vital, inflamed pulp that is deemed incapable of healing, thus necessitating root canal treatment. Key features may include sharp pain in response to thermal stimuli, lingering pain that persists for 30 seconds or longer after stimulus removal, spontaneous pain (unprovoked), and referred pain. Pain may be exacerbated by postural changes like lying down or bending over. Over-the-counter pain relievers are often ineffective in managing the discomfort. Common causes include deep caries, extensive restorations, or fractures that expose the pulp. Diagnosing symptomatic irreversible pulpitis can be challenging in the early stages because the inflammation may not yet have extended to the periapical tissues, meaning percussion might not elicit pain. In these situations, the patient’s dental history and thermal testing are the primary diagnostic tools for assessing pulpal status.
Asymptomatic Irreversible Pulpitis: This diagnosis indicates a vital, inflamed pulp that is incapable of healing, requiring root canal treatment, but without any clinical symptoms reported by the patient. These teeth usually respond normally to thermal testing, but they often have a history of trauma or deep caries that would likely lead to pulp exposure during caries removal. Despite the lack of symptoms, the underlying pulpal condition necessitates intervention.
Comparative testing for percussion and palpation should always begin with normal teeth to establish a baseline for the patient.
Pulp Necrosis: This diagnostic category signifies the death of the dental pulp, definitively requiring root canal treatment. The pulp is nonresponsive to pulp testing and is typically asymptomatic in itself. However, pulp necrosis can lead to apical periodontitis (pain to percussion or radiographic evidence of bone breakdown) if the root canal system becomes infected. It’s important to note that teeth may be nonresponsive to pulp testing for reasons other than necrosis, such as pulp canal obliteration (calcification), recent trauma, or simply a temporary state of unresponsiveness. This underscores the importance of comparative testing and considering the overall clinical picture.
Previously Treated: This category indicates that the tooth has already undergone endodontic treatment, and the root canals are obturated with filling materials (excluding intracanal medicaments). These teeth typically do not respond to thermal or electric pulp testing.
Previously Initiated Therapy: This diagnosis applies when a tooth has received partial endodontic therapy, such as a pulpotomy or pulpectomy. The response to pulp testing in these cases can vary depending on the extent of the previous treatment.
Key Takeaways for Pulpal Diagnosis
- Accurate pulpal and periapical diagnosis is essential for determining the correct clinical treatment, including the necessity of Rct Diagnosis.
- A standardized, clinically relevant diagnostic system is vital for clear communication and effective treatment planning in endodontics.
- Understanding the progressive nature of pulpal and periapical diseases is crucial for guiding clinicians to the most appropriate treatment approach.
- The diagnostic terms defined and endorsed by the AAE and American Board of Endodontics provide this necessary standardization.
- A comprehensive endodontic diagnosis always includes both a pulpal and periapical assessment for each tooth.
- In cases of diagnostic uncertainty, referring patients to an endodontist is a prudent step.
Apical Diagnoses Explained
Normal Apical Tissues: Normal apical tissues are not sensitive to percussion or palpation testing. Radiographically, the lamina dura surrounding the root apex is intact, and the periodontal ligament space exhibits a uniform width. Similar to pulp testing, establishing a baseline by testing normal teeth is essential for accurate percussion and palpation assessments.
Symptomatic Apical Periodontitis: This diagnosis indicates inflammation of the apical periodontium that produces clinical symptoms. The hallmark symptom is pain in response to biting and/or percussion or palpation. Radiographic changes may or may not be present, depending on the stage of the disease. Early stages might show a normal periodontal ligament width, while later stages can exhibit periapical radiolucency. Severe pain upon percussion and/or palpation is a strong indicator of a degenerating pulp and the need for root canal treatment.
Asymptomatic Apical Periodontitis: This condition involves inflammation and destruction of the apical periodontium, originating from pulpal pathology. It is characterized by an apical radiolucency on radiographs but lacks clinical symptoms, meaning there is no pain on percussion or palpation.
Chronic Apical Abscess: This represents an inflammatory reaction to pulpal infection and necrosis, developing gradually with minimal or no discomfort. A key feature is the intermittent discharge of pus through an associated sinus tract. Radiographically, signs of bone destruction, such as a radiolucency, are typically present. To pinpoint the source of a sinus tract, a gutta-percha cone can be gently inserted into the opening until it stops, followed by a radiograph to trace the tract back to its origin.
Acute Apical Abscess: This is an acute inflammatory response to pulpal infection and necrosis, characterized by rapid onset, spontaneous pain, extreme tenderness to pressure, pus formation, and swelling of surrounding tissues. Radiographic signs of bone destruction may be absent initially. Patients often experience systemic symptoms like malaise, fever, and lymphadenopathy.
