Shoulder Injury Related to Vaccine Administration (SIRVA) is a condition that, while rare, is gaining increased attention in the medical community. It’s characterized by persistent shoulder pain and dysfunction that arises typically within 48 hours following a vaccination administered in the deltoid muscle. As global vaccination efforts expand, understanding and accurately diagnosing SIRVA becomes increasingly crucial. This article delves into the essential aspects of SIRVA, with a particular focus on its diagnosis, to equip healthcare professionals and individuals with the knowledge needed for timely recognition and management.
What is SIRVA? Background and Significance
SIRVA is not a reaction to the vaccine itself, but rather an injury resulting from the administration process. It’s often linked to improper injection technique, which can lead to inflammation and injury of the shoulder structures surrounding the injection site. While mild, short-term shoulder discomfort is a common and expected side effect of intramuscular injections, SIRVA involves more severe and prolonged pain that can significantly impact a person’s quality of life. With millions receiving vaccinations annually, recognizing and effectively addressing SIRVA is paramount to minimizing patient discomfort and ensuring confidence in vaccination programs.
Epidemiology: How Common is SIRVA?
The exact incidence of SIRVA is still being studied, but it’s considered uncommon. Initially underreported, awareness of SIRVA has grown, particularly after its inclusion in the National Vaccine Injury Compensation Program (VICP) in 2017. Reports to the VICP have increased over the years, suggesting a greater recognition of the condition rather than necessarily a dramatic rise in occurrence. Studies indicate that SIRVA may be slightly more prevalent in women, and while it can occur across a wide age range, the type of vaccine associated with SIRVA cases varies, with influenza vaccines historically being frequently reported. Ongoing research is crucial to better define the epidemiology of SIRVA, especially in relation to newer vaccines like those for COVID-19.
Anatomy and Injury Mechanism in SIRVA
Understanding the anatomy of the shoulder is key to grasping how SIRVA occurs. Vaccines intended for intramuscular delivery in the deltoid can, if improperly administered, affect various structures. These include the glenohumeral joint, the surrounding shoulder capsule, the rotator cuff tendons, and the subacromial and subdeltoid bursae. The axillary nerve, which controls the deltoid muscle, also lies in proximity to the injection site and is potentially vulnerable.
Proper vaccine injection site and rotator cuff anatomy for understanding sirva diagnosis.
SIRVA injuries can arise from:
- Too deep injection: Penetrating the shoulder capsule can cause synovitis (joint inflammation) or even septic arthritis (joint infection).
- Injection into the rotator cuff: This can lead to tendinitis (tendon inflammation) or rotator cuff tears.
- Injection into the subacromial/subdeltoid space: Bursitis (inflammation of the bursa) and adhesive capsulitis (frozen shoulder) can result.
- Axillary nerve proximity injection: Nerve irritation, paresthesia (numbness/tingling), and temporary deltoid weakness are possible.
- Local inflammatory reaction: The vaccine serum itself can trigger inflammation (myositis, bursitis). Allergic reactions to vaccine components like egg proteins, gelatin, yeast, latex, or polyethylene glycol (in mRNA COVID-19 vaccines) can also contribute.
Anatomic structures at risk during vaccine injection, important for sirva diagnosis considerations.
The body’s inflammatory response to these injuries can further exacerbate tissue damage, potentially turning an initial minor injury into a more chronic problem. Pre-existing, asymptomatic rotator cuff issues, common in older individuals, can also be aggravated by vaccine administration, leading to acute symptoms.
Presentation and Symptoms: Recognizing SIRVA
While most vaccine-related shoulder discomfort resolves quickly, SIRVA is characterized by persistent and often debilitating pain. Key indicators include:
- Rapid onset: Pain typically starts within moments to 48 hours, and up to 4 days post-vaccination.
- Localized pain: Symptoms are concentrated in the vaccinated shoulder.
- Prolonged duration: Pain and dysfunction persist beyond a few days, often for weeks or months.
Common symptoms reported in SIRVA cases are:
- Shoulder pain: Nearly universally present.
- Limited Range of Motion: Difficulty moving the shoulder.
- Shoulder Weakness: Reduced strength in the affected arm.
- Paresthesia/Tingling: Numbness or tingling sensations.
Systemic symptoms like fever are uncommon in SIRVA, unless an infection is involved. It’s crucial to differentiate SIRVA from other shoulder conditions, making accurate diagnosis essential for appropriate management.
Clinical Evaluation and SIRVA Diagnosis
A thorough clinical evaluation is crucial for accurate Sirva Diagnosis. This process involves several key steps:
-
Patient History: A detailed history is taken to establish the temporal relationship between vaccination and symptom onset. It’s important to rule out pre-existing shoulder problems or other medical conditions that could be contributing to the pain.
-
Physical Examination:
- Inspection: The injection site is examined for redness (erythema), swelling (edema), or signs of infection.
- Palpation: Gentle touch to identify hematomas, abscesses, or crepitus (crackling sound).
- Range of Motion Assessment: Active and passive range of motion are evaluated to identify limitations and pain triggers.
- Strength Testing: Deltoid muscle strength is assessed through resisted abduction and forward flexion, although pain can confound strength evaluation.
- Neurovascular Exam: While vascular injuries are rare in SIRVA, a basic neurovascular exam is performed to rule out other issues and assess nerve function.
-
Diagnostic Studies: Imaging and electrodiagnostic studies play a vital role in confirming sirva diagnosis and ruling out other pathologies.
- Radiographs (X-rays): While often not revealing in early SIRVA, radiographs can rule out bony abnormalities.
- Magnetic Resonance Imaging (MRI): MRI is the imaging modality of choice for sirva diagnosis. It provides detailed visualization of soft tissues, allowing for the identification of:
- Subacromial bursitis
- Joint synovitis
- Adhesive capsulitis
- Rotator cuff injuries
- Hematomas
- Infections (contrast-enhanced MRI is helpful for suspected infections to assess tissue necrosis and bone involvement).
- Ultrasound: Ultrasound can be an alternative if MRI is unavailable, offering a less detailed but still valuable assessment of bursitis and rotator cuff issues.
- Electrodiagnostic Evaluation (Nerve Conduction Studies and Electromyography): Recommended if neurological symptoms (pain, numbness, weakness) are prominent. These studies are most accurate when performed 2-3 weeks post-vaccination to allow for nerve damage to be detectable. They help diagnose nerve injuries like neuritis or neuropathy.
Table 1. Anatomic Location and Potential Injuries Caused by SIRVA
| Anatomic Location | Potential Injuries |
|---|---|
| Deltoid muscle | Myositis, Abscess |
| Subacromial space | Bursitis, Septic bursitis |
| Rotator cuff | Tendonitis, Tear or rupture |
| Glenohumeral joint | Adhesive capsulitis, Septic arthritis |
| Axillary nerve | Neuritis, Neuropathy |
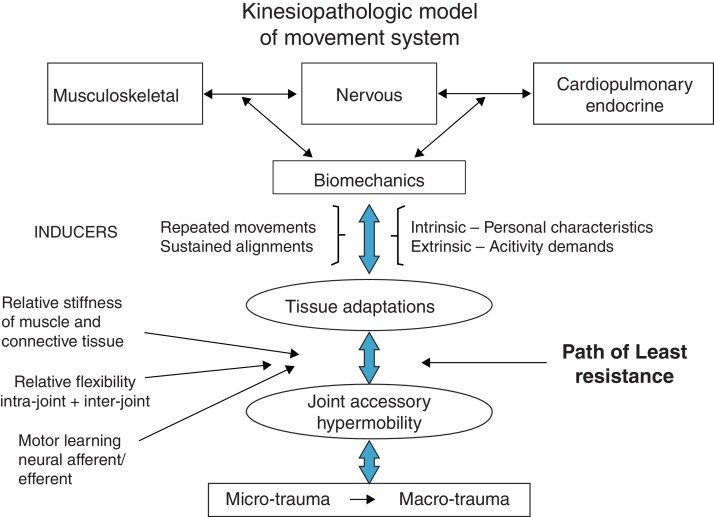
Table summarizing potential injuries based on anatomical location, crucial for sirva diagnosis.