Condensing Osteitis: This refers to a localized bony reaction to a low-grade inflammatory stimulus, typically seen at the apex of a tooth. It appears radiographically as a diffuse, radiopaque lesion.
Diagnostic Case Examples for RCT Diagnosis
Figure 1. This mandibular right first molar had previously been sensitive to cold and sweets, but these symptoms have subsided. Now, the tooth shows no response to thermal testing but is tender to biting and percussion. Radiographs reveal diffuse radiopacities around the root apices. Diagnosis: Pulp necrosis; symptomatic apical periodontitis with condensing osteitis. Non-surgical endodontic treatment is indicated, followed by a build-up and crown. The condensing osteitis is expected to regress over time, either partially or completely.
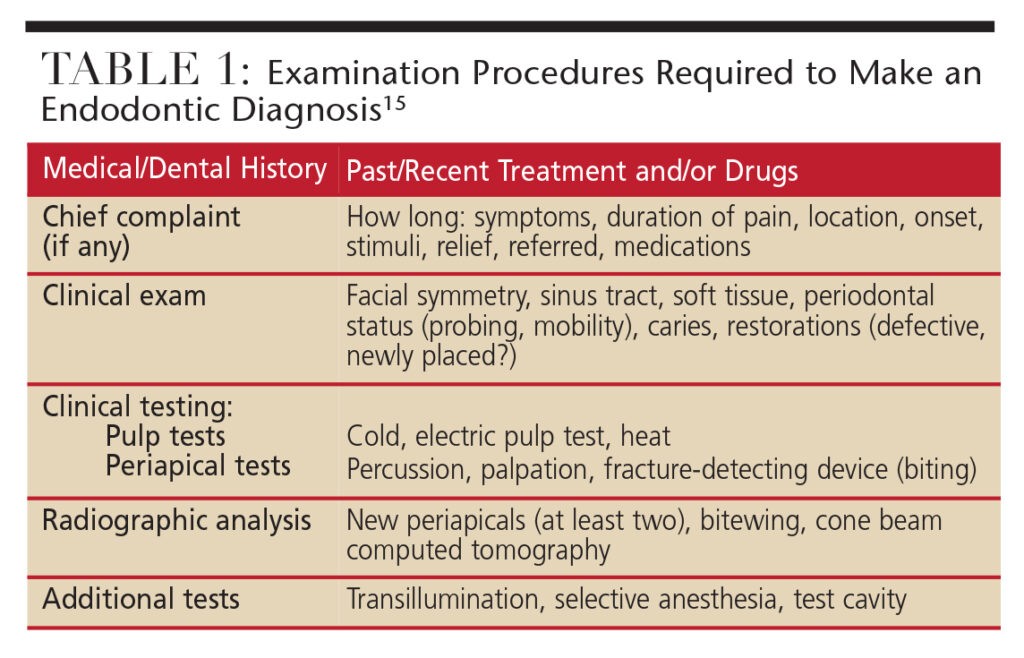 Figure 1: Mandibular right first molar with condensing osteitis
Figure 1: Mandibular right first molar with condensing osteitis
Figure 2. Following the placement of a full gold crown on a maxillary right second molar, the patient reported sensitivity to hot and cold liquids, which has now progressed to spontaneous discomfort. Thermal testing with a refrigerant spray elicits pain, and the discomfort lingers for 12 seconds after stimulus removal. Percussion and palpation responses are normal, and radiographs show no osseous changes. Diagnosis: Symptomatic irreversible pulpitis; normal apical tissues. Non-surgical endodontic treatment is recommended, with access to be restored with a permanent restoration. Note the severe distal caries on the maxillary second premolar, which, upon evaluation, was diagnosed as symptomatic irreversible pulpitis (hypersensitive to cold, lingering pain for eight seconds) and symptomatic apical periodontitis (pain to percussion).
Figure 3. A maxillary left first molar presents with occlusal-mesial caries, and the patient complains of sensitivity to sweets and cold liquids. There is no discomfort to biting or percussion. The tooth is hyperresponsive to thermal (cold) testing, but the pain does not linger. Diagnosis: Reversible pulpitis; normal apical tissues. Treatment involves caries excavation followed by a permanent restoration. If pulp exposure occurs during caries removal, non-surgical endodontic treatment and a crown would be necessary.
Figure 4. A mandibular right lateral incisor shows an apical radiolucency discovered during a routine examination. The patient has a history of trauma to the tooth more than 10 years prior, and the tooth is slightly discolored. It does not respond to thermal (cold) or electric pulp testing, while adjacent teeth respond normally. There is no tenderness to percussion or palpation. Diagnosis: Pulp necrosis; asymptomatic apical periodontitis. Treatment consists of non-surgical endodontic therapy, followed by bleaching and permanent restoration.