Table 2. Reported Symptoms or Diagnosis, Treatment, and Resolution of SIRVA
| Author | Patients, n | Reported Symptoms or Diagnosis | % | Treatments | n (%) | Resolution, n (%) |
|---|---|---|---|---|---|---|
| Atanasoff et al19 | 13 | Shoulder pain, Limited ROM, Altered sensation, Weakness | 100, 84.6, 30.8, 30.8 | NSAIDs, Steroid injection, Physical therapy, Surgery | 8 (61.5), 8 (61.5), 6 (46.2), 4 (30.8) | 4 (30.8) |
| Chuaychoosakoon et al13 | 1 | Shoulder pain, Limited ROM, Fever | 100 | Intravenous antibiotics | 1(100) | 1(100) |
| Cross et al29 | 2 | Shoulder pain, Limited ROM, Supraspinatus tear | 100, 100, 50 | Surgical joint washout, Steroid injection | 1 (50), 1 (50) | 2 (100) |
| Hesse et al10 | 16 | Subdeltoid bursitis | 100 | Surgery, Steroid injection | 4 (25), 1 (6.3) | 2 (12.5) |
| Hesse et al9 | 476 | Shoulder pain, Rotator cuff problems, Bursitis, Local reaction, Adhesive capsulitis, Adverse effects of vaccination, Neuritis, Impingement, Other, Not specified | 31.9, 13.9, 11.8, 8.2, 5.5, 2.5, 2.3, 1.9, 9.7, 18.5 | Physical or occupational therapy, Steroid injections, NSAIDs or other analgesics, Surgery, Oral steroids, Exercise routine, Opiates, Chiropractic treatment, Muscle relaxant, Acupuncture | 381 (80), 286 (61.1), 240 (50.4), 155 (32.5), 130 (27.3), 111 (23.3), 65 (13.7), 30 (6.3), 29 (6.1), 18 (3.8) | 116 (24.3) |
| Hibbs et al4 | 1,220 (symptoms), 546 (treatments) | Shoulder pain, Limb mobility decreased, Joint ROM decreased, Rotator cuff syndrome, Bursitis, Arthralgia, Frozen shoulder, Pain in joint involving shoulder region, Injection site joint pain, Stiffness shoulder, Shoulder bursitis, Injection site joint movement impairment | 44.1, 40.8, 22.1, 9.2, 9.0, 8.8, 5.2, 3.2, 2.9, 2.9, 2.8, 2.4 | Nonnarcotic analgesics, Physical therapy, Corticosteroid injection, Hot and cold therapy, Oral steroids, Narcotic analgesics, Home shoulder exercise, Pain medication, not specified, Surgery, Muscle relaxants, Topical analgesics, Massage, Chiropractic, Sling, Acupuncture, Shoulder manipulation with sedation, Antibiotics, Muscle stimulators, Other | 254 (46.5), 215 (39.4), 109 (20.0), 89 (16.3), 79 (14.5), 28 (5.1), 19 (3.5), 17 (3.1), 16 (2.9), 15 (2.7), 10 (1.8), 10 (1.8), 7 (1.3), 6 (1.1), 4 (0.7), 2 (0.4), 2 (0.4), 2 (0.4), 41 (7.5) | Not reported |
| Rodrigues et al14 | 1 | Shoulder pain, Limited ROM | 100 | Ice packs, Physical therapy, Oral steroids | 1(100) | Not reported |
| Veera et al20 | 1 | Shoulder pain, Decreased range of motion, Paresthesia | 100 | Osteopathic manipulative medicine under general anesthesia, Acupuncture treatments, Nonanesthetic osteopathic manipulations, Physical therapy | 1 (100) | 1 (100) |
| Wong et al30 | 1 | Shoulder pain, Rotator cuff bursitis, Impingement syndrome | 100 | Arthroscopic shoulder debridement, Subacromial bursectomy | 1 (100) | 1 (100) |
| Wright et al23 | 1 | Shoulder pain, Subacromial or subdeltoid bursitis | 100 | Steroid injection | 1 (100) | 1 (100) |
Summary of symptoms, diagnosis, treatments and resolution in SIRVA cases, supporting sirva diagnosis understanding.
Treatment Strategies for SIRVA
Treatment for SIRVA is individualized and guided by the sirva diagnosis, focusing on symptom relief and functional recovery. There’s no standardized protocol, but common approaches include:
-
Conservative Management (Non-surgical):
- Rest and Activity Modification: Avoiding activities that aggravate shoulder pain.
- Pain Relief Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) and analgesics are often the first line.
- Physical Therapy: Crucial for restoring range of motion, strength, and function.
- Corticosteroid Injections: Local or oral steroids may be used for persistent inflammation, such as bursitis or synovitis.
-
Surgical Intervention: Reserved for cases unresponsive to conservative treatment, or when structural damage like rotator cuff tears is diagnosed. Surgical options may include tissue repair or nerve decompression.
-
Management of Nerve Injury: Similar to non-infectious SIRVA, initial treatment is conservative, including:
- Rest, activity modification, NSAIDs.
- Nerve modulating medications (e.g., gabapentin, pregabalin).
- Physical therapy focusing on joint mobilization, muscle strengthening, nerve gliding, and desensitization.
-
Infection Management: If infection is diagnosed, treatment depends on severity:
- Oral antibiotics: For uncomplicated infections.
- Intravenous antibiotics, surgical debridement: For severe infections, abscesses, or necrotizing fasciitis. Diagnostic procedures like blood cultures, aspiration, biopsy, and imaging (MRI, ultrasound) are essential to guide treatment.
Outcomes and Prognosis after SIRVA Diagnosis
The long-term outcomes of SIRVA are variable, and data is still limited. Many patients experience residual pain and some degree of persistent range of motion restriction even after treatment. Studies indicate that a significant portion of SIRVA patients do not achieve full resolution of symptoms. However, early sirva diagnosis and prompt, appropriate treatment can improve the chances of a better outcome. Case reports sometimes show higher rates of recovery, potentially due to the nature of case-specific interventions. Ongoing research is needed to better understand the factors influencing SIRVA prognosis and to optimize treatment strategies.
Prevention of SIRVA: Best Practices
Preventing SIRVA is the most effective strategy. Emphasis should be placed on proper vaccine administration technique:
- Correct Needle Selection: Choosing the appropriate syringe, needle gauge, and needle length based on patient age and body size.
- Accurate Injection Site: Injecting into the thickest part of the deltoid muscle, at a 90-degree angle, approximately 2 inches below the acromion, and just below the armpit level. Careful anatomical landmark identification is crucial.
- Training and Education: Ensuring healthcare providers are thoroughly trained in proper intramuscular injection techniques.
While even with correct technique SIRVA can still occur in rare cases, meticulous attention to administration protocols can significantly minimize the risk.
Conclusion: The Importance of SIRVA Diagnosis and Awareness
As vaccination rates continue to rise globally, SIRVA is a condition that healthcare providers need to be increasingly aware of. While rare, its potential to cause significant and prolonged shoulder dysfunction necessitates a strong understanding of its diagnosis, management, and prevention. Accurate sirva diagnosis, based on clinical evaluation and appropriate diagnostic studies, is the cornerstone of effective treatment. Continued research, improved diagnostic protocols, and a focus on preventative injection techniques are essential to minimize the impact of SIRVA and ensure public confidence in vaccination programs.