Figure 5. A mandibular left first molar exhibits a large apical radiolucency encompassing both mesial and distal roots, with furcation involvement. Periodontal probing depths are within normal limits. The tooth is nonresponsive to thermal (cold) testing, and percussion and palpation elicit normal responses. A draining sinus tract is present on the midfacial attached gingiva, traced with a gutta-percha cone. Recurrent caries is noted around the distal margin of the crown. Diagnosis: Pulp necrosis; chronic apical abscess. Treatment includes crown removal, non-surgical endodontic treatment, and placement of a new crown.
Figure 6. A maxillary left first molar, previously endodontically treated over 10 years ago, presents with pain on biting for the past three months. Apical radiolucencies are visible around all three roots. The tooth is tender to percussion and fracture-detecting device testing. Diagnosis: Previously treated; symptomatic apical periodontitis. Treatment involves non-surgical endodontic retreatment, followed by permanent restoration of the access cavity.
Figure 7. A maxillary left lateral incisor exhibits an apical radiolucency. There is no history of pain, and the tooth is asymptomatic. It does not respond to thermal (cold) or electric pulp testing, while adjacent teeth respond normally. Percussion and palpation are not tender. Diagnosis: Pulp necrosis; asymptomatic apical periodontitis. Treatment is non-surgical endodontic therapy and placement of a permanent restoration.
Conclusion: The Importance of Accurate RCT Diagnosis
Recognizing that accurate pulpal and periapical diagnosis is the foundation for appropriate clinical treatment, dental professionals should consistently apply this universal classification system. This standardized approach, endorsed by the AAE and American Board of Endodontics, helps ensure effective clinical management in endodontics, particularly in determining the necessity of RCT diagnosis. While this system significantly reduces potential confusion, clinicians must remember that pulpal and periapical diseases are dynamic and progressive. Signs and symptoms can vary depending on the disease stage and patient-specific factors.
Remember, a definitive diagnosis is rarely based on a single piece of information. Treatment decisions should always be grounded in a comprehensive diagnosis. In situations where uncertainty prevails, it is always advisable for general practitioners to refer patients to an endodontic specialist for further evaluation and expert management.
References
- Glickman GN. AAE consensus conference on diagnostic terminology: background and perspectives. J Endod. 2009;35:1619.
- Seltzer S, Bender IB, Ziontz M. The dynamics of pulp inflammation: correlations between diagnostic data and actual histologic findings in the pulp. Oral Surg Oral Med Oral Pathol. 1963;16:846–871;969–977.
- Berman LH, Hartwell GR. Diagnosis. In: Cohen S, Hargreaves KM, eds. Pathways of the Pulp, 11th ed. St. Louis, MO: Mosby/Elsevier; 2011:2–39.
- Schweitzer JL. The endodontic diagnostic puzzle. Gen Dent. 2009;57(6):560–567.
- AAE Consensus Conference Recommended Diagnostic Terminology. J Endod. 2009;35:1634.
- American Association of Endodontists. Glossary of Endodontic Terms. 8th ed. 2012.
- Glickman GN, Bakland LK, Fouad AF, Hargreaves KM, Schwartz SA. Diagnostic terminology: report of an online survey. J Endod. 2009;35:1625.
- Jafarzadeh H, Abbott PV. Review of pulp sensibility tests. Part I: general information and thermal tests. Int Endod J. 2010;43:738–762.
- Jafarzadeh H, Abbott PV. Review of pulp sensibility tests. Part II: electric pulp tests and test cavities. Int Endod J. 2010;43:945–958.
- Newton CW, Hoen MM, Goodis HE, Johnson BR, McClanahan SB. Identify and determine the metrics, hierarchy, and predictive value of all the parameters and/or methods used during endodontic diagnosis. J Endod. 2009;35:1635.
- Levin LG, Law AS, Holland GR, Abbot PV, Roda RS. Identify and define all diagnostic terms for pulpal health and disease states. J Endod. 2009;35:1645.
- Gutmann JL, Baumgartner JC, Gluskin AH, Hartwell GR, Walton RE. Identify and define all diagnostic terms for periapical/periradicular health and disease states. J Endod. 2009;35:1658.
- Rosenberg PA, Schindler WG, Krell KV, Hicks ML, Davis SB. Identify the endodontic treatment modalities. J Endod. 2009;35:1675.
- Green TL, Walton RE, Clark JM, Maixner D. Histologic examination of condensing osteitis in cadaver specimens. J Endod. 2013;39:977–979.
- Abbott PV, Yu C. A clinical classification of the status of the pulp and the root canal system. Aust Dent J. 2007;52(Endod Suppl):S17–S31.
A version of this article originally appeared in ENDODONTICS: Colleagues for Excellence, Fall 2013. Reused with permission from the American Association of Endodontists, ©2013. The AAE clinical newsletter is available at [aae.org/colleagues](http://aae.org/colleagues).